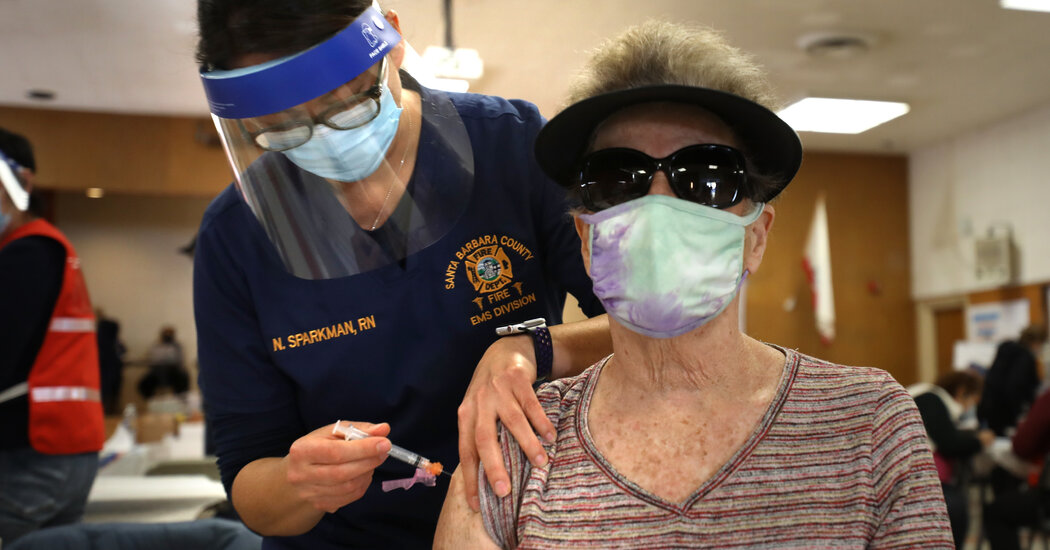
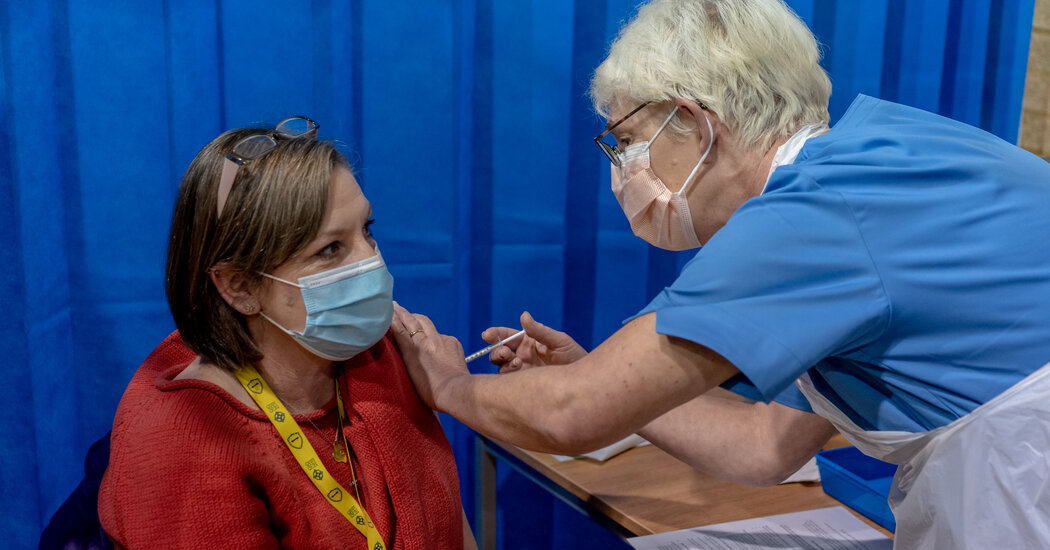
The Food and Drug Administration will hold a hearing this week to determine whether to grant emergency authorization to a coronavirus vaccine developed by Pfizer and BioNTech. The vaccine, which the companies claim is 95 percent effective, is one of two that could be ready for injections in the United States before the end of this year. The other, by Moderna, will be considered by the regulator for emergency approval next week. In early trials, the vaccine appeared to prevent the development of Covid-19 in around 94 percent of recipients.
The news is a welcome development in the otherwise grim saga of the fight against the coronavirus. The United States averages around 200,000 new cases each day, and more than 2,000 deaths.
An effective and widely available vaccine has long been promoted as the lifeline that will curb infections, save lives and pull a battered economy back from the brink. Yet the impending arrival of one or more vaccines raises questions about equity, education and how battered American institutions should prepare for the next pandemic, while repairing the damage wrought by this one.
As part of the DealBook D.C. Policy Project, The New York Times gathered a virtual panel of experts in early December to discuss the policy environment in a post-Covid world — or, at least, a post-Covid vaccine world.
The participants:
-
Ruth Faden, professor of bioethics at Johns Hopkins University
-
James E.K. Hildreth, professor of internal medicine, president and chief executive of Meharry Medical College
-
Marc Lipsitch, professor of epidemiology and director of the Center for Communicable Disease Dynamics at Harvard T.H. Chan School of Public Health
-
Thomas M. Moriarty, chief policy and external affairs officer and general counsel at CVS Health
-
Gregory A. Poland, professor of medicine and infectious diseases and director of the Vaccine Research Group at the Mayo Clinic
-
Monica Schoch-Spana, medical anthropologist and senior scholar with the Johns Hopkins Center for Health Security
-
Moderated by Carl Zimmer, The Times’s “Matter” columnist
An effective vaccine will be a huge breakthrough for society and the economy. But will it as effective in practice as in studies?
Gregory Poland of the Mayo Clinic, who is also editor in chief of the journal Vaccine, explained the extent to which early results of the various vaccine trials have defied even optimistic expectations. He described it as “as nothing short of dizzying,” and added:
“We were all prepared to see something like 50 to 70 percent efficacy, something like that. And to be in excess of 90 percent, 95 percent, puts it on par with the best vaccines that have ever been developed — and with apparent acceptable short-term safety. I think this is really going to have a profound effect on the field of vaccinology. I hate to overuse the word ‘paradigm-breaking,’ but it is, in many ways, to see something come to fruition within eight months like this.”
But Mr. Poland also warned of “surprises” when measuring the impact of the first generation vaccines:
“The efficacy measures we have were at times of relatively low transmission of disease compared to now. It was with masks on with people distanced, none of which will be true in time. So we may see some differences.”
Who should be first in line for the vaccinations? What’s fair when allocating a limited number of shots?
Even if vaccine injections are approved for use before the end of the year, the vast majority of people in the United States won’t notice any appreciable difference in their lives for at least three months, said Marc Lipsitch. Cases will continue to rise as winter temperatures force more people indoors, and there won’t yet be enough doses to cover the population.
That raises some thorny questions.
Earlier this month, the Advisory Committee on Immunization Practices at the Centers for Disease Control and Prevention voted to vaccinate health care workers and nursing home residents first. It proposed placing essential workers like bus drivers and grocery workers in the next tier of recipients.
Mr. Lipsitch is among those who supports the alternative recommendation of the National Academies of Sciences, Engineering and Medicine to dole out the vaccine based on people’s health conditions rather than their working ones:
“The only certain way, given what we know about the vaccine now, to get society back to being able to function is to have this be a less-severe disease. And the way you do that is to make the people in whom it’s severe no longer vulnerable.”
But Mr. Lipsitch also acknowledged that the vaccine might never fully rid the world of Covid-19. “I can’t conceive of its disappearing,” he said. “Viral infections this widespread don’t disappear on their own that I’m aware of, unless they’re out-competed by some new strain.”
He suggested, however, that Covid-19 might become less severe in the long term. “If everybody essentially in the world who’s not a newborn has either had the virus or had the vaccine,” he said, “there would be some immunity to severity, and some immunity to transmission, and so if I had to make a guess I would say it would become a seasonal disease like the flu.”
Your neighborhood pharmacy will soon become a major player in vaccine distribution.
Getting a Covid-19 vaccine to millions of people in every corner of the country is, of course, a huge logistical undertaking. Rather than relying on public health networks, the Trump administration has placed the nation’s two largest for-profit pharmacy chains, CVS and Walgreens, at the center of the nation’s vaccination effort.
That also puts those chains at the forefront of an effort to educate the public about a new vaccine, and to convince the many skeptics that the rapidly developed shot is safe. Thomas Moriarty of CVS Health shared a little of what that task looks like, noting that about three-quarters of all Americans live within three miles of a CVS, “and we have the ability to extend beyond that through vaccination clinics.”
The Road to a Coronavirus Vaccine
Words to Know About Vaccines
Confused by the all technical terms used to describe how vaccines work and are investigated? Let us help:
-
- Adverse event: A health problem that crops up in volunteers in a clinical trial of a vaccine or a drug. An adverse event isn’t always caused by the treatment tested in the trial.
- Antibody: A protein produced by the immune system that can attach to a pathogen such as the coronavirus and stop it from infecting cells.
- Approval, licensure and emergency use authorization: Drugs, vaccines and medical devices cannot be sold in the United States without gaining approval from the Food and Drug Administration, also known as licensure. After a company submits the results of clinical trials to the F.D.A. for consideration, the agency decides whether the product is safe and effective, a process that generally takes many months. If the country is facing an emergency — like a pandemic — a company may apply instead for an emergency use authorization, which can be granted considerably faster.
- Background rate: How often a health problem, known as an adverse event, arises in the general population. To determine if a vaccine or a drug is safe, researchers compare the rate of adverse events in a trial to the background rate.
- Efficacy: The benefit that a vaccine provides compared to a placebo, as measured in a clinical trial. To test a coronavirus vaccine, for instance, researchers compare how many people in the vaccinated and placebo groups get Covid-19. Effectiveness, by contrast, is the benefit that a vaccine or a drug provides out in the real world. A vaccine’s effectiveness may turn out to be lower or higher than its efficacy.
- Phase 1, 2, and 3 trials: Clinical trials typically take place in three stages. Phase 1 trials usually involve a few dozen people and are designed to observe whether a vaccine or drug is safe. Phase 2 trials, involving hundreds of people, allow researchers to try out different doses and gather more measurements about the vaccine’s effects on the immune system. Phase 3 trials, involving thousands or tens of thousands of volunteers, determine the safety and efficacy of the vaccine or drug by waiting to see how many people are protected from the disease it’s designed to fight.
- Placebo: A substance that has no therapeutic effect, often used in a clinical trial. To see if a vaccine can prevent Covid-19, for example, researchers may inject the vaccine into half of their volunteers, while the other half get a placebo of salt water. They can then compare how many people in each group get infected.
- Post-market surveillance: The monitoring that takes place after a vaccine or drug has been approved and is regularly prescribed by doctors. This surveillance typically confirms that the treatment is safe. On rare occasions, it detects side effects in certain groups of people that were missed during clinical trials.
- Preclinical research: Studies that take place before the start of a clinical trial, typically involving experiments where a treatment is tested on cells or in animals.
- Viral vector vaccines: A type of vaccine that uses a harmless virus to chauffeur immune-system-stimulating ingredients into the human body. Viral vectors are used in several experimental Covid-19 vaccines, including those developed by AstraZeneca and Johnson & Johnson. Both of these companies are using a common cold virus called an adenovirus as their vector. The adenovirus carries coronavirus genes.
- Trial protocol: A series of procedures to be carried out during a clinical trial.
One of Mr. Moriarity’s biggest concerns is whether people will be willing to take the vaccine. His team surveys up to 7,000 people two to three times a week about what he called the “hesitancy rate,” he explained:
“What we have seen in the data since getting past the election, and with the efficacy results of these vaccines becoming public, is that the hesitancy rate is starting to drop. There’s still going to be a core element of hesitancy — no question about it — but getting past the politics and seeing the results of the science is helping alleviate some of that hesitancy.”
The country needs to re-establish trust in institutions, because pandemics are here to stay.
Much of the conversation about the coronavirus pandemic has focused, understandably, on “getting back to normal.” Yet the inescapable truth is that, in many ways, there is no going back to the world as it was before the coronavirus. In a global economy in which pathogens can spread more quickly than ever before, the question is not if there will be another global pandemic, but when.
Monica Schoch-Spana, a medical anthropologist who studies the ways communities respond to disaster, talked about what needed to be done to repair institutions that struggled during this crisis to clearly and effectively communicate with the public:
“This is about trust, and trust building, and processes of reconciliation. And that takes time. And during that time, we can improve our messaging and involve trusted messengers. But what we’re talking about is re-establishing trust in institutions. We have to build processes for that, and strengthen the ones that are already there.”
She said that efforts to persuade the public to accept the vaccine will have to include different messages targeted at different communities:
“There will be certain messages that resonate really well in Baltimore City among local Black communities that may not resonate well with rural frontier Hispanics in southeastern Idaho. So we have to have those very hyperlocal perspectives.”
When it comes to public health education, the messenger is at least as important as the message.
Black, Latino and Asian communities have disproportionately borne the brunt of coronavirus cases in the United States. And yet, thanks to a legacy of racism in the American medical system, many in those communities are particularly wary of receiving the vaccine. Black adults, in particular, have expressed higher rates of vaccine hesitancy than others in the United States, a wariness fueled by the historical example of forced injections, forced sterilizations, unethical experimentation and other acts administered in the name of public health.
Opposition to the vaccine within these communities is of particular concern to James Hildreth, an immunologist who spent decades on H.I.V. and AIDS research as a professor at Johns Hopkins before taking over in 2015 as president of Meharry Medical College, a historically Black medical school in Nashville. He discussed his experience with what works in public health education — and what does not. “We discovered that the messages were fine, but if the messenger is not trusted you’re wasting your time,” he said:
“So we identified trusted messengers in those communities. We empowered them with the information they needed. They needed to believe it first — and accept it first — and they were the ones that delivered the messages that turned out to be quite effective. So that’s the model we’ve adopted to try to engage and reach minority communities with the vaccine.”
We have to take care of the virus. Then we have to take care of everything else.
The vaccine is not the end of the pandemic recovery period, but the beginning. Once the virus is under control, the nation faces disarray: millions of people unemployed, communities shattered by the loss of businesses, a generation with a disrupted education and deepened systemic inequalities.
“The pandemic did more than just make us physically sick,” said Ruth Faden, a bioethicist. But she explained how this pain could become a catalyst for a better society:
“I think it’s possible to envision a way in which for some of these horrible gaps in access, and the consequences that are lifelong for people’s prospects for a decent life, there will be an effort to fix them, perhaps with some urgency. I have to hope that something like that will happen as a consequence of what we’ve all gone through — and if not, it will be profoundly depressing.”