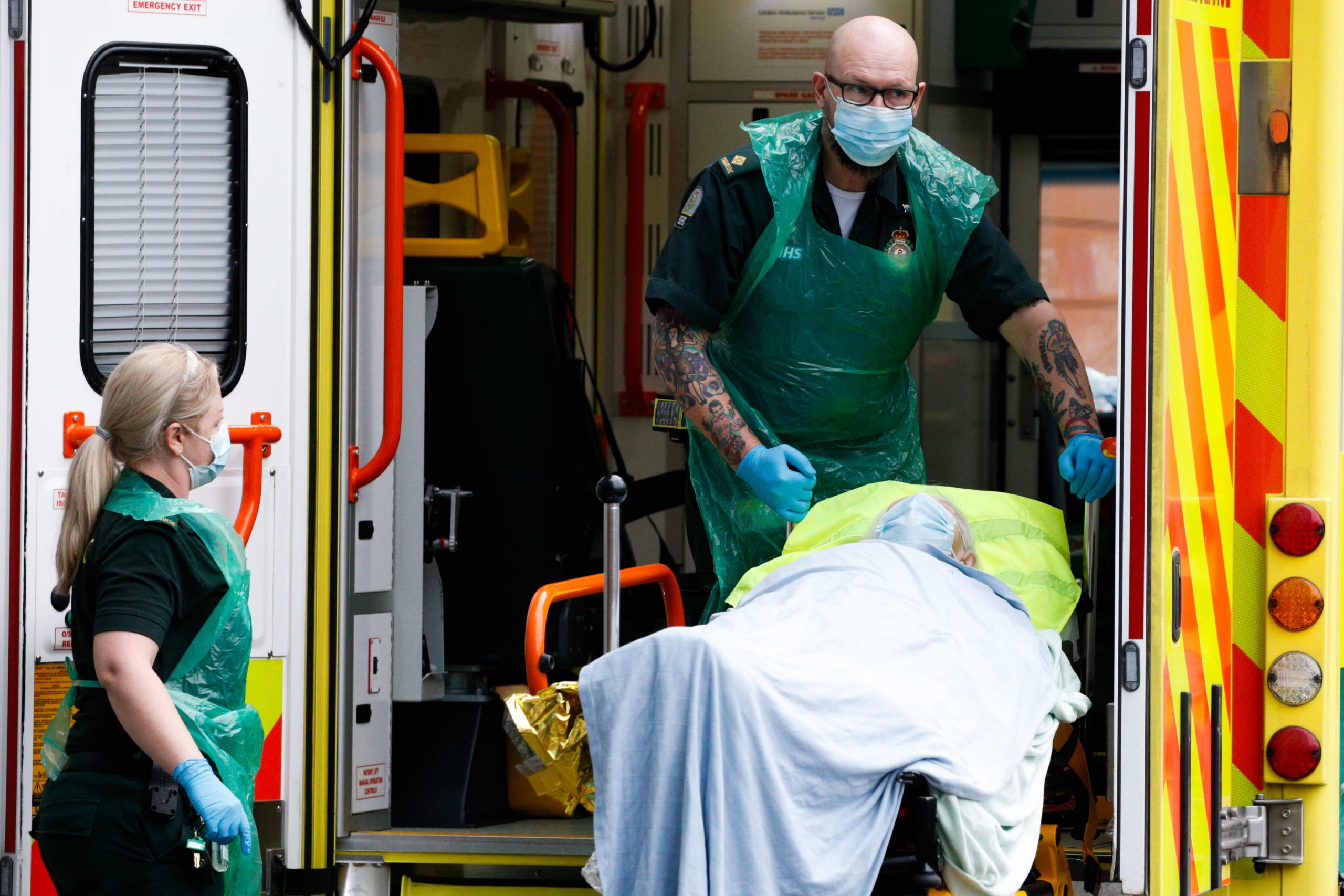
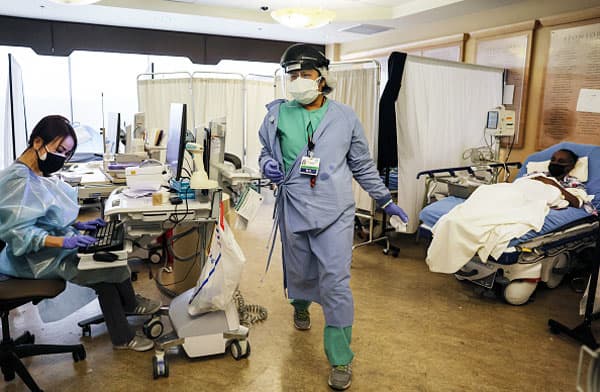
People in Africa who are seriously ill with Covid-19 are more likely to die than patients in other parts of the world, according to a report published Thursday in the medical journal The Lancet.
The report, which is based on data from 64 hospitals in 10 countries, is the first comprehensive look at what is happening to critically ill Covid patients in Africa, the authors say.
The increased risk of death only applies to seriously ill people, not to everyone with the disease. Overall, the disease and death rates from Covid appear to be lower in Africa than in the rest of the world. However, if the virus spreads faster in Africa, as in other regions, these results suggest that the death toll may worsen.
Among 3,077 critically ill patients admitted to African hospitals, 48.2 percent died within 30 days, compared with a global average of 31.5 percent, according to the Lancet study.
The study was observational, which meant the researchers tracked patients’ progress but did not experiment with treatments. The work was done by a large team called The African Covid-19 Critical Care Outcomes Study Investigators.
For Africa as a whole, the death rate among seriously ill Covid patients could be even higher than the study, the researchers said, as much of their information came from relatively well-equipped hospitals and 36 percent of those facilities in hospitals were South Africa and Egypt, which had better ones Resources than many other African countries. In addition, with a mean age of 56, the patients in the study were younger than many other critically ill Covid patients, suggesting that death rates outside the study may be higher.
The other eight countries in the study were Ethiopia, Ghana, Kenya, Libya, Malawi, Mozambique, Niger and Nigeria. Leaders from 16 other African nations had also agreed but ultimately refused to participate.
Reasons for the higher mortality rates are a lack of resources such as surge capacity in intensive care units, devices for measuring patient oxygen levels, dialysis machines and so-called ECMO devices for pumping oxygen into the bloodstream of patients whose lungs are so impaired that even a ventilator is used not enough to keep them alive.
However, the study’s authors suggested that the available resources were obviously not being used. Proning – placing patients on their stomachs to make it easier for them to breathe – was under-used and only performed on about a sixth of the patients who needed it.
Almost 16 percent of hospitals had ECMO, but fewer than 1 percent of patients offered it. Although 68 percent of the sites had access to dialysis to treat kidney failure, which is common in severe Covid cases, only 10 percent of critically ill patients received it. Half of the patients who died never received oxygen, but the study’s authors said they had little data to explain why.
A Lancet editorial by experts who were not involved in the study said, “It is common in Africa to have expensive equipment that is inoperable due to poor maintenance or a lack of skilled labor.” According to a report by Tropical Health and Education Trust from 2017, around 40 percent of medical equipment in Africa was out of order.
Another factor is that few doctors in Africa have pulmonary and critical care training that is considered essential to treating Covid patients.
As in other studies, chronic diseases such as diabetes, high blood pressure and diseases of the heart, kidneys or liver increased the risk of dying from Covid. This study was the first to involve a large proportion of HIV patients, which nearly doubled the risk of death. The report said, “Our data suggest that HIV / AIDS is a major risk factor for Covid-19 mortality.” However, the authors also said they had no data on how the severity of HIV infection was related could affect the risk.
An unexpected finding from the study was that, unlike Covid patients in the rest of the world, men in Africa are no more likely to die than women. This finding suggests that African women are at higher risk than women in other regions.
The authors suggested that women in Africa “may face barriers to access to care and limitations or prejudices in care when they are seriously ill”.
The editorial asked if new variants could cause the high mortality rate noted in the study, but also said, “This is a question that could take a long time to answer in a continent with severe sequencing deficiencies.”