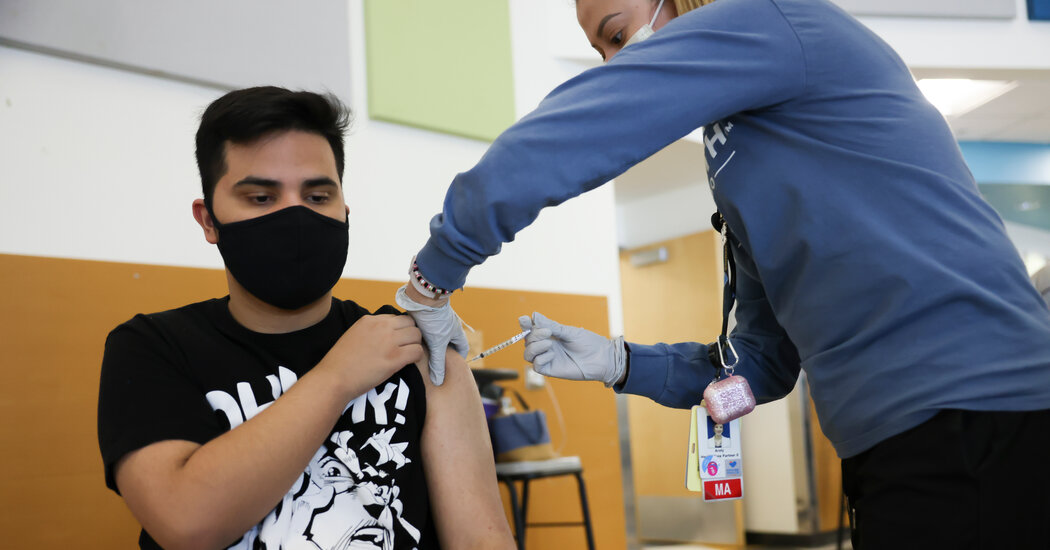
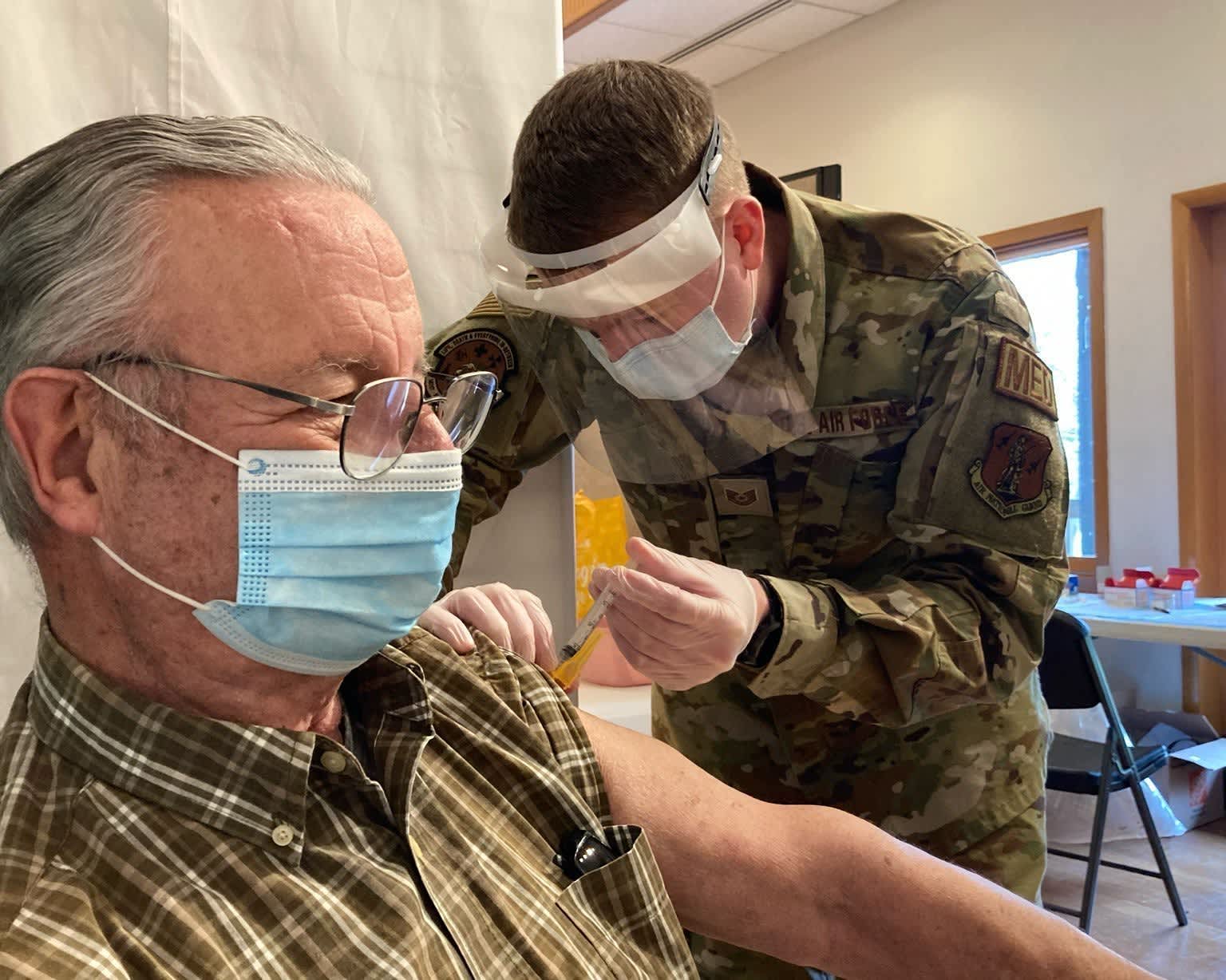
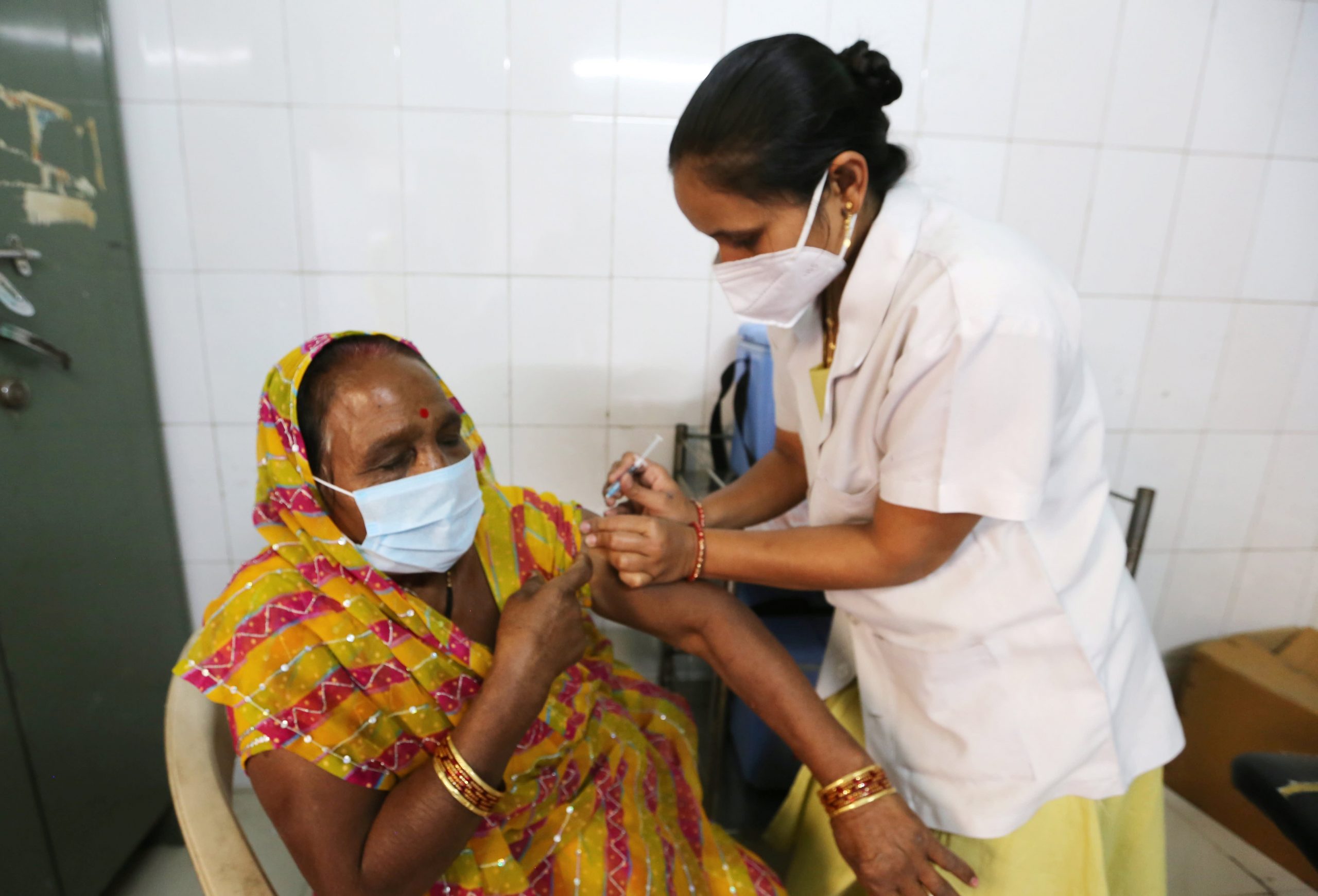
Marita Smith runs a nursing home in Seattle while Janet Snipes runs one in Denver. They share years of industry experience and painful memories of Covid-19, but have vastly different views on a new federal policy making vaccinations mandatory for all care home workers.
Ms. Smith said unvaccinated people should not be caring for a vulnerable population that has already been hit hard by the pandemic. The industry is seeing rising infection rates and deaths among residents again, but not reaching the highs of last year, and the mandate is expected to avert further increases.
“It’s great,” said Ms. Smith, administrator of the St. Anne Nursing and Rehab Center, calling the policy a “pretty big deal” that would “flush out health professionals who shouldn’t be in the health service.”
Such exits are exactly what worries Ms. Snipes, executive director of the Holly Heights Care Center in Denver. She, too, wants all homeworkers to be vaccinated, but not at the risk of losing employees who fail to do so in the midst of a labor shortage in an already high turnover industry.
Of the 1.5 million nursing home workers in the United States, approximately 540,000 – 40 percent of the workforce – are unvaccinated. Their fate could be directly affected by a directive announced by President Biden on Wednesday mandating vaccination of all nursing home workers, with the rules expected to go into effect in September. Institutions that fail to meet this goal could face fines or lose federal reimbursement, a major source of income for many.
The practical effect of the policy is that workers must be vaccinated or lose their jobs. Ms. Snipes said several employees told her they could leave. One who referred to her as her best nurse told her she was “very, very scared” of the vaccine, partly because she is black and worried about past medical experiments.
Getting vaccinated “is the safest thing for our residents and staff, but we believe he must contract all health care facilities,” Ms. Snipes said of President Biden. “We cannot afford to lose staff to hospitals and assisted living facilities.”
Several large nursing home chains and some states have already issued vaccination mandates. Industry officials said vaccinations were highly recommended, but their position on the new policy mirrored that of Ms. Snipes.
“We’re going to lose tens of thousands, maybe hundreds of thousands of workers,” said Mark Parkinson, president and chief executive officer of the American Health Care Association, a large nursing home trade group. He said he was hoping for policy changes and had already worked with Dr. Lee A. Fleisher, Chief Medical Officer of the Centers for Medicare & Medicaid Services, talked about it and looked for a meeting with Xavier Becerra, Secretary for Health and Human Services.
The most important change the industry is seeking is a signal from the administration that at some point there will be a mandate for all healthcare facilities so that nursing home workers can see there is nowhere else they can go. “Make it a commitment for everyone,” said Mr. Parkinson.
In fact, around 2,000 hospitals have already placed vaccination orders, reducing job opportunities for unvaccinated healthcare workers.
Dr. Fleisher said the CMS and the Centers for Disease Control and Prevention saw a “direct link” in the latest data between rising infections in nursing homes and unvaccinated staff.
Updated
Aug. 19, 2021, 6:01 p.m. ET
“The higher the percentage of unvaccinated workers, the higher the percentage of cases we have seen in these homes,” said Dr. Butcher. “There was a strong relationship.”
Currently, 60 percent of nursing home workers nationwide are vaccinated, well below the previous industry target of 75 percent by the end of June.
Parkinson said the industry is also lobbying the government to “launch a much more intense media campaign to influence workers” that vaccines are safe and effective. The trade organization also wants the government to create a grace period for hesitant employees.
Uy, a geriatrician and medical director of a Philadelphia nursing home, said he had seen the human resource challenges and was “excited about the mandate.”
“I’m exhausted,” he said. “The vaccine is like a small fortress around the weakest, in which the people inside remain safe even though a fire is raging outside.”
The mandate aims to avoid an increase in Covid cases and deaths in a high risk population.
Of the 625,000 Covid deaths to date in the US, almost a fifth – 133,700 – were residents of nursing homes, according to the CDC
Understand the state of vaccination and masking requirements in the United States
-
- Mask rules. The Centers for Disease Control and Prevention in July recommended that all Americans, regardless of vaccination status, wear masks in public places indoors in areas with outbreaks, reversing the guidelines offered in May. See where the CDC guidelines would apply and where states have implemented their own mask guidelines. The battle over masks is controversial in some states, with some local leaders defying state bans.
- Vaccination regulations. . . and B.Factories. Private companies are increasingly demanding coronavirus vaccines for employees with different approaches. Such mandates are legally permissible and have been confirmed in legal challenges.
- College and Universities. More than 400 colleges and universities require a vaccination against Covid-19. Almost all of them are in states that voted for President Biden.
- schools. On August 11, California announced that teachers and staff at both public and private schools would have to get vaccinated or have regular tests, the first state in the nation to do so. A survey published in August found that many American parents of school-age children are against mandatory vaccines for students, but are more supportive of masking requirements for students, teachers and staff who do not have a vaccination.
- Hospitals and medical centers. Many hospitals and large health systems require their employees to receive a Covid-19 vaccine, due to rising case numbers due to the Delta variant and persistently low vaccination rates in their communities, even within their workforce.
- new York. On August 3, New York City Mayor Bill de Blasio announced that workers and customers will be required to provide proof of vaccination when dining indoors, gyms, performances, and other indoor situations. City hospital staff must also be vaccinated or have weekly tests. Similar rules apply to employees in New York State.
- At the federal level. The Pentagon announced that it would make coronavirus vaccinations compulsory for the country’s 1.3 million active soldiers “by mid-September at the latest. President Biden announced that all civil federal employees would need to be vaccinated against the coronavirus or undergo regular tests, social distancing, mask requirements and travel restrictions.
And a recent CDC study of 4,000 nursing homes found that the effectiveness of Pfizer and Moderna vaccines among nursing home residents dropped from 75 percent in the spring to 53 percent by midsummer, when the delta variant spread further. “The results underline the crucial importance of the Covid-19 vaccination for employees, residents and visitors,” stated the authors of the study.
Health experts fear that unvaccinated employees could bring Covid-19 into a nursing home and infect residents. Nationwide, more than 80 percent of residents of nursing homes are vaccinated, but the number of cases in this population group is already increasing. In the week ending August 15, 354 care home residents died of Covid-19, the highest number since mid-March, and 3,585 tested positive, according to the CDC
The CDC has found that more employees are getting sick. In the week ending August 15, 5,810 nursing home employees contracted Covid-19, five times more than a month earlier, and 25 employees died.
Earlier this month, the Good Samaritan Society, which operates 142 nursing homes nationwide, announced that all 15,000 employees must be vaccinated by November 1, a position the company took after in homes where unvaccinated workers also tested positive , an increase in infections among residents was recorded. So far, the workforce has remained stable, said Randy Bury, the company’s CEO, who has argued in the past that such mandates would create safe and desirable jobs.
However, he argued that the Biden government’s new policy was wrong unless it was applied to the health sector as a whole. “What’s the difference in a nursing home versus a hospital?” Said Mr. Bury. “They are susceptible to the virus when they come into contact with unvaccinated employees.”
LeadingAge, a non-profit organization that represents 2,000 nursing homes and had previously requested mandates in individual homes, criticized the Biden policy for its narrow focus.
“The administration is right,” said Katie Smith Sloan, president and chief executive officer of LeadingAge, in a released statement. “We are at war. It would be a tragic misstep for the nurses who continue to struggle on the front lines to withdraw funds. “
Ms. Snipes, the director of Holly Heights in Denver, said she spent months training the staff and promoting vaccinations. She said most of her unvaccinated employees agreed to obey the mandate, but she mentioned three that she feared might leave. One told her that she did not want to put anything strange in her body. A second Catholic said he did not want an mRNA vaccine for religious reasons and that he had a letter of support from his bishop.
The third was the black nurse, who “sounds the most fearful of all the people I have spoken to,” said Ms. Snipes. “I want to save you as an employee.”