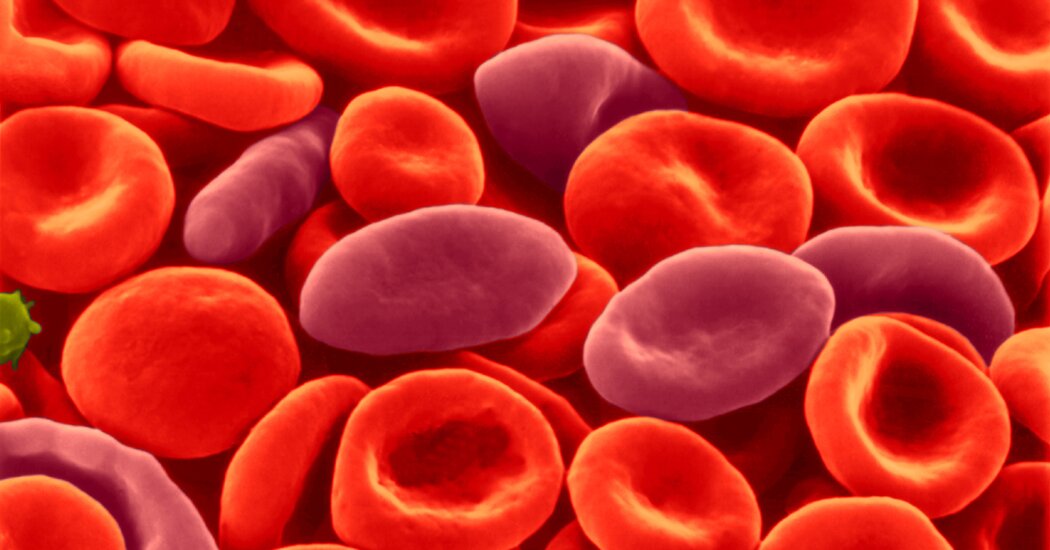
Hayley Arceneaux, 29, had hoped this would be the year she would achieve her goal of visiting all seven continents before she turned 30.
However, she won’t have time for it.
She goes into space.
Ms. Arceneaux, a medical assistant at St. Jude Children’s Research Hospital in Memphis, will be one of four people on a SpaceX Falcon 9 rocket taking off from Florida. It’s slated to launch later this year and be the first crewed mission to orbit Earth where no one on board is a professional astronaut.
“I asked, ‘Will I get a passport stamp to go into space?'” Ms. Arceneaux said. “But I don’t think I’ll do it. So I’ll just draw a star and the moon in one of my passports. “
This adventure is led by Jared Isaacman, a 38-year-old billionaire who announced in January that he had bought the rocket launch from SpaceX, the space company founded by Elon Musk. Mr. Isaacman said at the time that he wanted the mission to be more than an outing for the super rich and that he had given St. Jude two of the four available spots.
One of them will go to a random winner of a sweepstakes competition to raise money for the hospital, which treats children for free and develops cures for childhood cancer and other diseases.
The other seat, Isaacman said, is occupied by a front line health worker in St. Jude, someone who symbolizes hope.
On Monday, St. Jude and Mr. Isaacman officials announced that Ms. Arceneaux was the person they had selected.
Ms. Arceneaux could be the youngest American to ever travel to orbit. She will also be the first person to go into space with a prosthetic body. She was a patient in St. Jude nearly 20 years ago, and metal bars replaced parts of the bones in her left leg as part of her treatment for bone cancer.
In the past, this would have kept her firmly on the ground and would not have been able to meet NASA’s strict medical standards for astronauts. But the advent of privately funded space travel has opened the final frontier to some people who were previously excluded.
Dr. Michael D. Neel, the orthopedic surgeon who installed Ms. Arceneaux’s prosthesis, says that while artificial leg bones mean she can’t practice contact sports on Earth, they shouldn’t limit her on this SpaceX trek.
“It shows us that the sky is not the limit,” said Dr. Neel. “It’s Heaven and Beyond. I think that’s the real point of it all, that it has very few restrictions on what you can do. Unless you’re playing soccer up there. “
Ms. Arceneaux said she hoped to inspire patients at St. Jude.
“You will be able to see a cancer survivor in space, especially one who went through the same thing as you,” she said. “It will help you visualize your future.”
Richard C. Shadyac Jr., president of ALSAC, the St. Jude fundraising organization, said of Ms. Arceneaux, “If anyone was a symbol of hope, it was Hayley.”
Mrs. Arceneaux herself did not find out until early January that she would take a seat on the rocket. Hospital officials had vaguely told her there was an opportunity they wanted to talk to her about. She said she thought “maybe it would be a commercial or maybe give a speech somewhere.”
Instead, it was an opportunity to become an astronaut.
“I even kind of laughed,” said Ms. Arceneaux. “I thought: what? Yes. Yes, please, that would be great. “She added,” Let me talk to my mom. “
Her mother had no objection.
Ms. Arceneaux first stepped on St. Jude in 2002. She was 10 years old. She had earned her black belt in taekwondo shortly before, but complained of pain in her leg. Her mother saw a lump sticking out over her left knee. The pediatrician in the small town of St. Francisville, La., Where they lived not far from Baton Rouge, told them it was a cancerous tumor.
“We have all fallen apart,” said Mrs. Arceneaux. “I remember being so scared because by the age of 10 everyone I knew with cancer had died.”
In St. Jude, doctors gave the good news that the cancer had not spread to other parts of the body. Ms. Arceneaux had chemotherapy, prosthetic leg surgery, and long sessions of physical therapy.
Already at this young age, bald from chemotherapy, Ms. Arceneaux was helping with fundraising for St. Jude. The next year she was recognized by Louisiana Public Broadcasting with one of its Young Heroes Awards.
“When I grow up, I want to be a nurse in St. Jude,” she said in a video shown at the 2003 ceremony. “I want to be a mentor to patients. When they walk in I’ll say, “I had this when I was little and I’m fine.”
Last year Ms. Arceneaux was hired by St. Jude. She works with children with leukemia and lymphoma, such as a teenager she recently spoke to.
“I informed him that I had also lost my hair,” said Ms. Arceneaux. I said to him, ‘You can ask me anything. I am a former patient. I will tell you the truth, everything you want to know. ‘And he said,’ Are you really going to tell me the truth? ‘ And I said yes. “
His burning question: “Are you the one who goes into space?”
Mrs. Arceneaux had to evade. “I said, ‘Well, we’ll see who gets announced.'” She said. “But I think he knew because then he and his father said,” Yes! “and fifty.”
Ms. Arceneaux and Mr. Isaacman visited SpaceX’s California headquarters three times to meet with engineers and plan the trip. Unlike the missions SpaceX flies for NASA, it won’t go to the International Space Station, but will orbit the earth for three or four days before splashing off the coast of Florida.
“She has an adventurous spirit,” said Isaacman of Ms. Arceneaux. “And now she’s allowed to travel to the stars, which is pretty cool.”
It will be a few more weeks before they know who their companions will be.
The St. Jude Sweepstakes, featured in a television commercial that aired during the Super Bowl two weeks ago, will run until the end of the month. Around $ 9.5 million has been raised to date. That appears to be way below the $ 100 million Isaacman himself pledged for St. Jude, or the overall goal of $ 200 million. But Mr. Isaacman and Mr. Shadyac said the fundraiser was going beyond the sweepstakes and that they were happy with the progress.
“This is going to be a campaign that will last until launch,” said Shadyac.
The competition is structured in such a way that the amount of donations is effectively limited. Entry is free. A minimum donation of $ 10 buys 100 entries, and each additional dollar donated buys 10 additional entries, up to $ 1,000 for 10,000 entries.
There were some more expensive options that are now sold out. For example, Mr. Isaacman will give a donor who has donated $ 100,000 a ride on the Russian-built MiG-29 jet fighter he owns. The donor will also be given a trip to watch the launch at the Kennedy Space Center in Florida. But that donor still only has 10,000 entries in the contest, just like someone who donated $ 1,000.
Mr. Isaacman said this was a deliberate choice to prevent a wealthy person from trying to win the grand prize of a trip to space by buying millions of items.
“Will it represent everyone on earth and not just rich whites?” Mr. Isaacman said.
The fourth SpaceX seat goes to the winner of a competition sponsored by Shift4, Isaacman’s company, that sells terminals and point of sale systems for credit card processing to restaurants and other businesses. The “Shark Tank” -like competition calls on entrepreneurs to design an online shop with the Shift4 software and then publish a video on Twitter describing their business.
As of last week, fewer than 100 people had submitted full entries. “It means that once you’ve created and entered a Shift4 store, your chances are pretty amazing,” said Isaacman.