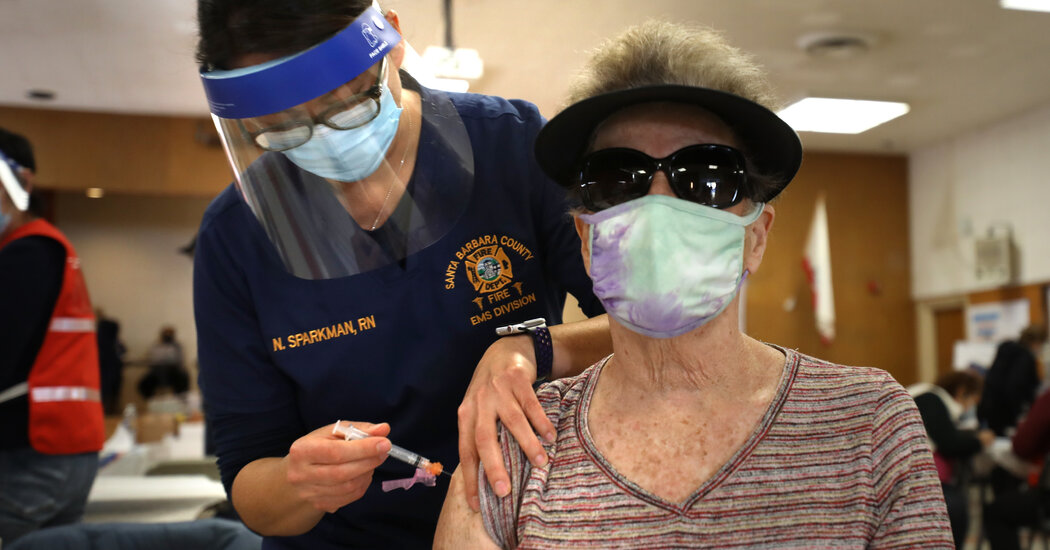
Many of the usual school opening requirements – including vaccines for teachers or students and low rates of infection in the community – are not required to safely teach children in person, according to a consensus among pediatric infectious disease experts in a new survey.
Instead, the 175 experts – mostly pediatricians with a focus on public health – largely agreed that it is safe for schools to now be open to elementary school students for full-time and in-person tuition. This also applies in communities where Covid-19 infections are widespread, provided that basic safety measures are in place. Most important are universal masking, physical distancing, adequate ventilation and avoidance of activities in large groups.
The experts were interviewed by the New York Times last week. Most believe that the level of virus spread in a community is not a key indicator of whether schools should be open, although many districts still rely on this metric. Schools should only close if there are Covid-19 cases in the school itself, most said.
“There is no situation where schools can only be opened if they have evidence of transmission in the school,” said Dr. David Rosen, Assistant Professor of Pediatric Infectious Diseases at Washington University in St. Louis.
The risk of dropping out of school is far greater, said many experts. “The mental health crisis caused by school closings will be a worse pandemic than Covid,” said Dr. Uzma Hasan, Head of Pediatric Infectious Diseases at RWJBarnabas Health in New Jersey.
These responses are largely in line with current federal guidelines that make no mention of vaccines and reflect key scientific evidence that schools are not a primary source of child or adult spread. The Centers for Disease Control and Prevention is expected to publish new recommendations on how to run schools safely on Friday, and the Biden administration has given priority to opening schools.
However, the expert consensus in the survey contradicts the position of certain policy makers, school administrators, parent groups and teacher unions. Some in these groups have indicated that they do not want to return to school buildings next fall if it is likely that teachers can be vaccinated, although not most of the students. Some districts have put up stiff resistance to the reopening, especially in large cities where teachers have threatened to strike if they are called back to school buildings.
Some experts agreed that open schools pose a risk, especially for the adults working there, saying that many parts of the country have not yet controlled the virus enough to be opened safely.
“If we wanted schools to reopen safely, we as a society would have had to work hard to keep transmission rates low and to invest resources in schools,” said Dr. Leana Wen, Emergency Doctor and Visiting Professor of Health Policy at George Washington University.
About half of the country’s students are still studying from home, and while the majority of districts have at least some face-to-face learning and are trying to reopen this spring, many students offer just a few hours a day or a few days a week .
The mismatch between the experts ‘preferred guidelines and school opening rules in many districts reflects political considerations and union demands, but it also changes scientists’ understanding of the virus. Many school policies were developed months ago before there was mounting evidence that Covid-19 did not spread easily in schools where basic safety precautions were in place. The guidelines could change again, they warned: Almost everyone raised concerns that new coronavirus variants could disrupt schools’ plans to be open in the spring or fall.
More than two-thirds of respondents said they had school-age children, and half had children in school at least temporarily. Overall, they were more likely to support opening their own schools. About 85 percent of those in communities where schools were open all day said their district made the right call, while only a third of those in places where schools were still closed made the right choice.
Updated
Apr. 11, 2021, 3:40 p.m. ET
“Closing the school in spring 2020 was the right decision: we didn’t know much about Covid at the time and didn’t know what role children could play in the transmission,” said Dr. Mitul Kapadia, director of pediatric physical medicine at the University of California, San Francisco. “We know now, and we know schools can open safely. Fear guides decisions even against the guidelines and recommendations of the medical and public health communities. “
The point of most agreement was to require masks for everyone. All respondents said it was important and many said it was a simple solution that made the need for other conditions for opening less important.
“What works in healthcare, masks, will work in schools,” said Dr. Danielle Zerr, professor and director of pediatric infectious diseases at the University of Washington. “Children are good at wearing masks!”
Half of the panel said a full return to school with no precautions – no masks, full classrooms, and all restored activity – would require all adults and children in the community to have access to vaccinations. (Vaccines have not yet been tested in children and will most likely not be available until 2022.)
But not everyone agreed that younger children need to be vaccinated to return to pre-pandemic school life. A fifth said a full reopening could occur without precaution once adults in the community and students were vaccinated, and 12 percent said it could happen once vaccines are available to all adults in the community.
The experts also questioned another strategy used by many districts that are open or due to open this spring: part-time opening for small and permanent cohorts of students who take turns participating in class schedules to reduce class size and the To maximize the distance between people. Only a third said it was very important for schools to do this, although three quarters said students should be six feet apart for some or all of the time. Three quarters said schools should avoid crowds, such as in hallways or cafeterias.
With universal masking, “school transfers are close to zero and cohorts are not required,” said Dr. Jeanne Ann Noble, Emergency Medicine Physician and Director of Covid Response at the University of California at San Francisco.
Limiting school hours increased other risks, such as disrupting children’s social development, disrupting family routines, and increasing the likelihood of children being exposed to a larger group of people outside of school.
The experts expressed deep concern about other risks for staying home students, including depression, hunger, anxiety, isolation, and learning loss.
“Children’s learning and emotional and in some cases physical health are severely affected by early school leaving,” said Dr. Lisa Abuogi, a pediatric emergency physician at the University of Colorado, and gave her personal opinions. “I spend some of my clinical time in the emergency room and the psychological distress we see in school-related children is no longer current.”
Respondents came from membership lists of three groups: the Pediatric Infectious Diseases Society, the Decision Sciences for Child Health Collaborative, and the American Academy of Pediatrics’ sub-specialty group in Epidemiology, Public Health, and Evidence. Some individual scientists also replied. Almost all of them were doctors, and more than a quarter of them had degrees in epidemiology or public health. Most worked in academia and about a quarter in clinical settings, and most said their daily work was closely related to the pandemic.
The survey asked experts about various strategies schools use to protect students and staff. The experts said many such measures would have some value, but identified two as the most important: wearing masks and distancing themselves.
Other widely used measures – such as frequent disinfection of buildings and surfaces, temperature controls, or the use of Plexiglas partitions – were seen as less important. A quarter said routine surveillance tests of students and staff are very important for opening schools.
“Masks are key,” said Dr. Noble. “Other interventions create a false sense of security.”
Many states have tied openings to community dissemination measures in the school, such as: B. the positivity rate of tests, the rate of new infections or the rate of hospital stays. But 80 percent of the experts said school districts shouldn’t base reopening decisions on infection data across the county. You should focus on virus cases in school.
Many districts have opened or are considering opening up to younger students before older ones. Research has shown that infection and spread in adolescent children become more similar to adults. The Biden administration has designed its reopening plans for children in kindergarten through eighth grade.
Just over half of pediatric infectious disease experts said fifth grade should be the cutoff when schools are partially open. Only 17 percent said the eighth grade should be. Despite the greater risk faced by high school students, many complained about the long-term effects of a year of extreme isolation on teenagers.
Although these experts specialized in children’s physical health, many concluded that the risks to mental health, social skills, and education outweighed the risks of the virus. The future prospects of the students, said Dr. Susan Lipton, director of pediatric infectious diseases at Sinai Hospital in Baltimore, are “torpedoed without the best academics, interaction with inspiring teachers who become mentors, clubs, sports and other opportunities to shine.”
“This is a generation devastating,” she said.