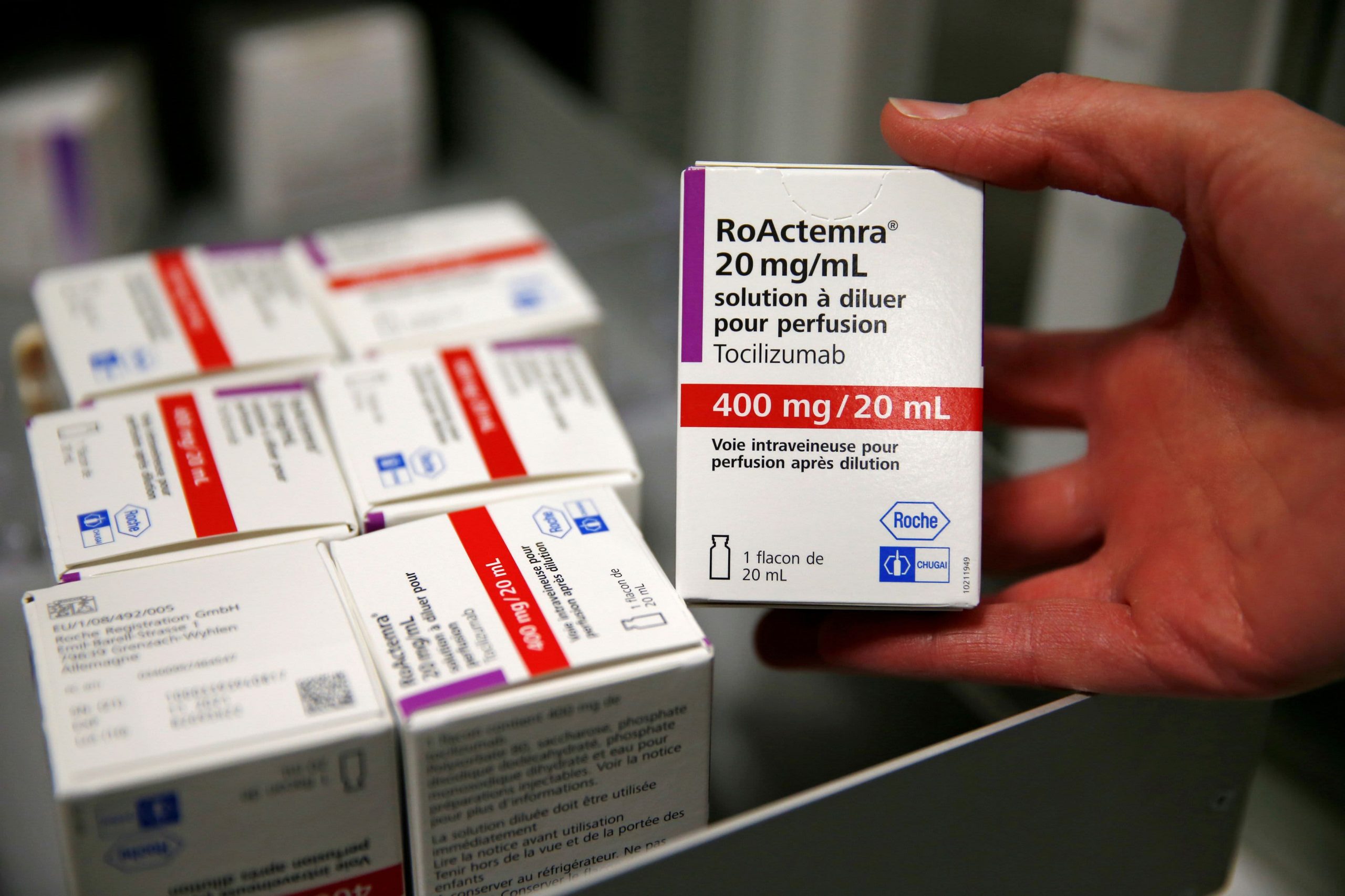
Texas has one of the most restrictive medical marijuana laws in the country, allowing prescription-only sales for a handful of conditions.
That didn’t stop Lukas Gilkey, CEO of Hometown Hero CBD in Austin, Texas. His company sells joints, blunts, gummy bears, steamers, and tinctures that provide a recovery high. In fact, business is booming online too, where he is selling to many people in other states with strict marijuana laws.
But Mr. Gilkey says he’s not an outlaw and that he doesn’t sell marijuana, just a close relationship. He offers products with a chemical compound – Delta-8-THC – which is extracted from hemp. Chemically, it is only slightly different from Delta 9, the main psychoactive ingredient in marijuana.
And that little distinction, it turns out, can make a big difference in the eyes of the law. According to federal law, psychoactive Delta 9 is expressly prohibited. However, delta-8 THC from hemp is not a loophole that some business owners claim they can sell in many states where hemp ownership is legal. The number of customers “coming to Delta 8 is staggering,” said Gilkey.
“You have a drug that essentially gets you high but is completely legal,” he added. “The whole thing is weird.”
The Rise of Delta 8 is a case study of how hardworking cannabis entrepreneurs are pulling hemp and marijuana apart to create countless new product lines with different marketing angles. They build brands from a variety of potencies, flavors, and strains of THC, the intoxicating substance in cannabis, and of CBD, the non-intoxicating compound often sold as a health product.
With Delta 8, entrepreneurs also believe they have found a way to exploit the country’s broken and convoluted laws on recreational marijuana use. However, it is not that simple. Federal agencies, including the Drug Enforcement Administration, are still reviewing their options for enforcement and regulation.
“Dealing with Delta-8 THC is in no way without significant legal risk,” said Alex Buscher, a Colorado attorney specializing in cannabis law.
However, cannabis industry experts said Delta 8 sales actually exploded. Delta 8 is “the fastest growing segment” of hemp products, said Ian Laird, CFO of New Leaf Data Services, which tracks the hemp and cannabis market. Estimating consumer sales at least $ 10 million, he added, “Delta 8 really came out of nowhere last year.”
Marijuana and hemp are essentially the same plant, but marijuana has higher concentrations of delta-9 THC – and as a source of poisoning, it has been a primary focus of business and state and federal lawmakers. Delta 8, if discussed at all, was an esoteric, less potent by-product of both plants.
That changed with the 2018 Farm Bill, an enormous federal law that, among other things, legalized the widespread cultivation and distribution of hemp. The law also specifically allowed the sale of the plant’s byproducts – the only exception was Delta 9, which had THC levels high enough to define it as marijuana.
With no mention of Delta 8 in the legislation, entrepreneurs jumped into the void and began extracting and packaging it as a legal edible and smokable alternative.
Exactly what type of high Delta 8 produces depends on who you ask. Some consider it “marijuana light” while others “refer to it as pain relief with less psychoactivity,” said David Downs, executive editor for content at Leafly.com, a popular source of news and information about cannabis.
In both cases, Delta 8 has become “extremely ascending,” Downs said, reflecting what he calls the “Interregnum of Prohibition of Doom,” where consumer demand and entrepreneurship exploit loopholes in rapidly evolving and broken laws.
“We are receiving reports that in prohibited states like Georgia you can go to a rest stop and look at what looks like a cannabis bud in a jar,” Downs said. The bud is hemp sprayed with highly concentrated Delta 8 oil.
Joe Salome owns the Georgia Hemp Company, which began selling Delta 8 locally in October and shipping it nationally – about 25 orders a day, he said. “It has moved out enormously.”
Its website touts Delta 8 as “very similar to its psychoactive brother, THC,” and offers users the same relief from stress and inflammation, “without the same fearful high that some may experience with THC.”
Mr Salome said he didn’t need to buy an expensive government license to sell medical marijuana because he felt protected by the farm bill.
“Everything is fine there,” he said, explaining that it was now legal to “sell all parts of the facility.”
The legal landscape is contradicting at best. Many states are more permissive than the federal government, which considers marijuana an illegal and highly dangerous drug under the Controlled Substances Act. Medical marijuana is legal in 36 states. It is legal for recreational use in 14 states.
But in the blink of an eye, the federal government opened the door to the sale of hemp products under the Agriculture Act, even in states that have not legalized recreational marijuana use. Few states like Idaho ban hemp altogether, but Delta 8 entrepreneurs are finding a receptive market in others.
Mr. Gilkey’s lawyers believe the farm bill is on their side. “Delta 8, when derived from or derived from hemp, is considered hemp,” said Andrea Steel, co-chair of the cannabis group of companies at Coats Rose, a Houston law firm. She stressed that the legality also depends on whether Delta 9 exceeds the legal limits.
Ms. Steel noted that when making a Delta 8 product, it can be difficult, if not impossible, to filter all of the Delta 9 out of hemp.
“Adding another crease,” she said, “a lot of labs don’t have the ability to differentiate between Delta 8 and Delta 9.”
Lisa Pittman, the other co-chair of the cannabis group of companies at Coats Rose, said the Farm Bill authors may not have considered the ramifications of the law in their reading of the subject.
Ms. Pittman said the ultimate question of a product’s legality may depend on other factors, including how the Delta 8 is manufactured and sourced. In particular, the lawyers said the DEA The rule on this topic seems to suggest that Delta 8 could be illegal if it is made “synthetically” rather than organically.
Lawsuits relating to the interpretation of the DEA rule are currently pending.
Mr Gilkey said he paid more than $ 50,000 in legal fees to make sure he wasn’t breaking the law. A US Coast Guard veteran, Mr. Gilkey worked on a boat anti-drug unit outside of San Diego. He “saw some really tough things,” he said, “and wasn’t happy about the war on drugs.”
He ran a shop in Austin that sold e-liquid for vaping machines. Then in 2019 he started his current business selling CBD. Late last spring, he said he was getting calls from customers on Delta 8.
“I said please explain what this is,” he recalled. Mr. Gilkey, whose company supplies products to other retail stores around the country, saw a great opportunity. After checking with the lawyers, he started packing gummies, vape pens, and other full-size products with Delta 8 that he received from a major hemp supplier.
“It’s about to go mainstream,” he said. And it’s just the beginning. “There is a Delta 10 in the works.”