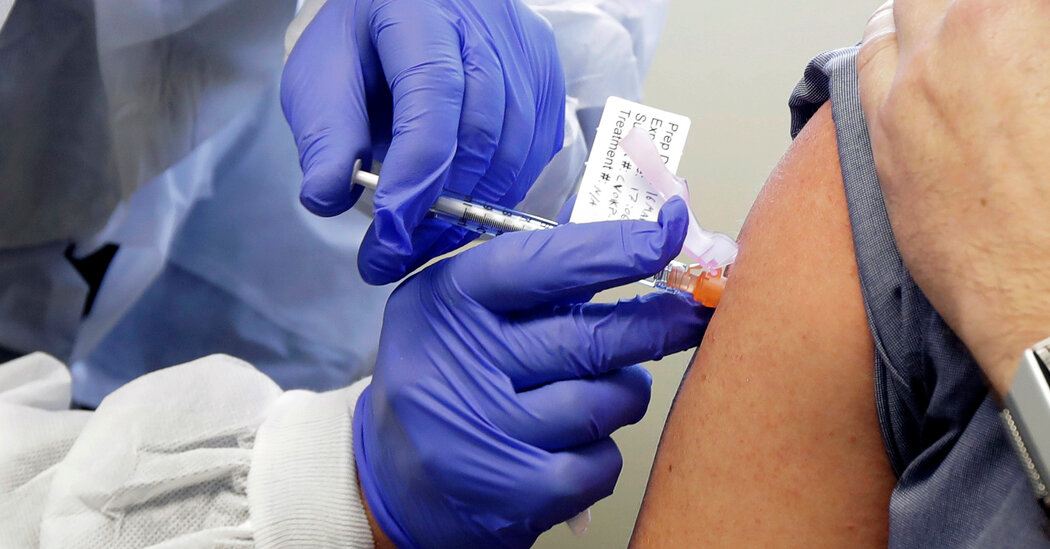
WASHINGTON – Newly released data confirmed on Tuesday that Moderna’s coronavirus vaccine offers high levels of protection and sets the stage for this week’s emergency approval from federal regulators and beginning its spread across the country.
The Food and Drug Administration intends to approve use of the vaccine on Friday, said people familiar with the agency’s plans. The decision would give millions of Americans access to a second coronavirus vaccine as early as Monday.
The FDA review confirms Moderna’s earlier assessment that the vaccine had an efficacy rate of 94.1 percent in a study of 30,000 people. Side effects, including fever, headache, and fatigue, were uncomfortable but not dangerous, the agency found.
The success of Moderna’s vaccine has become all the more important to fighting the pandemic as other vaccine efforts have stalled. The hopeful news comes at a time with a record number of coronavirus cases overwhelming hospitals and an ever-increasing death toll that hit a bleak milestone of 300,000 on Monday.
The data release is the first step in a public review process that includes a one-day meeting on Thursday by an independent panel of experts. You will hear from Moderna, FDA scientists, and the public before they vote on whether to recommend approval. The panel is expected to vote yes and the FDA generally follows the experts’ recommendations.
Distribution of about six million doses could then begin next week, significantly adding to the millions of doses already developed by Pfizer and BioNTech, the companies that only released the first emergency coronavirus vaccine last Friday . Healthcare workers received the first shots of the Pfizer BioNTech vaccine Monday with an efficacy rate of 95 percent.
The introduction of vaccines has been eagerly anticipated and is one of the most ambitious vaccination campaigns ever carried out in the United States.
Last summer, the federal government signed contracts with Moderna and Pfizer to dispense a total of 200 million cans in the first quarter of 2021. Since both vaccines require two doses, these contracts guaranteed enough doses for 100 million people.
Last week the government announced that it had bought an additional 100 million doses of Moderna for the second quarter, bringing the number of Americans who can be vaccinated to 150 million. That leaves the question of how and when the 180 million or so other Americans will be covered.
Both vaccines are made available to the public free of charge.
Moderna’s vaccine has become a symbol of government scientists’ successes during the pandemic. After China released the genetic sequence of the new virus in early January, scientists from Moderna and the National Institutes of Health were able to focus on designing a vaccine in just two days. Unlike Pfizer, Moderna has a close relationship with Operation Warp Speed, the federal program that seeks to get a vaccine to market quickly. Nearly $ 2.5 billion federal funding helped Moderna buy raw materials, expand its factory, and increase its workforce by 50 percent.
Moderna’s success contrasts with two other high profile projects the US had hoped would increase vaccine supply: one from pharmaceutical companies Sanofi from France and GlaxoSmithKline from the UK and one from Anglo-Swedish drug maker AstraZeneca and the Oxford University.
AstraZeneca and Oxford used two different doses in clinical trials in the UK and Brazil. The effectiveness was 62 percent at one level and 90 percent at the other. These jumbled results have made it unclear when AstraZeneca will have enough data to obtain an emergency clearance.
Meanwhile, Sanofi and GlaxoSmithKline received disappointing results with their vaccine in early clinical trials. While it produced a promising immune response in volunteers under the age of 50, it did not do so in older people. The companies are now planning a series of new studies with a different version of the vaccine. Due to the delay, they are unlikely to provide vaccines before the end of 2021.
Moderna’s vaccine worked equally well in white volunteers and in color communities. There was also no significant difference between protecting men and women or between healthy volunteers and those at risk for severe Covid-19 who developed conditions such as obesity and diabetes. For people aged 65 and over, the study found an estimated effectiveness of 86.4 percent, which is below the overall estimate of 94.1 percent. However, the apparent difference was not statistically significant.
So far, FDA reviews have shown two possible differences between vaccines, but the results may reflect a lack of data more than real differences. The Pfizer BioNTech study showed that the vaccine began protecting against the coronavirus within about 10 days of the first dose. The experiment with the vaccine from Moderna, however, did not show such a noticeable effect after the first dose.
However, in the early days of the Moderna study, there were fewer cases of Covid-19 among study participants, making it more difficult to measure the differences between the vaccinated group and the placebo group. In either case, health officials have said that for both vaccines, two doses are essential for complete protection.
Updated
Dec. 15, 2020 at 9:31 am ET
A second difference concerns the ability to prevent serious diseases. Moderna presented more evidence that its vaccine can, according to the review. In his study, 30 volunteers developed severe cases of Covid. All of them belonged to the placebo group, with no cases among the vaccinated people.
In the Pfizer BioNTech study, the results were less convincing. There were 10 severe cases in the placebo group and one in the vaccinated group. These numbers are too few to assess the vaccine’s ability to prevent serious diseases.
“The data available for these results did not allow firm conclusions,” said the FDA.
The documents released on Tuesday made it clear that side effects were particularly common after the second dose, but usually lasted only one day. Experts say people may need to take a day off after the shot.
During the Moderna trial, researchers also kept an eye out for volunteers who developed new disorders. In a multi-month study of 30,000 volunteers, it is normal for some to have conditions unrelated to the vaccine, health experts say. Comparing the rates between people receiving the vaccine and placebo, as well as general background rates, can help identify serious concerns and eliminate coincidences.
During the Moderna study, three vaccinated participants developed a form of temporary facial paralysis called Bell’s palsy, while one participant on the placebo experienced the same. Bell’s palsy, which can last weeks or longer, can be triggered by viral infections and other causes. Around 40,000 people develop the disease in the United States each year. Years of intensive research have found no evidence that any vaccine routinely recommended in the US causes Bell’s palsy.
In the review released Tuesday, the FDA said, “There is insufficient information currently available to establish a causal relationship with the vaccine.”
The Pfizer BioNTech study identified four cases in the vaccine group, including one in a person with a history of the disorder and none in the placebo group.
Dr. Peter Marks, the FDA’s lead vaccine regulator, said in an interview with JAMA Monday that the cases of Bell’s palsy in the study were most likely not caused by the vaccine and that the apparent difference between the two groups of volunteers was only one reason Random question.
“Our working hypothesis is just that this is an imbalance in the background rates, as we’ve seen in other studies,” he said.
In its analysis of the Moderna vaccine released Tuesday, the FDA said it plans to recommend prosecuting Bell palsy cases when the vaccines are rolled out.
“We’re going to ask about this just to wrap up that question,” said Dr. Marks on Monday.
The FDA’s analysis did not reveal any serious allergic reactions to the Moderna vaccine. The same was true for the Pfizer-BioNTech clinical trial, but when vaccinations began in the UK outside of that study, two people with a history of serious allergies had a severe and potentially life-threatening reaction called anaphylaxis.
UK health officials have said people with a history of anaphylaxis should avoid the Pfizer BioNTech vaccine.
In the United States, the Centers for Disease Control and Prevention has stated that people with serious allergies can be safely vaccinated, with close monitoring for 30 minutes after receiving the shot.
Moderna and Pfizer-BioNTech vaccines are similar in their ingredients, but not identical. Therefore, it is not clear whether an allergic reaction to one vaccine would occur with the other. Both are made up of genetic material called mRNA that is enclosed in a bladder made of a mixture of fats. The two companies use different fats.
Moderna has applied for approval to vaccinate people aged 18 and over, as in its study. The Pfizer BioNTech vaccine was approved for people aged 16 and over because the study included a number of younger volunteers. Both companies are conducting experiments with children aged 12 and over and plan to also study younger children.
Sharon LaFraniere contributed to the coverage.
[Like the Science Times page on Facebook. | Sign up for the Science Times newsletter.]