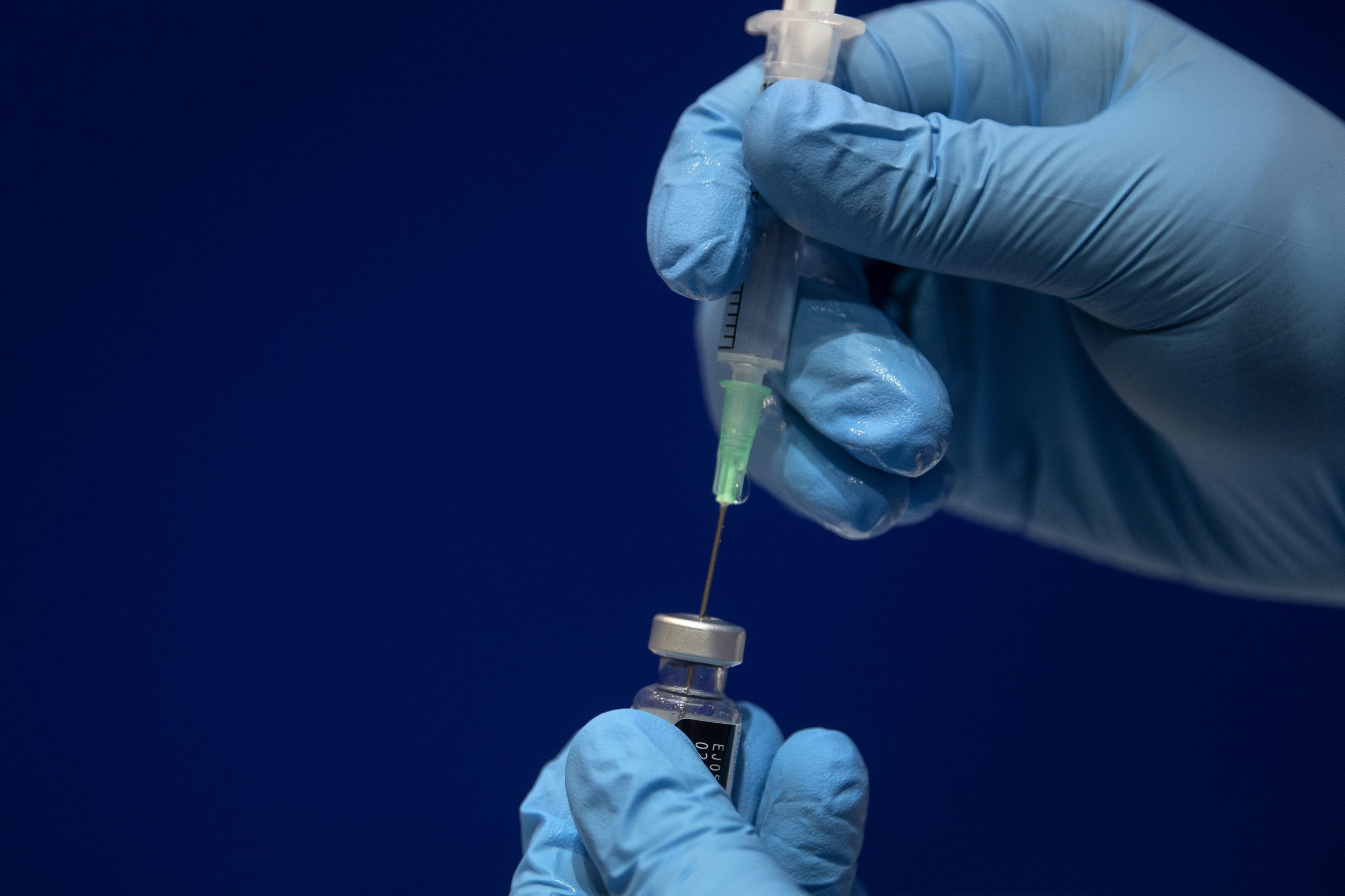
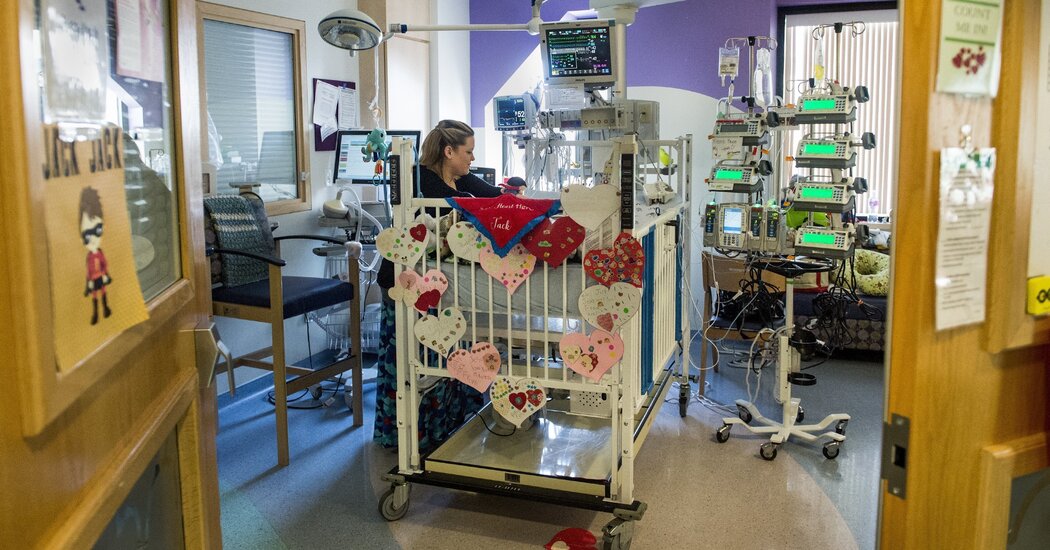
An ambulance crew waits with a patient outside the Coast Plaza Hospital emergency room during a surge in coronavirus disease (COVID-19) cases in Los Angeles, California on December 26, 2020.
David Swanson | Reuters
The Covid-19 outbreak is so severe in Los Angeles County that ambulances have to wait hours to drop patients off to emergency rooms.
Hospital beds are cluttered in souvenir shops, cafeterias, and conference rooms as hospitals struggle to find space for patients.
The Los Angeles County Emergency Services Department on Monday urged EMS workers to only administer supplemental oxygen when a patient’s saturation level drops below 90% in order to reduce oxygenation. Paramedics have also been advised not to transport adult heart attack patients to hospital unless they can restore “spontaneous circulation” in the field – to focus care on patients who are more likely to survive.
Los Angeles is facing an unprecedented surge in coronavirus patients that is marginalizing hospitals in the area. Public health officials warn that the already dire situation is likely to worsen in January.
“Many hospitals have reached a crisis point and are facing very difficult decisions about patient care,” said Dr. Christina Ghaly, the district’s health manager, at a press conference on Monday. She urged residents to avoid the emergency room unless they need serious medical attention.
Hospitals have reached their limits since Decemer, when the region’s intensive care unit capacity quickly dropped to zero, according to state health officials. More than 8,000 people have now been hospitalized with the virus in the county, and 20% of those people are in intensive care units, data from the county health department shows. With the virus so prevalent, public health officials warn that conditions are likely to get worse before they improve.
Paramedics (EMTs) and health care workers treat patients outside the Huntington Park Community Hospital emergency room during a surge in positive coronavirus disease (COVID-19) cases in Huntington Park, California, December 29, 2020.
Bing Guan | Reuters
Across California, approximately 370 people die from Covid-19 every day based on a weekly average – a nearly 46% increase compared to a week ago. This comes from a CNBC analysis of the data compiled by Johns Hopkins University.
In Los Angeles County, the coronavirus kills someone every 15 minutes on average, the county’s public health director Barbara Ferrer said during Monday’s briefing. The county exceeded a total of 11,000 deaths from Covid-19 on Tuesday, 1,000 of which occurred in less than a week, the health department said in a statement.
Everyone in the area should assume they will be exposed to the disease if they leave their home, Ferrer said. One in five people tested for Covid-19 in Los Angeles County has the virus.
“We’re likely to see the worst of conditions in January facing the entire pandemic, and that’s hard to imagine,” Ferrer said. “The rise in cases is likely to continue for weeks due to holiday and New Year’s parties and returning travelers.”
The staff was stretched thin
Los Angeles County is still grappling with the Covid-19 spate that was sparked by the Thanksgiving holiday and has yet to see the cases that are likely to follow the holidays in late December, Ghaly said. Hospitals are now trying to “do everything they can to prepare”.
Some coronavirus patients have to wait more than a day for a bed to be opened for them in the intensive care unit, shared Dr. Brad Spellberg, chief medical officer of the Los Angeles County University Medical Center’s Southern California Medical Center, emailed CNBC.
A health care worker examines patients in an oxygen tent outside the emergency room of Huntington Park Community Hospital during a surge in positive coronavirus (COVID-19) cases in Huntington Park, California, December 29, 2020.
Bing Guan | Reuters
The hospital had to recruit some of its health care workers to handle the influx of ICU patients, meaning there is no time for elective surgery or other life-saving procedures like colonoscopies, Spellberg said.
Governor Gavin Newsom said during a news conference Monday that the state had sent medical aid teams to the Los Angeles area to ease the burden on hospitals. However, if there is another spike in Covid-19 cases after the December break, the extra staff won’t be enough, Spellberg said.
“Our staff are still very thin, especially in the intensive care unit. You can’t just get more nurses and doctors in the intensive care unit,” Spellberg said in an email, urging people to continue following public health guidelines such as wearing of masks, physical distancing and avoiding the crowds to follow.
“We get knocked down”
The increase is due to the fact that California, along with other states in the United States, began to administer the first shots of Covid-19 vaccines from Pfizer and Moderna.
The state has received just over 2 million doses of vaccines, but only 24% of those have been given, according to the state’s Department of Health’s database last updated Wednesday. Newsom said Monday the process is too slow and the state “wants to see things go much faster”.
Ravina Kullar, a Los Angeles-based infectious disease expert and a member of the Infectious Diseases Society of America, told CNBC in a telephone interview that she expects vaccinations to speed up in the coming weeks, even though the shots won’t work immediately. Immunity takes a few weeks to build and too few are given to develop herd immunity that would protect the wider population.
“I think we’re going to see some sort of stability that plateau and decrease in some cases, but it will only take time,” said Kullar. “I think it will be until spring, summer, before something really becomes noticeable there.”
Kullar, who works in long-term care facilities and nursing homes in Los Angeles, said every facility she works with is battling a Covid-19 outbreak. These residents, along with health care workers, will be the first to receive vaccination shots in California when they are introduced, Newsom said, adding that there are approximately 3 million people in the state’s early stages of vaccination.
“We’re getting down,” said Kullar. “We have very few staff. I am exhausted, my colleagues are exhausted. It’s a very difficult situation out here.”
– The Associated Press contributed to this report.