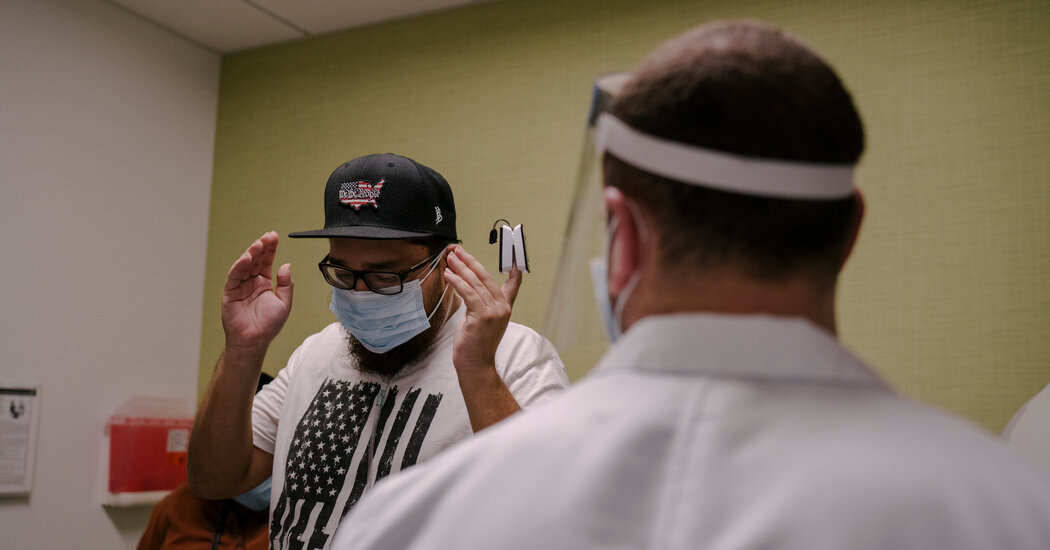
LOS ANGELES – Three days after his release from Martin Luther King Jr. Community Hospital, Gilbert Torres returned on a stretcher. A clear hose snaked from his nose to an oxygen tank. It was the last place he wanted to be.
But 30-year-old Torres, who had just spent two weeks in intensive care on a ventilator, was absent because his condition had worsened. He was there to visit a new outpatient clinic for Covid-19 survivors, to treat their remaining physical and psychological wounds – and to prevent them from having to be readmitted.
Several medical centers across the country, including Massachusetts General Hospital, have set up similar clinics, a sign that the need to address the long-term effects of Covid is increasingly recognized. Other hospitals that already had aftercare programs in the intensive care unit have added large numbers of Covid patients to their list: Indiana University Health Methodist Hospital, for example, has treated more than 100 patients. And some facilities, like Providence St. Jude in Fullerton, Calif., Have been doing recovery programs that also serve coronavirus patients who have never been hospitalized.
“We put a thousand percent of our energy into these patients,” said Dr. Jason Prasso, one of the intensive care physicians at the MLK hospital who started the clinic there. “We feel responsible for ensuring that they feel better after they leave the hospital.”
Long before the pandemic, doctors knew that some patients recovering from critical illness developed a constellation of symptoms known as post-intensive care syndrome, which can include muscle weakness and fatigue. Depression, anxiety, and cognitive impairment occur in about half of people who have spent time on ventilators in an intensive care unit. About a quarter of these patients develop post-traumatic stress disorder. The risk is higher in patients who have stopped breathing, have long hospital stays, and are being treated with medication to calm or paralyze – all of which are common in sick coronavirus patients. A new, peer-reviewed study of 45 ex-ICU patients with Covid-19 at Mount Sinai Hospital in New York found that more than 90 percent met the criteria for the syndrome.
Dr. Prasso and his colleagues started the clinic at MLK after discovering that many of the patients whose lives they had saved received little follow-up care. The hospital is in a low-income neighborhood where health services, which were inadequate before the pandemic, have become increasingly scarce.
Since opening in August, the clinic has seen more than 30 patients. Visits that take place on Tuesday morning and include a physical exam and mental health screening often involve discussions about housing, food security, and employment issues that can arise from long-term symptoms. Spiritual care is also offered to patients.
The first to go to Mr. Torres’ exam room in February was Rudy Rubio, a hospital chaplain who had often visited him in the intensive care unit. The pastor asked if they could pray together and offered to get him a Bible.
Mr Torres, whose parents fled the war in El Salvador, grew up in the neighborhood cleaning large rigs in a Blue Beacon truck wash. Although he was morbidly obese – a risk factor for severe Covid – he liked to run and cycle and was rarely needed to see a doctor. Little did he know how he got infected with the coronavirus or got so sick that doctors had to insert a breathing tube within hours of arriving at MLK. Before he showed any signs of improvement, they feared that he would not survive.
“You were spared,” said the chaplain in the clinic. “What are you going to do with this opportunity?”
When Dr. Prasso entered the room, Mr. Torres did not recognize him at first without protective clothing and helmet. “It was you,” he said when realization dawned.
When the doctor examined him, Mr Torres said he could walk short distances, but feared that if he did, his oxygen levels would drop. “It’s a bit of a mind game,” said Dr. Prasso. “You may feel short of breath, but your oxygen may still be completely normal.”
The clinic would ensure Mr. Torres got a portable oxygen machine as small tanks are in short supply nationally, the doctor said. He explained that it could take a few weeks to several months for patients to be weaned. Some may need it indefinitely.
Updated
April 1, 2021, 11:02 p.m. ET
Mr Torres raised another problem. A physiotherapist who was supposed to visit him had canceled. “Many of the agencies are a little bit against going into people’s homes because of Covid,” said Dr. Prasso. He said the clinic could instead enroll Mr. Torres on a pulmonary rehabilitation program so that he could work with therapists who would focus on restoring his lungs.
Mr Torres said he was concerned and was haunted by memories of ICU monitors beeping and a feeling of suffocation. He had hardly slept since his return and had not yet seen his 5-year-old son, who was temporarily living with grandparents. Mr. Torres was afraid of collapsing in front of him.
“Everything you feel is normal,” said Dr. Prasso. “Just know that what you went through was trauma. It takes time for this to heal. “
The two exchanged memories of the moment when Mr. Torres’ breathing tube was removed. “You asked me to take the tube out and as soon as we took the tube out you asked for it to be put back in,” said Dr. Prasso.
“It was hard to breathe,” said Mr Torres. “I didn’t want to be awake.”
“This guy had a vice handle on my hand,” said Dr. Prasso to Mr. Torres’ partner, Lisseth Salguero, who had joined him in the exam room. Family members who are themselves at risk for mental health problems are encouraged to accompany patients to the clinic. Ms. Salguero had developed Covid symptoms on the same day as Mr. Torres but recovered quickly. Since he had returned home she had woken up to check Mr. Torres’ oxygen levels at night. “I’m happy as long as he’s okay,” she said.
The extraordinary stress of being in intensive care during the Covid-19 era is often compounded by almost unbearable loneliness. Visitor restrictions designed to lessen the transmission of the virus can mean weeks apart from loved ones. “I kept asking for someone to hold my hand,” Mr. Torres recalled. “I wanted contact.”
The employees became de facto family. “You have no one but your nurses,” said Mr Torres.
For these ICU carers, caring for Covid patients while being among the few connections to their family leads to deep emotional ties. Nina Tacsuan, one of Mr. Torres’ nurses, couldn’t hold back her tears when she saw him in the clinic.
“Thank you for keeping me alive and for giving me a second chance,” Mr. Torres said to her. “I’m thankfull.”
“You are my age,” said Ms. Tacsuan. “It was just very difficult all along.”
Often the experience ends with heartbreak: at the time of Mr. Torres’s hospitalization, only about 15 percent of Covid patients at MLK treated with ventilators had survived to go home.
Those who survive, like him, inspire employees to keep going. As a rule, however, intensive care workers have no way of seeing their ex-patients once they are better. The clinic has changed that.
Ms. Tacsuan and a nurse manager, Anahiz Correa, joked that Mr. Torres was no longer welcome in their intensive care unit
When the ambulance picked him up to go home, Mr Torres said he was feeling much better than when he arrived. He reunited with his young son Austin a few days later and has continued to improve over the past few weeks.
Mr. Torres visited the clinic twice more, in February and March. Although he refused outpatient rehabilitation and instead chose to climb stairs and do other exercises at home, he said he felt cared for and was glad to have left.
A social worker there connected him to a family doctor in the MLK system for further follow-up examinations. An osteopath manipulated his back and taught him to stretch to alleviate the persistent discomfort from his time in the hospital bed. And last week, at his last appointment, the clinic put up a congratulatory banner shouting, “Surprise!” As he walked in to mark his “graduation” because he didn’t need to use an oxygen tank.
He said he needed more strength and stamina to return to his physically demanding truck wash job, but “I do a lot more things.” And fear is no longer haunted by him, he added. “I feel great.”