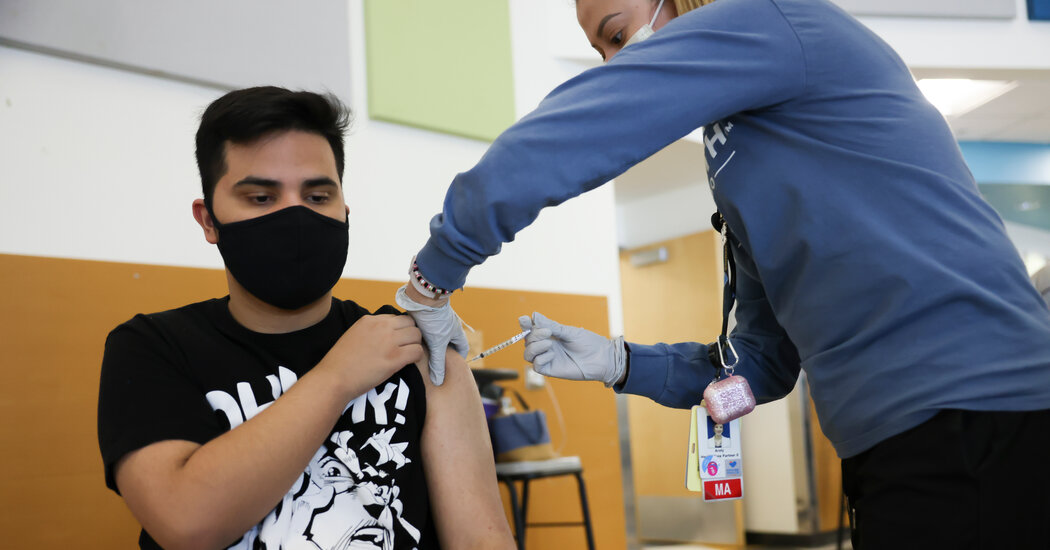
Magic mushrooms are seen in a grow room in the Netherlands in this 2007 file photo.
Peter Dejong | AP
Entrepreneur Dick Simon has never shied away from speaking up about business topics other CEOs might find too stigmatized to touch. He has spent years dedicated to improving U.S. business relations with Iran, and more recently, the Boston-based CEO has embraced another passion: improving the market for and medical community’s understanding of how psychedelic drugs can be used to treat mental illness. It’s a health, and emerging health business, that Simon came to appreciate through the firsthand frustration of watching people in his life suffering — not just from mental illness, but from the failure of existing and costly medical treatments.
Drugs long stigmatized, such as psilocybin and MDMA, are rising in profile as mental illness treatment options. Just last week, results from a phase 3 trial of MDMA combined with talk therapy for post-traumatic stress disorder showed results that were impressive.
“This is a pivotal event,” said Elemer Piros, a biotech analyst at Roth Capital Partners who covers the emerging alternative mental health treatment space. “It may not seem humongous, but it is one of the best and most rigorously executed trials in the space. And the results corroborate what we have seen time and time again from smaller studies over the past two decades,” he said, referencing remission rates double that of a placebo. “The magical experiences kept showing up, but no one had the courage to take it through to regulators.”
The annual Healthy Returns Summit is on Tuesday, May 11. Meg Tirrell speaks with CDC’s Dr. Rochelle Walensky, Pfizer’s head of vaccine R&D, and Eli Lilly CEO David Ricks. Bertha Coombs talks mental health care with Centene CEO Michael Neidorff and dives into the future of telehealth with Teladoc CEO Jason Gorevic. Jim Cramer closes the day with Abbott CEO Robert Ford. Register now.
The results of the MDMA study, whose senior author is Rick Doblin, Ph.D., founder and executive director of the Multidisciplinary Association for Psychedelic Studies (MAPS), are expected to be published in Nature Medicine on Monday and FDA approval could come by 2023, according to a New York Times report.
A recent Imperial College London study of psilocybin use in depression reported in The New England Journal of Medicine also produced positive results. Before the end of the year, clinical results also are expected from a study involving Compass Pathways — which IPO’d late last year — using its approach of guided psilocybin experiences as a treatment for drug-resistant depression.
“People still believe that ‘your brain on drugs’ commercial is the truth rather than all scientific evidence on major therapeutic benefits,” said Simon, who heads the Psychedelic Medicines for Mental Health Group at entrepreneurial network YPO and also serves on an advisory council at Mass General Hospital on the topic. (Dr. Sharmin Ghaznavi, Mass General Hospital Assoc. Director, Center for the Neuroscience of Psychedelics, will speak at the CNBC Healthy Returns Summit on Tuesday, May 11.)
A focus on depression treatment outcomes
There are example of stigmatized drugs in FDA-approved medical usage, ketamine, for example, as an anesthesia since the 1970s, and ultimately, used on an “off-label” basis to treat depression based on the existing FDA authorization. In 2019, a Johnson & Johnson ketamine-derived treatment for drug-resistant depression was the first new approach for the mental health condition specifically approved by the FDA in decades.
The current treatment approach of helping people to live with depression and PTSD, and on medication, creates a patient population and cost factor that is a burden on the health-care system. That may ultimately help the new drug companies gain acceptance if the clinical trials results continue to be positive.
A close friend of Simon’s almost lost a child suffering from mental illness. The individual was looking at a prognosis of never going back to school, never being able to work, at best not being a danger to themselves with medication. “That was not a prognosis you want for a 20-year-old,” he said. “They had tried everything, and eventually out of complete desperation, they started learning about the potential for psychedelic-assisted therapies, and it worked,” he told CNBC in an interview conducted late last year.
Now, he says, that person is off medication, in a relationship and leading a normal professional life.
Mental illness is among the most costly medical expenses in the U.S., and it has a high cost to employers in lost productivity. In 2019, 51.5 million adults were living with a mental illness in the U.S., and the number of people suffering and drug costs, already in the tens of billions of dollars annually, are projected to grow in the years ahead, with Covid-19 compounding mental health issues globally.
Roughly 7% of Americans suffer depressive episodes annually, and roughly 1% are resistant to treatment, the latter associated with a significantly higher economic burden including hospitalization. Americans who suffer depressive episodes have additional bouts within 2-5 years at a rate exceeding 40%, according to a recent Cowen & Company research report on Compass Pathways, and that risk increases with each new depressive episode.
“Covid has done a lot of terrible things, but it has elevated mental health visibility, and as a result of that there is lots of interest,” Simon said.
Public vs. professional acceptance of illegal drugs
Denver became the first city in the U.S. to decriminalize psychedelic mushrooms in 2019, and in a 2020 ballot measure, voters in Oregon made it the first state to decriminalize mushrooms and legalize them for treatment purposes. But investors behind the new drug treatment approaches are not focused on public acceptance, the trend of microdosing (for which they say data remains slim) or consumer recreational market potential, though many do find ideas about these drugs to be outdated.
“Consciousness is not the key here,” Simon said. “For purely medical use, there is a tremendous amount of data and traction for expanding use, which is where I’m focused.”
One of the biggest investors in the emerging field is Atai Life Sciences, a holding company for multiple biotech start-ups pursuing alternative treatments for depression, anxiety and addiction based on stigmatized drugs, and backed by venture capitalist Peter Thiel. It recently filed for an IPO.
Atai’s chairman Christian Angermayer — who says he has never touched a beer even though he comes from Bavaria where it is “our daily nutrition,” or smoked a joint or cigarette — is a personal believer in the power of psychedelics to have a positive influence on life. He described his first experience with psychedelics as “the single most meaningful thing” in his life.
“Nothing else even comes close,” Angermayer told CNBC in an interview conducted late last year.
But his personal experience is distinct from his role as an investor and executive focused on the mental health market needs. Angermayer was an early investor in Compass Pathways, where one of the founders, Lars Christian Wilde, suffered from drug-resistant depression and found help in psychedelics.
“We want to bring it back to the legal realm, but in the shamanistic setting of today, and that is with a therapist. We want to make it legal, but solely for doctors or psychotherapists in a clinical setting,” said Angermayer, who will speak at CNBC Healthy Returns on Tuesday. “These are not drugs you can take alone and not everyone can afford to go to the Amazon and see a shaman. We need to bring it into the medical system.”
Investment risks
A common thread among those closely watching, and investing in this space, is the personal experience with family and friends suffering from mental illness and struggling to find a successful medical treatment. “These people have been suffering for decades,” said Piros, who has a family member now struggling with depression and who has not yet found an effective medical therapy.
The new companies come with a high level of investment risk, common in the biotech space, with early trials showing promise but the business generating no revenue today. Advocates and investors in these alternative drug treatments say the economic argument is compelling when compared to current options.
Piros, who has spent more than two decades analyzing biotech companies, says investors need to be mindful that when you get involved with a development stage company it is not about the money being made already, but factors including how long the companies will have IP protection, when they can be expected to enter the market, and potential cash flows over a period between a decade to 15 years.
I’m not a medical professional or a researcher, but as a CEO and entrepreneur, I’m someone who is used to making things happen.
Dick Simon, heads the Psychedelic Medicines for Mental Health Group at entrepreneurial network YPO
Unlike biotechs working with brand new compounds which have a failure rate as high as 90%, the trials using psychedelic drugs that have been studied for decades are less likely to result in outright failures. Still, Piros said that the proper way to think about this new theme is as part of an existing investment risk tolerance for the biotech sector, and these new drugs should be no more than 10% of that existing allocation.
“It’s not chronic medicine, which as a business model is reasonably predictable and a great business model. It remains to be seen how this business model works, but … if we only need treatment for depression twice a year to be in remission that is a thousand times better than anything we can offer today, and PTSD has no approved drug,” Piros said. “It’s not like a crapshoot anymore.”
If a company like Compass makes it to market, its treatment approach could reach millions of Americans — estimates range from roughly 2 million to 4 million — not being served well by the current class of depression drugs. Pricing of the treatment could be $10,000, according to Cowen estimates, or as high as a $20,000, according to Piros, which he said is closer to the cost of current treatments. Depending on the number of patients who are resistant to current drugs that the therapy reaches, a 5%-7% market share could be worth billions. According to a Cowen estimate, $1 billion in annual sales; according to Berenberg Capital Markets, more than $2.5 billion; and according to Piros, possibly as much as $5 billion for a new, successful entrant at peak.
“We don’t expect 5% penetration two years after launch, more like five to seven years after launch, and going beyond 5% is crazy. But that is still a very large chunk of value,” Piros said. “We don’t need to go to the consumer angle.”
Many factors would influence the overall size of the market, from patients who are designated as good candidates for the new treatments, to the number of treatments needed, the infrastructure required for the guided sessions, which need to be in controlled environments like existing treatment centers that currently administer ketamine, and physician acceptance. Compass is creating 100 centers to train medical professionals and offer guided therapy, and plans to grow to 3,800 centers in a peak year.
Medical resistance
Getting the medical establishment to embrace these treatments may be among the most difficult parts of the journey. Piros said he has discussed alternative treatments with psychiatrists on behalf of his family, but they told him they would not be interested until there are decades of placebo-controlled trial data behind the drugs. “These were young doctors, fully up to date on the latest trials and literature. It’s going to be a long road before full acceptance.”
Cowen expects the existing anti-depression drugs in the SSRI (selective serotonin reuptake inhibitor) class, which account for upwards of 75% of prescriptions, to remain the first line of choice in therapy, but its analysts also wrote in a recent report that surveying and interviews it has conducted with doctors indicate roughly 30% of patients are resistant to these drugs and as many as 1 in 4 patients might be considered for new treatment alternatives.
The executives in the field know the history, and even with seven decades of research into use of psychedelics culminating in the latest, more rigorous work, they expect continued resistance. But they are determined, and now with a growing body of clinical trial data to back up psychedelics.
“There are those who have been out there in the wilderness metaphorically, major institutions carrying on research over the last decade. How do I help them get past the stigma society still has around this work?” Simon asked. “How do you get veterans groups who don’t like the fact that 22 veterans a day commit suicide, and each year more die in suicide than in all wars since 9/11, how do you engage them, across the political spectrum? I’m not a medical professional or researcher, but as a CEO and entrepreneur, I’m someone who is used to making things happen.”
After his initial psychedelic trip, Angermayer said the first thought he had was that he needed to call his parents and tell them how much he loved them. The second thought: “This must be legal as a treatment. … We’re several years away. It’s not tomorrow, but it’s not in ten years,” he said.
If you are having thoughts of suicide, call the National Suicide Prevention Lifeline at 1-800-273-8255 (TALK) or go to SpeakingOfSuicide.com/resources for a list of additional resources.
For more exclusive insights from our reporters and speakers, sign up for our Healthy Returns newsletter to get the latest delivered straight to your inbox weekly. For a front row seat at CNBC Events, you can hear directly from the visionary executives, innovators, leaders and influencers taking the stage in “The Keynote Podcast.” Listen now, however you get your podcasts.