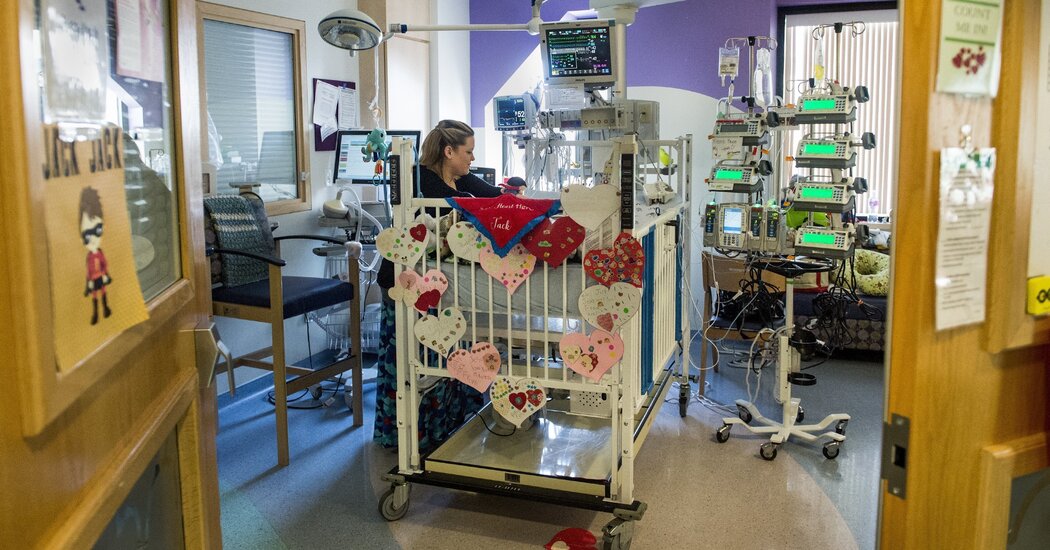
EL HUSSEINEYA, Egypt – A scream pierced the night from the balcony of an Egyptian hospital. A nurse yelled that patients in the intensive care unit in Covid were gasping for air.
Ahmed Nafei, who was standing outside, passed a security guard, stormed in and saw that his 62-year-old aunt was dead.
Angry, he took out his cell phone and started filming. It appeared that the hospital had run out of oxygen. Monitors beeped. One nurse was clearly desperate and crouched in a corner when her colleagues tried to resuscitate a man with a manual ventilator.
At least four patients died.
Mr Nafei’s 47-second video this month about the chaos at El Husseineya Central Hospital, about two and a half hours northeast of Cairo, went viral on social media.
As the outrage grew, the government denied the hospital had run out of oxygen.
An official statement released the following day concluded that the four deceased had suffered “complications” and denied that the deaths were “in any way related” to anoxia. Security officers interrogated Mr. Nafei and officials accused him of breaking rules that prohibit visiting and filming in hospitals.
However, an investigation by the New York Times found otherwise.
Witnesses, including medical staff and patient relatives, said in interviews that oxygen pressure had fallen to steeply low levels. At least three patients, and possibly a fourth, died of a lack of oxygen. A detailed analysis of the video by doctors in Egypt and the United States confirmed that the chaotic scene in the intensive care unit indicated an interruption in oxygen supply.
The fatal lack of oxygen was the end result of a cascade of problems in the hospital, our research found. By the time the patients suffocated in the intensive care unit, an ordered oxygen release was hours too late and a backup oxygen system had failed.
“We will not bury our heads in the sand and pretend everything is fine,” said a doctor at the hospital on condition of anonymity because he feared arrest. “The whole world can admit there is a problem, but not us.”
The government’s rush to deny the episode is just the latest example of the lack of transparency in its response to the Covid crisis, which has sparked cynicism and distrust of its public assurances.
For many Egyptians, Mr Nafei’s video offered a rare and uncensored look at the real toll of the coronavirus at the height of Egypt’s second wave of pandemics.
The government admitted that four people died in intensive care that day, January 2, but denied that it was due to a lack of oxygen.
The Ministry of Health’s statement stated that the deceased patients were mostly elderly, that they died at different times, and that at least a dozen other patients, including newborns in incubators, were connected to the same oxygen network and unaffected. These factors confirmed “the lack of a link between the deaths and the alleged lack of oxygen”.
Medical staff confirmed that the hospital’s oxygen supply was not completely depleted, but said the pressure was dangerously low. In the intensive care unit, it is even worse and not enough to keep the patients alive. The pressure may have been lower because the intensive care unit’s oxygen vents were at the end of the network or because of other inefficiencies in the pipeline.
Updated
Jan. 18, 2021, 5:26 p.m. ET
Efforts by hospital staff to correct the shortage were thwarted by further mishaps. When they tried to switch the intensive care unit oxygen supply from the hospital’s main tank to the reserve reserve, the reserve system appeared to be overloaded and failed.
Earlier in the day, aware that they were running out of breath, hospital officials had requested more oxygen from the Ministry of Health. But the van that was due in the afternoon was more than three hours late.
“If it had arrived by 6 p.m., none of this would have happened,” said the hospital doctor.
The medical experts who analyzed the video, including six doctors in the United States and Egypt, discovered details that aid in the determination of oxygen failure.
In the video, none of the patients appear to be connected to the central oxygen line.
A doctor uses a portable tank, which is usually used in an emergency and only temporarily. And just a few feet away, a group of nurses are trying to resuscitate a patient with a manual pump that does not appear to be connected to an oxygen source.
“There is no oxygen tube attached to the airbag,” said Dr. Hicham Alnachawati, a New York emergency doctor who worked in intensive care units in hospitals. It doesn’t happen. It’s impossible if you don’t have oxygen. “
Another doctor who checked the video, Dr. Bushra Mina, the Egyptian-American head of pulmonology at Lenox Hill Hospital who has cared for hundreds of Covid-19 patients in New York, noted the “urgency” of the doctor and nurses in the video “Trying to Oxygenate the Patients.” supply or supplement. “
“It can be overwhelming, even in the US where you have a lot of resources,” said Dr. Mina. “Imagine Egypt where resources are limited and you exceed your capacities.”
The oxygen crisis at El Husseineya Central Hospital may not have been the only one.
Signs of shortages in other hospitals flooded social media for a week. A hospital director on social media urged people to donate portable oxygen tanks, citing a “critical need”. A patient in another hospital filmed himself in the isolation ward and said, “We don’t have enough oxygen.” And a video of a scene similar to the one Mr. Nafei saw was posted online.
These claims could not be independently verified.
“Is there a real problem?” asked Ayman Sabae, a researcher with the Egyptian Personal Rights Initiative, a human rights group. “Nobody but the government can claim to have this information.”
The government’s record during the crisis has not instilled confidence that it aligns with the Egyptians.
President Abdel Fattah el-Sisi has denounced critics of the government’s coronavirus efforts as “enemies of the state”. His security services expelled a foreign journalist who questioned the official toll. Prosecutors have warned that anyone who spreads “false news” about the coronavirus can face a prison sentence of up to five years.
And the government has waged a bitter feud with doctors who earlier revolted in the pandemic over lack of protective equipment. Some of the doctors were thrown in jail.
“They’re trying to control the narrative, they’re trying to make sure things look like they’re under control, and part of that is controlling the information that is being shared with the public,” Sabae said. “I have no problem with that if the government gives us credible information that we can rely on.”
When the El Husseineya Central Hospital video came out instead, the answer was to tell the Egyptians not to believe what they were seeing.
“This is not a scene showing a lack of oxygen,” said Mamdouh Ghorab, the governor of Al Sharqiya, the governorate that also includes El Husseineya Central Hospital. He spoke on a pro-government television show that did not interview or invite witnesses to question the official narrative.
Even the official numbers are suspect. Egypt has reported over 150,000 Covid cases and over 8,000 deaths, remarkably low numbers for the region and for a country of over 100 million people.
However, outside experts and even some government officials say both numbers are a huge undercount, largely due to the lack of comprehensive testing and because the laboratories that run tests don’t always report their results to the government.
Although the lack of oxygen at El Husseineya Central was denied, officials began taking steps to address the problem and tacitly acknowledged it.
Health Minister Hala Zayed recognized a shortage of oxygen delivery trucks and delays in distribution. President Sisi called on the government to double oxygen production to meet the surge in demand.
The government appears to have taken another action in response to the video of the crisis in El Husseineya Central. Visitors must now leave their phones at the door.
Mona El-Naggar reported from El Husseineya and Yousur Al-Hlou from New York. Video by Arielle Ray and Ben Laffin.