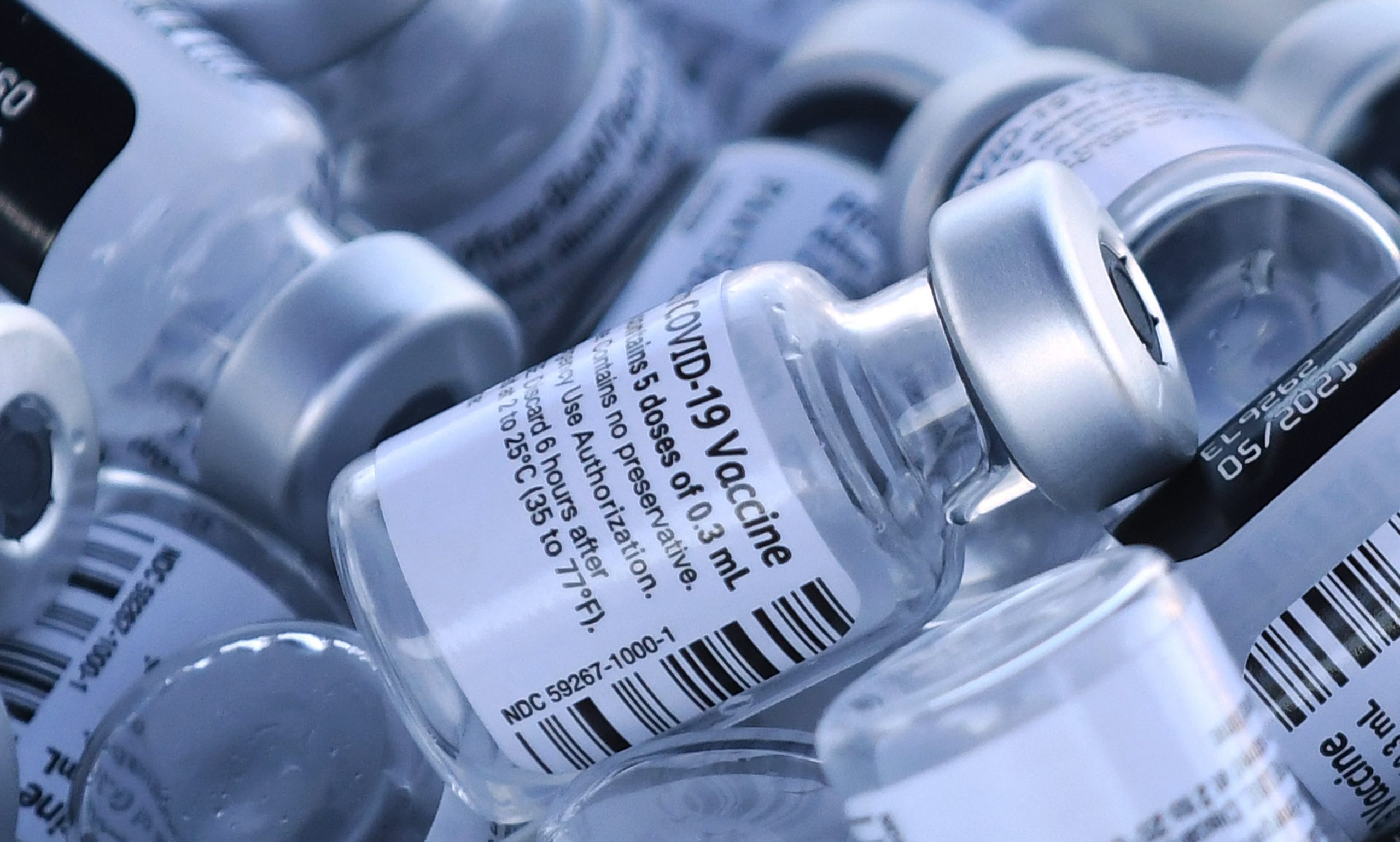
In the past few weeks, scientists have been raising the alarm about new variants of the coronavirus that carry a handful of tiny mutations, some of which appear to make vaccines less effective.
But it’s not just these small genetic changes that are cause for concern. The novel coronavirus tends to mix up large chunks of its genome when making copies of itself. Unlike small mutations, which are like typos in sequence, a phenomenon called recombination is similar to a large copy-and-paste mistake, where the second half of a sentence is completely overwritten with a slightly different version.
A number of new studies suggest that recombination can allow the virus to transform itself in dangerous ways. In the long run, however, this biological machinery could provide a silver lining in helping researchers find drugs that will stop the virus.
“There’s no question that recombination is taking place,” said Nels Elde, an evolutionary geneticist at the University of Utah. “And in fact, it’s probably a little underrated and could even play a role in creating some of the new worrying variants.”
The coronavirus mutations that most people have heard of, like the one in the B.1.351 variant first discovered in South Africa, are changes in a single “letter” of the virus or RNA’s long genetic sequence. Because the virus has a robust system for proofreading its RNA code, these small mutations are relatively rare.
In contrast, recombination is widespread in coronaviruses.
Researchers at Vanderbilt University Medical Center, led by virologist Mark Denison, recently looked at how replication goes wrong in three coronaviruses, including SARS-CoV-2, which causes Covid. The team found all three viruses showed “extensive” recombination when replicated separately in the laboratory.
Scientists fear that recombination could combine different variants of the coronavirus into more dangerous versions in a person’s body. For example, variant B.1.1.7, first discovered in Great Britain, had more than a dozen mutations that appeared suddenly.
Dr. Elde said the recombination may have brought together mutations from different variants that may have arisen spontaneously within the same person over time or that co-infected someone at the same time. At the moment this idea is speculative: “It’s really hard to see these invisible scars from a recombination event.” And while it is possible to get infected with two variants at the same time, this is considered rare.
Katrina Lythgoe, an evolutionary epidemiologist at the Oxford Big Data Institute in the UK, is skeptical that co-infection is common. “But the new worrying variants have taught us that rare events can still have a big impact,” she added.
Recombination may also allow two different coronaviruses from the same taxonomic group to exchange some of their genes. To investigate this risk more closely, Dr. Elde and his colleagues tracked the genetic sequences of many different coronaviruses, including SARS-CoV-2 and some of its distant relatives that are known to infect pigs and cattle.
Using specially developed software, the scientists highlighted the places where the sequences of these viruses aligned and matched – and where they did not. The software suggested that in the last few centuries of virus evolution, many of the recombination events involved segments that made up the spike protein that helps the virus enter human cells. This is worrying, the scientists said, because it could be one way that one virus essentially infects another virus.
“Through this recombination, a virus that cannot infect humans could recombine with a virus like SARS-CoV-2 and take over the sequence for the tip and infect people,” said Stephen Goldstein, an evolutionary virologist who worked on the study.
Updated
Apr. 5, 2021, 8:13 p.m. ET
The results, which were posted online on Thursday but not yet published in a scientific journal, provided new evidence that related coronaviruses are quite promiscuous in terms of recombining with one another. There were also many sequences that appeared in the coronaviruses that seemed to come out of nowhere.
“In some cases, it almost looks like a sequence is coming from space, from coronaviruses that we don’t even know about,” said Dr. Elde. The recombination of coronaviruses across completely different groups has not been studied in detail, also because such experiments may have to be subject to a government review in the USA due to security risks.
Feng Gao, a virologist at Jinan University in Guangzhou, China, said that while the Utah researchers’ new software found unusual sequences in coronaviruses, it does not provide any iron evidence of recombination. It could just be that that’s how they evolved.
“Diversity, no matter how much, doesn’t mean recombination,” said Dr. Gao. “It could well be caused by tremendous diversification during virus development.”
Scientists have limited knowledge of whether new pandemic coronaviruses can arise through recombination, said Vincent Munster, a viral ecologist at the National Institute for Allergies and Infectious Diseases who has been studying coronaviruses for years.
Yet this evidence is growing. In a study published in July and officially published today, Dr. Munster and coworkers suggest that recombination is likely, as both SARS-CoV-2 and the virus behind the original SARS outbreak in 2003 resulted in a version of the spike protein that enables them to skillfully invade human cells. This spike protein binds to a specific entry point in human cells called ACE2. This paper calls for stronger coronavirus surveillance to see if there are others who are using ACE2 and therefore may pose similar threats to humans.
Some scientists are studying recombination machinery not only to ward off the next pandemic, but also to combat it.
For example, Dr. Vanderbilt’s Denison, in his recent study of the recombination of three coronaviruses, found that blocking an enzyme known as nsp14-ExoN in a mouse coronavirus caused a decrease in recombination events. This suggests that the enzyme is critical to the ability of coronaviruses to mix and match their RNA during replication.
Now, Dr. Denison and Sandra Weller, virologist at the University of Connecticut Medical School, asked whether this finding could treat people with Covid.
Certain antiviral drugs, like remdesivir, fight infection by acting as RNA bait that speeds up the viral replication process. But these drugs don’t work as well as some coronaviruses would have hoped. One theory is that the enzyme nsp14-ExoN removes the errors caused by these drugs and thus saves the virus.
Dr. Denison and Dr. Among other things, Weller are looking for drugs that block the activity of nsp14-ExoN and allow remdesivir and other antiviral agents to work more effectively. Dr. Weller compares this approach to cocktail therapies for HIV, which combine molecules that act on different aspects of virus replication. “We need combination therapy for coronavirus,” she said.
Dr. Weller notes that coronaviruses share nsp14-ExoN, so a drug that successfully suppresses it can work against more than just SARS-CoV-2. You and Dr. Denison are still in the early stages of drug discovery and are testing various molecules in cells.
Other scientists see potential in this approach not only to make drugs like remdesivir work better, but also to prevent the virus from correcting one of its replication errors.
“I think it’s a good idea,” said Dr. Goldstein, “because you would drive the virus into what is known as a ‘failure catastrophe’ – basically it would mutate so severely that it is fatal to the virus.”