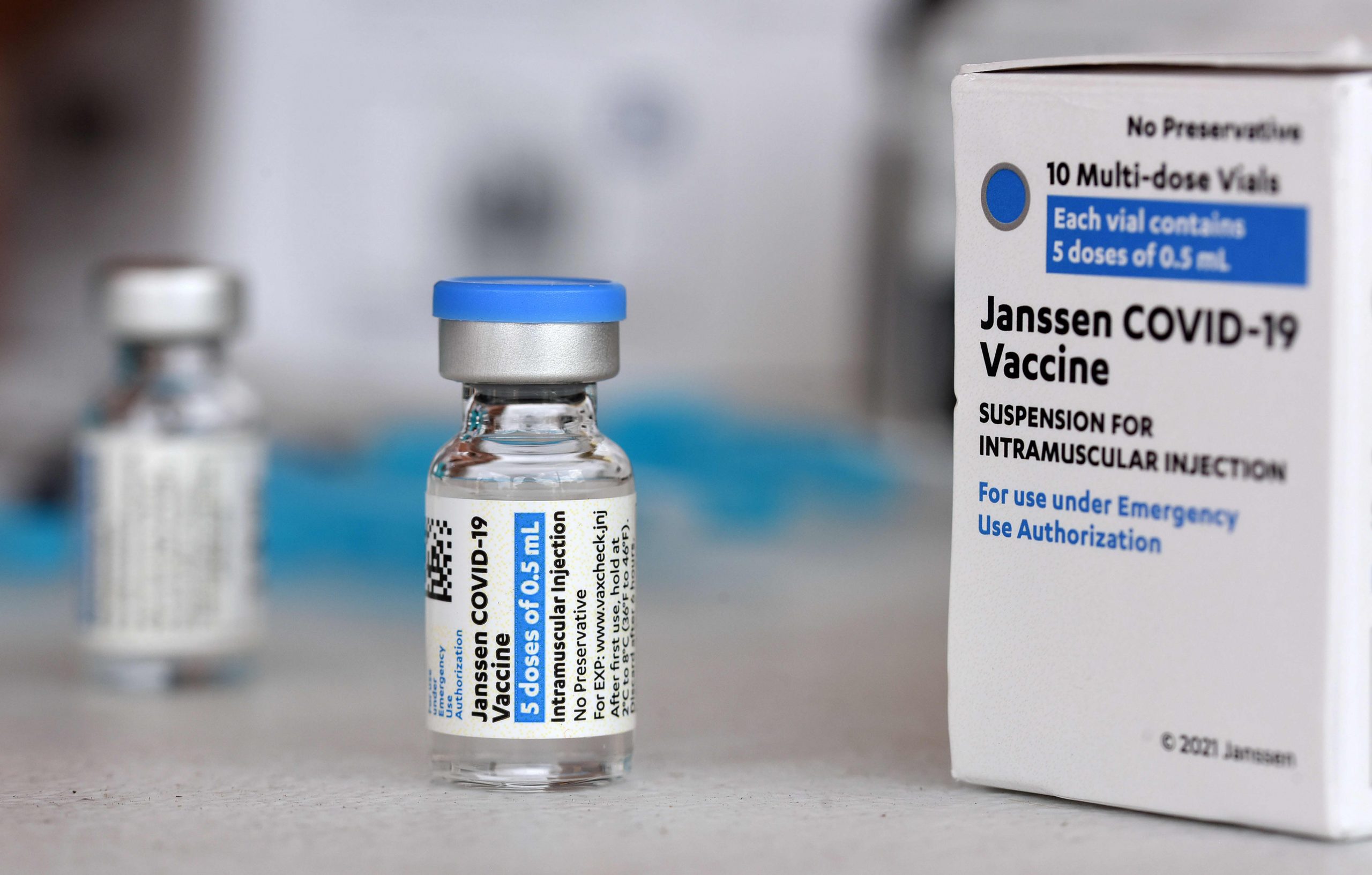
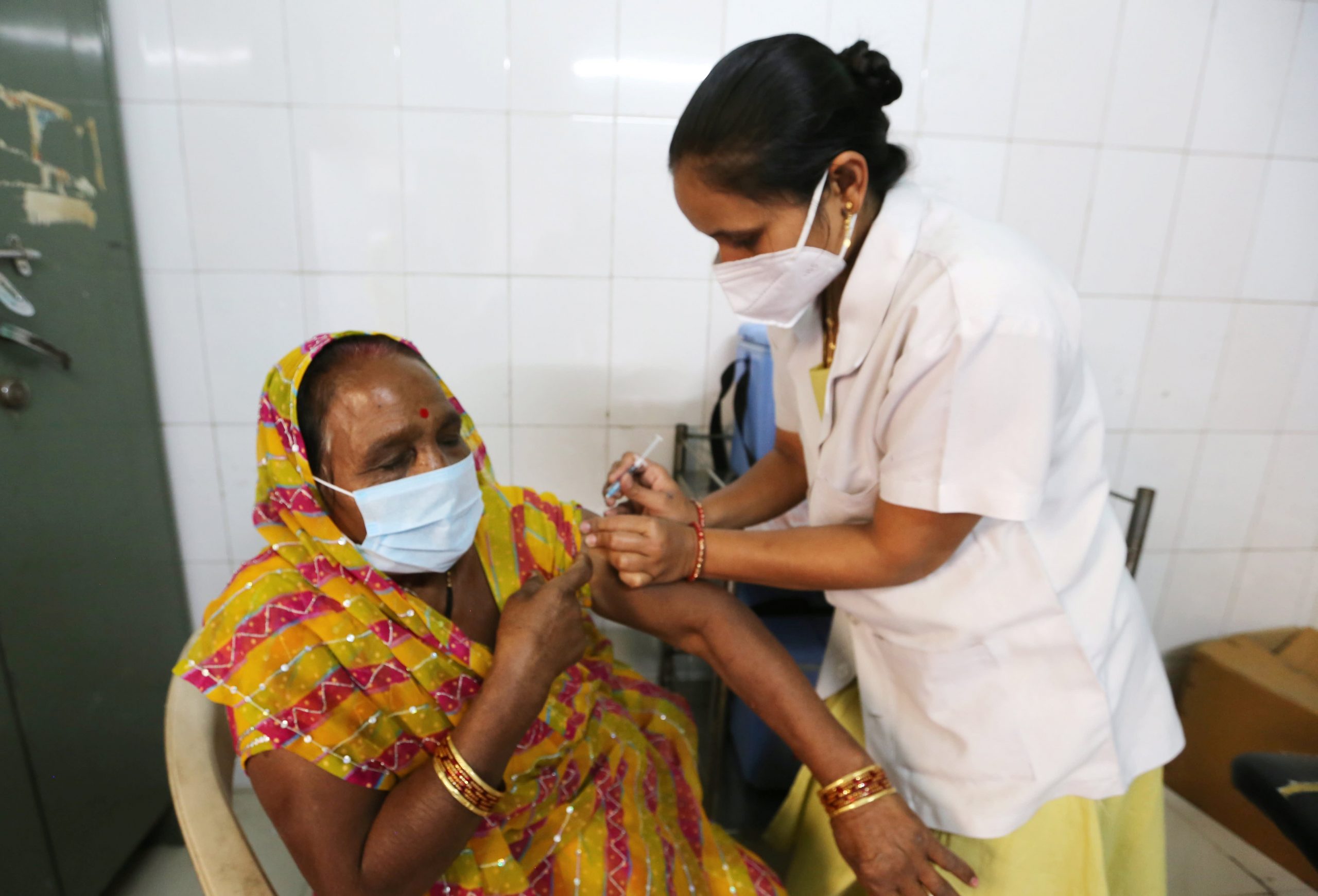
In late 1910, a deadly plague spread across northeast China and reached the city of Harbin. Tens of thousands of people coughed blood; Her skin was circumcised and turned purple. They all died.
This outbreak shook the Qing government: They did not know what disease caused these deaths, much less how to control them. So they brought in one of the best trained doctors in Asia at the time, Dr. Wu Lien-Teh. After an autopsy, Dr. Wu Yersinia pestis, a bacterium similar to the one that caused the bubonic plague in the west. He recognized the Manchurian plague as a respiratory disease and urged everyone, especially health professionals and law enforcement officials, to wear masks.
The Chinese authorities followed his call and combined the masking with strict bans enforced by the police. Four months after the doctor was called in, the plague ended. Although Dr. Often overlooked in western countries, Wu is considered a public health pioneer in world history, helping to change the course of a respiratory disease spread by droplets that could have ravaged China in the early 20th century and potentially spread widely in addition, expand its borders.
While the Chinese followed these strategies at the time, health professionals in the US and other western countries struggled to get people to listen to them during the Covid-19 pandemic. China also faced challenges early on, but the country’s institutional memory from previous virus outbreaks helped turn the tide. And with many Americans giving up masking, striving to restore normalcy to places where the risk of infection remains high and reluctant to get vaccinated, some public health experts have turned to Dr. Respected Wu’s success and looked for lessons on how to deal with not only Covid but also future epidemics.
Some scientists Dr. Wu, however, believe that the wrong lesson is drawn from his legacy: no single individual can save a nation. “We can’t always wait for historical figures,” said Alexandre White, a medical sociologist and historian at Johns Hopkins University in Baltimore. Instead, he and other experts say countries like the United States must reckon with their unequal and strained public health systems in order to better cope with health threats.
Dr. Wu was born as Ngoh Lean Tuck on March 10, 1879 on Penang, an island off the coast of the Malaysian peninsula, as the son of Chinese immigrants. (He later changed his name to Wu Lien-Teh, sometimes spelled Wu Liande)
When he was 17 years old, Dr. Wu received a scholarship to study at Emmanuel College in England and stayed to study medicine at St. Mary’s Hospital in London. As part of his training, he studied infectious diseases at the Liverpool School of Tropical Medicine and the Pasteur Institute in Paris.
When he returned to Malaysia in 1903, Dr. Wu one of the earliest people of Chinese descent to graduate as a doctor from the west.
In May 1908, Dr. Wu and his wife went to China, where he was appointed Vice Director of the Imperial Army College near Beijing. This enabled him to investigate when people in Manchuria died of an unknown disease.
Dr. Wu entered a place where experts like him were in short supply and urgently needed. At the time, China was in political turmoil: Russia and Japan vied for control of Manchuria, and both saw the plague as an opportunity to advance their goals. Western countries at the time largely viewed China as “the sick man of the east,” a country overburdened with disease, opium addiction, and ineffective government.
Historians studying China say the government accepted and internalized this label. But when Dr. Wu entered, he had the social and political influence to be a catalyst for change.
Dr. Wu is often referred to as the “man behind the mask,” an inventor of the use of face coverings to prevent the spread of respiratory diseases. Much of that narrative came from him in his autobiography, said Marta Hanson, also a medical historian with Johns Hopkins. Earlier iterations of the mask existed in other countries, and some Chinese were already putting on Japanese-style respirators before Dr. Wu arrived in Harbin.
What is true is that Dr. Wu introduced and encouraged a Western-born idea to the Chinese public. The mask he designed was based on Victorian-era ventilators: layers of padding made of cotton and gauze tied with strings so the user could attach it to the head. The mask was cheap and easy to make.
In addition to the masks, officials enforced a strict cordon sanitaire, another method that dates back at least as far as the 19th century when French officials tried to contain the spread of yellow fever. Travel was restricted, government officials were ordered to shoot anyone who tried to escape, and police officers went door to door looking for someone who had died of the plague. Borrowing from some of these techniques during the fight against Covid last year, China severely restricted transportation around Wuhan and people needed permission from authorities to leave their homes.
In the spring, after the plague was brought under control in China, Dr. Wu hosted the International Pest Conference. Respirators and masks were the focus of the conversation, and many Western scholars believed they could be effective in preventing the plague.
While masks became a political hotspot during the Spanish pandemic flu in the US and elsewhere, the idea of using them persisted in China, and gauze masks became a major tool on the Nationalist Party’s political agenda when it took over in 1928. Public health officials recommended that all citizens wear gauze masks when they have an outbreak of meningitis or cholera in public places.
By then, masks had become a symbol of hygienic modernity and contributed to the greater acceptance of wearing masks in China, said Dr. Hanson. At the beginning of the 21st century, the SARS epidemic has once again highlighted the need for masks and other public health interventions in China and other East Asian countries.
In 1930 Dr. Wu appointed head of new national health organization. But after the Japanese invaded northern China in 1937 and his house in Shanghai was shot at, Dr. Wu took refuge in his native Malaysia. There he ended his career as a family doctor and died in 1960 at the age of 80.
Medical historians and public health experts have several theories to support Dr. To explain Wu’s success in convincing the Chinese authorities to control the plague.
One factor that Dr. Wu likely helped, medical historians say, is by making masks affordable and accessible. A similar approach was used during the coronavirus pandemic in Hong Kong, where each resident was offered a free, reusable mask and kiosks were opened to the public for distribution.
Countries that have provided significant health mandate compliance assistance to their citizens during this pandemic have generally fared better than places that have left the same measures to individuals, said Dr. White by Johns Hopkins.
And the more affordable and accessible public health policies are, the more likely they are to be passed, said Kyle Legleiter, senior director of policy advocacy at the Colorado Health Foundation.
Another factor contributing to Dr. Wu’s success in China might have contributed to the awe residents and officials showed for him as a figure of authority, said Yanzhong Huang, senior fellow on global health at the Council on Foreign Relations.
In a way, Dr. Anthony Fauci, President Biden’s senior medical advisor at Covid and a well-known public health figure since the 1980s, has a role similar to that of Dr. Wu in China, said Dr. Huang. But his message may not always get through because Americans are more polarized in their political identities and beliefs.
Dr. Legleiter added that public health news only penetrates when the public identifies with or trusts this figure in authority.
“A single person represents a wider range of institutions or systems that they speak for,” said Dr. Legleiter. For example, those who are conservative may like Dr. Fauci and other scientists place them in the “elite” category. As such, they are more likely to violate the public health policies that such figures of authority promote and to adhere to the proclamations of those with whom they most identify.
Others say that public health is inseparable from the legitimacy of the state that promotes it. At the turn of the 20th century, China was in dire straits, said Dr. Hanson. Dr. Wu helped bring China out of a turbulent time, and enforcing public health measures gave the country more legitimacy.
Similarly, some experts believe the current pandemic may be a catalyst for change as it exposed public health systems in the United States, Britain, and other Western countries.
“Since the mid-19th century, the West has generally seen its ability to control infectious diseases as a sign of its civilizational superiority over much of the rest of the world,” said Dr. White. While China was then viewed as the sick man in the world, some commentators in China are now trying to brand the United States with that label.
Ruth Rogaski, a medical historian at Vanderbilt University who specializes in studying the Qing Dynasty and modern China, believes the coronavirus crisis is also an opportunity for thought, which can be very motivating.
“Epidemics can serve as turning points,” said Dr. Rogaski. “Opportunities to rethink, retool and even revolutionize health approaches.”