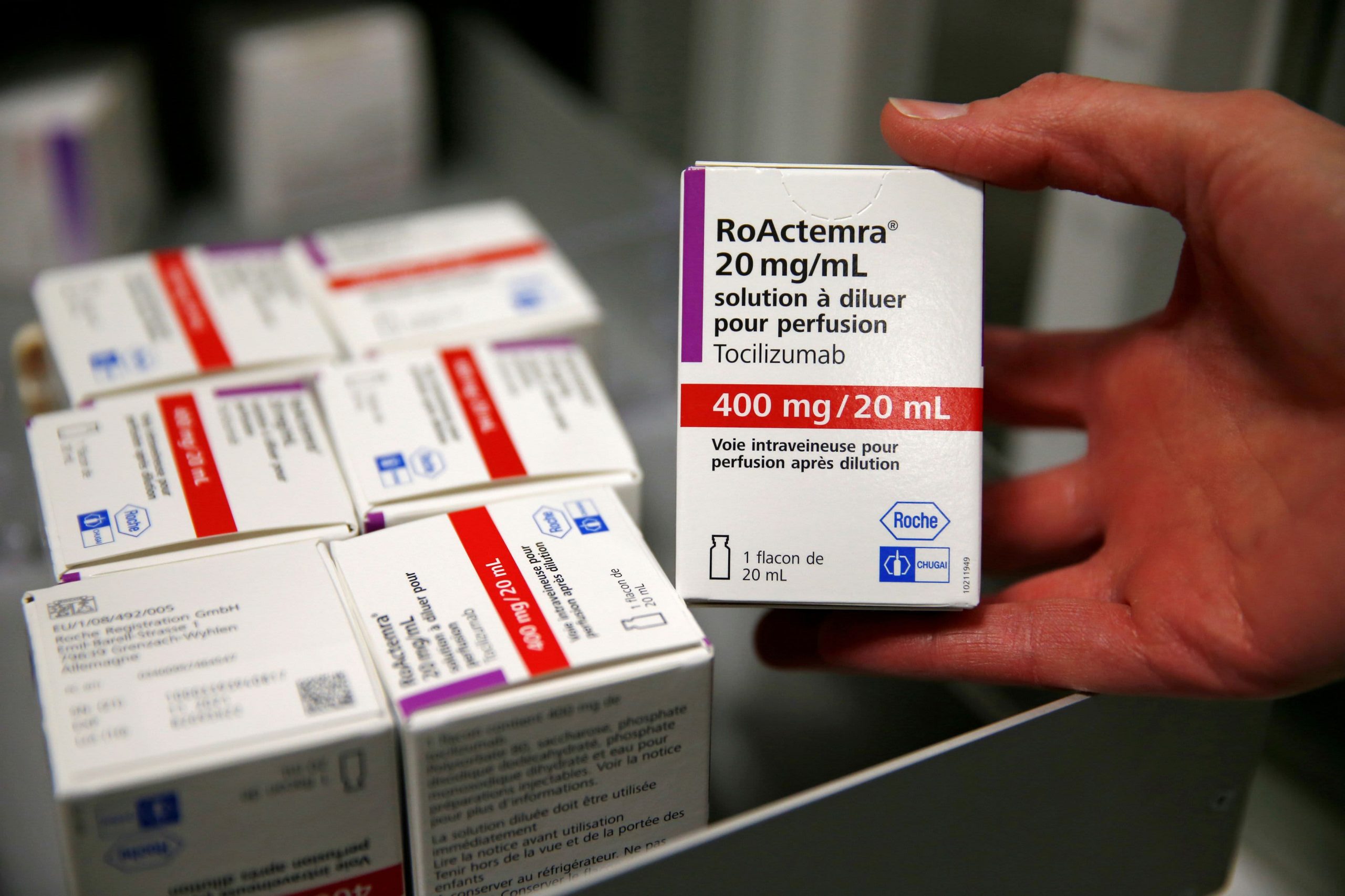
A pharmacist shows a box of tocilizumab, which is used to treat rheumatoid arthritis, in the pharmacy of Cambrai Hospital in France on April 28, 2020.
Pascal Rossignol | Reuters
A drug used to treat people with rheumatoid arthritis appears to reduce the risk of death in hospitalized patients with severe Covid-19, especially when combined with the steroid dexamethasone, Oxford University researchers said Thursday.
Oxford researchers found that the drug tocilizumab, an intravenous drug of A department of the Swiss drug manufacturer Roche also shortened the length of stay for patients in hospitals and reduced the need for a ventilator. The study was part of the recovery study, which has tested a number of potential treatments for Covid-19 since March.
“Previous studies of tocilizumab had shown mixed results and it was unclear which patients might benefit from the treatment,” said Peter Horby, professor at Oxford University and co-investigator for the recovery study, in a statement. “We now know that tocilizumab benefits apply to all COVID patients with low oxygen levels and significant inflammation.”
A total of 2,022 patients were randomly selected to receive tocilizumab, sold under the brand name Actemra, by intravenous infusion and compared to 2,094 patients who were randomly selected to receive standard care alone. The researchers said 82% of patients were also taking a steroid like dexamethasone, another drug that was found to reduce deaths in the sickest Covid-19 patients.
Researchers said 596 patients in the tocilizumab group died within 28 days, compared with 694 patients in the standard care group. That means that for every 25 patients treated with tocilizumab, “an extra life would be saved,” said Oxford researchers.
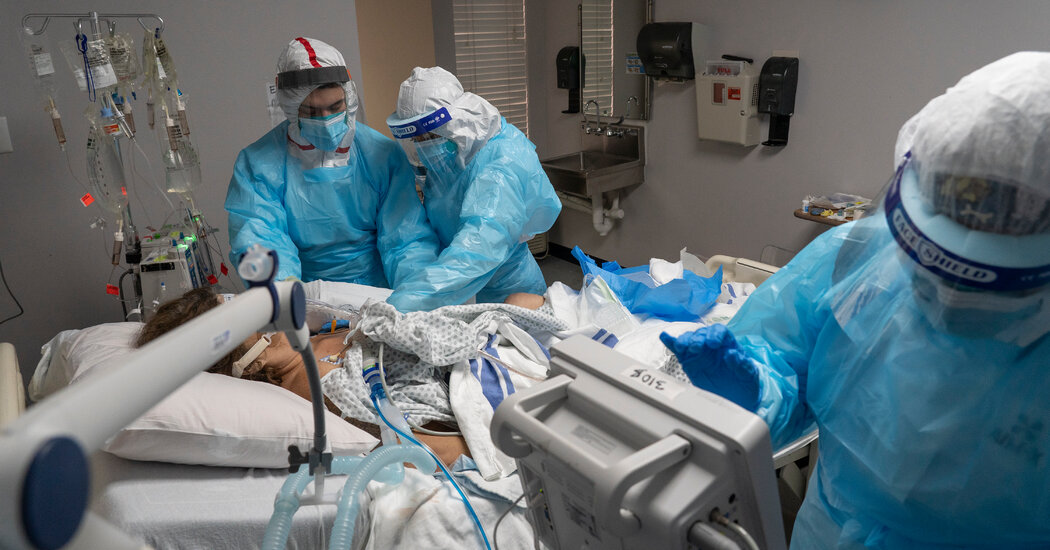
The drug increased the chances of being discharged from 47% to 54% within 28 days, the researchers said. The benefits have been seen in all patients, including those who need mechanical ventilators in an intensive care unit, they added. In patients who were not given a ventilator prior to the start of the study, tocilizumab reduced the chance of getting invasive mechanical ventilation or death from 38% to 33%, the researchers said.
The researchers said that using tocilizumab in combination with dexamethasone reduced mortality by about a third in patients who require oxygen and by almost half in patients who require a ventilator.
The results of the Oxford study have not yet been published in a peer-reviewed journal.
Public health officials and infectious disease experts say world leaders will need a range of drugs and vaccines to end the pandemic that, according to Johns, will infect more than 107.4 million people in just over a year and has killed at least 2.3 million people at Hopkins University.
In the US, the Food and Drug Administration has approved Gilead Sciences’ antiviral drug Remdesivir for the treatment of Covid-19 patients who are 12 years or older and require hospitalization.
The FDA has approved the use of two monoclonal antibody treatments as well as two vaccines – from Pfizer and Moderna. A third vaccine from Johnson & Johnson is expected to receive FDA approval as early as this month.
The Covid-19 Therapy Randomized Evaluation, or Recovery Study, was launched in March by researchers at Oxford University to find treatments for Covid-19. The study previously showed that hydroxychloroquine, lopinavir ritonavir, azithromycin, and convalescent plasma had no benefits for patients hospitalized with Covid-19.
The study is currently investigating aspirin, the anti-inflammatory drugs baricitinib and colchicine, and Regeneron’s antibody cocktail.