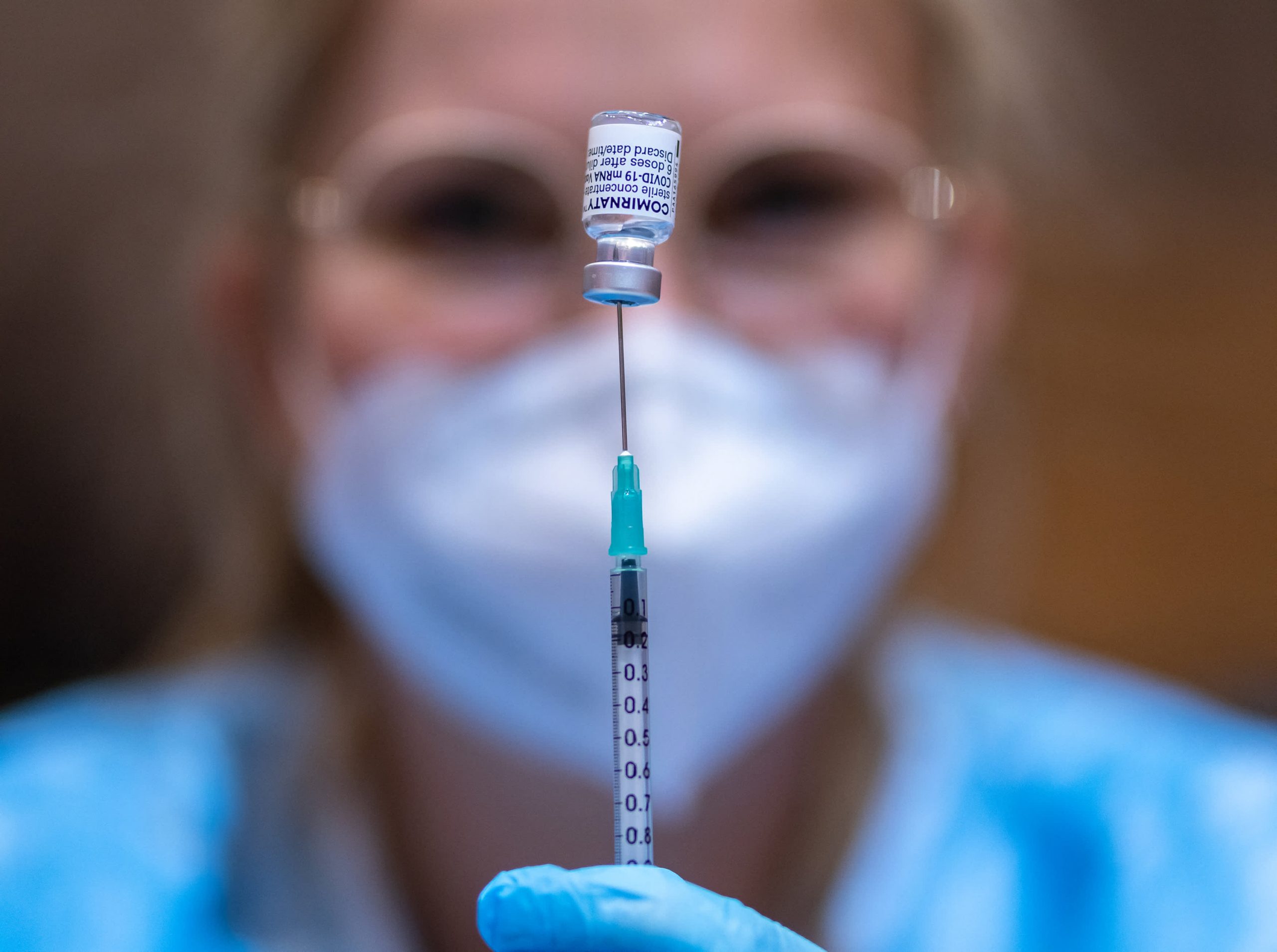
Two years ago a sneeze or cough would not have been a cause for concern, but now even the mildest symptoms can make us wonder, “Do I have Covid?”
At the beginning of the pandemic, we learned about the typical signs of infection, which can include loss of taste and smell, fever, cough, shortness of breath, and fatigue. But what about now, more than a year later? Have the symptoms changed since the Delta variant is currently the most common form of the virus in the US?
There is little data on this question and much remains to be unraveled.
Unvaccinated patients make up the vast majority of patients hospitalized with Covid-19, so they are more likely to develop severe symptoms such as difficulty breathing or persistent chest pain or pressure. In areas with lower vaccination rates, such as Louisiana, Texas, and Arkansas, unvaccinated children and young adults are hospitalized in higher numbers than at other times during the pandemic. Researchers don’t yet know for sure whether Delta is solely responsible for these severe symptoms or whether it is the rise in childhood infections that may lead to more hospitalizations.
The Delta variant is almost twice as contagious as previous variants and just as contagious as chickenpox. It replicates quickly in the body, and people carry large amounts of the virus in their noses and throats.
Dr. Andrew T. Chan, an epidemiologist and physician at Massachusetts General Hospital and a lead investigator on the Covid Symptom Study, has tracked millions of people from the UK, United States and Sweden through an app that prompts participants to report their symptoms. A preprint of data from the study that has not yet been published in a peer-reviewed journal suggests that those who are vaccinated are well protected against Delta. Breakthrough infections, while rare, tend to produce milder symptoms that are shorter in duration.
Understand the delta variant
At this point, nearly 90 percent of the UK adult population had received at least one dose of the vaccine. In the United States, 71 percent of adults are partially vaccinated.
In vaccinated adults, “the symptoms we are seeing now are much more likely to be identified with a cold,” said Dr. Chan. “We still see people presenting with a cough, but we’re also seeing a higher prevalence of things like runny nose and sneezing.” Headaches and sore throats are other top complaints, he added. Fever and loss of taste and smell are reported to a lesser extent.
Updated
Aug. 12, 2021, 11:24 p.m. ET
Dr. Chan said that at the time the Delta variant became widespread in the UK, researchers began seeing milder symptoms from late spring, which also coincided with the country’s mass vaccination program.
Pediatricians in New York City, where 67 percent of adults are fully vaccinated, say they see many of the same symptoms in children that they have seen since the pandemic began, and that the more severe cases usually occur in unvaccinated adolescents. especially those with underlying conditions like diabetes or obesity. Some toddlers or school-age children can also get very sick with Covid, but doctors don’t always know why one child gets much sicker than another, said Dr. Sallie Permar, Pediatrician-in-Chief at New York-Presbyterian and Weill Cornell Medicine.
Fever, cough, fatigue, headache and sore throat are the “classic presentation of Covid” in symptomatic children, she added.
If your child has potential Covid symptoms, including gastrointestinal issues, get both you and your child to take a Covid test and then stay home until the results are negative, said Dr. Adam Ratner, director of the Department of Pediatric Infectious Diseases at Hassenfeld Children’s Hospital at NYU Langone.
“That’s part of how we keep schools safe,” he added.
Tests are important for adults too, the experts said. Even if you have been vaccinated and your symptoms are mild, it is best to get tested. The Centers for Disease Control and Prevention believe that people who have been vaccinated can still pass the virus on to others.
“It is time to be humble that this is a new twist. We’re still learning, “said Dr. Mark Mulligan, the director of the NYU Langone Vaccine Center and the director of the Infectious Diseases Department at NYU Langone Health. “Be careful and play it safe when taking a test.”