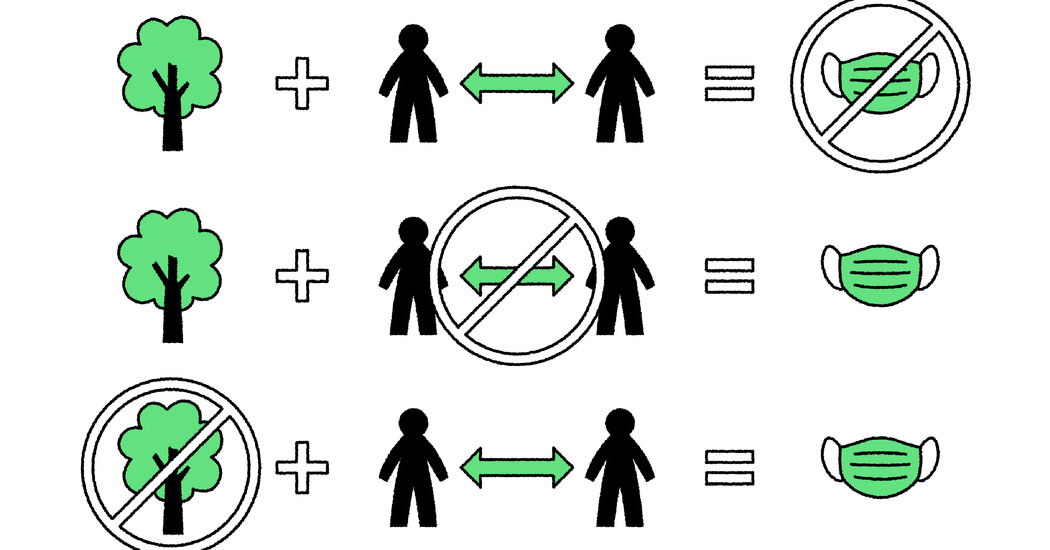
Since the delta variant is spreading among the unvaccinated, many fully vaccinated people also worry. Is it time to mask again?
While there is no one-size-fits-all answer to the question, most experts agree that masks remain a wise precaution in certain situations for both vaccinated and unvaccinated people. How often you use a mask depends on your personal health tolerance and risk, the infection and vaccination rates in your community, and who you spend time with.
The bottom line is this: while a full vaccination protects against serious illness and hospitalization from Covid-19, no vaccine offers 100 percent protection. As long as large numbers of people remain unvaccinated and the coronavirus continues to spread, those vaccinated will be exposed to the Delta variant and a small percentage of them will develop what are known as breakthrough infections. Here you will find answers to frequently asked questions about how to protect yourself and reduce your risk of a breakthrough infection.
When should a vaccinated person wear a mask?
To decide if a mask is needed, first ask yourself these questions.
-
Are the people I am with also vaccinated?
-
What is the fall and vaccination rate in my community?
-
Will I be in a poorly ventilated indoor or outdoor area? Will the increased risk of exposure last a few minutes or hours?
-
How high is my personal risk (or the risk to my fellow human beings) for complications from Covid-19?
Experts agree that you don’t need to wear a mask if everyone you are with is vaccinated and symptom-free.
“I don’t wear a mask when hanging out with other people who have been vaccinated,” said Dr. Ashish K. Jha, Dean of Brown University School of Public Health. “I don’t even think about it. I go to the office with a few people and they are all vaccinated. I’m not worried. “
But once you venture into closed public spaces, where the chances of encountering unvaccinated people are greater, a mask is probably a good idea. A full vaccination remains the strongest protection against Covid-19, but the risk is cumulative. The more opportunities you give the virus to challenge the antibodies you made with your vaccine, the higher your risk of exposure to exposure so great that the virus breaks the protective barrier of your immune system.
Because of this, your community’s fall and vaccination rate is one of the most important factors influencing mask needs. For example, in Vermont, Massachusetts, Connecticut, and Rhode Island, more than 70 percent of adults are fully vaccinated. In Alabama, Mississippi, and Arkansas, fewer than 45 percent of adults are vaccinated. In some counties, overall vaccination rates are far lower.
“We are currently two Covid nations,” said Dr. Peter Hotez, dean of the National School of Tropical Medicine at Baylor College of Medicine and co-director of the Center for Vaccine Development at Texas Children’s Hospital. In Harris County, Texas, where Dr. Hotez is alive, case numbers are up 114 percent in the past two weeks, and only 44 percent of the community is fully vaccinated. “I wear a mask indoors most of the time,” said Dr. Hotez.
Finally, masking is more important in poorly ventilated indoor spaces than outdoors, where the risk of infection is extremely low. Dr. Jah notices that he recently stormed into a cafe, exposed because vaccination rates are high in his area, and was only there for a few minutes.
Your personal risk also counts. If you are elderly or have immunocompromised your antibody response to the vaccine may not be as strong as a young person’s response. It is a good idea to avoid crowded rooms and wear a mask if you are indoors and do not know the vaccination status of those around you.
Use the Times tracker to find vaccination rates and case numbers in your area.
Why does the delta variant cause experts to rethink the mask guidance?
When the US Centers for Disease Control and Prevention announced that people who had been vaccinated could forego wearing masks, the number of cases declined, vaccinations increased, and the highly contagious Delta variant had not yet caught on. Since then, Delta has spread rapidly and now accounts for more than 83 percent of cases in the United States.
It is known that people infected with the Delta variant shed much higher amounts of the virus over longer periods of time compared to previous lines of the coronavirus. A preliminary study estimated that viral loads are 1,000 times higher in people with the delta variant. These high viral loads give the virus more opportunities to challenge your antibodies and breach your vaccine protection.
“This is twice as transferable as the original line from Covid,” said Dr. Hotez. “The reproductive number of the virus is around 6,” he said, referring to the number of people a virus carrier is likely to infect. “That means that 85 percent of the population must be vaccinated. Only a few areas of the country achieve that. “
Updated
July 22, 2021, 1:43 p.m. ET
Is it safe for people who have been vaccinated to go to restaurants, museums, cinemas, weddings, or other large gatherings?
The answer depends on your personal risk tolerance and the level of vaccinations and Covid-19 cases in your community. The more time you spend with unvaccinated people in closed rooms for a long time, the higher the risk of crossbreeding with the Delta variant or other variants that may appear.
Large gatherings, by definition, offer more opportunities to contract the coronavirus, even if you are vaccinated. Scientists have documented breakthrough infections at a recent Oklahoma wedding and July 4th celebrations in Provincetown, Massachusetts.
But even with the Delta variant, a full vaccination seems to be around 90 percent effective to prevent serious illnesses and hospital stays caused by Covid-19. However, if you are at a very high risk of complications from Covid-19, you should consider avoiding risky situations and wearing a mask if the vaccination status is unknown to those around you.
Healthy vaccinated people with a low risk of complications have to decide what personal risk they want to accept. Wearing a mask at large indoor gatherings will reduce the risk of infection. If you are healthy and vaccinated but are caring for an aging parent or spending time with others at high risk, you should also consider their risk when deciding whether to attend an event or wear a mask.
“When I go into a public area, I usually wear a mask,” said Dr. Hotez. “Until recently, I used to take my son and his girlfriend out to a restaurant for dinner and I wouldn’t wear a mask because the broadcast was so advanced. Now I’m not so sure. I can change the way I think about restaurants while Delta is getting faster. “
If breakthrough infections are rare, why keep hearing about them?
Breakthrough infections get a lot of attention because people who have been vaccinated talk about them on social media. If breakthrough infection clusters occur, it is also reported in science journals or in the media.
However, it’s important to remember that while breakthrough cases are relatively rare, they can still happen no matter what vaccine you’re given.
“No vaccine is 100 percent effective at preventing disease in vaccinated people,” says its CDC website. “There will be a small percentage of fully vaccinated people who will still get sick, hospitalized, or die of Covid-19.”
A breakthrough case doesn’t mean your vaccine isn’t working. In fact, most breakthrough infection cases result in no symptoms or only mild illness, which shows that the vaccines are working well to prevent serious illness from Covid-19.
As of July 12, more than 159 million people in the United States were fully vaccinated against Covid-19. Of these, only 5,492 had breakthrough cases that resulted in serious illness. including 1,063 who died. That’s less than 0.0007 percent of the vaccinated population. Now 99 percent of Covid-19 deaths are among the unvaccinated.
Many infectious disease experts are frustrated that the CDC only documents cases where a vaccinated person with Covid-19 is hospitalized or dies. But many breakthrough infections are still being discovered in asymptomatic people who are frequently tested, such as baseball players and Olympic athletes. Many of these people travel or spend long periods of time in close quarters with others.
“Sports figures are different,” said Dr. Yeh. “Part of the problem is that they also encounter a lot of unvaccinated people, even in their own small circle.”
I am vaccinated. How often should I be tested for Covid-19?
If you’re fully vaccinated and know you’ve been exposed to someone with Covid-19, it’s a good idea to get tested even if you don’t have symptoms.
And if you have cold symptoms or other signs of infection, experts agree that you should be tested. Many vaccinated people who do not wear masks have caught colds in the summer, which lead to runny nose, fever and cough. But it’s impossible to tell the difference between a summer cold and Covid-19. Anyone with cough or cold symptoms should wear a mask to protect their surroundings and get tested to rule out Covid-19. It’s a good idea to have a few Covid tests on hand at home as well.
“If I woke up one morning and had symptoms of a cold, I would put on a mask at home and get tested,” said Dr. Yeh. “I don’t want to cause breakthrough infections in other members of my family, and I don’t want to give it to my 9 year old child.”