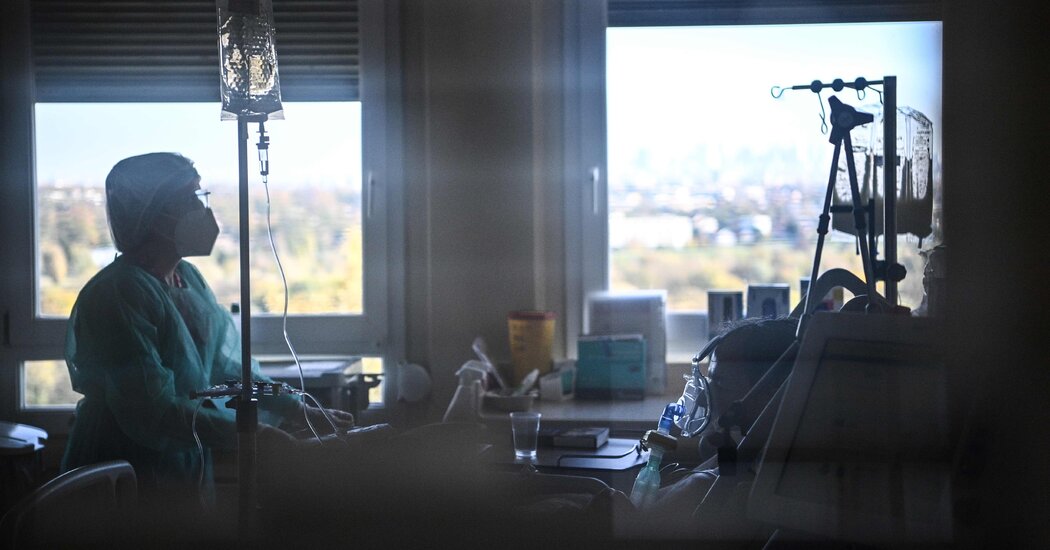
Gabrielle Dawn Luna sees her father with every patient she treats.
As a nurse in the emergency room at the same hospital where her father died of Covid in March last year, Ms. Luna knows firsthand what it is like for a family to hold onto any new information. She has become aware of the need to take extra time to explain developments to a patient’s family members who are frequently checking for updates.
And Mrs. Luna was willing to share her personal loss if it helps, as she recently did with a patient whose husband has died. But she also learned to hold it back to respect each person’s grief, as she did when a colleague’s father succumbed to the disease.
It is a challenge to let oneself grieve enough to help patients without feeling overwhelmed.
“Sometimes I think it’s too much of a responsibility,” she said. “But that’s the job I signed up for, isn’t it?”
The Lunas are a foster family. Her father, Tom Omaña Luna, was also a lifeguard and was proud when Mrs. Luna came to him in the field. When he died on April 9, Ms. Luna, who also had mild symptoms of Covid-19, took about a week off. Her mother, a nurse in a long-term care facility, then spent about six weeks at home.
“She didn’t want me to go back to work for fear that something would happen to me too,” said Ms. Luna. “But I had to go back. You needed me “
As her hospital in Teaneck, New Jersey swelled with virus patients, she struggled with stress, burnout, and an excruciating fear that left an open wound on her grief: “Did I give it to him? I don’t want to think about it, but it’s a possibility. “
Like the Lunas, many who treated millions of coronavirus patients in the United States last year come from medically defined families. It is a calling that is passed down through the generations and connects spouses and siblings who are states apart.
It’s a bond that brings the success of shared experiences, but for many, the pandemic has also brought a variety of fears and stresses with it. Many have been concerned about the risks they are taking and those their loved ones are exposed to every day. They worry about the invisible scars they have left.
And for those like Ms. Luna, the care they give coronavirus patients is shaped by the beloved healer they lost to the virus.
Working through grief
For Dr. Nadia Zuabi is so new to the loss that she still refers to her father, another ambulance in the present.
Your father, dr. Shawki Zuabi spent his final days at her UCI Health hospital in Orange County, California before dying of Covid on January 8th. The younger Dr. Zuabi returned to work almost immediately, hoping to carry on with the purpose and camaraderie of her colleagues.
She had expected that working with the people who had cared for her father would deepen her commitment to her own patients, and to some extent, too. Most importantly, she realized how important it is to balance this stressful emotional availability with her own well-being.
“I always try to be as empathic and compassionate as possible,” said Dr. Zuabi. “There is a part of you who may have to build a wall as a survival mechanism because I don’t think it’s sustainable to feel it all the time.”
The work is filled with memories. When she saw the fingertips of a patient, she remembered how her colleagues had also pricked her father’s to check insulin levels.
“He had all these bruises on his fingertips,” she said. “It just broke my heart.”
The two had always been close, but they found a special bond when she went to medical school. Doctors often descend from doctors. About 20 percent in Sweden have parents with medical degrees, and researchers believe the rate is similar in the United States.
The older Dr. Zuabi had a present for conversation and loved talking about medicine with his daughter as he sat in his living room chair with his feet propped up. She is still in her residency training and would reach out to him all last year for advice on the challenging Covid cases she was working on and he would dispel her doubts. “You have to trust yourself,” he told her.
Updated
March 13, 2021, 6:24 p.m. ET
When he caught the virus, she took each day off to be by his bedside and continued their conversations. Even when he was intubated, she pretended they were still talking.
She still does. After difficult shifts, she turns to her memories, the part of him that stays with her. “He really thought I was going to be a great doctor,” she said. “If that’s what my father thought of me, it must be true. I can do it, even if it doesn’t feel like it sometimes. “
Love tempered by risk and horror
Just as medicine is often a passion that arises from a set of values passed down from one generation to the next, so it is also one that is shared by siblings and that brings healers together in marriage.
A quarter of doctors in the US are married to another doctor, according to a study published in the Annals of Internal Medicine. Maria Polyakova, a professor of health policy at Stanford University, said she wouldn’t be surprised if the number of doctors in the U.S. who had siblings with medical degrees was about as high as the Swedish, about 14 percent.
In interviews with a dozen doctors and nurses, they described how helpful it has long been to have a loved one who knows the rigors of the job. But the pandemic has also shown how frightening it can be to put a loved one at risk.
A nurse’s brother took care of her when she had the virus before volunteering at another virus hotspot. A doctor chatted with her children about what would happen if she and her husband both died from the virus. And others described crying softly during a will talk after putting their children to bed.
Dr. Fred E. Kency Jr., a doctor at two emergency rooms in Jackson, Miss., Understood that he was surrounded by danger while serving in the Navy. He never expected that he would face such a threat in civil life or that his wife, an internist and pediatrician, would face the same dangers.
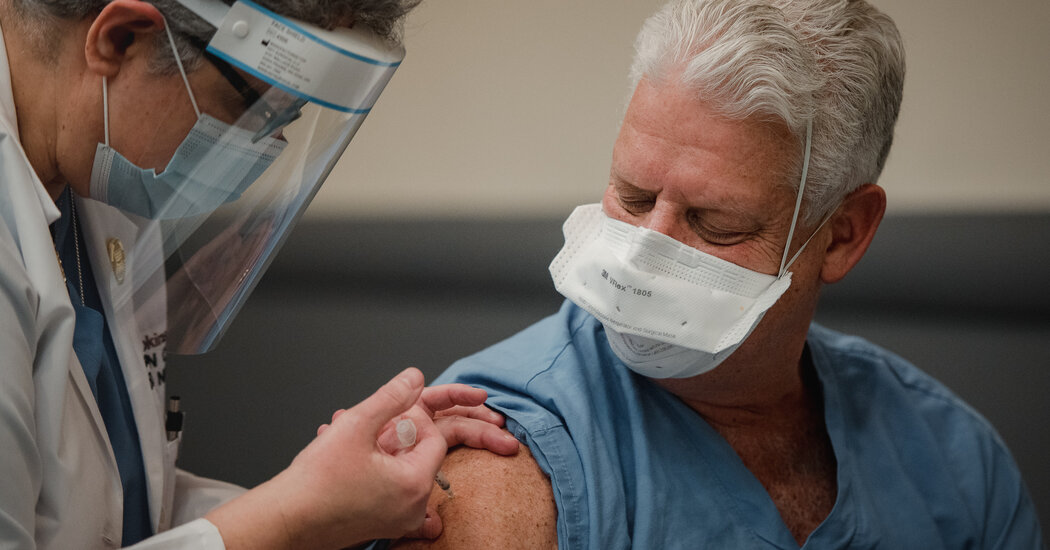
“It’s scary to know that my wife has to go to the rooms of patients with Covid every day,” said Dr. Kency before he and his wife were vaccinated. “But it is a reward to know that not just one of us, the two of us, are doing everything we can to save lives in this pandemic.”
The vaccine has eliminated fears of being vaccinated at work among vaccinated medical professionals, but some express deep concern at the toll that working in a year of horror has left their closest relatives.
“I am concerned about the amount of suffering and death she sees,” said Dr. Adesuwa I. Akhetuamhen, an emergency physician at Northwestern Medicine in Chicago, about her sister, the doctor at the Mayo Clinic in Rochester, Minn. I feel like I learned to deal with this while working in the emergency room before Covid started, but it’s not something that should be happening in her specialty as a neurologist. “
She and her sister, Dr. Eseosa T. Ighodaro, have been on the phone regularly to compare notes on the precautions they have taken, to update their families, and to support one another. “She totally understands what I’m going through and encourages me,” said Dr. Ighodaro.
The seemingly endless intensity of work, increasing deaths, and the careless attitudes of some Americans about safety precautions have caused anxiety, fatigue, and burnout in a growing number of healthcare workers. Almost 25 percent of them are most likely to have PTSD, according to a survey published by the Yale School of Medicine in February. And many have left the field or are considering doing so.
Donna Quinn, a midwife at NYU Health in Manhattan, has feared that her son’s experience as an ambulance doctor in Chicago will cause him to leave the field he recently came to. He was in his final year of residence when the pandemic started and he volunteered on the intubation team.
“I’m concerned about the toll he’s taking emotionally,” she said. “There were nights when we tearfully talked about what happened to us.”
She still has nightmares that are sometimes so terrible that she falls out of bed. Some are about her son or about patients she cannot help. In one, a patient’s bed linen is transformed into a towering monster that chases her out of the room.
The purpose of a nurse
When Ms. Luna first returned to her emergency room at Holy Name Medical Center in Teaneck, New Jersey after her father’s death, she felt that something was missing. She had got used to having him there. It had been nerve-wracking when she was asked, “Is that my father?” On every urgent intercom call after a resuscitation. But at least she could stop by now and then to see how he was doing.
Furthermore, she had never known what it was like to be a nurse without him. She remembered going to elementary school to step into the field and using a yellow highlighter to paint over almost every line in his large textbooks.
During breakfast last March, Ms. Luna told her father how upset she was after holding an iPad for a dying patient to say goodbye to a family who couldn’t go to the hospital.
“This is our job,” she recalled Mr. Luna. “We’re here to act as a family when the family can’t be there. It’s a difficult role. It will be difficult, and there will be more times that you have to do it. “
Kitty Bennett contributed to the research.