Johnson & Johnson expects to release critical results from its Covid-19 vaccine trial in as little as two weeks — a potential boon in the effort to protect Americans from the coronavirus — but most likely won’t be able to provide as many doses this spring as it promised the federal government because of unanticipated manufacturing delays.
If the vaccine can strongly protect people against Covid-19, as some outside scientists expect, it would offer big advantages over the two vaccines authorized in the United States. Unlike those products, which require two doses, Johnson & Johnson’s could need just one, greatly simplifying logistics for local health departments and clinics struggling to get shots in arms. What’s more, its vaccine can stay stable in a refrigerator for months, whereas the others have to be frozen.
But the encouraging prospect of a third effective vaccine is tempered by apparent lags in the company’s production. In the company’s $1 billion contract signed with the federal government in August, Johnson & Johnson pledged to have 12 million doses of its vaccine ready by the end of February, ramping up to a total of 100 million doses by the end of June.
Federal officials have been told that the company has fallen as much as two months behind the original production schedule and won’t catch up until the end of April, when it was supposed to have delivered more than 60 million doses, according to two people familiar with the situation who were not authorized to discuss it publicly. Carlo de Notaristefani, lead manufacturing adviser for Operation Warp Speed, the federal vaccine development program, acknowledged a delay, but said the company might be able to catch up with initial production goals by March.
“I agree there was a problem,” Dr. de Notaristefani said. But he added, “Manufacturing of pharmaceuticals is not a black box where you turn the key and start counting.”
Any delay could be critical because the federal government has secured only enough vaccine doses to inoculate 200 million of the roughly 260 million eligible adults in the first half of this year. With the nation in the grip of its largest surge of the coronavirus to date and the death toll escalating to as high as 4,000 a day, Americans desperate to be vaccinated are lining the sidewalks outside vaccination centers.
Fears about the virus have only escalated with the scientific discovery last month that the country has been seeded with a new, highly contagious variant. On Tuesday, the Trump administration announced it would no longer hold back vaccine stocks for second doses in order to get more people at least partly vaccinated more quickly.
Dr. Paul Stoffels, Johnson & Johnson’s chief scientific officer, said he expected to see clinical trial data showing whether his company’s vaccine is safe and effective in late January or early February. But he declined to provide details about the company’s production capacity.
“We are not ready to release the numbers month by month at the moment, as we are in the discussion with the F.D.A.,” he said.
If the data is positive and the Food and Drug Administration authorizes the vaccine for emergency use, he added, “hopefully somewhere in March we’ll be able to contribute” to the nation’s vaccination drive.
That Johnson & Johnson’s timetable has slipped is not unusual given the frantic pace of vaccine development amid the worst pandemic in a century. But the delay also highlights the unrealistic promises of Operation Warp Speed.
The premise of the program was that the federal government would front the costs of development and manufacturing so that vaccine makers could mass-produce doses even before the vaccines were proved to work. Moncef Slaoui, chief scientific adviser for Warp Speed, said in December that Johnson & Johnson’s vaccine would be a “game changer” in the pandemic.
But at a Tuesday news conference, Dr. Slaoui said that instead of 12 million doses envisioned in the contract by the end of February, the company was likely to have in the “single-digit” millions. He also said the company was “trying to make that number get as close to a double-digit number as possible, and then a larger number in March and a much larger number in April.” Another person familiar with the company’s progress said it was poised to deliver only perhaps three million or four million doses of its vaccine by the end of next month.
In a statement, a Johnson & Johnson spokesman said, “We are confident we can meet our contractual obligations to supply our vaccine candidate to the U.S. government.”
Dr. de Notaristefani, Operation Warp Speed’s manufacturing chief, said the government’s contracts with vaccine makers were written at a time of great uncertainty, with the understanding that unforeseen obstacles could throw off the timetables. “Numbers are never cast in stone when you start a new process,” he said, adding that the company had to transfer its manufacturing from the Netherlands to a plant in Baltimore. “I really think that technically they couldn’t do it earlier.”
Dr. Marcus Plescia, the chief medical officer for the Association of State and Territorial Health Officials, said that state health officials were clearly excited about Johnson & Johnson’s one-dose vaccine.
Covid-19 Vaccines ›
Answers to Your Vaccine Questions
If I live in the U.S., when can I get the vaccine?
While the exact order of vaccine recipients may vary by state, most will likely put medical workers and residents of long-term care facilities first. If you want to understand how this decision is getting made, this article will help.
When can I return to normal life after being vaccinated?
Life will return to normal only when society as a whole gains enough protection against the coronavirus. Once countries authorize a vaccine, they’ll only be able to vaccinate a few percent of their citizens at most in the first couple months. The unvaccinated majority will still remain vulnerable to getting infected. A growing number of coronavirus vaccines are showing robust protection against becoming sick. But it’s also possible for people to spread the virus without even knowing they’re infected because they experience only mild symptoms or none at all. Scientists don’t yet know if the vaccines also block the transmission of the coronavirus. So for the time being, even vaccinated people will need to wear masks, avoid indoor crowds, and so on. Once enough people get vaccinated, it will become very difficult for the coronavirus to find vulnerable people to infect. Depending on how quickly we as a society achieve that goal, life might start approaching something like normal by the fall 2021.
If I’ve been vaccinated, do I still need to wear a mask?
Yes, but not forever. The two vaccines that will potentially get authorized this month clearly protect people from getting sick with Covid-19. But the clinical trials that delivered these results were not designed to determine whether vaccinated people could still spread the coronavirus without developing symptoms. That remains a possibility. We know that people who are naturally infected by the coronavirus can spread it while they’re not experiencing any cough or other symptoms. Researchers will be intensely studying this question as the vaccines roll out. In the meantime, even vaccinated people will need to think of themselves as possible spreaders.
Will it hurt? What are the side effects?
The Pfizer and BioNTech vaccine is delivered as a shot in the arm, like other typical vaccines. The injection won’t be any different from ones you’ve gotten before. Tens of thousands of people have already received the vaccines, and none of them have reported any serious health problems. But some of them have felt short-lived discomfort, including aches and flu-like symptoms that typically last a day. It’s possible that people may need to plan to take a day off work or school after the second shot. While these experiences aren’t pleasant, they are a good sign: they are the result of your own immune system encountering the vaccine and mounting a potent response that will provide long-lasting immunity.
Will mRNA vaccines change my genes?
No. The vaccines from Moderna and Pfizer use a genetic molecule to prime the immune system. That molecule, known as mRNA, is eventually destroyed by the body. The mRNA is packaged in an oily bubble that can fuse to a cell, allowing the molecule to slip in. The cell uses the mRNA to make proteins from the coronavirus, which can stimulate the immune system. At any moment, each of our cells may contain hundreds of thousands of mRNA molecules, which they produce in order to make proteins of their own. Once those proteins are made, our cells then shred the mRNA with special enzymes. The mRNA molecules our cells make can only survive a matter of minutes. The mRNA in vaccines is engineered to withstand the cell’s enzymes a bit longer, so that the cells can make extra virus proteins and prompt a stronger immune response. But the mRNA can only last for a few days at most before they are destroyed.
“You can get it and you’re done,” he said. “Everybody is eager to have it out there. It has a lot of potential.”
But even if Johnson & Johnson’s vaccine pans out, Dr. Plescia said, it won’t be enough. He predicted that state health departments would need a total of four vaccines in the next six months if they hope to reach their goals of offering a vaccine to every American who wants one.
“Or else the public is going to get very frustrated, because they’re ready for it to be opened up and there isn’t adequate supply to do that,” Dr. Plescia said.
Johnson & Johnson is by no means alone in its manufacturing delays. Dr. Albert Bourla, Pfizer’s chief executive, told investors last fall that his company had agreed to deliver 40 million doses of its vaccine to the federal government in 2020, assuming it proved successful in clinical trials. In the end, the company had only half that many ready to ship.
No one — including company executives — knows whether Johnson & Johnson’s vaccine will work. But Lynda Coughlin, a virologist at the University of Maryland School of Medicine who is not involved in the trial, said that the design of the vaccine and the results from early trials made her optimistic.
“Hopefully the results from Johnson & Johnson are just really going to knock it out of the park,” she said.
Johnson & Johnson’s Covid vaccine is fundamentally different from the authorized vaccines from Moderna and Pfizer-BioNTech. Those two consist of genetic molecules encased in oily bubbles. Johnson & Johnson built its vaccine from a virus that causes common colds, known as an adenovirus.
Testing the vaccine on monkeys, the researchers found that a single shot was enough to protect the animals from infection. When they tried out different formulations of the vaccine in early clinical trials, they were pleased to see that the vaccine prompted a strong antibody response with a single dose.
On Wednesday, Johnson & Johnson researchers and their colleagues published the full details of these early clinical trials in the New England Journal of Medicine. They reported that when they checked the blood of volunteers 71 days after receiving a single dose, their levels of coronavirus antibodies were still high. In some cases they were still increasing.
As results of the early clinical trials emerged over the summer, the company had to make a high-stakes decision: proceed with a clinical trial of two doses, which had the most likelihood of success, or try one with a single dose, which would be far more useful for getting shots to the masses — if it worked. The company decided to roll the dice with a single-shot trial.
“We know from vaccination campaigns that the simpler the logistics, the more successful the program,” said Dr. Dan Barouch, a virologist at Beth Israel Deaconess Medical Center who pioneered adenovirus vaccines in the early 2000s and collaborated with Johnson & Johnson researchers on the trial.
If many people began developing immunity from a single-shot dose, it might become harder for the virus to move from person to person, bringing down the high rates of new cases and easing the burden of the pandemic.
“A vaccine that is one dose would have a tremendous, tremendous public health impact, of course for low-income countries, but also in high-income countries,” said Ruth Faden, a professor of biomedical ethics at Johns Hopkins University.
While other vaccine developers moved quickly into late-stage trials, Johnson & Johnson deliberately moved more slowly so it could focus on ramping up manufacturing of its vaccine. At a facility in the Netherlands, researchers grew cells in which their adenoviruses could multiply. Adjusting the chemistry in giant vats, the scientists found a recipe for producing the vaccine at a fast, reliable rate.
Johnson & Johnson also began working early with other companies to prepare to manufacture the vaccine across the world. In April, it announced a partnership with the Maryland-based Emergent BioSolutions to manufacture the vaccine for the United States. Researchers from Johnson & Johnson began visiting Emergent BioSolutions starting that month to help it prepare for producing the adenoviruses.
“It was much more than a paper exercise: ‘Here’s the recipe, follow this,’” said Remo Colarusso, vice president at Janssen Supply Chain. “This is complex manufacturing.”
By the fall, Emergent BioSolutions was growing cells that were spewing out new adenoviruses. When Johnson & Johnson announced the start of its final Phase 3 trial, executives began making aggressive projections. “We are now committed to make more than one billion doses during 2021, and more after that,” Dr. Stoffels said at a September news conference.
The company then secured more deals to provide the vaccine to countries around the world. In 2021, Johnson & Johnson has promised to supply 200 million doses to Covax, an international partnership seeking to distribute coronavirus vaccines to nations that would not otherwise be able to afford them. It will supply another 300 million to Covax in 2022.
Soon after Johnson & Johnson started its trial, cases surged around the world. All the Phase 3 clinical trials of Covid vaccines accelerated because trials end only after a specified number of volunteers — from both the placebo and vaccinated groups — get sick. In November, the Pfizer-BioNTech and Moderna vaccine trials both delivered impressive results, with efficacy rates around 95 percent.
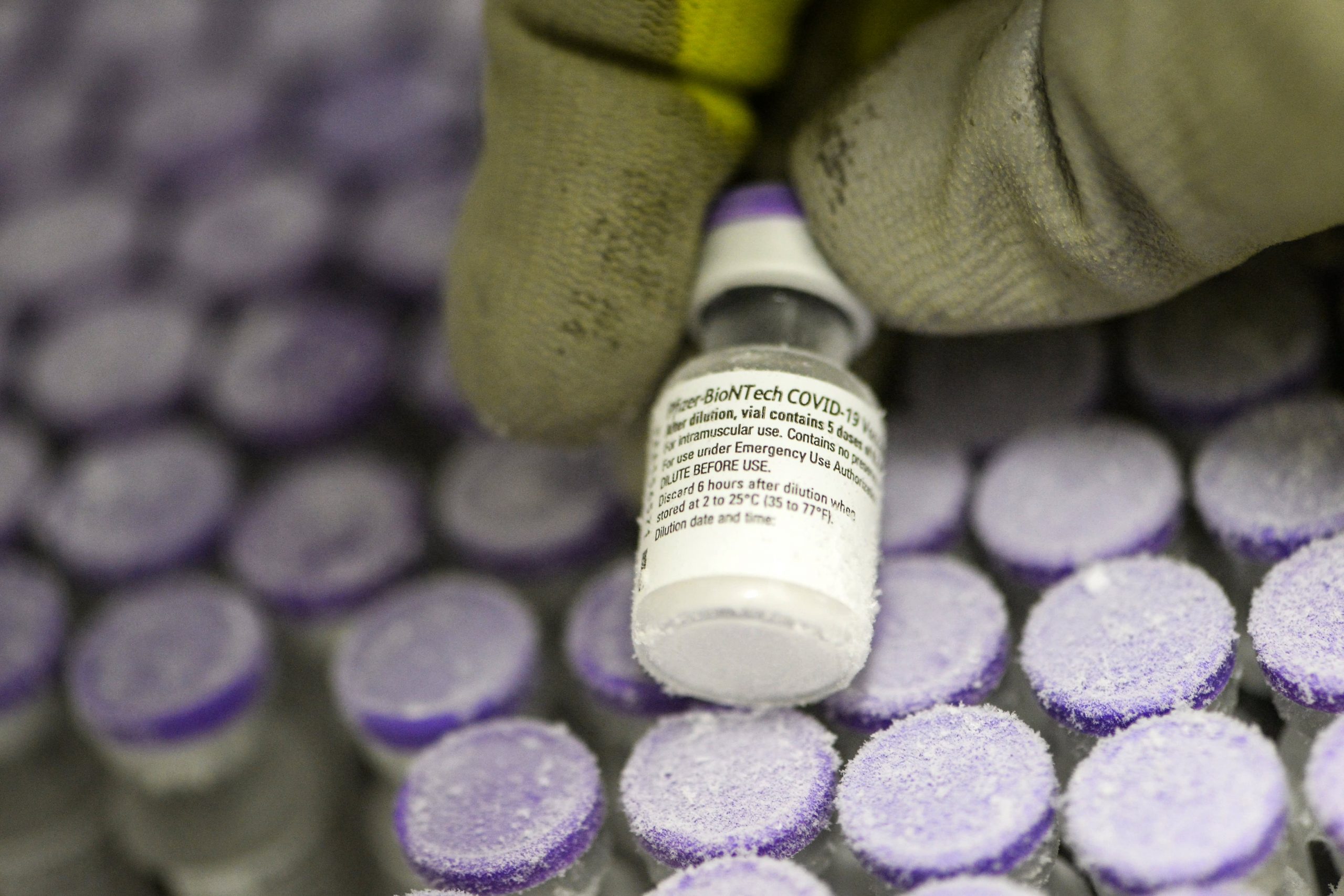
The F.D.A. authorized both vaccines for the United States, and other countries soon followed suit. But these two vaccines had some major shortcomings that soon became impossible to ignore. Both vaccines have to be kept in a deep freeze to prevent them from degrading. Once they reach a hospital or clinic, they have to be used before they spoil. In New York City and elsewhere, unused vaccines have ended up in the trash.
Once data collection is complete at the end of January or early February, an advisory board will review the data and report its analysis on safety and efficacy to Johnson & Johnson. F.D.A. regulators are already evaluating manufacturing data weeks ahead of when Johnson & Johnson is expected to apply for emergency authorization. Hiccups as small as mold in part of a facility could spur further delays.
Katie Thomas contributed reporting.