Within a few weeks, two variants of the coronavirus have become so popular that you can regularly hear their unfathomable alphanumeric names on the television news.
B.1.1.7, first identified in the UK, has demonstrated the ability to spread widely and quickly. In South Africa, a mutant called B.1.351 can evade human antibodies and affect the effectiveness of some vaccines.
Scientists have also kept an eye on a third variant that originated in Brazil and is called P.1. Research on P.1 had been slower since its discovery in late December, so scientists weren’t sure how much to worry about it.
“I held my breath,” said Bronwyn MacInnis, an epidemiologist at the Broad Institute.
Now three studies offer a sobering story of P.1’s meteoric rise in the Amazonian city of Manaus. It most likely occurred there in November and then led to a record spike in coronavirus cases. It came to dominate the city in part because of an increased risk of contagion, research found.
However, the ability to infect some people who had immunity to previous attacks from Covid-19 was also gained. And laboratory experiments suggest that P.1 could weaken the protective effects of a Chinese vaccine currently used in Brazil.
The new studies have yet to be published in scientific journals. Their authors warn that findings from cells in laboratories do not always translate into the real world, and they have only just begun to understand how P.1 behaves.
“The results apply to Manaus, but I don’t know if they apply to other locations,” said Nuno Faria, a virologist at Imperial College London who led much of the new research.
But even with the puzzles that existed around P.1, experts said it was a variant that should be taken seriously. “It is right to be concerned about P.1, and this data gives us the reason why,” said William Hanage, epidemiologist at Harvard TH Chan School of Public Health.
P.1 is now spreading across the rest of Brazil and has been found in 24 other countries. In the United States, the Centers for Disease Control and Prevention has registered six cases in five states: Alaska, Florida, Maryland, Minnesota, and Oklahoma.
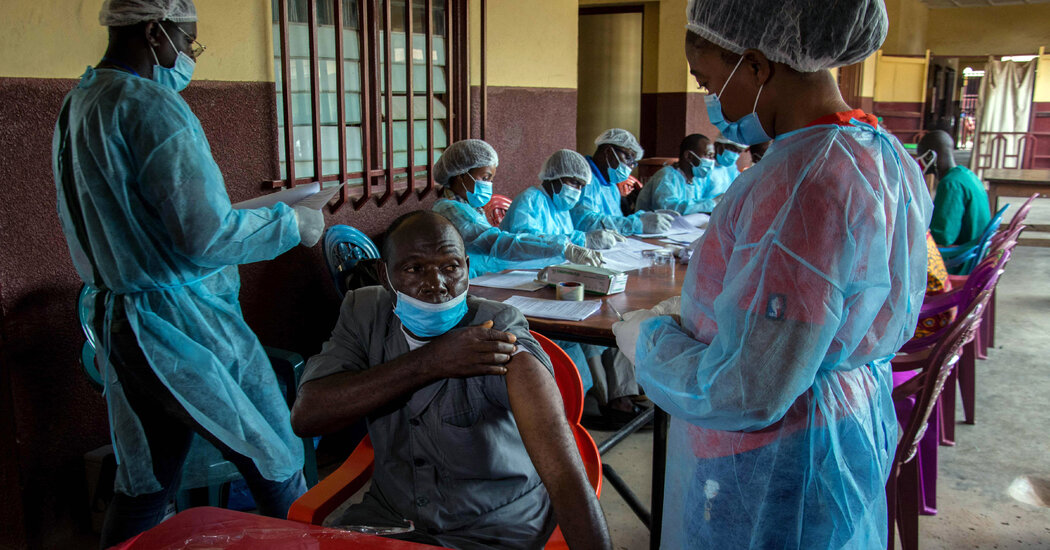
To reduce the risk of P.1 outbreaks and reinfections, Dr. Faria, it is important to double up on any measure to slow the spread of the coronavirus. Masks and social distancing can work against P.1. And vaccinations can help reduce transmission and protect those who become infected from serious illnesses.
“The ultimate message is that you need to step up all vaccination efforts as soon as possible,” he said. “You have to be one step ahead of the virus.”
Dr. Faria and his colleagues began tracking down the coronavirus when it exploded in Brazil last spring. Manaus, a city of two million people in the Brazilian Amazon, was particularly hard hit. At the height of spring, the Manaus cemeteries were overwhelmed by the corpses of the dead.
But after a peak in late April, Manaus appeared to have overcome the worst of the pandemic. Some scientists believed the decline meant Manaus had gained herd immunity.
Dr. Faria and his colleagues looked for coronavirus antibodies in samples from a Manaus blood bank in June and October. They found that roughly three-quarters of Manaus residents were infected.
However, towards the end of 2020, the number of new cases increased again. “There were actually far more cases than the previous peak of cases, which was in late April,” said Dr. Faria. “And that was very puzzling to us.”
To look for variants, Dr. Faria and his colleagues launched a new genome sequencing effort in town. While B.1.1.7 had arrived in other parts of Brazil, they did not find it in Manaus. Instead, they found a variant that no one had seen before.
Updated
March 1, 2021, 9:49 p.m. ET
Many variants in their samples shared a set of 21 mutations that were not seen in other viruses circulating in Brazil. Dr. Faria texted a colleague, “I think I’m seeing something really strange and I’m pretty worried about it.”
Some mutations in particular worried him, as scientists had already found them in B.1.1.7 or B.1.351. Experiments suggested that some of the mutations might make the variants better able to infect cells. Other mutations allow them to evade antibodies from previous infections or to be produced by vaccines.
While Dr. Faria and his colleagues analyzed their results, researchers in Japan made a similar discovery. Four tourists who returned home from a trip to the Amazon on Jan. 4 tested positive for the coronavirus. Genome sequencing revealed the same mutations that Dr. Faria and his colleagues in Brazil saw.
Dr. Faria and his colleagues posted a description of P.1 on an online virology forum on January 12th. Then they investigated why P.1 is so common. Its mutations could have made it more contagious, or it could have been lucky. Coincidentally, the variant might have surfaced in Manaus when the city became more relaxed about public health policies.
It was also possible that P.1 became common because it could re-infect people. Usually, coronavirus reinfections are rare as the antibodies produced by the body after infection are effective for months. However, it was possible that P.1 had mutations that made it difficult for these antibodies to attach to it, allowing them to slip into cells and cause new infections.
The researchers tested these possibilities by tracking P.1 from its earliest samples in December. At the beginning of January it was 87 percent of the samples. By February it had completely taken over.
The researchers combined the data from genomes, antibodies and medical records in Manaus and came to the conclusion that P.1 conquered the city thanks to biology rather than luck: its mutations contributed to its spread. Like B.1.1.7, it can infect more people on average than other variants. They estimate that it is between 1.4 and 2.2 times more transmissible than other coronavirus lineages.
But it also gets a benefit from mutations that allow antibodies from other coronaviruses to escape. They estimate that out of 100 people who were infected in Manaus last year, between 25 and 61 were re-infected by P.1.
The researchers found support for this conclusion in an experiment in which they mixed P.1 virus with antibodies from Brazilians who had Covid-19 last year. They found that the effectiveness of their antibodies against P.1 decreased six-fold compared to other coronaviruses. This decline could mean that at least some people are susceptible to new infections from P.1.
“There seems to be a growing body of evidence to suggest that most of the second wave-related cases are actually some kind of reinfection,” said Dr. Faria.
Dr. Faria and other researchers are now looking across Brazil to observe the spread of P.1. Dr. Ester Sabino, an infectious disease expert at the University of São Paulo Faculty of Medicine, said one of the new outbreaks has occurred in Araraquara, a Brazilian city of 223,000 that did not have high rates of Covid-19 before P.1 arrived.
If the people of Araraquara did not have high antibody levels prior to P.1’s arrival, it suggests that the variant may have spread to locations without Manaus’ extreme history. “This could happen in any other place,” she said.
Michael Worobey, a virologist at the University of Arizona who was not involved in the research, said it was time to pay attention to P.1 in the US. He expected it to become more common in the United States, although it would have to compete with B.1.1.7, which could soon become the predominant variant in much of the nation.
“At least it will be one of the competitors,” said Dr. Worobey.
In their experiments, Dr. Faria and his colleagues also received antibodies from eight people who received CoronaVac, a Brazilian-made vaccine that was used in Brazil. They found that the antibodies produced by the vaccine were less effective at stopping the P.1 variant than other types.
Dr. Faria warned that these results, taken from cells in test tubes, don’t necessarily mean vaccines are less effective at protecting real people from P.1. Vaccines can very well provide strong protection against P.1, even if the antibodies they produce are not quite as effective. And even if the variant manages to infect vaccinated people, they will most likely remain protected from a severe attack of Covid-19.
For Dr. Sabino is the ultimate meaning of P.1 the threat that variants pose if they can appear anywhere in the world.
“It’s just a matter of time and chance,” she said.