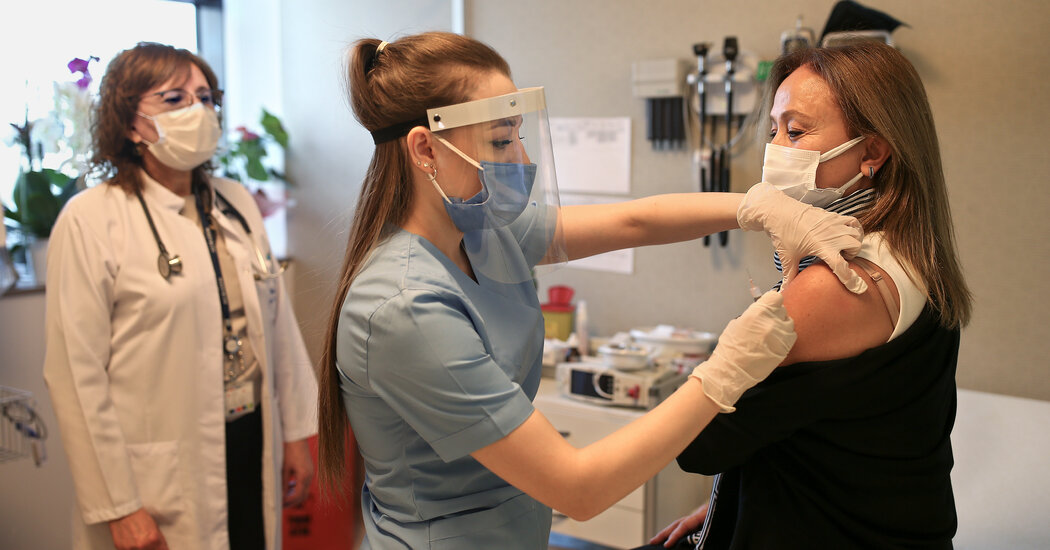
There are currently more than 100,000 different face masks for sale. They come in silk, cotton, and synthetics; with and without filter; over the head and over the ears. They have sparkles and sunflowers; friendly greetings and insults; Cartoon characters and teeny reindeer.
What they don’t have is a label that shows how well they block infectious particles, an omission that has frustrated public health officials during the coronavirus pandemic. These experts find that the effectiveness of different designs varies widely and some particles barely filter out.
“The most basic and basic question is, what is the safest mask and how can I make sure I have it and my family members and children have it?” said Fran Phillips, who resigned from her post as Assistant Secretary of Health of Maryland in August. “It’s so amazing that we’re here right now and don’t have that information.”
This could change soon. A division of the Centers for Disease Control and Prevention is working to develop minimum standards of filter efficiency and labels showing which products meet them for the vast and confusing market for masks and other face coverings.
The National Institute for Safety and Health at Work, a division of the CDC known as NIOSH, tacitly published guidelines drafted next month with an industry standard organization, ASTM International (formerly the American Society for Testing and Materials).
“When you have a standard, you can know what level of protection is being achieved and you can consistently evaluate these products,” said Maryann D’Alessandro, director of the NIOSH National Personal Protective Technology Laboratory.
Since the beginning of the pandemic, there has been hardly any nationwide supervision of masks and other face coverings. Both the Food and Drug Administration and the CDC have some authority over the industry. The FDA, which regulates medical devices, shares authority with NIOSH for monitoring N95 respirators, which are most protective devices on the market. However, most of the masks worn by the public are just pieces of cloth and are not subject to any government oversight.
Sales of masks spiked after the FDA issued an emergency measure in April – when healthcare facilities struggled to secure enough protective gear – that in part said the agency would not take action against companies that sell them to the general public . At the same time, however, the FDA also stated that these products “may or may not meet the liquid barrier or filtration efficiency”. That warning did no harm to the market, and some critics now blame the FDA for the poor quality of many products sold.
“There were many things the FDA could have done to improve the situation, especially after research was released into which masks worked and which didn’t,” said Diana Zuckerman, president of the National Center for Health Research, a nonprofit health policy group. “The FDA could have issued instructions that masks should be attached, at least two layers of fabric, not made of stretchable materials, etc. Instead, there was one free for all.”
The effectiveness of masks “can be between 0 and 80 percent depending on the material composition, number of layers and layer bonding,” said Dale Pfriem, president of Protective Equipment Consulting Services and member of the working group for the development of standards dealing with mask guidelines.
The gold standard for masks is the N95, which is tight and can filter out at least 95 percent of very small particles. But N95 masks are generally reserved for naturopaths and have been in short supply since the outbreak began. Hospitals desperate for more N95 have been driven to a booming black market to keep them secure.
To make up for the shortage, the FDA approved the sale of the KN95, the Chinese equivalent of the American N95, last spring. However, the agency soon discovered fraudulent and counterfeit products and narrowed the range of allowable KN95 imports. Nevertheless, the agency admits that there is still widespread fraud and that countless companies label masks that do not meet FDA standards with “KN95”.
Updated
Apr. 16, 2020, 4:13 pm ET
One step below the N95 in terms of protection are FDA approved surgical masks that must meet certain government standards. The surgical mask style is often copied by companies that sell imitations that do not offer the same level of protection.
And then there’s the Wild West: Millions of masks made of every possible fabric, from individual layers up, as well as headscarves and gaiters, closed loops of fabric that can be worn around the neck and extend over the lower part of the face.
Almost any mask is better than no mask, say public health experts. The CDC has updated its guidelines on masks several times to find that a tightly woven, multi-layered fabric provides better protection than a single-layer or loose-knit mask – both for the wearer and for those who come in with the wearer Contact. However, the agency’s website does not provide clarity on whether masks with filters provide better protection than those without filters, and how synthetic fabrics compare to cotton or other materials.
“There was a critical need for some sort of national program to test and certify masks and communicate with people about how they are used and cared for,” said Linsey Marr, professor of civil and environmental engineering at Virginia Tech and lead expert for viruses in the air.
A working group of federal and industry representatives has proposed high and low filtration requirements that manufacturers and distributors can adopt and list on their labels. The lower standard is a 20 percent filtration barrier and the higher is 50 percent.
These numbers are more protective than they sound. Filtration Efficiency Percentages are based on a product’s efficiency in filtering 0.3 micron particles, which are the most commonly used particulate matter standard for NIOSH testing.
“A 20 percent efficiency at 0.3 micrometers would mean 50 percent efficiency for 1 to 2 micrometers particles and 80 percent efficiency for blocking particles 4 to 5 micrometers or larger in size,” said Dr. Marr. “I think it will be useful.”
According to Dr. Marr, the coronavirus itself is 0.1 micrometers in size, but is transported in aerosols, which can range in size from around 0.5 micrometers upwards.
Jeffrey Stull, a member who helps write the standards, said the group would also rate masks and face covers for “breathability”. The standard project has been a long way.
“It was a very difficult process,” said Stull, president of International Personnel Protection Inc. “We have been trying to find that consensus on what the level of performance should be. We were initially talking about higher levels and they said,” No. “80 percent of the industry can’t stick to it – it won’t do anyone any good.” So we had to compensate. “
Manufacturers who want to ensure that they meet the ASTM standard must first have their products tested by an accredited laboratory. They should also be able to demonstrate that their masks provide adequate adaptation to the general population. Those who comply with the standards can then determine that they meet the ASTM standard for the product or packaging. However, there is no enforcement mechanism.
Daniel Carpenter, Professor of Government at Harvard, described the work of NIOSH in the development of the standard “Regulatory Entrepreneurship”.
It says, ‘Let’s use the tools we have, even if we don’t have formal regulatory tools, “Carpenter said.” It’s an alternative way of regulating. It can have a pretty important regulatory effect because if it does If you do not comply with the standards, you will not receive a seal of approval.
Mr. Pfriem hopes that the standards will prevail. “What we have here is a really good standard,” he said. “Manufacturers will have something to design their products and incorporate into their marketing materials and packaging, and consumers will have a sense of confidence.”
He added, “I can tell you that a lot of what is marketed on eBay and other websites and manufactured, for example, in your neighbor’s garage, cannot meet this standard.”