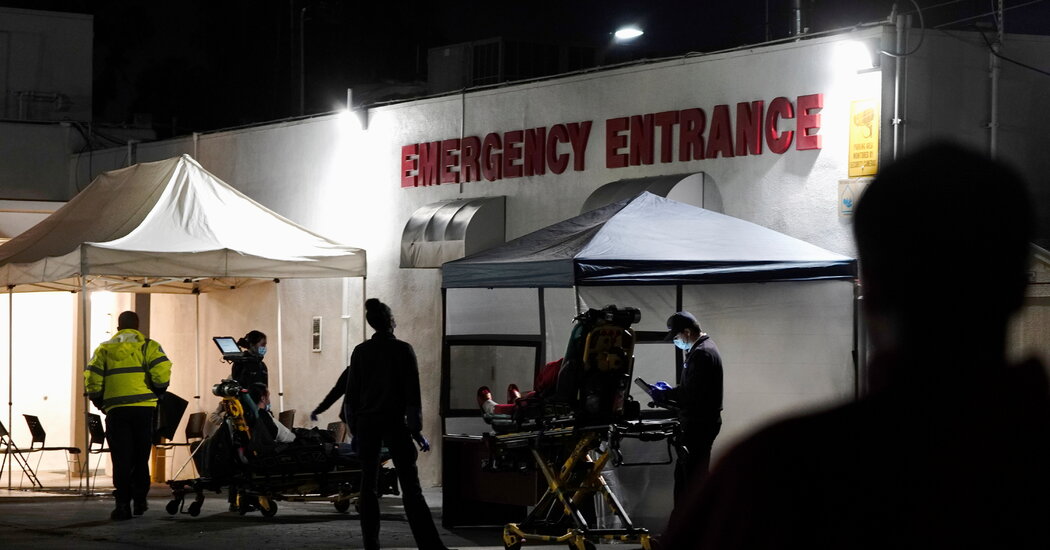
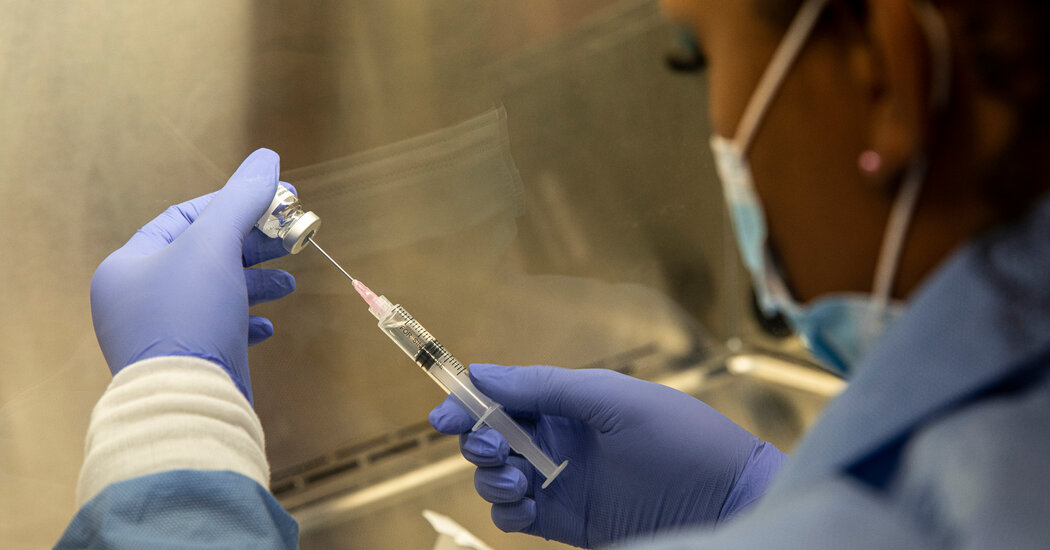
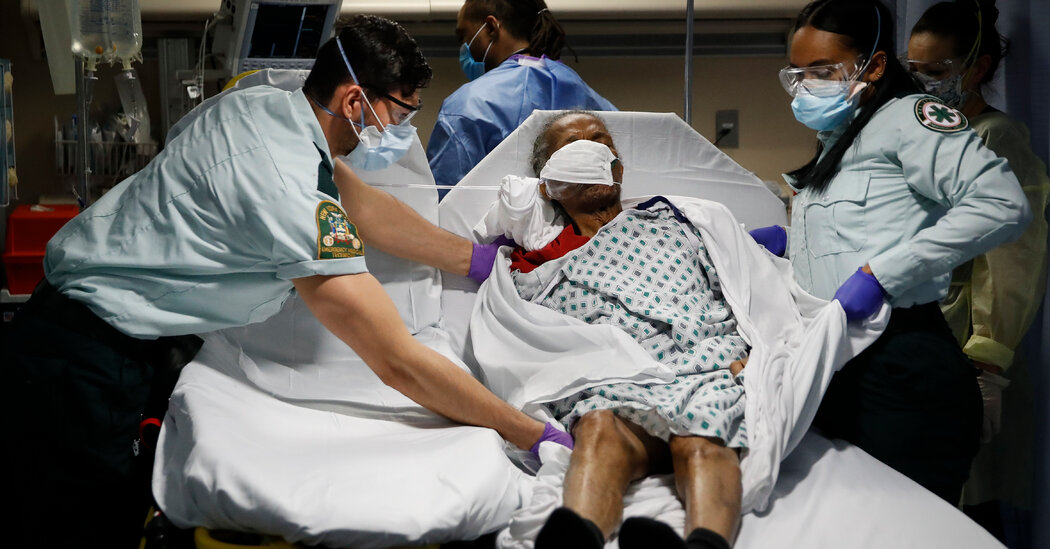
WASHINGTON — More than 200,000 Americans flocked to the Affordable Care Act’s online marketplace to sign up for health insurance during the first two weeks of an open enrollment period created by President Biden — a sign that those who lost insurance during the pandemic remain in desperate need of coverage.
At the same time, a provision in the president’s $1.9 trillion stimulus law to make Medicaid expansion more fiscally appealing has prompted deeply conservative Alabama and Wyoming to consider expanding the government health program to residents who are too rich to qualify now but too poor to afford private health plans.
Eleven years after President Barack Obama signed his signature domestic achievement, and after several near-death experiences, the health law is again expanding.
The Biden White House will celebrate Tuesday’s anniversary in a big way. The president will visit Ohio as part of his “Help Is Here” tour to talk up the stimulus law, which greatly expanded subsidies to make insurance affordable for tens of millions of people. And Mr. Biden’s newly installed health secretary, Xavier Becerra, whom the Senate confirmed just last week, will travel to Carson City, Nev., to help mark the moment.
The provision in the $1.9 trillion “American Rescue Plan” is the first major change to the health law since its passage. The new subsidies last for only two years, and it will take some time for the full emergency aid to reach people. Even so, nearly everyone who buys insurance will be eligible to do so at a discount.
But Mr. Biden has a new challenge: living up to his campaign promise to expand the law, including making the new subsidies permanent, creating a “public option” for consumers who wish to buy into a government-run insurance plan, and tackling not only the rising cost of health insurance premiums, but also the soaring price of prescription drugs.
“The Affordable Care Act was about trying to create the ground rules so that health insurance was real — it provided real financial security and was affordable — but we’re at this point where we’ve got to address the other side of the equation,” said Frederick Isasi, the executive director of Families USA, a consumer advocacy group that has supported the law.
“We’ve got to address the sector’s pricing abuses, and that’s fundamentally the big question the administration and Congress are facing,” Mr. Isasi added. “Are they going to have the political will to do that?”
On Capitol Hill, Mr. Biden is facing pressure from the left. Last week, progressives introduced legislation to create what they call “Medicare for all,” a single-payer, government-run insurance program that has been embraced by Senator Bernie Sanders, independent of Vermont, and Representative Alexandria Ocasio-Cortez, Democrat of New York.
Interest among Democrats appears to be growing; a majority of the caucus now backs the bill, and several moderates have recently signed on as sponsors, including Representative Frank Pallone Jr., Democrat of New Jersey and the chairman of the House Energy and Commerce Committee, which has jurisdiction over the measure. He has scheduled a hearing for Tuesday to consider legislation to expand health coverage and lower costs.
“The energy around it is largely stoked by the horrible things we’ve seen over the last year,” said Representative Pramila Jayapal, Democrat of Washington, the lead sponsor of the Medicare for All Act. She added, “Even if we do the things we are doing right now, we are still leaving out too many people, and we are still not addressing the cost issues of this unsustainable for-profit system.”
Mr. Biden, however, rejected Medicare for all during his campaign, and a senior administration official said Wednesday that the president did not intend to embrace the plan.
About 30 million Americans remain uninsured, and the Kaiser Family Foundation recently estimated that the number of people with employer-based insurance dropped by two million to three million from March to September last year. But the foundation has also estimated that 85 percent of those who lost coverage were eligible for either Medicaid or for subsidies under the Affordable Care Act — an option that did not exist during the last major recession.
“This is really the first true test of the A.C.A.,” said Cynthia Cox, who directs a Kaiser Family Foundation program on the law. “In past recessions, you usually see the uninsured rate increase significantly. We don’t know for sure yet, but all indications are that the uninsured rate has not gone up by much, likely in large part thanks to the A.C.A.”
Expanding access to health care has been a core issue for Mr. Biden, both when he was vice president and during his campaign for the White House. When the act was signed into law, he memorably used an expletive to whisper in Mr. Obama’s ear that it was a big deal.
A week after he took office, Mr. Biden ordered the law’s federally run insurance marketplace to reopen for three months, from February to May 15, to help people struggling to find coverage.
In previous years, Americans in the 36 states that rely on the federal marketplace were eligible to sign up outside the fall enrollment period only if they had “qualifying life events,” including job losses. The current surge in enrollment is more than double the number of people who signed up during the same two-week periods in 2019 and 2020.
Frequently Asked Questions About the New Stimulus Package
How big are the stimulus payments in the bill, and who is eligible?
The stimulus payments would be $1,400 for most recipients. Those who are eligible would also receive an identical payment for each of their children. To qualify for the full $1,400, a single person would need an adjusted gross income of $75,000 or below. For heads of household, adjusted gross income would need to be $112,500 or below, and for married couples filing jointly that number would need to be $150,000 or below. To be eligible for a payment, a person must have a Social Security number. Read more.
What would the relief bill do about health insurance?
Buying insurance through the government program known as COBRA would temporarily become a lot cheaper. COBRA, for the Consolidated Omnibus Budget Reconciliation Act, generally lets someone who loses a job buy coverage via the former employer. But it’s expensive: Under normal circumstances, a person may have to pay at least 102 percent of the cost of the premium. Under the relief bill, the government would pay the entire COBRA premium from April 1 through Sept. 30. A person who qualified for new, employer-based health insurance someplace else before Sept. 30 would lose eligibility for the no-cost coverage. And someone who left a job voluntarily would not be eligible, either. Read more
What would the bill change about the child and dependent care tax credit?
This credit, which helps working families offset the cost of care for children under 13 and other dependents, would be significantly expanded for a single year. More people would be eligible, and many recipients would get a bigger break. The bill would also make the credit fully refundable, which means you could collect the money as a refund even if your tax bill was zero. “That will be helpful to people at the lower end” of the income scale, said Mark Luscombe, principal federal tax analyst at Wolters Kluwer Tax & Accounting. Read more.
What student loan changes are included in the bill?
There would be a big one for people who already have debt. You wouldn’t have to pay income taxes on forgiven debt if you qualify for loan forgiveness or cancellation — for example, if you’ve been in an income-driven repayment plan for the requisite number of years, if your school defrauded you or if Congress or the president wipes away $10,000 of debt for large numbers of people. This would be the case for debt forgiven between Jan. 1, 2021, and the end of 2025. Read more.
What would the bill do to help people with housing?
The bill would provide billions of dollars in rental and utility assistance to people who are struggling and in danger of being evicted from their homes. About $27 billion would go toward emergency rental assistance. The vast majority of it would replenish the so-called Coronavirus Relief Fund, created by the CARES Act and distributed through state, local and tribal governments, according to the National Low Income Housing Coalition. That’s on top of the $25 billion in assistance provided by the relief package passed in December. To receive financial assistance — which could be used for rent, utilities and other housing expenses — households would have to meet several conditions. Household income could not exceed 80 percent of the area median income, at least one household member must be at risk of homelessness or housing instability, and individuals would have to qualify for unemployment benefits or have experienced financial hardship (directly or indirectly) because of the pandemic. Assistance could be provided for up to 18 months, according to the National Low Income Housing Coalition. Lower-income families that have been unemployed for three months or more would be given priority for assistance. Read more.
During the last open enrollment period, 340,000 new users of the marketplace signed up during the first two weeks. That period ended on Dec. 15.
That an additional 200,000 people signed up so soon “is not surprising,” given the pandemic-driven need, said Mr. Isasi, of Families USA.
What is surprising, said Ms. Cox, of the Kaiser Family Foundation, is that Republicans in Alabama and Wyoming — states among those that have doggedly rejected the Medicaid expansion that the law encouraged — have raised the prospect of doing so under generous incentives included in the stimulus law.
In Alabama, a spokeswoman for Gov. Kay Ivey, a Republican, has said that the governor is “open to the discussion” about expanding Medicaid, but that state leaders needed more information about the cost. In Wyoming, a bill to authorize Medicaid expansion, sponsored by a Republican lawmaker, gained committee approval last week in the State Legislature and passed the Wyoming House on Monday night, according to The Casper Star-Tribune, though the State Senate had killed a similar bill earlier that evening.
“I don’t think anyone was necessarily expecting any states to take this money,” Ms. Cox said. “It’s a significant financial incentive that states have to expand Medicaid, but the thought was that there would be so much political opposition in these states that they might not want to expand the program.”
The Affordable Care Act has been under attack from Republicans since its passage, both in the courts and on Capitol Hill, where Republicans tried but repeatedly failed to repeal the measure. The push in the courts did scale back the initial law, when the Supreme Court invalidated its provision requiring states to expand Medicaid.
The legal campaign to undo the law continues. The Supreme Court is currently considering whether Congress’s elimination of financial penalties for most Americans who fail to obtain insurance rendered the whole law unconstitutional. But during oral arguments, at least five justices indicated they were likely to keep the law intact.
The Trump administration, which pushed the lawsuit, worked aggressively to gut the health law. President Donald J. Trump used his executive authority to make it easier for small businesses to band together and offer plans that escape some of the requirements of the Affordable Care Act, like mental health coverage and maternity care.
He also sharply cut funding for “health care navigators” to help consumers, who were left to sift through insurance options largely on their own. A survey last year by the Kaiser Family Foundation found that about half of those who looked for coverage during the 2020 open enrollment period encountered difficulties, and nearly five million consumers sought in-person help but were unable to get it. The Biden administration is now running television commercials promoting the open enrollment period and is spending $2.3 million to support navigator programs.
Democrats, including Mr. Obama and Speaker Nancy Pelosi, who was also speaker in 2010 and was crucial to the law’s passage, were hoping to celebrate the 10th anniversary of the Affordable Care Act with much fanfare last year, but the emerging coronavirus pandemic scuttled their plans.
Instead, Mr. Obama posted a slickly produced video on his Facebook page that opened with an image of him surrounded by White House staff members rising in applause as Congress approved the legislation — a night, he said in the video, that “meant more to me than the night I was elected.” To his right, rising up beside him, was the future president, Mr. Biden.