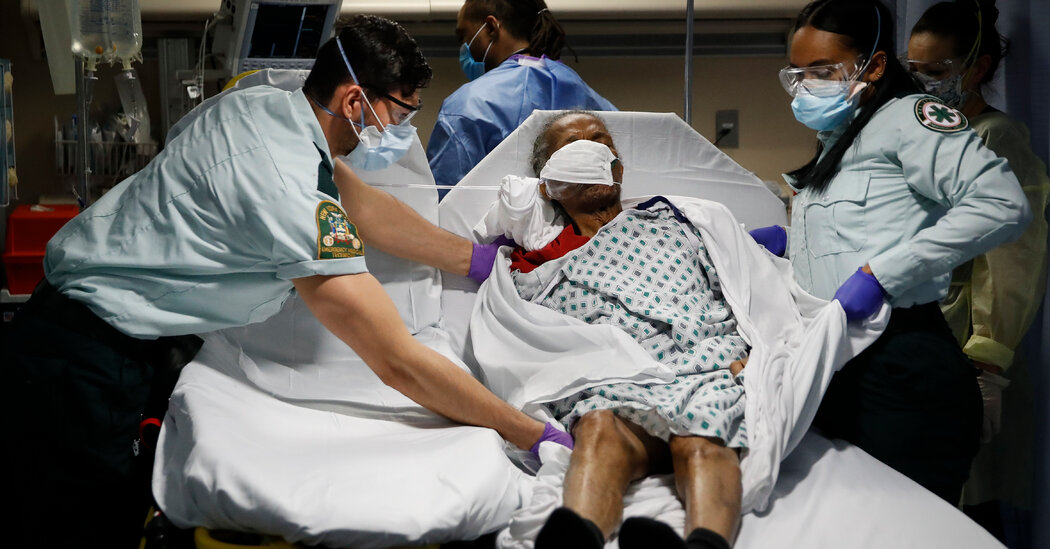
Exceptionally high turnover among nursing home workers likely contributed to the shocking number of deaths in facilities during the pandemic, the authors of a new study suggested.
The study, published Monday in Health Affairs, a health policy journal, provides a comprehensive overview of turnover rates in 15,645 nursing homes across the country, taking into account nearly all federal government certified facilities. The researchers found that the average annual rate was 128 percent, with some facilities having sales in excess of 300 percent.
“It was really breathtaking,” said David Grabowski, professor of health policy at Harvard Medical School and one of the study’s authors. Researchers pointed to the results to urge Medicare to publish staff turnover rates at individual locations in nursing homes to highlight substandard conditions and pressure owners to make improvements.
Inadequate staffing – and low wages – have long plagued nursing homes and the quality of care for the more than one million residents who live in these facilities. However, the pandemic has exposed these issues even more sharply. Investigations are ongoing by some states to monitor the facilities as cases in Covid are uncontrolled and deaths have skyrocketed.
The high turnover rate likely made it harder for nursing homes to conduct strong infection controls during the pandemic and led to widespread spread of the coronavirus, said Ashvin Gandhi, lead author and health economist and assistant professor at the University of California Los Angeles Anderson School of Management.
Nursing home owners blame Medicaid, the state’s program for the care of the skilled elderly, for the inadequate reimbursement.
“Recruiting and retaining workers is one of the most pressing challenges facing long-term carers and we have been calling for help for years,” said Dr. David Gifford, chief medical officer of the American Health Care Association and the National Center for Assisted Living Trading Group, said in an email statement.
“It is high time providers were given the right resources to invest in our frontline caregivers to improve the quality of care,” he said.
At least 172,000 deaths from the virus had been reported among residents or employees of nursing homes and other long-term care facilities by the end of February, according to a database compiled by the New York Times. The death toll in nursing homes alone has caused more than a third of all Covid deaths in the United States, although mortality and case rates have fallen sharply as more than 70 percent of residents have received vaccinations.
Industry criticism has also centered on the decade-long ownership of nursing homes by private equity and other private investment firms, where profits for investors took precedence over residents’ welfare. These owners have long been accused of under-staffing their facilities and underpaid workers.
Updated
March 1, 2021, 9:49 p.m. ET
Labor is one of the primary costs of running a nursing home, said Dr. Gandhi. “It’s generally not a very high-margin industry,” he said. “Any institution trying to maximize its profits will think carefully about its staffing costs.”
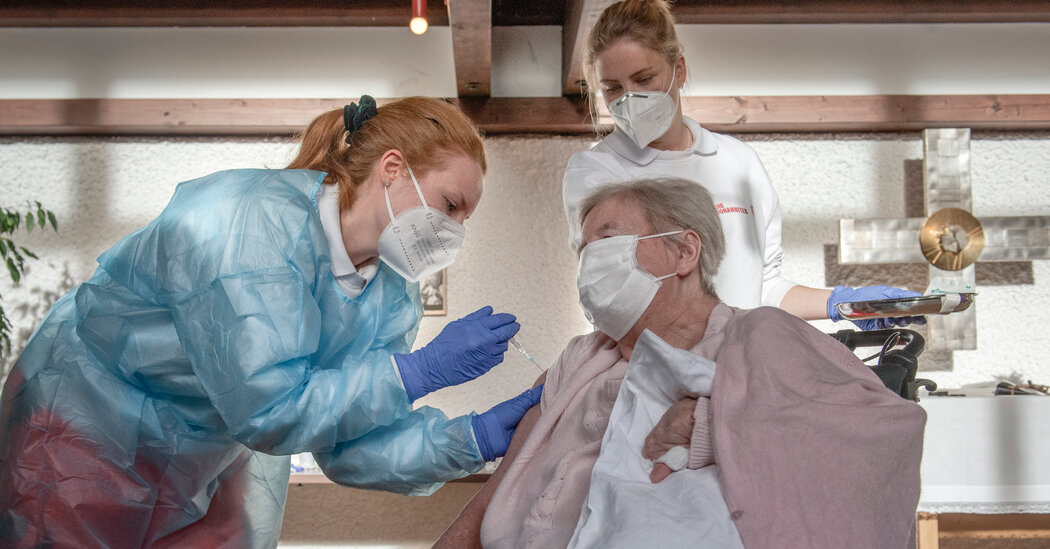
Nursing home staff have also shown resistance to being vaccinated against the coronavirus, making it difficult for public health officials and nursing homes to provide comprehensive vaccination coverage for a single facility. If a vaccinated nurse leaves the hospital and is replaced, the facility must ensure that the new employee is vaccinated as well, especially given the reluctance of some workers to receive a coronavirus shot.
“Trying to get a single shot is not enough,” said Dr. Gandhi. “You need continuous vaccination work.”
Registered nurses, who are the most skilled workers, had the highest turnover rates, and turnover varied widely across institutions. The states with the highest rates included Oklahoma, Montana, and Kansas. Facilities with low star ratings on the Medicare website that compared nursing homes had the highest average sales and nursing homes with high ratings had the lowest sales. Revenue was also higher at for-profit organizations owned by chains that serve Medicaid beneficiaries, according to the study.
Melissa Unger, the executive director of SEIU 503, a division of the Service Employees International Union in Oregon, said nurses have difficulty working in facilities with too few employees to adequately care for residents.
“You don’t feel good about the work you do,” said Ms. Unger, noting that many of the employees are women and people of color. “They’re doing all of this for shitty benefits and low wages.”
Summer Trosko, a union member who works at a nursing home in Oregon, said she was used to colleagues leaving burnout because of under-staffing and lack of funds. “You get tired and just can’t take it anymore and stop,” she said. Many are being replaced with people who have just graduated from high school with little education, she said.
In addition to making turnover rates available to the public, the authors point out a number of steps lawmakers could take to improve retention. Medicare could include sales in its star rating system, and Medicare and Medicaid could reward nursing homes with higher rates when they had lower sales. “If we want to change nursing homes, we have to start with the staff,” said Dr. Grabowski.
Researchers used newly available payroll-based data collected by the Centers for Medicare and Medicaid Services for Registered Nurses, Licensed Practical Nurses, and Certified Nursing Aides to calculate turnover rates in 2017 and 2018. They looked at the percentage of hours a care worker worked in a given year and calculated higher rates if the person who left the company had done more care.