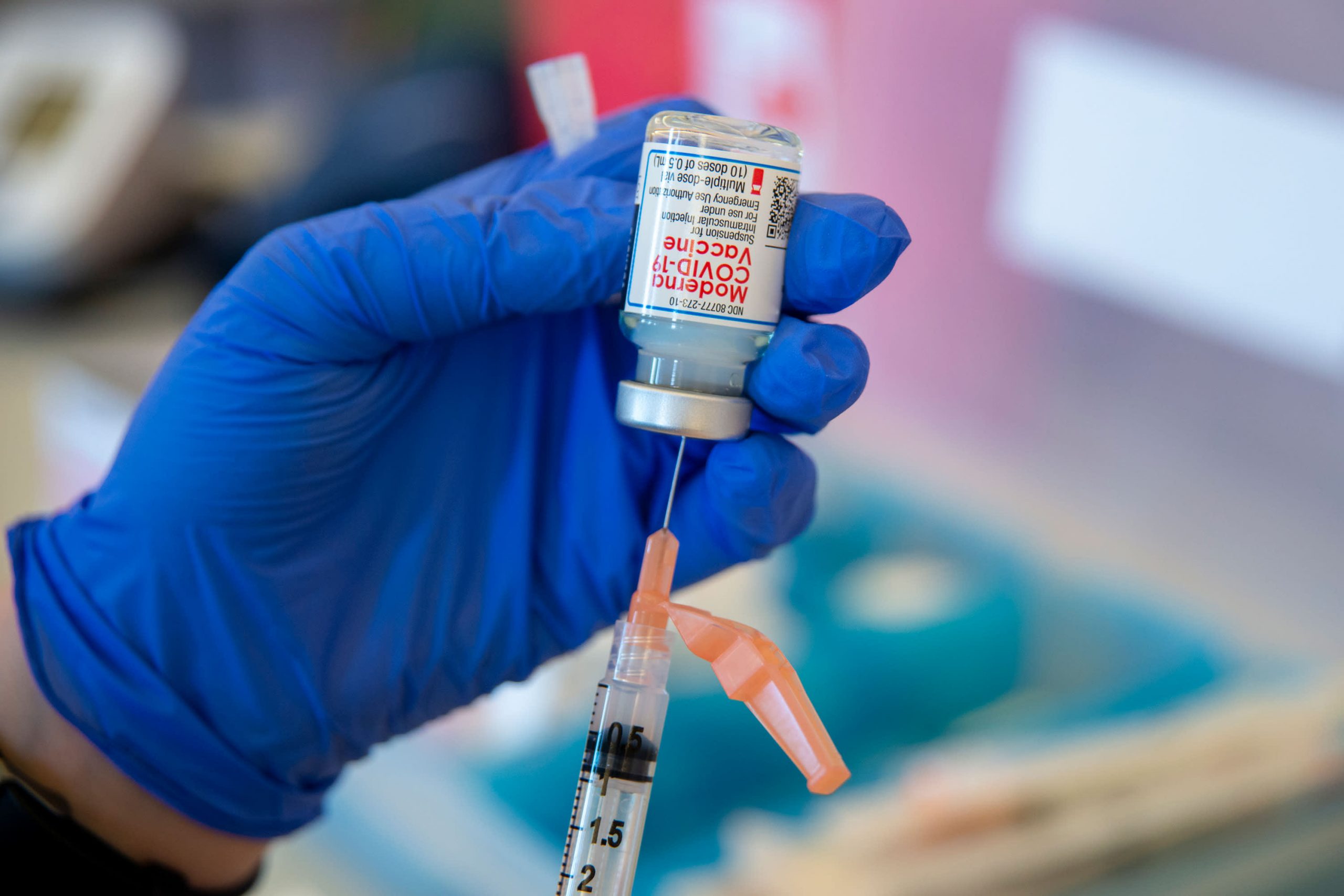
The severe lower leg injuries Tiger Woods sustained in a car accident on Tuesday usually lead to a long and dangerous recovery that, according to medical experts who have treated similar injuries, calls into question his ability to return to professional golf.
Athletes with severe leg injuries believed to ruin their careers have returned – quarterback Alex Smith returned to play football after a cruel broken leg last season, and golfer Ben Hogan returned after a car accident decades ago .
But Woods’ injuries are more extensive and his path to recovery is littered with serious obstacles. Infection, inadequate bone healing, and in Woods’ case, previous injuries and chronic back problems can make months or even years of recovery even more difficult and reduce the chances of him playing again.
In the accident near Los Angeles, Woods’ right lower leg was bruised, his right foot was badly injured, and his leg muscles became so swollen that surgeons had to cut open the tissue covering them to relieve the pressure, Dr. Anish Mahajan, the chief physician at Harbor-UCLA Medical Center where Woods, 45, was treated, wrote in a Twitter message on Wood’s account.
Doctors also inserted a bar into Wood’s shin and screws and pins into his foot and ankle. Doctors familiar with these types of injuries described the complications that they typically pose.
The injuries are common among drivers involved in car accidents, said Dr. R. Malcolm Smith, chief of orthopedic trauma at Massachusetts General Hospital in Boston. Usually they happen when the driver desperately hits the brakes while a car is spiraling out of control.
When the front end of the car is smashed, immense force is transferred to the driver’s right leg and right foot. “This happens every day with car accidents in this country,” said Dr. Smith.
Such lower leg fractures occasionally bring “massive disabilities” and other serious consequences, said Dr. Smith. “A very rough estimate is that there is a 70 percent chance that it will heal completely,” he added.
The crash caused a cascade of injuries. It shattered Woods’ tibia with primary fractures in the upper and lower portions of the bones and a scattering of bone fragments. When the bones in Wood’s shin burst, they damaged muscles and tendons; Pieces protruded from his skin.
The trauma caused bleeding and swelling in his leg and threatened his muscles. Surgeons had to quickly cut into the thick layer of tissue covering his leg muscles to relieve the swelling. If it hadn’t been for them, the tissue covering the swelling muscle would have acted like a tourniquet, restricting blood flow. The muscle can die within four to six hours.
It is possible that a muscle may have died between the accident and the operation anyway. Dr. Smith said, “Once you’ve lost it, you can’t get it back.”
Patients who are used this procedure must be hospitalized until the muscle swelling subsides. This can take a week or more. Sometimes, even after a few weeks, the swelling has not gone down enough to close the wound, requiring surgeons to transplant skin over the opening.
Dr. Kyle Eberlin, a reconstructive surgeon at Massachusetts General Hospital, said doctors often need to transplant skin from the thigh or back to plug the holes where bones protrude from the skin. This is known as a free flap. They cut pieces of skin the size of a football and carefully use a microscope to connect tiny blood vessels about a millimeter in diameter from the skin graft to the blood vessels near the wounds.
Infection is a risk with fractures that break through the skin and insert chopsticks and pens into the bones after surgery, with an amputation in the worst case, said Dr. Smith. The likelihood of infection depends on the level of contamination and the size of the wound.
In car accidents, gravel and sometimes dirt can get into wounds and increase the chances of infection, said Dr. Eberlin.
Opening the muscle shell can increase the risk of infection, said Dr. Reza Firoozabadi, an orthopedic trauma surgeon at Harborview Medical Center in Seattle.
In large trauma centers like Massachusetts General or UCLA, the free flap procedures are performed within 48 hours. However, it is more typical to operate within a week of the injury, said Dr. Eberlin.
Rehabilitation will be long and arduous. If Woods needed a free valve – which trauma surgeons say is likely – “it will be months and months before he can put weight back on his leg,” said Dr. Eberlin.
Woods also risks fractures that do not heal or grow together very slowly, said Dr. Firoozabadi. “To heal things, you need good blood circulation,” he said. “With such an injury, the blood flow is disturbed.”
As a result, Wood’s lower leg bones could take five to 14 months to grow together, provided they do so at all.
The biggest hurdle will be his foot and ankle injuries, said Dr. Firoozabadi and others. Restoring mobility and strength can take three months to a year. Depending on the extent of these injuries, Woods can barely walk even after rehabilitation.
His rehabilitation can be made more difficult by a back operation in December. Woods also went to rehab for an addiction to pain medication; Managing pain while he is recovering can now be difficult.
Still, some athletes have returned from serious injuries. Smith, the Washington Football Team quarterback, had a similar leg injury and returned to play in October. But it took two years and 17 operations, and along the way he developed infection of the wounds and sepsis, a life-threatening condition. And Smith had no injuries to his foot or ankle.
Golfer Ben Hogan broke his collarbone, pelvis, left ankle, and a rib. The injuries were severe but not comparable to Woods’ injuries.
With his foot and ankle injuries and severe injuries to his leg, “Woods may never play golf again,” said Dr. Smith.