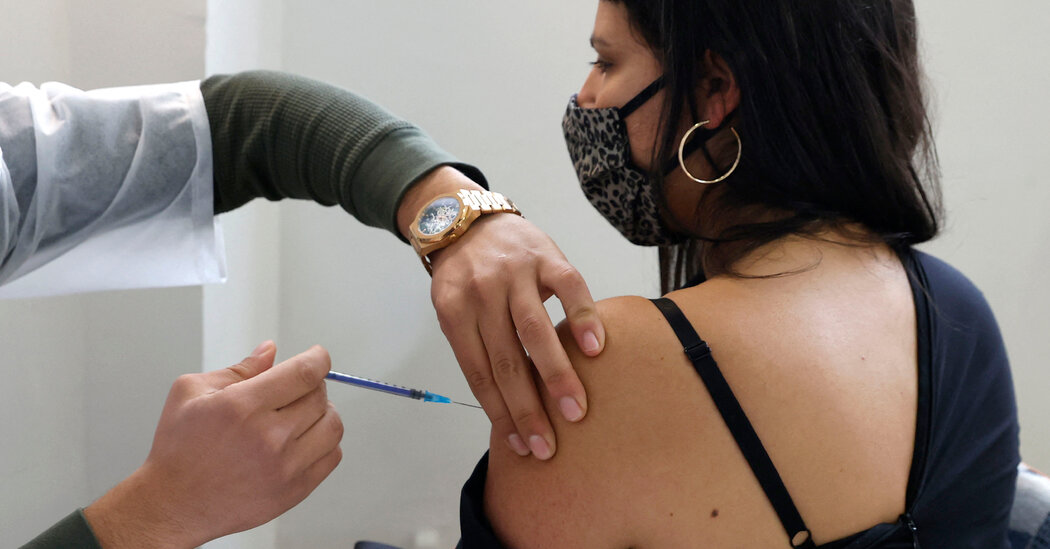
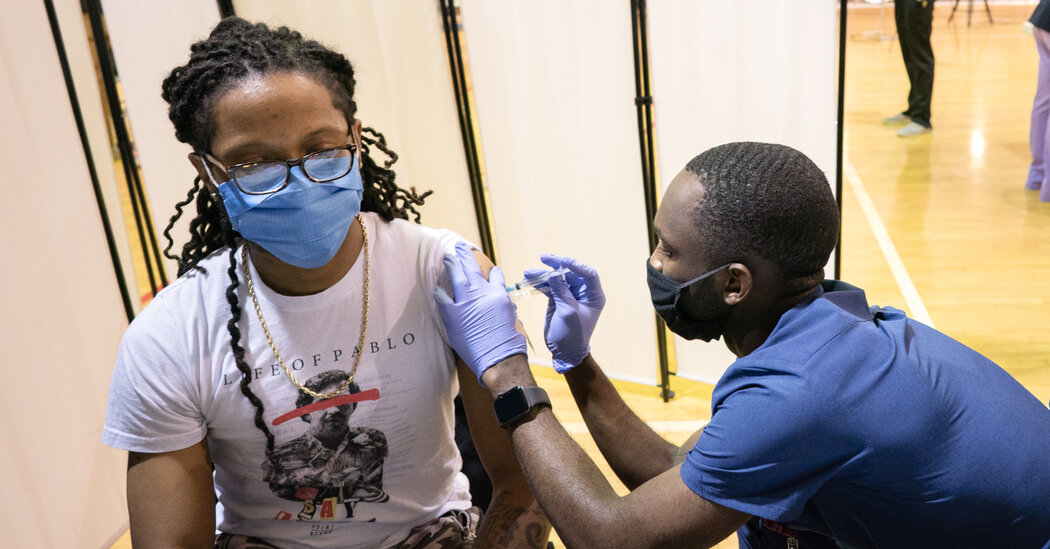
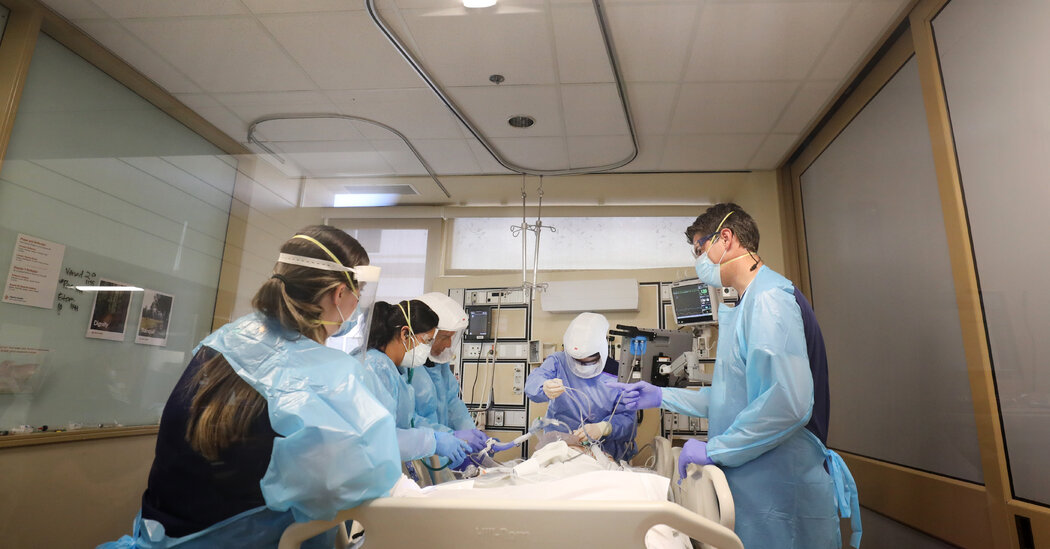
The Centers for Disease Control and Prevention published three studies on Wednesday that federal officials said provided evidence that booster shots of the Pfizer BioNTech and Moderna coronavirus vaccines would be needed in the coming months.
However, some experts said the new research did not support the decision to recommend a booster dose to all Americans.
Taken together, the studies show that while the vaccines are still highly effective against hospital admissions and deaths, their bulwark against infection with the virus has weakened in recent months.
The finding is consistent with early data from seven states compiled this week by the New York Times, suggesting an increase in breakthrough infections and a smaller increase in hospital admissions among vaccinated people as the Delta variant spread in July.
The decline in effectiveness against infections may be due to declining vaccine immunity, failure of precautionary measures like wearing masks, or the rise of the highly contagious Delta variant, experts said – or a combination of all three.
“We are concerned that this pattern of decline that we are seeing will continue in the coming months, which could result in decreased protection from serious illness, hospitalization and death,” said Dr. Vivek Murthy, the surgeon general, at a press conference at the White House on Wednesday.
Citing the data, federal health officials outlined a plan for Americans who received the two vaccines to receive a booster dose eight months after receiving their second dose starting September 20.
People who have received the Johnson & Johnson vaccine may also need additional doses. That vaccine wasn’t launched until March 2021, however, and a plan to deploy boosters will be drawn up after reviewing new data expected over the next few weeks, officials said.
Some scholars were skeptical of the government’s new initiative.
“These data support the administration of additional doses of the vaccine to severely immunocompromised individuals and nursing home residents, not the general public,” said Dr. Celine Gounder, Infectious Disease Specialist at Bellevue Hospital Center and former advisor to the administration for the pandemic.
Boosters would only be justified if the vaccines didn’t prevent hospital stays with Covid-19, she said.
“Feeling sick like a dog and staying in bed but not lying in hospital with severe Covid is not reason enough,” said Dr. Gounder. “We will be better protected by vaccinating the unvaccinated here and around the world.”
It’s unclear whether a third dose would help people who didn’t evoke a robust immune response to the first two doses, said Bill Hanage, an epidemiologist at Harvard TH Chan School of Public Health.
And the recommendation for boosters could also undermine confidence in the vaccines, he warned: “A third shot will increase skepticism among people who have not yet received a dose that the vaccines will help them.”
Taken together, the new studies show overall that vaccines are about 55 percent effective against all infections, 80 percent against symptomatic infections, and 90 percent or more against hospitalization, noted Ellie Murray, an epidemiologist at Boston University.
“These numbers are actually very good,” said Dr. Murray. “The only group for which this data would suggest boosters for me are the immunocompromised.”
Updated
Aug. 19, 2021, 10:57 a.m. ET
The apparent decrease in the vaccine’s effectiveness against infection could instead have been caused by increased exposure to the highly contagious Delta variant during a period of unrestrained social interaction, she added: “This seems like a real possibility to me, given many early vaccines motivated were the desire to see friends and family and return to normal. “
Dr. Murray said a booster vaccination would undoubtedly boost a person’s immunity, but the added benefit can be minimal – and just as easily achieved by wearing a mask or avoiding indoor dining and crowded bars.
The government’s focus on vaccines has undermined the importance of building other precautions into people’s lives in a convenient and sustainable way and strengthening testing capacity, said Dr. Murray and other experts.
“This is one of the reasons I think the government’s focus on vaccines is so damaging to morality,” she added. “We probably won’t get back to normal anytime soon.”
Before people can start the booster, the Food and Drug Administration must first authorize a third dose of the vaccines manufactured by Pfizer-BioNTech and Moderna, and an advisory committee from the CDC must review the evidence and make recommendations.
One of the new CDC studies analyzed the effectiveness of vaccines in residents of nearly 4,000 nursing homes from March 1 to May 9 before the advent of the Delta variant and of nearly 15,000 nursing homes from June 21 to August 1 as the new infections variant dominated in the country.
The effectiveness of the vaccines in preventing infection dropped from about 75 percent to 53 percent between those dates, the study found. The protection of the vaccines against serious illness has not been assessed.
Understand the state of vaccination and masking requirements in the United States
-
- Mask rules. The Centers for Disease Control and Prevention in July recommended that all Americans, regardless of vaccination status, wear masks in public places indoors in areas with outbreaks, reversing the guidelines offered in May. See where the CDC guidelines would apply and where states have implemented their own mask guidelines. The battle over masks is controversial in some states, with some local leaders defying state bans.
- Vaccination regulations. . . and B.Factories. Private companies are increasingly demanding corona vaccines for employees with different approaches. Such mandates are legally permissible and have been confirmed in legal challenges.
- College and Universities. More than 400 colleges and universities require a vaccination against Covid-19. Almost all of them are in states that voted for President Biden.
- schools. On August 11, California announced that teachers and staff at both public and private schools would have to get vaccinated or have regular tests, the first state in the nation to do so. A survey published in August found that many American parents of school-age children are against mandatory vaccines for students, but are more supportive of masking requirements for students, teachers and staff who do not have a vaccination.
- Hospitals and medical centers. Many hospitals and large health systems require their employees to receive a Covid-19 vaccine, due to rising case numbers due to the Delta variant and persistently low vaccination rates in their communities, even within their workforce.
- new York. On August 3, New York City Mayor Bill de Blasio announced that workers and customers will be required to provide proof of vaccination when dining indoors, gyms, performances, and other indoor situations. City hospital staff must also be vaccinated or have weekly tests. Similar rules apply to employees in New York State.
- At the federal level. The Pentagon announced that it would make coronavirus vaccinations compulsory for the country’s 1.3 million active soldiers “by mid-September at the latest. President Biden announced that all civil federal employees would need to be vaccinated against the coronavirus or undergo regular tests, social distancing, mask requirements and travel restrictions.
Nursing homes did not have to report the number of residents vaccinated until after June 6, which “makes comparisons over time very difficult,” said Dr. Murray. “It is entirely possible that the effectiveness of the vaccine reported here has not really diminished over time.”
The decline in effectiveness could also be due to the spread of the Delta variant, said Dr. Gounder.
“It makes sense to give vaccinated nursing home residents an extra dose of vaccine, but what will have an even bigger impact on protecting these nursing home residents is vaccinating their caregivers,” she said. Many caregivers in long-term care facilities remain unvaccinated.
A second study evaluated data from New York State from May 3 to July 25, when the Delta variant grew to more than 80 percent of new cases. The effectiveness of vaccines in preventing cases in adults fell from 91.7 percent to 79.8 percent during that time, the study found. But the vaccines remained just as effective at preventing hospital stays.
In those weeks, New York recorded 9,675 breakthrough infections – about 20 percent of the state’s total cases – and 1,271 hospital admissions of vaccinated people, accounting for 15 percent of all Covid-19 hospital admissions.
Although fully immunized people of all ages contracted the virus, the vaccine’s effectiveness fell the most, from 90.6 percent to 74.6 percent in people ages 18 to 49 – who are often the least likely to take precautions and are most likely to socialize .
Data from Israel suggests immunity to infection has declined in vaccinated adults aged 65 and over. But in the New York data, the effectiveness of the vaccines in this group hardly diminished.
Adults aged 65 and over were hospitalized more often than other age groups, regardless of their vaccination status. But the vaccines did not show a decrease in effectiveness against hospital admissions in any of the age groups.
The CDC’s third study found the vaccines showed 90 percent effectiveness against hospital stays in the country, “which is excellent,” noted Dr. Gounder.
The vaccines provided less protection against hospitalization in immunocompromised people. “But not all immunocompromised people will respond to an extra dose of vaccine,” noted Dr. Gounder.
To protect these vulnerable people, everyone around them should be vaccinated and continue to wear masks, she added.
The vaccines appear to be less effective than the studies that led to their approval, as those studies were done before the delta variant emerged.
Statistically, as more unvaccinated people become infected, recover, and gain natural immunity, the vaccines may lose relative effectiveness. And scientists always expected that the proportion of those who were vaccinated among those infected would increase if more people were vaccinated.
If preventing infection is the goal, it would be smarter to develop a booster shot of a nasal spray vaccine that will create better immunity in the nose and throat where the virus enters the body, said Dr. Gounder.