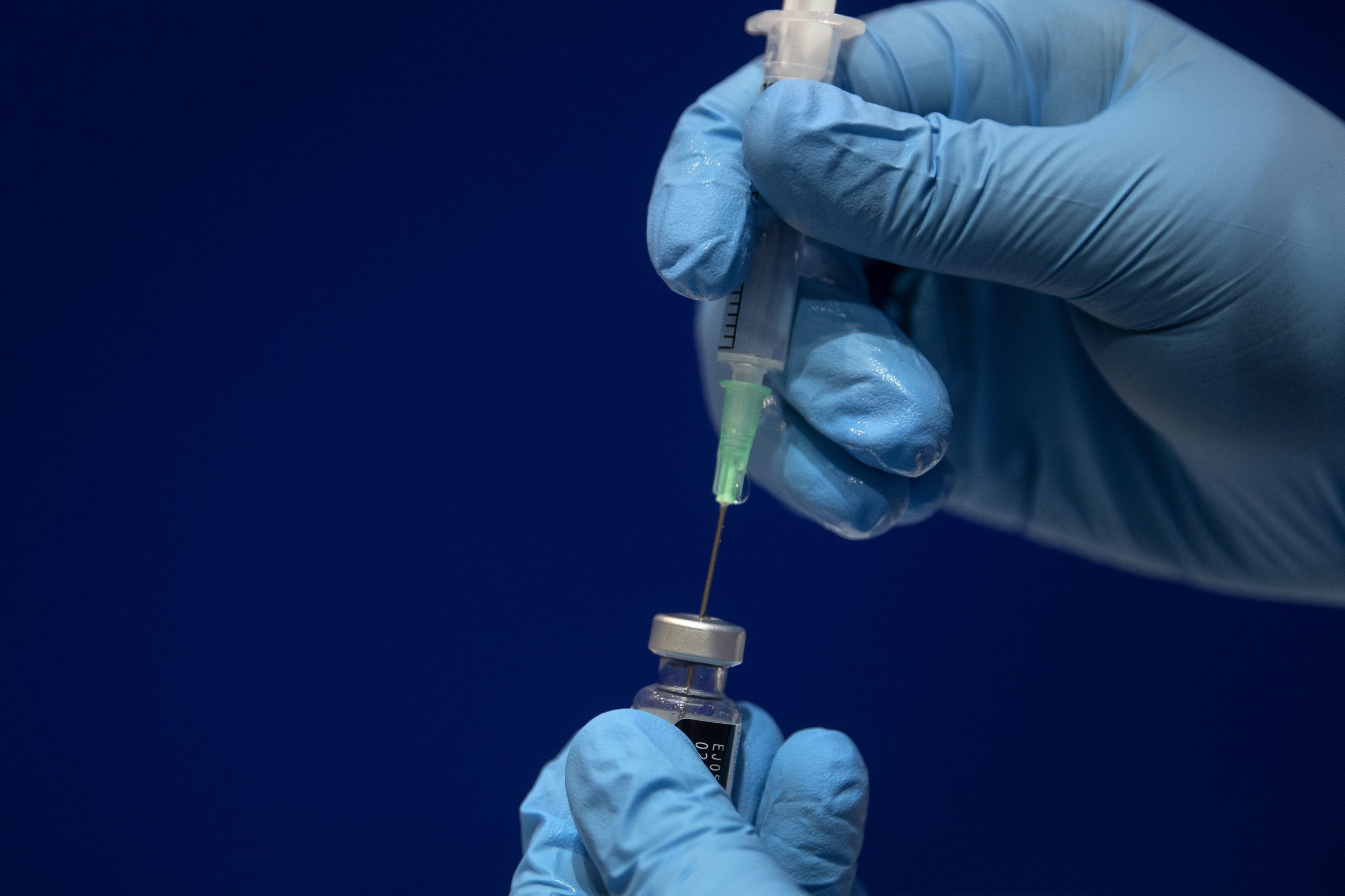
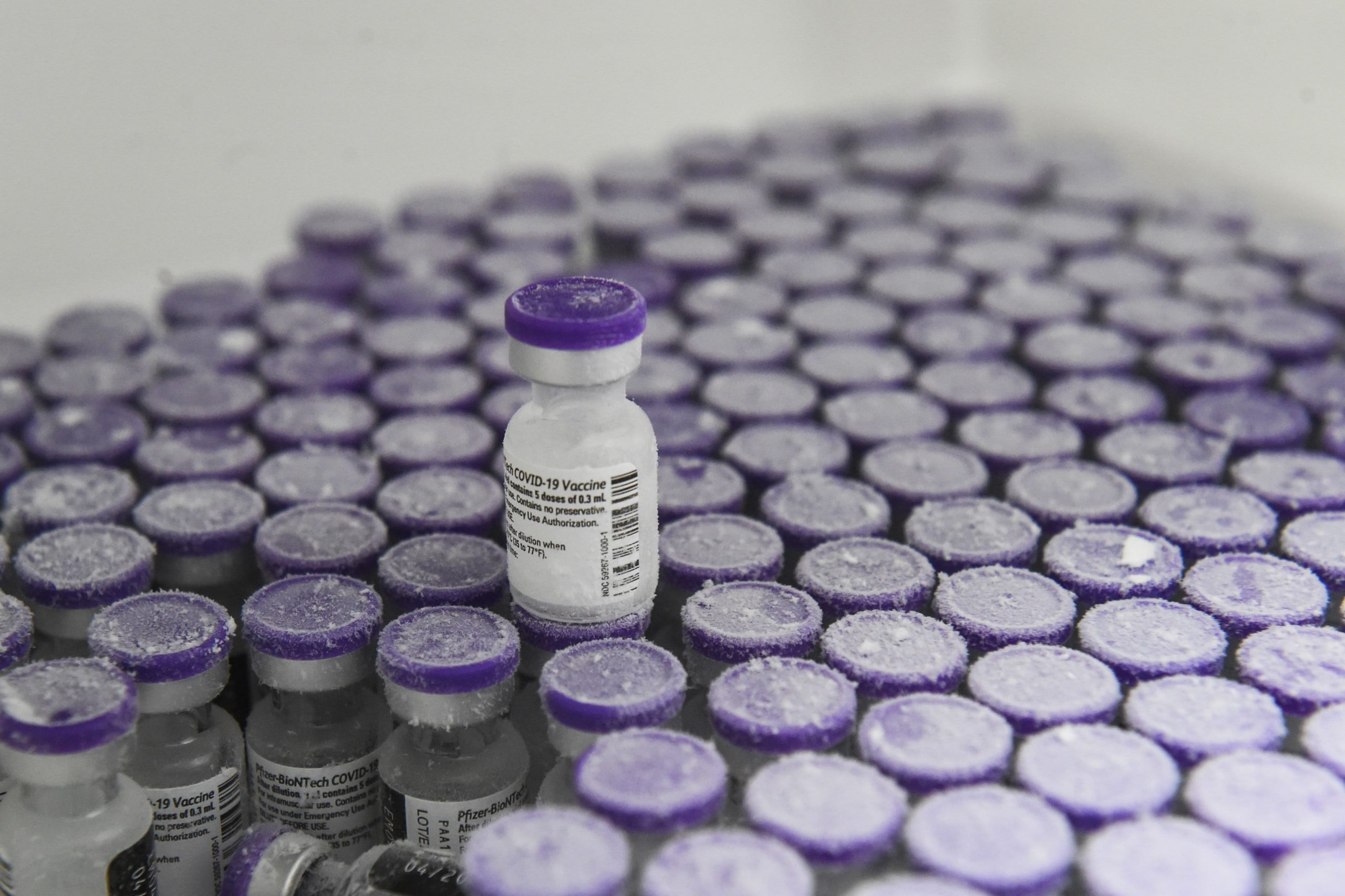
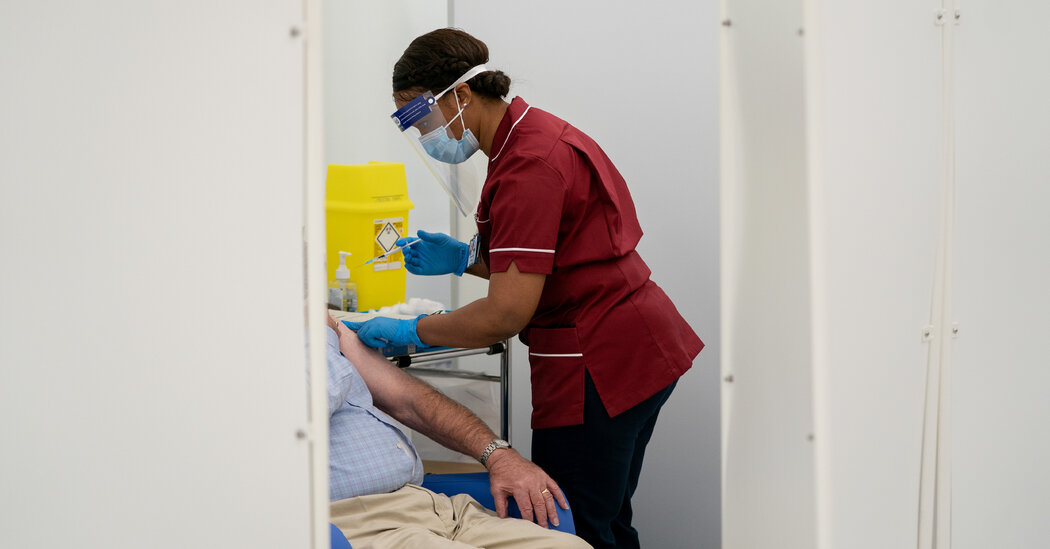
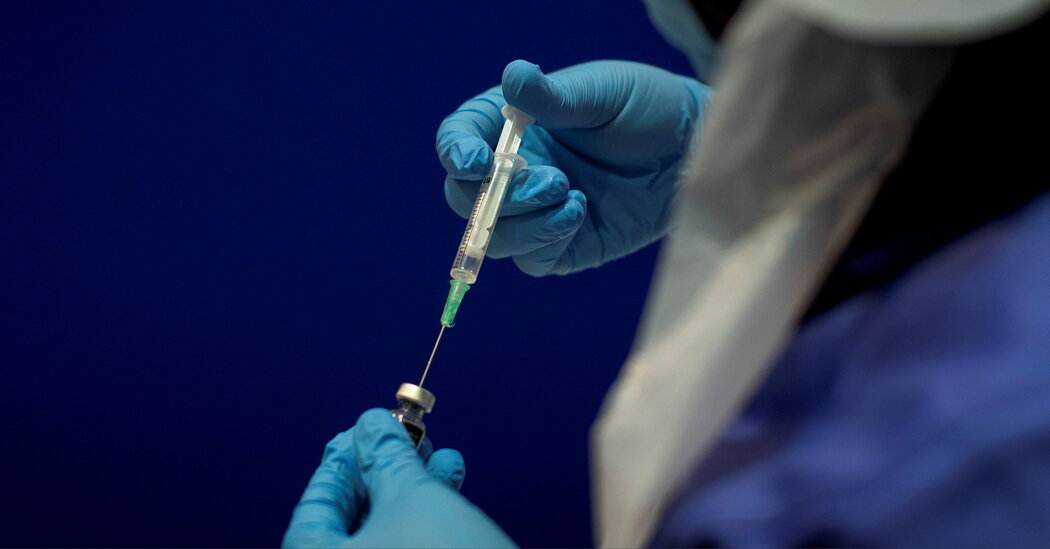
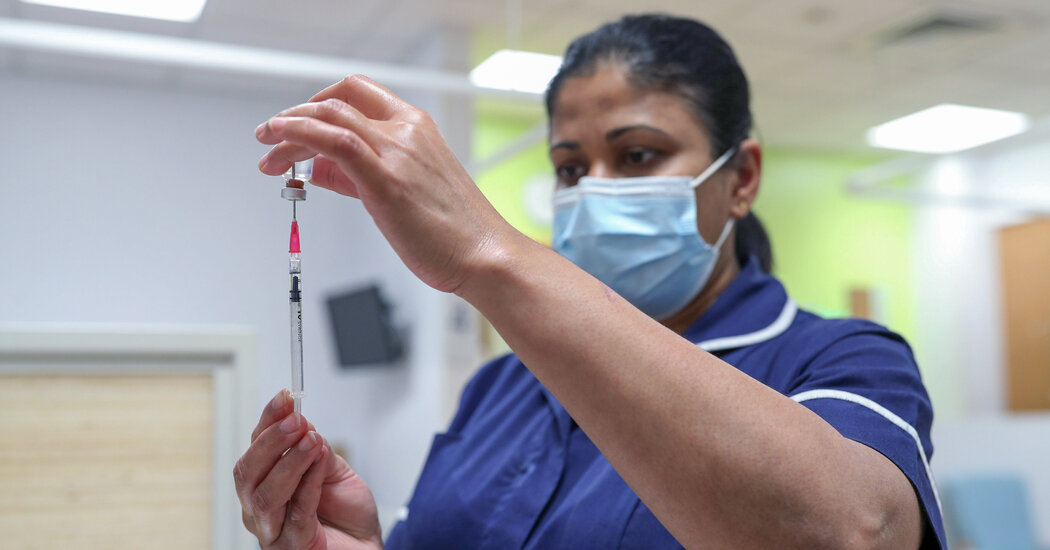
Pfizer officials met privately with senior U.S. scientists and regulators on Monday to press for rapid approval of booster coronavirus vaccines amid growing public confusion over whether they are needed and opposition from federal health officials who say that the additional doses are now not required.
The high-level online meeting, which lasted an hour, and at which Pfizer’s chief scientist briefed virtually every top doctor in the federal government, took place the same day Israel began feeding heart transplant patients and others on the third dose of the Pfizer BioNTech vaccine administer weakened immune system. Officials said after the meeting that more data – and possibly several months – would be needed before regulators could determine whether booster injections were needed.
The two developments underscored the intensifying debate about whether booster injections are required in the US, when and for whom. Many American experts, including Dr. Anthony S. Fauci, President Biden’s senior medical advisor on the pandemic, have said there isn’t enough evidence yet that boosters are necessary. However, some say Israel’s move may anticipate a government decision to recommend it to at least the weak.
Pfizer is collecting information on antibody responses from those receiving a third dose, as well as data from Israel, and expects to share at least part of that in a formal application to the Food and Drug Administration for its coronavirus vaccine to expand its emergency clearance in the coming weeks.
However, the final decision on booster vaccination, several officials said after the meeting, will also depend on real-world information the Centers for Disease Control and Prevention has gathered about breakthrough infections – those that occur in people who have been vaccinated – who are serious or ill Cause hospital stays.
And any booster vaccination recommendations are likely to be calibrated within age groups as well, officials said. For example, if booster shots are recommended, they could first go to residents of nursing homes who received their vaccines in late 2020 or early 2021, while older people who received their first vaccinations in the spring may have to wait longer. And then the question arises, what kind of booster: a third dose of the original vaccine or perhaps a vaccination tailored to the highly contagious Delta variant, which is on the rise in the USA.
“It was an interesting meeting. They shared their data. There was nothing like a decision, ”said Dr. Fauci in a short interview Monday night, adding, “This is just part of a much bigger puzzle, and it’s part of the data, so there’s no question of a compelling case either way.”
Amy Rose, a Pfizer spokeswoman, said in a statement, “We had a productive meeting with US public health officials about elements of our research program and preliminary booster data.”
The Ministry of Health and Welfare, which convened the meeting, issued its own statement confirming the government’s stance. “At this point, fully vaccinated Americans don’t need a booster dose,” it said.
With less than half of the United States’ population being fully vaccinated, some experts said Monday the country must continue to focus on giving all Americans their first dose. The most important task of the Food and Drug Administration is to increase public confidence by granting full approval to the coronavirus vaccines used, which are initially approved in an emergency.
“At this point the most important strengthening we need is vaccinating people,” said Dr. Carlos del Rio, an infectious disease expert at Emory University in Atlanta. The booster doses in Israel, he added, “will help us answer some questions, but at the end of the day I disagree with what they are doing. I think it’s terribly premature. “
Within the Biden government, some fear that if Americans are convinced that coronavirus vaccines only offer short-lived immunity before needing a boost, they are less likely to accept vaccination. Those concerns could fall by the wayside, however, if new data from Israel, expected in the next few weeks, conclusively shows that immunity wears off after six to eight months, significantly increasing the risks for the elderly or other vulnerable populations.
The government convened the meeting on Monday in response to the announcement last week by Pfizer and its German partner BioNTech that they would develop a version of their vaccine targeting the Delta variant and reported promising results from studies with people who A third dose of the vaccine received original vaccine six months after the second.
The new dates Not yet published or peer-reviewed, but as announced by companies that they would submit data to the Food and Drug Administration to approve booster vaccinations surprised the Biden White House.
In an unusual joint statement Thursday evening, hours after Pfizer-BioNTech’s announcement, the FDA and CDC pushed back.
“Americans who are fully vaccinated currently do not need a booster,” the statement said, adding, “We are prepared for booster doses when and when science shows they are needed.”
The move can make economic sense for Pfizer-BioNTech. Since the outbreak of the pandemic, the partner companies have been following a “get to market first” strategy in the manufacture and marketing of their vaccines.
The companies did not accept federal funds or participate in Operation Warp Speed, former President Donald J. Trump’s fast-track vaccine initiative. Not only were they the first to get Food and Drug Administration approval for their coronavirus vaccine, the first to use the novel mRNA technology, but also the first to get their vaccine approved in adolescents.
The strategy has “paid off as well as you could wish,” said Steve Brozak, president of WBB Securities, a biotechnology-focused research investment bank.
Last week, Pfizer and BioNTech said a booster given six months after the second dose of the vaccine increased the effectiveness of antibodies against the original virus and beta variant by five to ten times. But antibody levels may not be the best biological measure of need for booster doses, say experts, who say it’s no surprise that antibodies increase after a third dose.
“The antibody response is not the only measure of immune protection,” said Dr. Leana S. Wen, a former health commissioner for Baltimore. “There have been several studies to suggest that these vaccines also stimulate B-cell and T-cell immunity. Even if there aren’t that many antibodies, it doesn’t mean someone isn’t protected. “
In Israel, the government has agreed to provide Pfizer with data on its vaccine recipients, and Pfizer has cross-checked the Israeli data with the results of its own laboratory tests. Some people familiar with the data say this suggests that those vaccinated may lose immunity after about six to eight months, leading to an increasing number of breakthrough infections.
The participants in Monday’s meeting were a who’s who of government doctors: Dr. Fauci; Dr. Rochelle Walensky, director of the Centers for Disease Control and Prevention; Dr. Francis Collins, the director of the National Institutes of Health; Dr. Vivek Murthy, the general surgeon; Dr. Rachel Levine, the assistant secretary of health; Dr. Janet Woodcock, acting FDA commissioner; Dr. Peter Marks, the director of the FDA’s Center for Biologics Evaluation and Research; and Dr. David Kessler, a former FDA commissioner who, among other things, leads the Biden government’s vaccine distribution efforts.
Dr. Del Rio, of Emory University, complained that the meeting was held privately on Monday instead of Pfizer publicly presenting its dates to the CDC’s Advisory Committee on Vaccine Practices, which will ultimately recommend whether booster injections are needed.
Just over two-thirds of American adults – 67.7 percent – got at least one Covid-19 shot, according to the CDC. The president had hoped to have at least partially vaccinated 70 percent of adults by July 4th.
Still, the national vaccination campaign has made it clear that the vaccine is successful in preventing disease, and studies suggest that vaccines against the Delta variant remain effective. Outbreaks occur in areas with low vaccination rates and the number of national cases has increased recently; according to a database from the New York Times.
World Health Organization officials on Monday stressed the importance of prioritizing global vaccine production and distribution over booster development, given the large gaps between countries’ vaccine programs.
“That doesn’t mean one or the other; it brings order to a crisis, ”said Dr. Michael Ryan, the organisation’s executive director of the emergency health program, on what the organization calls a two-stage pandemic.
Lauren McCarthy contributed to the coverage.