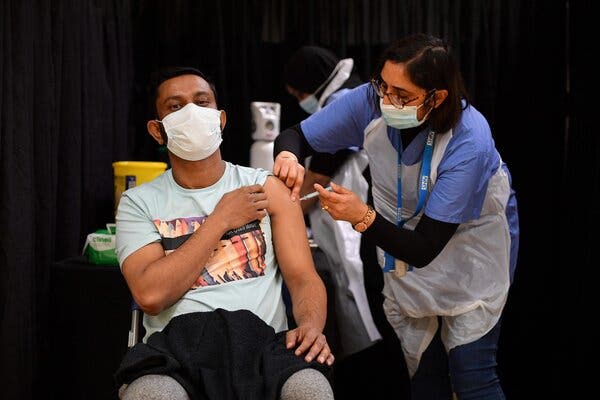
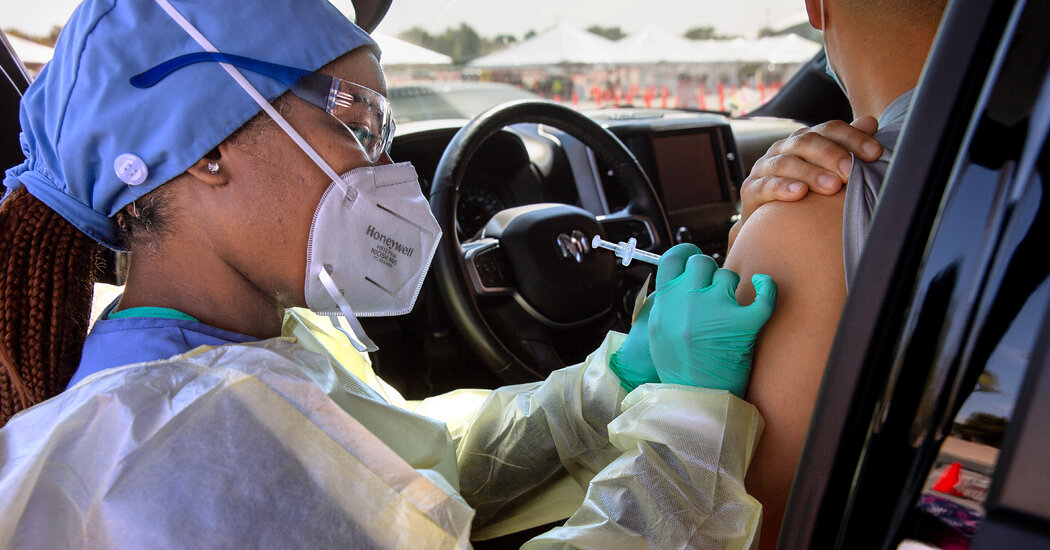
A vaccination center in London in April. The British authorities are considering reintroducing local lockdowns to stem the spread of a coronavirus variant first detected in India.Credit…Justin Tallis/Agence France-Presse — Getty Images
LONDON — Prime Minister Boris Johnson of Britain said on Friday that vaccination protocols would be changed to swiftly deliver second doses to people over 50-years-old to combat the spread of a coronavirus variant first detected in India, a warning sign for countries that are easing restrictions even though their own vaccination campaigns are incomplete.
“We believe this variant is more transmissible than the previous ones,” Mr. Johnson said. What remained unclear, he said, was by how much. The infectiousness of the variant first detected in India remains the subject of intense study and some leading experts have said it is too early to assess its transmissibility.
If it proves significantly more transmissible, he said, “we face some hard choices.” He added that there was no evidence that the variant was more likely to cause serious illness and death, and there was no evidence to suggest vaccines were less effective against the variant in preventing serious illness and death.
While he said the country would not delay plans to ease restrictions on Monday, he warned that the spread of the variant could force the government to change course.
“This new variant could pose a serious disruption to our progress,” he said at a news conference on Friday.
The numbers of cases involving the variant, known as B.1.617, rose from 520 last week to 1,313 cases this week in Britain, according to official statistics.
The extent to which the variant has spread globally is unclear, because most countries lack the genomic surveillance capabilities employed in England.
That surveillance capability has allowed health officials in Britain to spot the rise of concerning variants more quickly than other nations, offering an early warning system of sorts as a variant seen in one nation almost invariably pops up in others.
Most cases detected in Britain are in northwestern England. The focus has been on Bolton, a town of nearly 200,000 that has one of the country’s highest rates of infection and where health officials have warned of widespread community transmission of the B.1.617 variant. Some cases have also been reported in London. The rapid spread of the variant has led officials to debate speeding up dosing schedules and opening up access to shots in hot spots to younger age groups.
National restrictions in England are scheduled to be eased on Monday, with indoor dining and entertainment returning, before a full reopening in June. But officials have cautioned that those plans might be in danger.
In Scotland, First Minister Nicola Sturgeon said on Friday that plans to ease restrictions in Glasgow would be delayed at least a week out of concern about an uptick in cases that officials said may be being driven by the variant.
Much is unknown about the new variant, but scientists fear it may have driven the rise of cases in India and could fuel outbreaks in neighboring countries.
Dr. Maria Van Kerkhove, the technical lead of the World Health Organization’s coronavirus response, said a study of a limited number of patients, which had not yet been peer-reviewed, suggested that antibodies from vaccines or infections with other variants might not be quite as effective against B.1.617. The agency said, however, that vaccines were likely to remain potent enough to provide protection from serious illness and death.
British officials have said the variant appears to be more contagious than the B.1.1.7 variant, which was detected last year in Kent, southeast of London and swept across Britain in the winter, forcing the country into one of the world’s longest national lockdowns. The B.1.1.7 variant has now been found in countries around the world.
In the United States, the B.1.1.7 variant did become the predominant version of the virus, now accounting for nearly three-quarters of all cases. But the U.S. surge experts had feared ended up a mere blip in most of the country. The nationwide total of daily new cases began falling in April and has now dropped more than 85 percent from the horrific highs of January.
The B.1.617 variant has been found in virus samples from 44 countries and was designated a variant of concern by the W.H.O. this week, which means there is some evidence that it could have an impact on diagnostics, treatments or vaccines and needs to be closely monitored.
Christina Pagel, a member of a group of scientists advising the government, known as SAGE, said postponing next week’s reopening would avoid “risking more uncertainty, more damaging closures and longer recovery from a worse situation.”
“We need to learn from previous experience,” Dr. Pagel, the director of the Clinical Operational Research Unit at University College London, said on Twitter.
Britain briefly reopened its economy at the end of last year, only to abruptly impose new restrictions that remained in place for months as it fought a deadly wave of infections.
In an attempt to offer at least partial protection to as many people as quickly as possible, Britain spaced injections between doses for two-stage coronavirus vaccines up to 12 weeks after the first vaccines were approved in December. That was far longer than the three- or four-week interval employed by most other countries.
Mr. Johnson said that those older than 50 will now be able to get second doses after eight weeks.
“It is more important than ever that people get the additional protection of a second dose,” he said.
The speedy rollout saved at least 11,700 lives and prevented 33,000 people from becoming seriously ill in England, according to research released by Public Health England on Friday.
Infections, serious illness and deaths have plummeted across Britain. Only 17 deaths were reported on Friday.
But the vaccination campaign has slowed down since last month because of supply shortages and the need to start distributing second doses. The number of daily first doses on average last month was 113,000, far below the average of 350,000 daily doses administered in March.
Only those over 38-years-old are currently eligible for vaccination.
It remains unclear whether the country has the vaccine supplies on hand to move rapidly to surge more into communities around the country to speed up vaccinating younger age groups.
Correction: May 14, 2021
An earlier version of this item misstated the affiliation of Christina Pagel, a science adviser. Ms. Pagel is a member of Independent SAGE, a group of expert advisers unaffiliated with the government. She is not a member of SAGE, a panel of government advisers.
| United States › |
United StatesOn May 14 |
14-day change |
| New cases |
41,044 |
–32% |
|
| New deaths |
732 |
–12% |
|
| World › |
WorldOn May 14 |
14-day change |
| New cases |
41,044 |
–24% |
|
| New deaths |
732 |
–18% |
|
U.S. vaccinations ›

 A tour group in Manhattan the day after the federal guidance changed mask guidance for vaccinated people. New York said Thursday it was reviewing the recommendations.Credit…Benjamin Norman for The New York Times
A tour group in Manhattan the day after the federal guidance changed mask guidance for vaccinated people. New York said Thursday it was reviewing the recommendations.Credit…Benjamin Norman for The New York Times
Minnesota’s statewide mask mandate is over. But in Minneapolis, the state’s largest city, face coverings are still required.
In Michigan, Kentucky and Oregon, governors cheerily told vaccinated people that they could go out maskless. But mask mandates remained in force for New Yorkers, New Jerseyans and Californians.
So unexpected was new federal guidance on masks that in Kansas City, Mo., Mayor Quinton Lucas went from saying he would not change his mask order, to saying he would think about it, to announcing that he was getting rid of it altogether, all in the span of about seven hours.
Across the country, governors, store owners and people running errands were scrambling on Friday to make sense of the abrupt change in federal guidelines, which said fully vaccinated people could now safely go most places, indoors or outdoors, without a mask.
At least 20 states that still had mask mandates in place this week said by Friday evening that they would exempt fully vaccinated people or repeal the orders entirely, while at least five others with mask requirements had not announced any changes. The rapidly changing rules brought an end to more than a year of mandatory masking in much of the country, even as some said they were not yet ready to take off their face coverings.
“I’m going to wear a mask for a long time to come,” said Fanny Lopez, 28, who was grocery shopping in San Antonio on Friday morning while wearing a black cloth mask. “I trust the mask more than the vaccine. The government messages are confusing, telling us to wear a mask one day and the next day no.”
The sudden shift in public health advice resonated at every level of government, from City Hall in Hartsville, S.C., where a local mask mandate was allowed to expire, to Nevada’s Gaming Control Board, which said it was not practical “to attempt to enforce a mask mandate tethered to an individual’s vaccination status,” to the U.S. Capitol, where the attending physician said House members would still have to cover their faces on the floor of the chamber.
But the shift was perhaps most challenging for governors and big-city mayors, many of whom have expended significant political capital on mask orders in the face of protests and lawsuits, and who were not given a heads-up about the change in federal policy before it was announced on Thursday.
Mayor Lucas said he could not keep Kansas City’s order in place since there was no easy way to differentiate people who are fully vaccinated — now 36 percent of Americans — from the 64 percent who are not.
“While I understand the C.D.C.’s theory that they could just create a rule that says vaccinated folks go anywhere without a mask, and everybody else who’s unvaccinated will follow it, I don’t know if that’s the type of rule that was written in coordination with anyone who has been a governor or a mayor over the last 14 months,” said Mr. Lucas, a Democrat.
The new guidance from the Centers for Disease Control and Prevention, which came amid a steep drop in new cases and an expansion of vaccine eligibility to everyone 12 and older, signaled a shift toward pre-pandemic social norms, when no one thought twice about buying groceries or sitting down in their cubicle with a bare mouth and nose. Walmart announced on Friday that fully vaccinated employees and customers would no longer need to wear masks, and Costco issued a similar announcement.
“At least 20 times today I kept grabbing my short pockets looking for my face mask,” said Erik Darmstetter, who is fully vaccinated and owns Office Furniture Liquidations in San Antonio. “It wasn’t there. I keep forgetting we don’t need it anymore.”
Others were moving more slowly. Gov. Phil Murphy of New Jersey, a Democrat, said he would keep his state’s mask mandate in place, writing on Twitter that “we’re making incredible progress, but we’re not there yet.” And Gov. Charlie Baker of Massachusetts, a Republican, indicated he would revisit his state’s rules next week, but he did not announce any immediate changes.
When asked on Friday about how the C.D.C.’s guidelines would affect Mr. Biden’s executive order requiring masks on federal property, Jen Psaki, the White House press secretary, said at a news conference that it “may take a couple of days” to adopt the agency’s advice. She added that there are no plans to change the federal order mandating masks on public transportation.
On the question of possible vaccine passports, Ms. Psaki said the administration was prioritizing remained focused on the vaccination campaign, and that the administration was “not currently considering federal mandates,” and did not have plans to change its approach.
“We also understand that private sector companies may decide that they want to have requirements. That’s up to them to make that determination,” she said.
 Administering a coronavirus shot during a vaccination day for homeless people in Montevideo, Uruguay, on Thursday.Credit…Raul Martinez/EPA, via Shutterstock
Administering a coronavirus shot during a vaccination day for homeless people in Montevideo, Uruguay, on Thursday.Credit…Raul Martinez/EPA, via Shutterstock
BUENOS AIRES — For most of the past year, Uruguay was held up as an example for keeping the coronavirus from spreading widely as neighboring countries grappled with soaring death tolls.
Uruguay’s good fortune has run out. In the last week, the small South American nation’s Covid-19 death rate per capita was the highest in the world, according to data compiled by The New York Times.
As of Wednesday, at least 3,252 people had died from Covid-19, according to the Uruguayan Health Ministry, and the daily death toll has been about 50 during the past week.
Six out of the 11 countries with the highest death rates per capita are in South America, a region where the pandemic is leaving a brutal toll of growing joblessness, poverty and hunger. For the most part, countries in the region have failed to acquire sufficient vaccines to inoculate their populations quickly.
Contagion rates in Uruguay began inching up in November and soared in recent months, apparently fueled by a highly contagious variant first identified in Brazil last year.
“In Uruguay, it’s as if we had two pandemics, one until November 2020, when things were largely under control, and the other starting in November, with the arrival of the first wave to the country,” said José Luis Satdjian, the deputy secretary of the Health Ministry.
The country with the second-highest death rate per capita is nearby Paraguay, which also had relative success in containing the virus for much of last year but now finds itself in a worsening crisis.
Experts link the sharp rise in cases in Uruguay to the P.1 virus variant detected in Brazil.
“We have a new player in the system and it’s the Brazilian variant, which has penetrated our country so aggressively,” Mr. Satdjian said.
Uruguay closed its borders tightly at the beginning of the pandemic, but towns along the border with Brazil are effectively binational and have remained porous.
The outbreak has strained hospitals in Uruguay, which has a population of 3.5 million.
On March 1, Uruguay had 76 Covid-19 patients in intensive care units. This week, medical professionals were caring for more than 530, according to Dr. Julio Pontet, president of the Uruguayan Society of Intensive Care Medicine who heads the intensive care department at the Pasteur Hospital in Montevideo, the capital.
That number is slightly lower than the peak in early May, but experts have yet to see a steady decline that could indicate a trend.
“It is still too early to reach the conclusion that we’ve already started to improve, we’re in a high plateau of cases,” Dr. Pontet said.
Despite the continuing high number of cases, there is optimism that the country will be able to get the situation under control soon because it is one of the few in the region that has been able to make quick progress on its vaccination campaign. About a quarter of the population has been fully immunized.
“We expect the number of serious cases to begin decreasing at the end of May,” Dr. Pontet said.
 A man in Los Angeles being vaccinated in March. The C.D.C. released a study on Friday providing more evidence that the vaccines are working well in real world settings.Credit…Allison Zaucha for The New York Times
A man in Los Angeles being vaccinated in March. The C.D.C. released a study on Friday providing more evidence that the vaccines are working well in real world settings.Credit…Allison Zaucha for The New York Times
The Pfizer-BioNTech and Moderna coronavirus vaccines are 94 percent effective at preventing symptomatic Covid-19 illness, according to a new study of more than 1,800 health care workers in the United States.
The research, which the Centers for Disease Control and Prevention released on Friday, provides yet more evidence that the vaccines are working well even outside controlled clinical trials.
“This report provided the most compelling information to date that Covid-19 vaccines were performing as expected in the real world,” Dr. Rochelle Walensky, the C.D.C. director, said in a statement on Friday.
“This study, added to the many studies that preceded it, was pivotal to C.D.C. changing its recommendations for those who are fully vaccinated against Covid-19.”
The findings are based on an ongoing study of health care workers in 25 states. This interim analysis included data on 1,843 health care workers who were routinely tested for infection with the coronavirus. More than 80 percent of participants were female.
Some 623 workers tested positive between January and mid-March. Those who were fully vaccinated were 94 percent less likely to develop symptomatic coronavirus infections than their unvaccinated peers, the researchers found. The figures are consistent with the efficacy estimates from the clinical trials.
The scientists also found that a single dose of the two-shot regimen was 82 percent effective at preventing symptomatic infection. That figure is higher than has been reported in other studies and may be a result of the relative youth of the study participants, who had a median age of 37 to 38. Fewer than 2 percent were 65 or older.
C.D.C. scientists had previously found that fully vaccinated health care, frontline and essential workers were 90 percent less likely to contract the coronavirus. Those findings helped allay fears that vaccinated people might still be likely to carry the virus, even asymptomatically, and spread it to others.
The concern was one of the main rationales for asking vaccinated Americans to continue to wear masks, a recommendation that the C.D.C. lifted on Thursday.
 Maj. Gen. Dany Fortin, right, with Prime Minister Justin Trudeau of Canada in Ottawa in December.Credit…Sean Kilpatrick/The Canadian Press, via Associated Press
Maj. Gen. Dany Fortin, right, with Prime Minister Justin Trudeau of Canada in Ottawa in December.Credit…Sean Kilpatrick/The Canadian Press, via Associated Press
The senior military commander who was appointed by Prime Minister Justin Trudeau of Canada last fall to oversee the distribution of Covid-19 vaccines in the country has quit that post and is now the subject of a military investigation, officials said late Friday.
In a brief, joint statement, the Department of National Defense and the Canadian Armed Forces announced Maj. Gen. Dany Fortin’s resignation but offered no details about the nature of the investigation. The department declined to comment.
Before General Fortin became Canada’s vaccine coordinator, he led military missions to help workers in long-term care homes that were overwhelmed by Covid infections. He is a former commander of the NATO mission in Iraq.
General Fortin is now the third senior leader in the Canadian Armed Forces under scrutiny. Adm. Art McDonald stepped aside as chief of the defense staff, the country’s top military job, in February after the military police opened an investigation into unspecified accusations against him. The same month, the military police also began investigating the previous chief of the defense staff, Gen. Jonathan Vance, who held the post until his retirement from the army in January.
General Vance has been accused publicly of inappropriate behavior toward female subordinates. He has denied wrongdoing.
 Coronavirus test samples being readied for processing and eventual genomic sequencing at Duke University.Credit…Pete Kiehart for The New York Times
Coronavirus test samples being readied for processing and eventual genomic sequencing at Duke University.Credit…Pete Kiehart for The New York Times
On Dec. 29, a National Guardsman in Colorado became the first known case in the United States of a contagious new variant of the coronavirus.
The variant, called B.1.1.7, had roiled Britain, was beginning to surge in Europe and threatened to do the same in the United States. And although scientists didn’t know it yet, other mutants were also cropping up around the country. They included variants that had devastated South Africa and Brazil and that seemed to be able to sidestep the immune system, as well as others homegrown in California, Oregon and New York.
This mélange of variants could not have come at a worse time. The nation was at the start of a post-holiday surge of cases that would dwarf all previous waves. And the distribution of powerful vaccines made by Moderna and Pfizer-BioNTech was botched by chaos and miscommunication. Scientists warned that the variants — and B.1.1.7 in particular — might lead to a fourth wave, and that the already strained health care system might buckle.
That didn’t happen. B.1.1.7 did become the predominant version of the virus in the United States, now accounting for nearly three-quarters of all cases. But the surge experts had feared ended up a mere blip in most of the country. The nationwide total of daily new cases began falling in April and has now dropped more than 85 percent from the horrific highs of January.
Experts still see variants as a potential source of trouble in the months to come — particularly one that has battered Brazil and is growing rapidly in 17 U.S. states. But they are also taking stock of the past few months to better understand how the nation dodged the variant threat.
They point to a combination of factors — masks, social distancing and other restrictions, and perhaps a seasonal wane of infections — that bought crucial time for tens of millions of Americans to get vaccinated. They also credit a good dose of serendipity, as B.1.1.7, unlike some of its competitors, is powerless against the vaccines.
 At a bookstore in San Francisco in March. Until the pandemic, there had seldom been a cultural push for mask wearing in the United States.Credit…Jim Wilson/The New York Times
At a bookstore in San Francisco in March. Until the pandemic, there had seldom been a cultural push for mask wearing in the United States.Credit…Jim Wilson/The New York Times
Once Americans return to crowded offices, schools, buses and trains, so too will their sneezes and sniffles.
Having been introduced to the idea of wearing masks to protect themselves and others, some Americans are now considering a behavior scarcely seen in the United States but long a fixture in other cultures: routinely wearing a mask when displaying symptoms of a common cold or the flu, even in a future in which Covid-19 isn’t a primary concern.
Such routine use of masks has been common for decades in other countries, primarily in East Asia, as protection against allergies or pollution, or as a common courtesy to protect nearby people.
Leading American health officials have been divided over the benefits, partly because there is no tidy scientific consensus on the effect of masks on influenza virus transmission, according to experts who have studied it.
Nancy Leung, an epidemiologist at the University of Hong Kong, said that the science exploring possible links between masking and the emission or transmission of influenza viruses was nuanced — and that the nuances were often lost on the general public.
 Changi Airport in Singapore this week. The airport outbreak began with an 88-year-old member of the airport cleaning crew who was fully vaccinated but who tested positive for the virus on May 5.Credit…Wallace Woon/EPA, via Shutterstock
Changi Airport in Singapore this week. The airport outbreak began with an 88-year-old member of the airport cleaning crew who was fully vaccinated but who tested positive for the virus on May 5.Credit…Wallace Woon/EPA, via Shutterstock
SINGAPORE — Singapore said on Friday that it would ban dining in restaurants and gatherings of more than two people to try to stem a rise in coronavirus cases, becoming the latest Asian nation to reintroduce restrictions after keeping the illness mostly in check for months.
The new measures came after the city-state recorded 34 new cases on Thursday, a small number by global standards, but part of a rise in infections traced to vaccinated workers at Singapore Changi Airport.
The airport outbreak began with an 88-year-old member of the airport cleaning crew who was fully vaccinated but who tested positive for the virus on May 5. Co-workers who then became infected later visited an airport food court, where they transmitted the virus to other customers, officials said.
None of the cases linked to the airport outbreak are believed to have resulted in critical illness or death, according to officials.
In all, 46 cases have been traced to the airport, the largest of about 10 clusters of new infections in the country.
“Because we do not know how far the transmission has occurred into the community, we do have to take further, more stringent restrictions,” said Lawrence Wong, co-chair of Singapore’s coronavirus task force. The measures will be in effect for about one month beginning on Sunday.
According to preliminary testing, many of those infected were working in a zone of the airport that received flights from high-risk countries, including from South Asia. Several have tested positive for the B.1.617 variant first detected in India, which the World Health Organization has said might be more contagious than most versions of the coronavirus.
Singapore health officials said that of 28 airport workers who became infected, 19 were fully vaccinated with either the Pfizer or Moderna vaccines, the only two approved for use in Singapore.
“Unfortunately, this mutant virus, very virulent, broke through the layers of defense,” Transport Minister Ong Ye Kung told a virtual news conference on Friday.
Mr. Ong also said that the rise in cases “very likely” means that a long-delayed air travel bubble with Hong Kong would not begin as scheduled on May 26.
Singapore, a prosperous island hub of 5.7 million people, saw an explosion of infections among migrant workers living in dormitories, but a two-month lockdown and extensive testing and contact tracing contained the outbreak. Although Singapore has kept much of its economy open, its vaccination effort has not moved as quickly as many expected: less than one-quarter of the population has been fully inoculated.
Changi Airport, which served more than 68 million passengers in 2019, is operating at 3 percent of capacity as Singapore has paused nearly all incoming commercial traffic. Employees there work under strict controls, wearing protective gear and submitting to regular coronavirus tests.
Singapore joins Japan, Thailand and other Asian countries that have struggled to contain new outbreaks fueled in part by variants. But Paul Ananth Tambyah, president of the Asia Pacific Society of Clinical Microbiology and Infection, said that the rise in cases was not overly worrying.
“The reason for my optimism is that we now have effective vaccines, better diagnostics, proven treatments and even potential prophylactic agents,” he said. “If these are employed in a targeted approach, it is unlikely that we will end up with the same problems we had last year.”
 Workers moved oxygen cylinders for transport at a factory in New Delhi on Sunday. The city has now received enough oxygen to share its supply.Credit…Atul Loke for The New York Times
Workers moved oxygen cylinders for transport at a factory in New Delhi on Sunday. The city has now received enough oxygen to share its supply.Credit…Atul Loke for The New York Times
After shortages in oxygen in New Delhi led to scores of people dying in hospitals, officials said there was now enough supply in the Indian capital to start sharing a surplus of the lifesaving gas to needier parts of the country.
For weeks, the New Delhi government appealed to Prime Minister Narendra Modi for a larger share of India’s oxygen reserves, with the battle for air ending up in the nation’s highest court.
On Thursday, just days after receiving the amount it had requested, New Delhi’s second-highest official, Manish Sisodia, said the city’s demand had fallen and its excess supply should be reallocated.
“The number of cases is coming down, hospital bed occupancy is coming down, and demand for oxygen, too, is down,” Mr. Sisodia told The New York Times.
It was an indication that the crisis in the capital might be reaching a peak.
The oxygen shortage in New Delhi began in April and has been linked to dozens of deaths, in and out of hospitals.
Health care facilities and crematories were overwhelmed, and medical professionals and residents were left scrambling for scarce resources.
Thousands of people in the city of 20 million stood in line at oxygen refilling stations, bringing cylinders into hospitals for friends and family or hoarding them at home in case the need arose.
The rise of new coronavirus infections in India has slowed. But, in pattern seen in nation after nation battered by the virus, death rates often plateau a few weeks later. And with the virus spreading in low-income rural areas, the overall crisis shows no sign of abating.
As of Wednesday, the official death toll surpassed 258,000, although experts suspect the true number to be much higher.
As the smoke from New Delhi crematories starts to clear, dozens of bodies have surfaced along the holy Ganges River in the states of Uttar Pradesh and Bihar.
Krishna Dutt Mishra, an ambulance driver in the Bihari village of Chausa, said that poor people were disposing of bodies in the river because the cost of cremations had become prohibitively expensive.
On Friday, the Indian news media showed bodies wrapped in cloth of the saffron color, considered auspicious in Hinduism, buried in shallow graves on the sandy banks of the Ganges River in the Unnao district of Uttar Pradesh.
Priyanka Gandhi, a leader of the opposition Indian National Congress party, called for a High Court investigation, saying that what was happening in Uttar Pradesh was “inhuman and criminal.”
 A woman from the Guatemalan Maya community in Lake Worth, Fla., at a Covid vaccine center last month.Credit…Saul Martinez for The New York Times
A woman from the Guatemalan Maya community in Lake Worth, Fla., at a Covid vaccine center last month.Credit…Saul Martinez for The New York Times
Latino adults in the United States have the lowest rates of Covid-19 vaccination, but among the unvaccinated they are the demographic group most willing to receive the Covid shots as soon as possible, a new survey shows.
The findings suggest that their depressed vaccination rate reflects in large measure misinformation about cost and access, as well as concerns about employment and immigration issues, according to the latest edition of the Kaiser Family Foundation Covid-19 Vaccine Monitor.
Earlier polls had suggested that skepticism about the vaccine was widespread among Latinos, but the latest survey showed that hesitation is declining.
Nearly 40 percent of all the unvaccinated Latinos responding to the survey said they feared they would need to produce government-issued identification to qualify. And about a third said they were afraid that getting the shot would jeopardize either their immigration status or that of a family member.
Their responses also pointed to the importance of community-based access. Nearly half said they would be more likely to be vaccinated if the shots were available at sites where they normally go for health care.
 A protest in Utah last year. Some readers expressed hope that the rule change would prompt people to get vaccinated but others worried about “cheaters.”Credit…Rick Bowmer/Associated Press
A protest in Utah last year. Some readers expressed hope that the rule change would prompt people to get vaccinated but others worried about “cheaters.”Credit…Rick Bowmer/Associated Press
Throughout the pandemic, few topics have touched so raw a nerve in the United States as mask wearing. Confrontations have erupted from state capitols to supermarket checkout aisles, and debates raged over whether mask mandates violate First Amendment rights.
The Centers for Disease Control and Prevention provoked a flood of reaction with its announcement on Thursday that Americans who are fully vaccinated may stop wearing masks or maintaining social distance in most indoor and outdoor settings. Here’s a sampling, edited for length and clarity, of how Times readers reacted to the news on Facebook and on our website:
“I think this is a good incentive for the hesitators. Hopefully they’ll want to participate in activities (the ones that require proof of vaccination) maskless, so perhaps this will be an incentive, as they see others in the community enjoying life more.” writes Jerry B., on Facebook.
“Very, very few people have been wearing masks for the past 6 months. Covid is a real risk — I certainly don’t want it — but our cases have dropped precipitously, even with minimal masking. This announcement is welcome — the world will not end if people stop masking,” writes Stephen from Oklahoma City.
“I see the need for this policy change, but I fear that the cheaters — those who are not vaccinated but pretend to be — will be the ruin of us all,” writes Cary in Oregon.
“I have my doubts about the incentivization bit,” writes Andrew from Colorado Springs, Colo. “I figure it will simply mean that suddenly everyone’s been fully vaccinated, true or not. That said, as a double-shotted person, I figure my chances of being taken out by an anti-vaxxer are now less than my chances of being taken out by a texting driver. I’m down with that.”
“What’s to stop anti-masker/anti-vaxxer contrarians from mingling unmasked with the vaccinated population? I have little trust in this,” writes Mary Beth in Santa Fe, N.M.
“I am fully vaccinated and caught Covid anyway. I do think it made my symptoms more mild, but you can bet your bippy I’m going to be wearing my mask when I am out of quarantine.” — writes Jaime P., on Facebook.
What do you think about the guidance? Join the conversation.
Kevin Hayes contributed research.