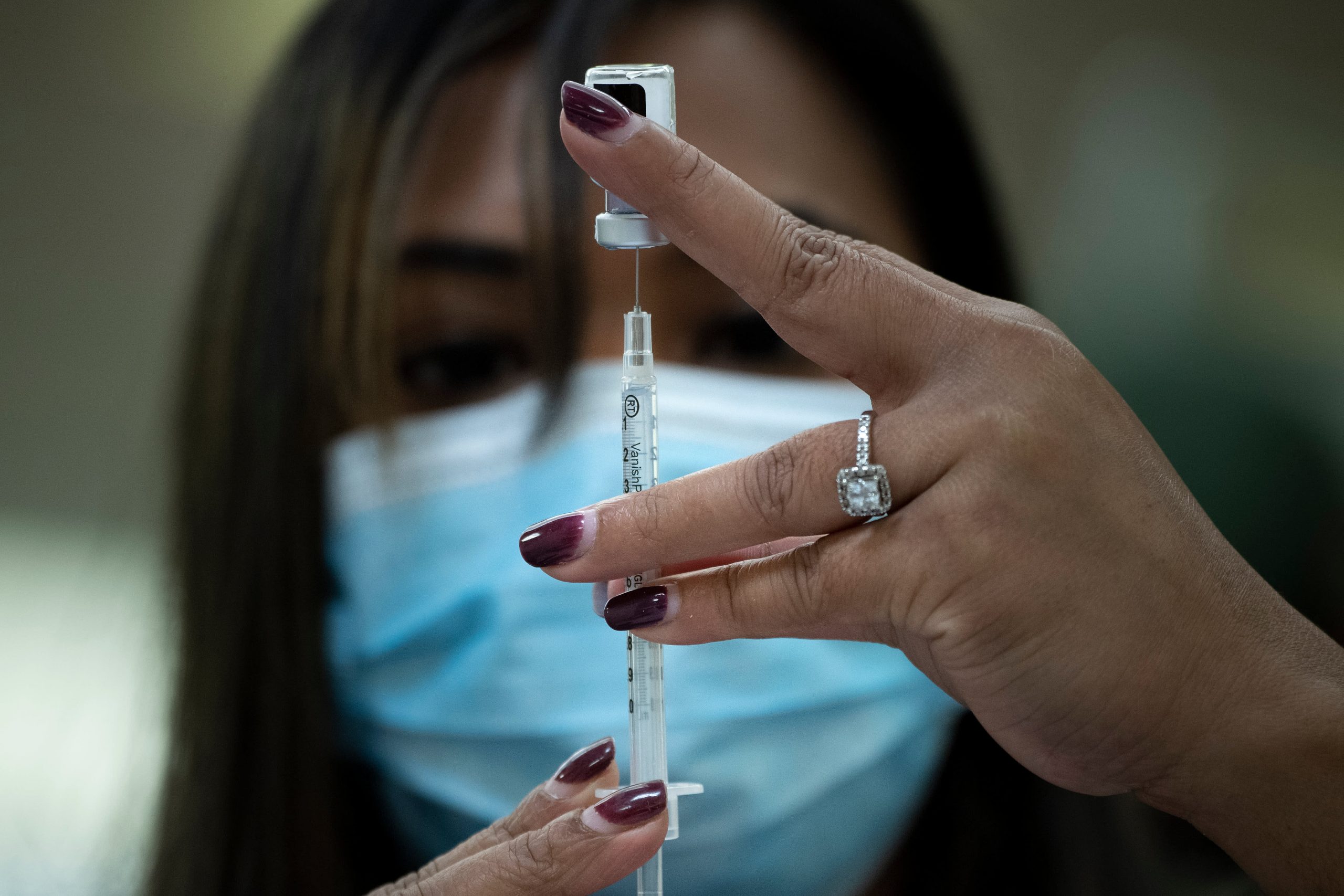
The American healthcare system may buckle under the weight of the coronavirus pandemic, but one number is inexplicably falling.
Disciplinary measures against doctors fell sharply in the first nine months of 2020. The National Practitioner Data Bank, a federal registry of health professionals and institutions, has recorded 4,393 reports of adverse behavior against doctors. Compared to 5,225 reports over the same period in 2019, that’s a decrease of nearly 16%, the U.S. Department of Health told CNBC.
The total includes 3,752 actions taken by government regulatory agencies, compared to 4,521 in the same period in 2019. Also in 2020, 641 doctors had limited or suspended their clinical privileges through September, compared to 704 in the same period last year.
The reasons for the decline are unclear. The pandemic forced widespread delays in non-Covid proceedings. In one study, more than 28 million elective surgeries were delayed or canceled in 2020. Patient advocates also point to the shortage of doctors during the pandemic, the crushes of critically ill patients, and even the heroic status of healthcare workers serving on the front lines of the crisis.
The president of the Federation of State Medical Boards denied that the shortage of doctors was a factor in states taking fewer measures against doctors over the past year.
“The guiding light, our north star, is the protection of the public,” said Dr. Humayun Chaudhry told USA Today in September. “It’s the facts of the complaint and the case. The problem of the workforce is not taken into account in individual cases.”
However, the decline in reports to the National Practitioner Data Bank almost certainly doesn’t mean the problem physicians’ problem is gone, patient safety experts say, despite extensive reforms in recent years.
“The mechanism is there. Indeed, it is required. And yet it does not work,” said Dr. Lucian Leape, Professor of Retired Health Policy at the Harvard School of Public Health.
Leape, whose 1994 publication “Error in Medicine” is widely recognized as revolutionizing the profession’s approach to medical errors, founded the Lucian Leape Institute, a think tank to improve patient safety.
Leape told CNBC’s American Greed that despite numerous safeguards – such as requiring incidents to be reported to the database and doctors being certified and assessed regularly – there are still too many incentives to maintain the status quo.
“Even if you get it right,” he said, “people fight back viciously because their livelihoods are at stake. And that’s a deterrent. Nobody wants to spend their time in court defending the fact that they’re doing this Guy asked to go. “
Activate ‘Dr. Death’
Leape is quick to point out that problem physicians are a tiny part of the profession. However, their effects can be catastrophic.
Neurosurgeon Christopher Duntsch, who came to be known as “Dr. Death,” was able to practice in at least four Texas hospitals over a period of three years, despite dozens of botched surgeries and two patient deaths. In 2017, a Texas judge sentenced 49-year-old Duntsch to life imprisonment for deliberately injuring an elderly person.
This photo from the Dallas County Jail shows Christopher Duntsch. A Texas jury found the neurosurgeon guilty on Tuesday, February 14, 2017 of mutilating patients who had turned to him for surgery to fix debilitating injuries.
Dallas County Jail via AP
The patient, 74-year-old Mary Efurd, became paraplegic after Duntsch botched her spinal surgery. Fellow surgeon Robert Henderson, who took care of Efurd after the incident, told CNBC’s American Greed that the complications were so severe that he wondered if Duntsch was really a doctor.
“I couldn’t imagine someone taking an anatomy class in medical school doing so much harm,” said Henderson.
In fact, Duntsch had an extensive and real resume, including a medical degree from the University of Tennessee at Memphis and a prestigious scholarship in spinal surgery.
Duntsch did not respond to several American Greed requests for comment.
Prosecutors said Duntsch could stay active that long because of the many cracks in a system designed to root out bad doctors. Alleged safeguards include a requirement to report incidents to the National Practitioner Data Bank, which Congress set up specifically in 1986 to prevent problem doctors from moving from hospital to hospital.
Two days after a committee at Baylor Plano Hospital in Dallas found that Duntsch had violated his standard of care in two botched operations, Duntsch simply resigned instead of being discharged. A fire would have been reported to the database. There was no resignation.
The hospital has since changed its name to Baylor Scott & White Health. Spokeswoman Jennifer McDowell declined to go into details of the case.
“Dr. Duntsch, who started his career in North Texas with impressive references and excellent referrals, ended up hurting families, employees, and the trust we all have in doctors,” McDowell said in an email. “Out of respect for the affected patients and families and the privilege of a number of details, we will continue to limit our comments. There is nothing more important to us than serving our community through high-quality, trustworthy healthcare.”
In another case, Dallas Medical Center granted Duntsch temporary privileges. He wasn’t hired. The reporting requirements for the database only apply to employees.
“Everyone knows when to get in touch, and no one likes breaking someone’s reputation,” said Michelle Shugart, Dallas County’s assistant district attorney who prosecuted Duntsch. “And so they are using these little techniques to find ways to avoid reporting someone.”
In a statement to American Greed, Dallas Medical Center spokesman Vince Falsarella said the facility had been in new ownership since Duntsch’s time there.
“The administration that existed at that time is no longer in the hospital,” he wrote. “Dallas Medical Center has a thorough physician certification process in place that meets all industry standards, best practices, and guidelines and regulations from the National Practitioner Data Bank to ensure the safety of our patients.”
Another hospital, the Legacy Surgical Center in Frisco, north of Dallas, said it had changed hands since Duntsch began practicing there. The fourth, University General in Houston, has closed.
None of the hospitals have been charged with criminal misconduct. The Texas Department of Health fined Baylor Plano $ 100,000 for violating the state’s administrative law in 2014, but subsequently overturned the finding without explanation.
Shugart believes some facilities were motivated by something more sinister than just avoiding the hassle of reporting a bad doctor.
“Neurosurgeons are one of the most lucrative aspects of the hospital business,” she said. “The financial incentives are a big part of what drives him and the people around him.”
Leape, the patient safety expert, said bad doctors don’t operate alone.
“These people have enablers,” he said. “This neurosurgeon didn’t take his patients out of thin air. Doctors refer patients. Neurosurgeons receive their patients from other doctors.”
Attention patient
To make matters worse, patients have few options to see a doctor in advance. The National Practitioner Database is confidential to the general public – you can find out the number of complaints, but not the doctors or institutions behind them.
For this reason, Leape believes it is important for patients who have had a bad experience with a doctor to report it.
“You need to make some noise,” he said. “You should go to the board of directors of the hospital and say, ‘You have to do something about this person’.”
Ultimately, Leape believes the rules need to be tightened. He advocates a federal patient safety agency to enforce standards and remove bad doctors, rather than the current patchwork of state regulators and hospital committees.
“We ask people to regulate their own profession and regulate themselves, and people just can’t,” he said.
Leape said hospitals – large chains in particular – have begun to prioritize patient safety. But he said that consciousness can only go so far.
“The systems are only as good as the people in them,” he said. “Systems work when people make them work.”
See how Christopher Duntsch got the nickname “Dr. Death” and how he got away with it for so long. Check out a NEW American Greed on Monday, February 1st at 10pm ET / PT on CNBC only.