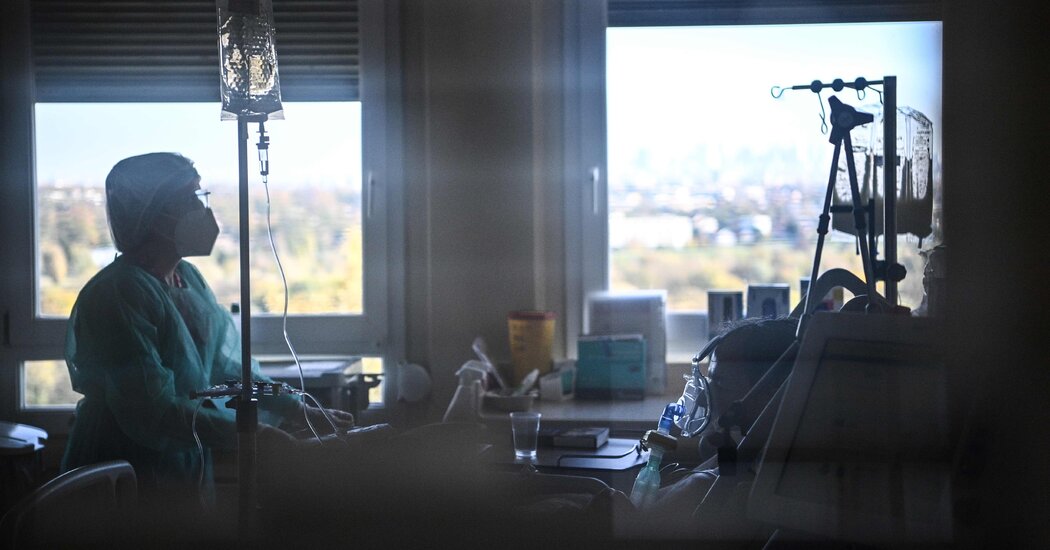
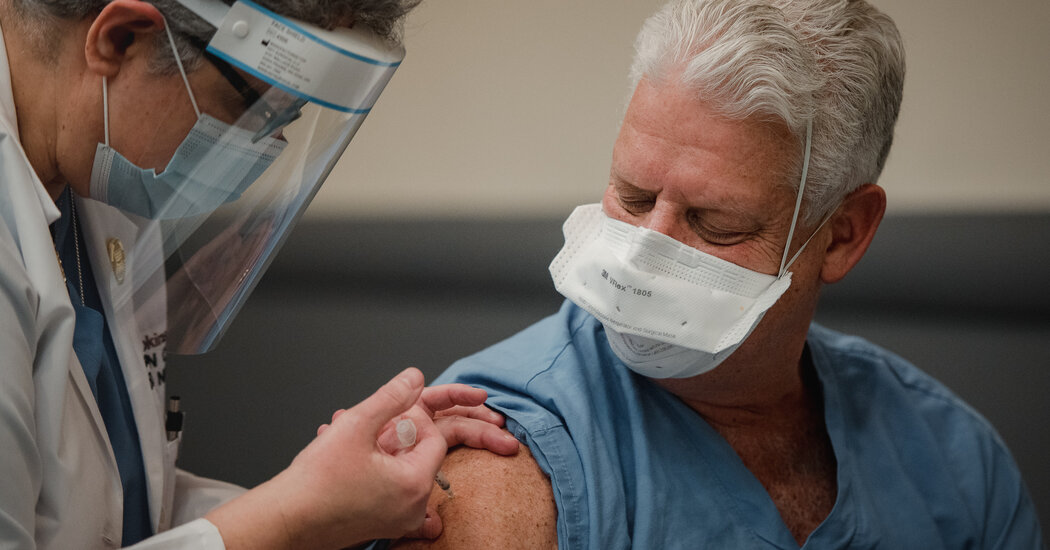
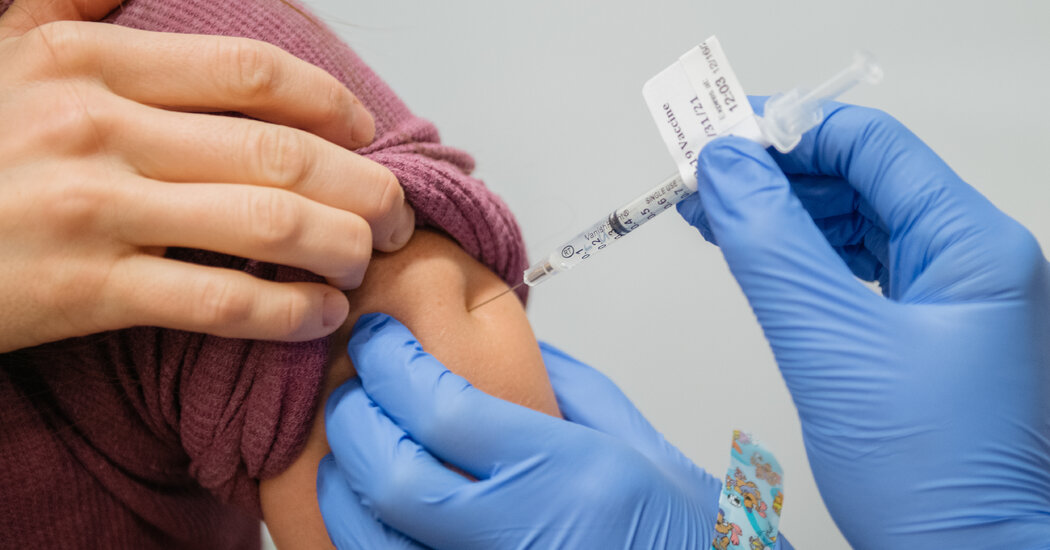
A 20 year old who works on computers. A young researcher studying cancer. Technicians in basic research laboratories.
These are some of the thousands of people who have been vaccinated against the coronavirus at Columbia University, New York University, Harvard, and Vanderbilt hospitals, despite millions of frontline workers and older Americans waiting their turn.
The Centers for Disease Control and Prevention have issued recommendations to ensure the country’s vaccines reach those most at risk first: healthcare workers interacting with Covid-19 patients, residents and nursing home workers, followed by Persons aged 75 and 75 older and certain essential employees.
Each state has its own version of the guidelines, but as the rollout pace has accelerated, the pressure for a more flexible approach has increased. Officials from the CDC and the Food and Drug Administration recently suggested that it might be wiser to just relax the criteria and distribute the vaccine as widely as possible.
However, these officials did not intend that the vaccines should be given to healthy people in their twenties and thirties, in front of the elderly, important workers, or anyone else at risk. States should continue to prioritize groups that “make sense,” said Dr. Stephen Hahn, the FDA commissioner, told reporters on Friday.
But a handful of the most prestigious academic hospitals in the country have already taken the idea much further. Workers unrelated to patient care who are not 75 years of age or older were offered admissions. Some of the institutions were among the earliest recipients of the limited shipments in the United States.
“Cronyism and connections have no place in the launch of this vaccine,” said Ruth Faden, a bioethicist at Johns Hopkins University in Baltimore. “If we don’t do it right, the consequences can be pretty disastrous, so it’s very important that people here are overly sensitive to the rules of the game.”
The CDC never intended to include workers who do not interact with patients, such as administrators and graduate students, in the first tier of priority vaccinations, said Dr. Stanley Perlman, an immunologist at the University of Iowa and a member of the committee issued the recommendations.
“It all got so confusing,” he said. “Looking back, I think it probably had to be a bit more specific about what we thought because we never thought of hospital administrators.”
In Nashville, Vanderbilt University Medical Center asked all staff whether they were treating patients or not to register for the vaccination. Vaccinations began in December when the Tennessee Hospital Association approved vaccinations for all hospital workers regardless of role.
On January 6, the medical center announced plans to begin vaccinating its high-risk patients, but only after “the initial vaccine dose to well over 15,000 at the medical center,” according to an email it sent to the medical center working people had administered “patients.
“We continue to follow instructions received from the Tennessee Department of Health when we vaccinate Vanderbilt Health staff and other priority groups of patients, staff and community health workers,” said John Howser, chief communications officer for the medical center. said in a statement.
But the Tennessee Department of Health sees it differently. “Hospitals have been encouraged since the onboarding process began to use any remaining vaccines to vaccinate high priority populations,” said Bill Christian, a department spokesman.
“Some hospitals have interpreted their ‘staff’ broadly,” he added.
The Tennessee department, he said, “continues to applaud hospitals that have only prioritized their high-risk frontline staff for vaccination and made any remaining vaccinations available to meet community vaccination needs,” groups with high priority.
“I wish our elderly relatives had the vaccine before I did,” said a young Vanderbilt employee who has no contact with patients and asked not to be identified for fear of reprisals.
In Boston, Brigham and Women’s Hospital and Massachusetts General Hospital, both affiliated with Harvard University, have immunized more than 26,000 employees, including those involved in patient care, researchers who may come into contact with coronavirus samples, and those involved in clinical trials are Rich Copp, a spokesman for the hospitals.
The reason? Some laboratory scientists may be needed in the hospitals if the coronavirus returns. “Our experience in the first wave showed that some members of the research community may need to be redeployed to support work in patient care with Covid,” said Copp.
Still, the medical centers have announced plans to immunize the rest of their staff from Monday.
In New York State, only a fraction of the estimated 2.1 million front-line workers were vaccinated. Governor Andrew Cuomo has threatened to impose fines of up to $ 100,000 on hospitals for not vaccinating fast enough to use their doses.
At Columbia University, the news quickly spread to research laboratories far removed from patient care: If you showed up at Millstein Hospital, the university’s primary medical center, you could get vaccinated, regardless of whether your work involved patients had to do.
According to information from several university employees, doctoral students, postdocs and researchers were soon lining up in the hospital auditorium. Almost everyone in a cancer research center affiliated with the hospital received the vaccine.
Hospital officials said that at some point they became aware of emails directing people to the auditorium, but that anyone who didn’t need the vaccine was turned away.
“We have worked to vaccinate tens of thousands of employees, starting with those with patient contact, and we are constantly striving to improve our vaccination process,” said Kate Spaziani, vice president of communications at the hospital.
She added, “We will do this until everyone gets a vaccine. We follow all guidelines from the New York State Department of Health on vaccine priority. “
However, some recipients were upset to learn that they did not qualify according to state guidelines.
“My understanding now is that it wasn’t our turn and I feel terrible if I get out of line,” said a young researcher whose work has no bearing on Covid-19. “I’m also honestly a little angry at the hospital and the university for not controlling it properly.”
At NYU’s Langone Medical Center, contact with non-patient staff was more conscious.
“We currently only offer the Covid-19 vaccine to frontline employees,” the center’s website says. “We will send a message to our patients as soon as we have the vaccine available for patients.”
In an email to staff on December 28, Dr. Anil Rustgi, Dean of the Faculties of Health Sciences and Medicine, said the center has completed vaccinating its 15,000 patient-interacting staff and will begin vaccinating all other staff. Elderly adults or other New York State priority groups were not mentioned.
An email sent Tuesday to NYU Medical Center employees who hadn’t yet signed up for a vaccination said, “As a health care worker, you have the opportunity to get a vaccine that millions across the country want – and You can have it: right now. “
In a tacit admission that these employees would not qualify for the vaccine anytime soon, the email warned that once the eligibility criteria are expanded, the state may have to wait weeks, if not months, to get it based on demand and Maintain availability. ”
State officials were dismayed that both NYU and Columbia had opened vaccinations for low-risk employees before millions of citizens needed the shots.
On Friday, New York expanded its guidelines on vaccination to include key workers and those over 75.
The guidelines “do not, however, provide a license to vaccinate all hospital staff regardless of their role,” said Gary Holmes, a spokesman for the state health department. “While we don’t know all the facts here, DOH will investigate if there is a violation.”
In private, some state officials were furious. Institutions should instead have asked the state what to do next once the immunization of frontline workers is complete, one official said on condition of anonymity as he was not empowered to discuss the matter.
“The only reason they have as much vaccine as they do is because they were vaccine administrators – because they have a cold store,” the official said. “It wasn’t NYU’s vaccine for NYU”
The problem is not limited to academic medical centers. Some hospitals have carried out so few checks that many people have been able to circumvent the line with false claims about the vaccines.
For example, in Maricopa County, Arizona, an online form recommends that applicants use a personal email address instead of one associated with a hospital, and not require employee identification numbers.
“Yes, we want people to be vaccinated, but we need to make sure the high-risk groups get access,” said Saskia Popescu, an epidemiologist at the University of Arizona Hospital. When the process is so disorganized, “trust in the process damages public health, and I think it’s just really heartbreaking.”
Some university employees, including some who unknowingly wrongly accepted the vaccine, were also dissatisfied with what they viewed as an unjust and unfair trial.
“It’s such a naked display of privilege, you know?” said a Columbia faculty member who failed to receive the vaccine and asked not to be identified for fear of retaliation by administrators. “It’s because we’re in elite universities and medical centers.”