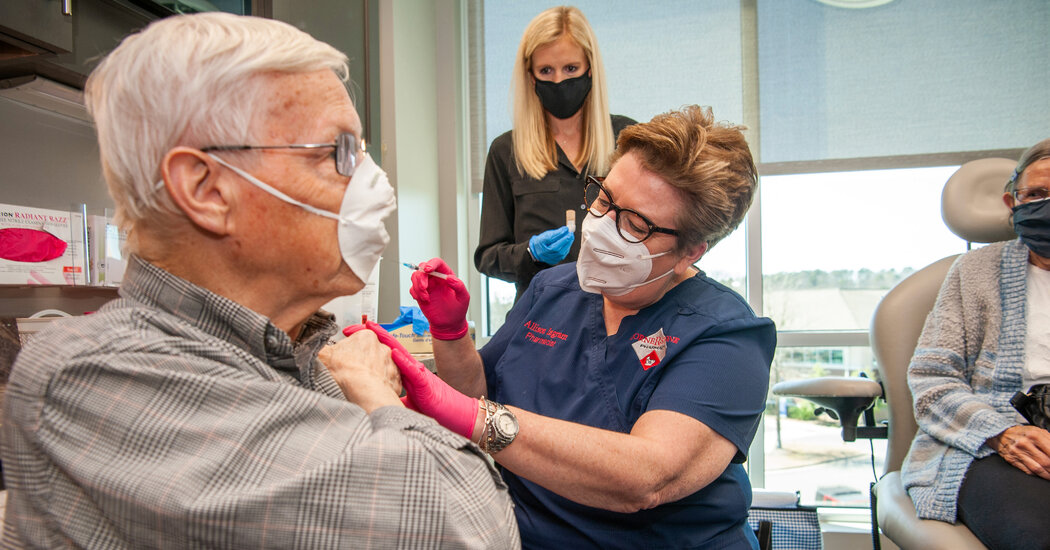
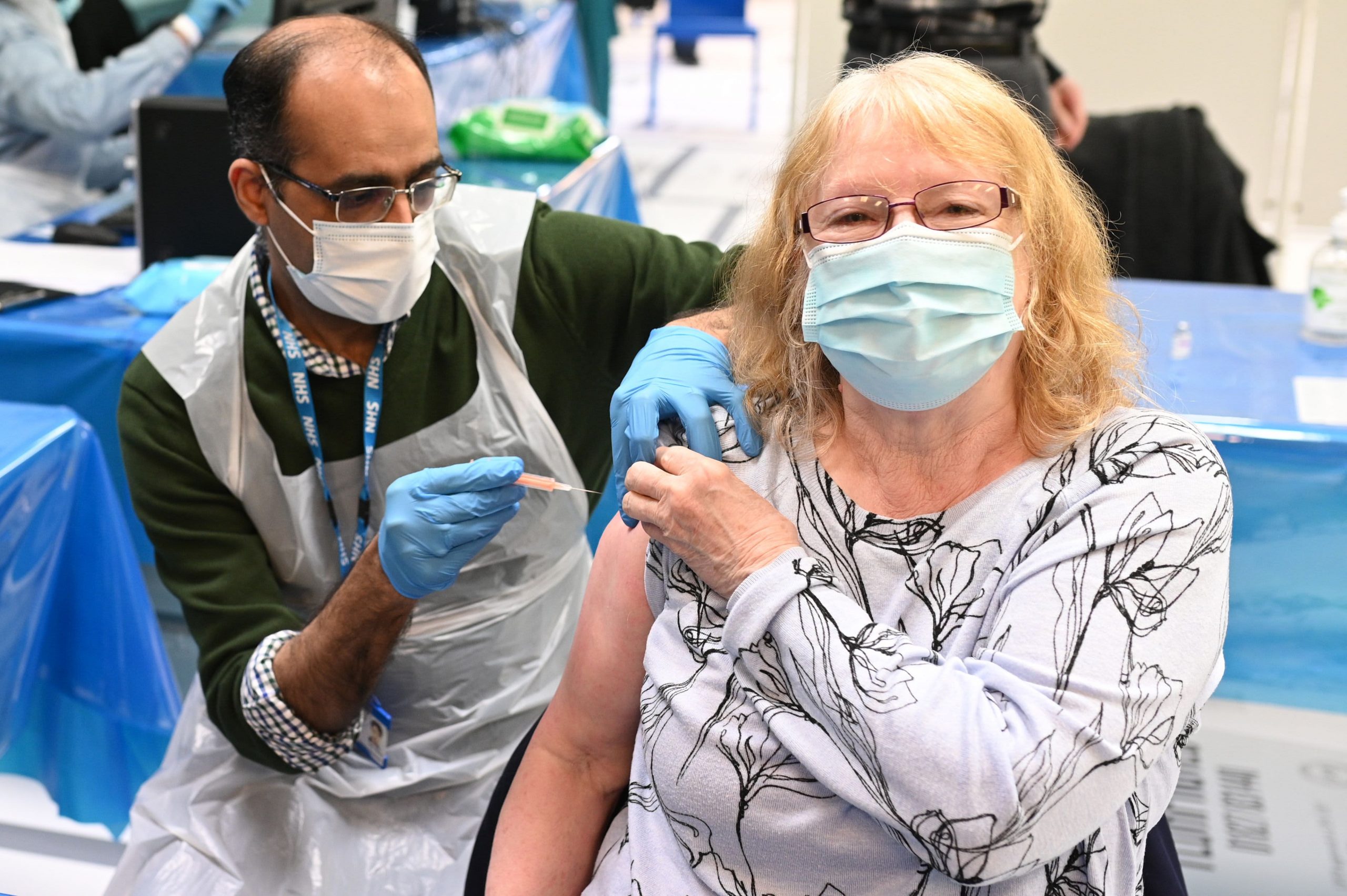
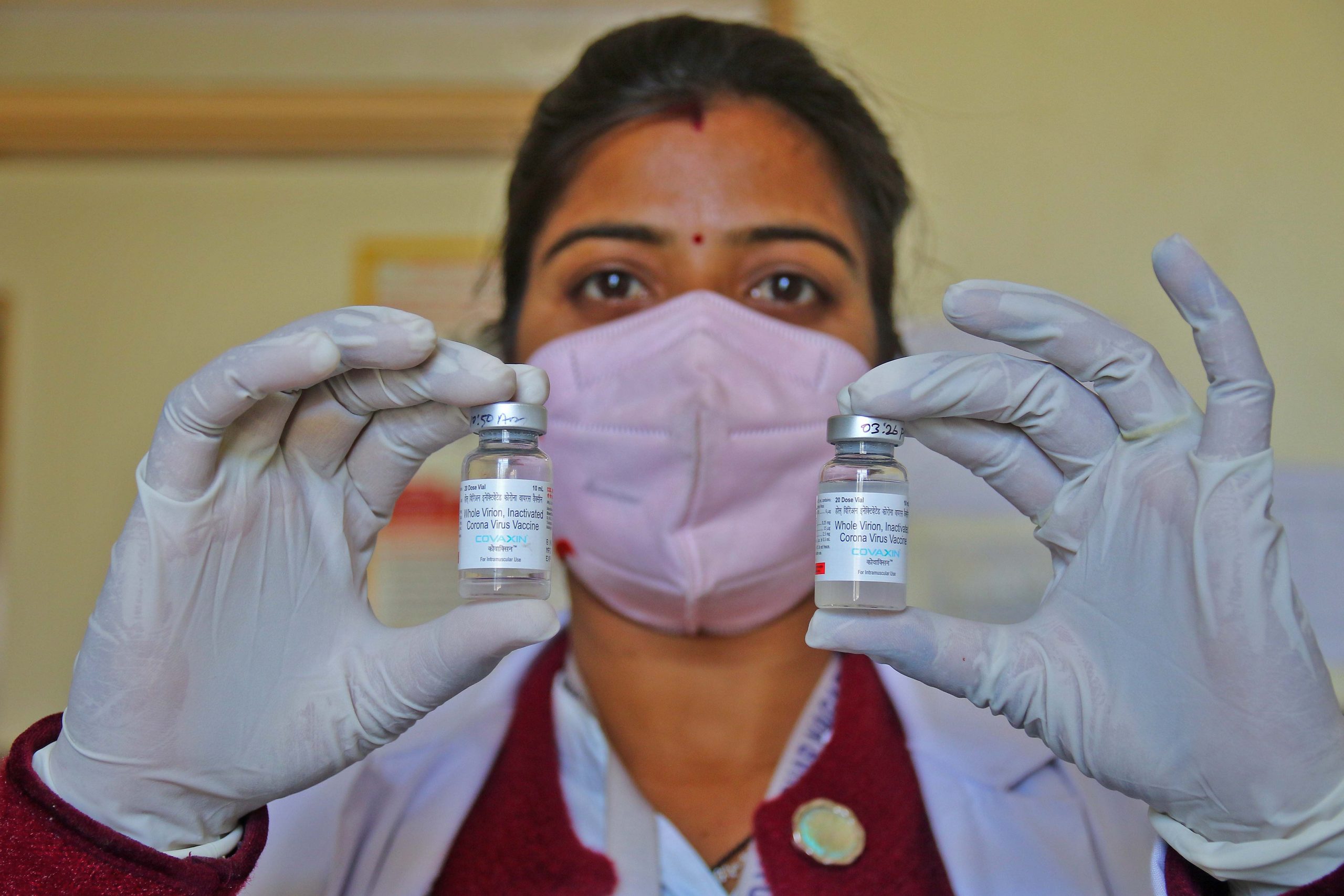
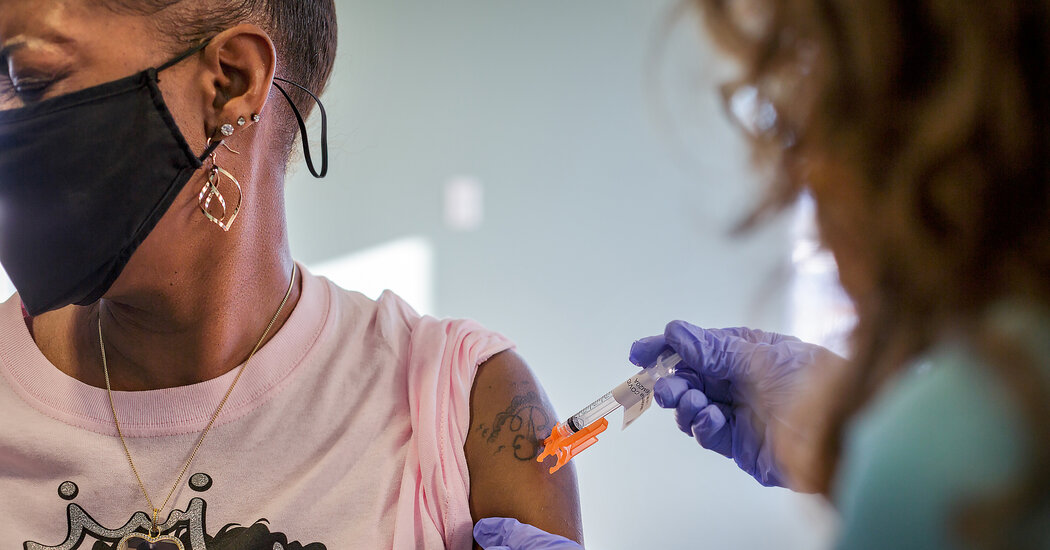In the rush of getting an elusive vaccine appointment, the leftover dose has become the stuff of the pandemic.
Additional footage to be used within hours of leaving the cold store has been distributed to drugstore customers buying midnight snacks, people who are nurse friends, and people who show up at certain grocery stores and pharmacies at closing time. At some major vaccination sites, the race to use each dose triggers a series of phone calls at the end of the day.
In either case, if the remaining dose cannot find an available arm, it must go to the trash.
Now a New York-based start-up wants to put the rush for leftover cans in order. Dr. B, as the company is called, compares vaccine providers who are receiving additional vaccines with people who are willing to receive them right away.
Since the service began last month, more than 500,000 people have submitted a variety of personal information to sign up for the service, which is free and free for providers too. Two vaccination centers have started testing the program, and the company said about 200 other providers had applied to participate.
Dr. B is just an attempt to coordinate the chaotic patchwork of public and private websites that allow eligible people to find vaccine appointments. Critics said the current system is confusing, unreliable, and often requires access to the Internet and time to search for websites for the infrequent appointment. In many places, people who are not yet eligible for a shot are also largely ignored, missing the opportunity to put them on a formal waiting list.
While Dr. B does not solve all of these broader problems, if it increases the hope that it will, it could serve as a model for better and fairer vaccination planning.
“I think this is a great idea,” said Sharon Whisenand, the administrator for the Randolph County’s Department of Health in rural Missouri.
Ms. Whisenand said 60 to 80 people did not show up for the county’s first mass vaccination event in late January, prompting her staff to make dozens of calls to people on a waiting list at the end of the day. “We sounded a bit like a call center,” she said. The workers eventually found enough buyers to give most of the extra doses, but some shots were thrown away.
Dr. B is a not-for-profit organization founded as a not-for-profit company whose mission is to ensure the efficient and fair distribution of vaccines. But its founder, Cyrus Massoumi, a tech entrepreneur, took Dr. B not yet described. He said he is funding the project out of pocket and has no plans to generate any income. The company is named after his grandfather, nicknamed Dr. Bubba wore and became a doctor during the 1918 pandemic influenza.
Mr. Massoumi is the founder and former CEO of ZocDoc, which helps patients find available doctor appointments, and the founder of Shadow, a company that uses technology and on-site volunteers to bring lost pets together with their owners. Like these two efforts, Dr. B, to make connections between groups who need something from each other.
“Ultimately, patients need this vaccine, and there are providers who need help getting it to the priority people,” Massoumi said in an interview. “That’s my motivation.”
After Mr Massoumi came up with the idea for Dr. B, he recruited several engineers from Haven, a now-defunct healthcare collaboration between Amazon, Berkshire Hathaway and JP Morgan, to build the website and underlying database. Amazon has also donated web services, Massoumi said.
The half a million people who signed up for the service entered basic biographical information such as date of birth, address, underlying health conditions, and the type of work they did. When vaccine providers near you receive additional doses, they will be notified by SMS and have 15 minutes to respond. Then they have to be ready to travel quickly to the vaccination site.
The company’s database sorts people according to local vaccine priority rules, so providers have a better chance of delivering their leftover shots to those most in need.
For many vendors, this proper practice would be a welcome change from the random systems they currently use. At some pharmacies and supermarket chains, workers have combed the aisles to find people ready to get vaccinated at the last minute. Elsewhere, vaccine hopefuls wait in line at the end of each shift, which could pose a risk of infection, especially for the most vulnerable.
Despite some grumbling about younger, healthier people skipping the line by snapping leftover cans, public health experts and many ethicists say the most important thing is that the vaccines don’t go to waste. At the start of the vaccine rollout, some politicians like New York Governor Andrew M. Cuomo threatened sanctions against providers for failing to follow the priority rules exactly, and a doctor in Texas lost his job after giving leaked doses to people with illness including his wife.
For those offered a last minute vaccine, “that person shouldn’t say no because they want it to go to someone else,” said Dr. Shikha Jain, assistant professor of medicine at the University of Illinois, Chicago, and a contributor -founder of IMPACT, a group that worked to improve the fair distribution of vaccines. “However, it’s really important to be deliberate and fair,” she said.
Mr Massoumi said he took several steps to make sure the service was fair. This included turning down early media inquiries from mainstream publications and instead using Dr. B on Zoom calls with representatives from groups such as black churches and Native American community groups, as the pandemic has disproportionately affected non-white groups.
Updated
March 9, 2021, 11:16 p.m. ET
“It was really important to him to put these communities at the top or get the information early,” said Brooke Williams, Black and a member of the Resistance Revival Chorus in New York. She joined one of the early Zoom calls and started spreading the word.
“To hear about gunshots being thrown away was just heartbreaking and annoying,” she said.
However, the service suffers from some of the same obstacles that have hampered vaccination efforts so far. While signing in is easy, it requires an internet connection as well as instant access to a mobile phone. Due to the last minute nature of the leftover cans, attendees need flexible schedules and access to transportation.
“It’s still heavily dependent on the Internet, so it depends on who’s hearing about it,” said Arthur Caplan, a medical ethicist at New York University’s Grossman School of Medicine. “It seems like he’s trying to solve a problem and do something good, but I’m sad that governments – counties, cities, national organizations – didn’t prepare for it and then didn’t respond faster to advice and To give instructions. “
Mr. Massoumi noted that the website allowed people such as community volunteers to sign up on behalf of others. The site is also available in Spanish.
He noted that the setup of the program, which allows users to log in and then wait for a notification in order of priority, is better than other sites that require hours of website updating when there is a chance they are lucky to achieve a rare opening.
What you need to know about the vaccine rollout
Some local health authorities, including Washington, DC and West Virginia, are moving to a similar pre-registration system that can help level the playing field.
“It feels like you don’t know where you are and the only way to save your spot is to update a browser,” said John Brownstein, a researcher at Boston Children’s Hospital, who runs VaccineFinder.org , an online portal that helps people book vaccine appointments.
For Brittany Marsh, who owns a pharmacy in Little Rock, Ark., Figuring out what to do with leftover cans has been a daily problem.
She said the number of no-shows had increased as vaccines became more available and others had to cancel at the last minute because they developed Covid-19 or were exposed to someone who did. Although sometimes people call, she said, “More than once we just have a no-show.”
Ms. Marsh has been testing Dr. B. and said this saved her staff the hassle of calling a waiting list from other customers to quickly fill the open spaces. With Dr. B she said, “I know they at least call what we think is the right group of people to get these shots so we never have to waste any.”
Dr. B only disclosed a few details about which providers have expressed interest in using its platform. Apart from the fact that the providers are based in 30 states and include doctors’ offices, pharmacies, and medical departments of large academic institutions.
The company collects sensitive personal information, which it promises to strictly protect, even though the data is not protected by the federal health privacy law known as HIPAA, as the company is not itself a medical service provider.
When asked about his long-term plans for the company, Mr Massoumi declined, noting that the vaccination race was not going to end anytime soon.
“Right now we just want the vaccines to be allocated in the best possible way,” he said. “I can’t think of a better way of spending money on solving the pandemic. So we’re just bowing our heads and focusing on it.”