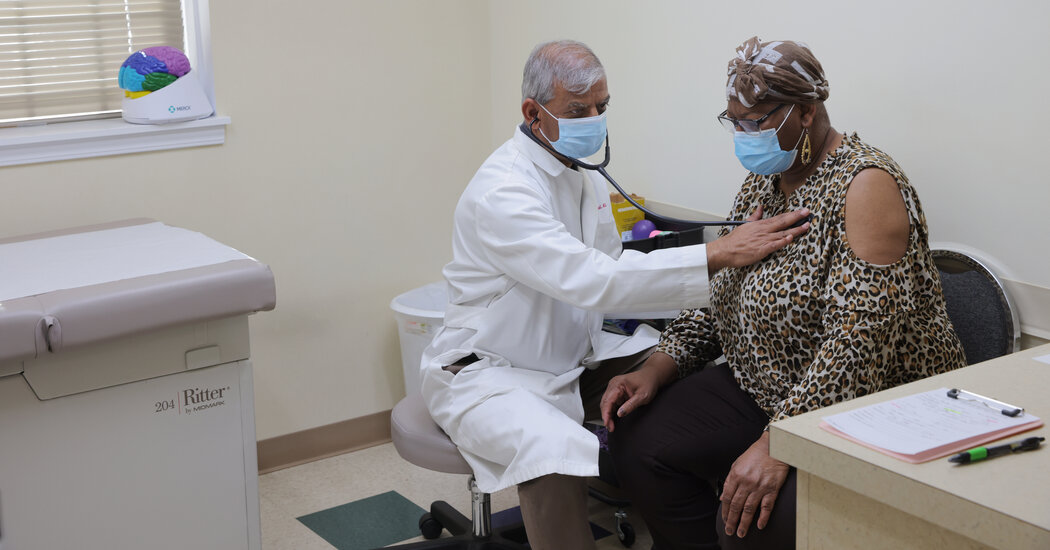
Yvette Lowery usually gets her annual mammogram in March. But last year when the pandemic took hold and medical facilities closed, the center she goes to canceled her appointment. Nobody could tell her when to set a new appointment.
“They just said keep calling back, keep calling back,” said Ms. Lowery, 59, who lives in Rock Hill, SC
Ms. Lowery felt a lump under her arm in August but was not able to make an appointment until October.
Eventually she was diagnosed with stage 2 breast cancer, started chemotherapy in November, and had a double mastectomy that month.
“I’ve seen a lot of patients at an advanced stage,” said Dr. Kashyap B. Patel, one of Ms. Lowery’s physicians and executive director of Carolina Blood and Cancer Care Associates. If her cancer had been discovered last May or June, it would likely have been caught before it spread, said Dr. Patel.
According to experts, months of bans and waves of Covid cases closed clinics and testing laboratories or cut working hours in other locations over the past year, leading to a sharp decline in the number of screenings, including breast and colon cancers.
Numerous studies have shown that the number of patients screened or diagnosed decreased in the first few months of the pandemic. By mid-June, the rate of screenings for breast, colon and cervical cancer was still 29 to 36 percent below their prepandemic levels, according to a data analysis by the Epic Health Research Network. According to network data, hundreds of thousands fewer screenings were done in the past year than in 2019.
“We still haven’t caught up,” said Dr. Chris Mast, vice president of clinical informatics at Epic, who develops electronic health records for hospitals and clinics.
Another analysis of the Medicare data found that cancer screenings declined as Covid cases rose over certain periods in 2020. Analysis, conducted by Avalere Health, a consulting firm for the Community Oncology Alliance, which represents independent cancer specialists, found test scores in November were about 25 percent lower than in 2019. The number of biopsies used to diagnose used by cancer decreased by about a third.
While it is too early to fully appreciate the full impact of the delays in screenings, many cancer specialists are concerned about the emergence of patients with more severe disease.
“In practice, there is no question that we see patients with advanced breast cancer and colon cancer,” said Dr. Lucio N. Gordan, President of the Florida Cancer Specialists & Research Institute, one of the largest independent oncology groups in the country. He is working on a study to see if these lack of screenings have resulted in more patients with later-stage cancer overall.
And although the number of mammograms and colonoscopies has risen again in recent months, many people with cancer go undetected, doctors report.
Some patients, like Ms. Lowery, were unable to make an appointment after the clinics reopened due to pent-up demand. Others skipped regular tests or ignored worrying symptoms because they were afraid of getting infected or because they couldn’t afford a test after losing their job.
Updated
March 17, 2021, 8:59 p.m. ET
“The fear of Covid was more tangible than the fear of missing a screen that detected cancer,” said Dr. Patrick I. Borgen, the chairman of surgery at Maimonides Medical Center in Brooklyn, who also directs the breast center. His hospital treated so many coronavirus patients early on that “we are now called a Covid hospital,” he said, and healthy people stayed away to avoid contagion.
Even patients at high risk due to their genetic makeup or because they had cancer before have missed critical screenings. Dr. Ritu Salani, director of gynecological oncology at UCLA Health Jonsson Comprehensive Cancer Center, said a woman at risk for colon cancer had a negative test in 2019 but did not go to her usual screening last year because of the pandemic.
When she went to see her doctor, she had advanced cancer. “It’s just a devastating story,” said Dr. Salani. “Screening tests are really designed for when patients are not feeling bad.”
Ryan Bellamy was in no hurry to postpone an aborted colonoscopy last spring, despite the presence of blood in his stool prompting him to check for symptoms. “I really didn’t want to go to the hospital,” said Mr Bellamy. He decided he was unlikely to have cancer. “They’re not following me, so I’m okay with Googling,” he told himself.
Mr Bellamy, a Palm Coast, Florida resident, said that after his symptoms worsened, his wife insisted that he go for a test in December and have a colonoscopy in late January. With a new diagnosis of stage 3 rectal cancer, 38-year-old Bellamy is undergoing radiation and chemotherapy.
Colon screening stayed significantly lower in 2020, declining about 15 percent from 2019, according to data from the Epic network, although overall screening was down 6 percent. The analysis looked at screenings for more than 600 hospitals in 41 states.
Lung cancer patients have also been delayed in seeking appropriate treatment, said Dr. Michael J. Liptay, chairman of cardiovascular and thoracic surgery at Rush University Medical Center in Chicago. One patient had an imaging that showed a spot in their lungs and they should follow up just like the pandemic. “Additional workup and maintenance has been postponed,” said Dr. Liptay. By the time the patient was fully examined, the cancer had grown in size. “It wasn’t good waiting 10 months,” said Dr. Liptay, although he wasn’t sure if previous treatment would have changed the patient’s prognosis.
Just as previous economic recessions resulted in people foregoing medical care, the economic downturn during the pandemic also prevented many people from seeking help or treatment.
“We know there is cancer,” said Dr. Barbara L. McAneny, the executive director of New Mexico Oncology Hematology Consultants. Many of their patients stay away, even if they are insured, because they cannot afford the deductibles or co-payments. “We see this, especially with our poorer people who are marginalized anyway and live from paycheck to paycheck,” she said.
Some patients ignored their symptoms for as long as they could. Last March, Sandy Prieto, a school librarian who lived in Fowler, California, had a stomach ache. But she refused to go to the doctor because she didn’t want Covid. After a telemedicine visit to her family doctor, she tried over-the-counter medication, which did not help with pain and nausea. She continued to refuse.
“It got to a point where we had no choice,” said her husband Eric, who had repeatedly urged her to see a doctor. Jaundice and severe discomfort, she went to the emergency room in late May and was diagnosed with stage 4 pancreatic cancer. She died in September.
“If it hadn’t been for Covid and we’d taken her somewhere sooner, she would still be with us today,” said her sister Carolann Meme, who had tried to convince Ms. Prieto to go to an academic medical center where she could go a clinical trial may be advisable.
When patients like Ms. Prieto are treated virtually instead of being seen in person, doctors can easily overlook important symptoms or recommend medication instead of telling them to come in, said Dr. Ravi D. Rao, the oncologist who treated Ms. Prieto. Patients could downplay how sick they feel or fail to mention the pain in their hip, he said.
“In my opinion, telemedicine and cancer don’t travel together,” said Dr. Rao. He also used telemedicine during the pandemic but said he had worked to keep his offices open.
Other doctors defended the use of virtual visits as a critical tool when office visits were too dangerous for most patients and staff. “We were grateful for robust telemedicine when people just couldn’t come to the center,” said Dr. Borrowing from Maimonides. However, he acknowledged that patients were often reluctant to discuss their symptoms during a telemedicine session, especially a mother whose young children could hear what they were saying. “It’s not private,” he remarked.
Some health networks say they have taken aggressive steps to counter the effects of the pandemic. Kaiser Permanente, the major California managed care company, saw a decline in breast cancer screenings and diagnoses on their first home order last year in the north of the state. “Doctors immediately teamed up” to get in touch with patients, said Dr. Tatjana Kolevska, Medical Director of the Kaiser Permanente National Cancer Excellence Program.
Kaiser also relies on its electronic health records to make appointments for women who are overdue for their mammograms, when they want to book an appointment with their GP, or even get a prescription for new glasses.
While Dr. Kolevska says waiting to see data for the entire system, she was encouraged by the number of patients in her practice who are now up to date with their mammograms.
“All of these things helped tremendously,” she said.