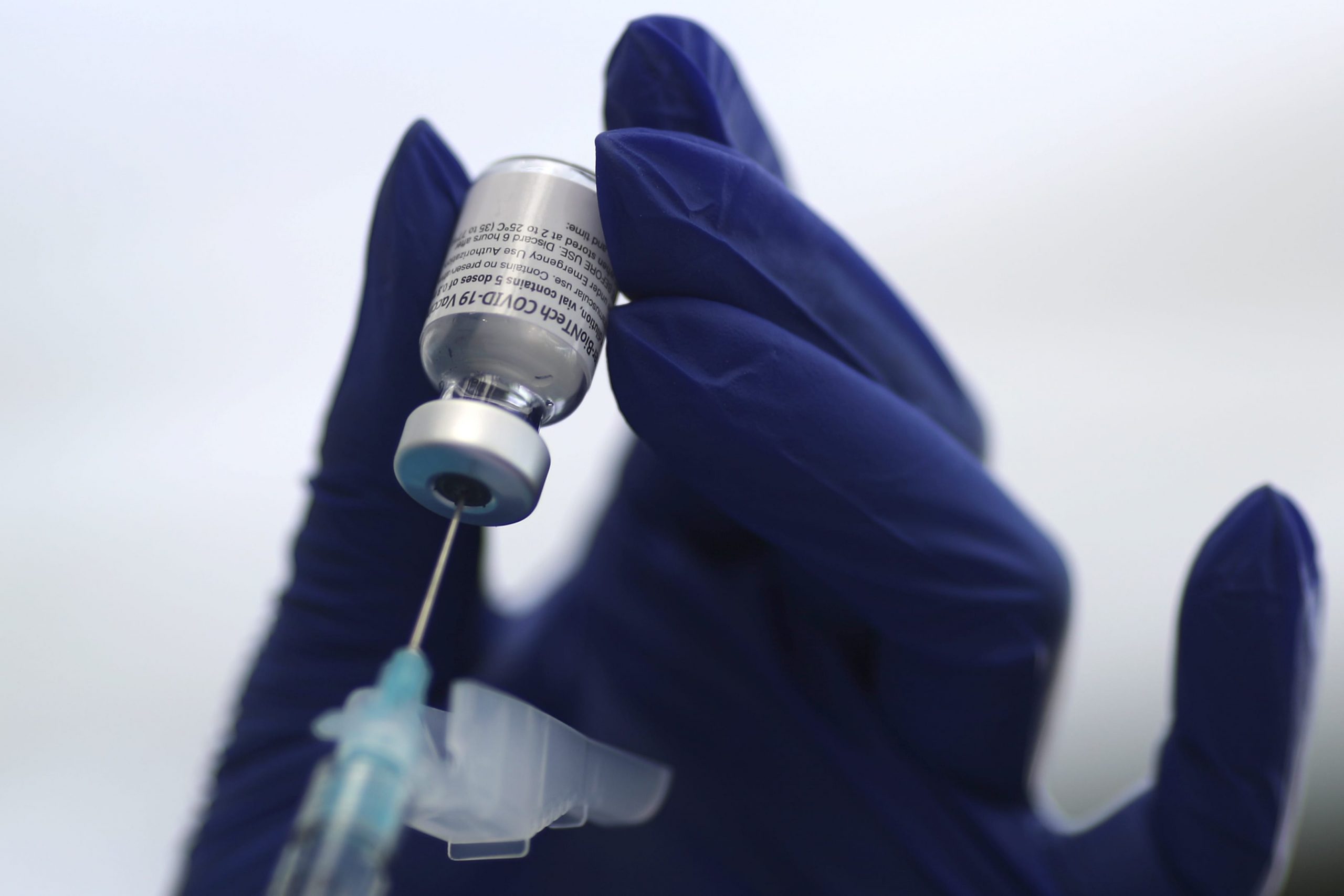
Just weeks into the country’s coronavirus vaccination effort, states have begun broadening access to the shots faster than planned, amid tremendous public demand and intense criticism about the pace of the rollout.
Some public health officials worry that doing so could bring even more chaos to the complex operation and increase the likelihood that some of the highest-risk Americans will be skipped over. But the debate over how soon to expand eligibility is intensifying as deaths from the virus continue to surge, hospitals are overwhelmed with critically ill patients and millions of vaccine doses delivered last month remain in freezers.
Governors are under enormous pressure from their constituents — especially older people, who vote in great numbers and face the highest risk of dying from the virus — to get the doses they receive into arms swiftly. President-elect Joseph R. Biden Jr.’s decision, announced Friday, to release nearly all available doses to the states when he takes office on Jan. 20, rather than holding half to guarantee each recipient gets a booster shot a few weeks after the first, is likely to add to that pressure.
Some states, including Florida, Louisiana and Texas, have already expanded who is eligible to get a vaccine now, even though many people in the first priority group recommended by the Centers for Disease Control and Prevention — the nation’s 21 million health care workers and three million residents of nursing homes and other long-term care facilities — have not yet received a shot.
On Friday afternoon, New York became the latest state to do so, announcing that it would allow people 75 and over and certain essential workers to start receiving a vaccine on Monday.
But reaching a wider swath of the population requires much more money than states have received for the task, many health officials say, and more time to fine-tune systems for moving surplus vaccine around quickly, to increase the number of vaccination sites and people who give the shots, and to establish reliable appointment systems to prevent endless lines and waits.
Some states’ expansions have led to frantic and often futile efforts by older people to get vaccinated. After Florida opened up vaccinations to anyone 65 and older late last month, the demand was so great that new online registration portals quickly overloaded and crashed, people spent hours on the phone trying to secure appointments and others waited overnight at scattered pop-up sites offering shots on a first-come first-served basis.
Similar scenes have played out in parts of Texas, Tennessee and a handful of other states.
Still, with C.D.C. data suggesting that only about a third of the doses distributed so far have been used, Alex M. Azar II, the health and human services secretary, told reporters this past week: “It would be much better to move quickly and end up vaccinating some lower-priority people than to let vaccines sit around while states try to micromanage this process. Faster administration would save lives right now, which means we cannot let the perfect be the enemy of the good.”
The C.D.C. guidelines were drawn up by an independent committee of medical and public health experts that advises the agency on immunization practices; it deliberated for months about who should get vaccinated initially, while supplies were still very limited. The committee weighed scientific evidence about who is most at risk of getting very sick or dying from Covid-19, as well as ethical questions, such as how best to ensure equal access among different races and socioeconomic groups.
Although the committee’s recommendations are nonbinding, states usually follow them; in this case, the committee suggests that states might consider expanding to additional priority groups “when demand in the current phase appears to have been met,” “when supply of authorized vaccine increases substantially” or “when vaccine supply within a certain location is in danger of going unused.”
Dr. Kevin Ault, an obstetrician at the University of Kansas Medical Center who serves on the advisory committee that came up with the C.D.C. guidelines, said that it was reasonable for states to start vaccinating new groups before finishing others, but that they should be careful about exacerbating inequities and biting off more than they can chew.
“Obviously if you’re going to vaccinate that group you need to have a well-thought-out plan in hand,” he said, referring to the over-65 population. “Having people camping out for vaccine is less than ideal, I would say.”
He added, “We put a lot of thought and effort into our guidelines, and I think they are good.”
After the first vaccines were given in mid-December, a dichotomy emerged between governors who were adhering precisely to the guidelines and others who moved quickly to populations beyond health care workers and nursing home residents.
Until Friday, Gov. Andrew M. Cuomo of New York, a Democrat, had threatened to penalize hospitals that provided shots to people who are not health care workers. By contrast, Gov. Ron DeSantis of Florida, a Republican, traveled to retirement communities around his state to emphasize the importance of getting people 65 and older, who number more than five million there, immunized fast.
“In Florida we’ve got to put our parents and grandparents first,” Mr. DeSantis said at The Villages, the nation’s largest retirement community, just before Christmas.
Decisions on how soon to expand eligibility for the shots have not fallen neatly along partisan lines.
Covid-19 Vaccines ›
Answers to Your Vaccine Questions
If I live in the U.S., when can I get the vaccine?
While the exact order of vaccine recipients may vary by state, most will likely put medical workers and residents of long-term care facilities first. If you want to understand how this decision is getting made, this article will help.
When can I return to normal life after being vaccinated?
Life will return to normal only when society as a whole gains enough protection against the coronavirus. Once countries authorize a vaccine, they’ll only be able to vaccinate a few percent of their citizens at most in the first couple months. The unvaccinated majority will still remain vulnerable to getting infected. A growing number of coronavirus vaccines are showing robust protection against becoming sick. But it’s also possible for people to spread the virus without even knowing they’re infected because they experience only mild symptoms or none at all. Scientists don’t yet know if the vaccines also block the transmission of the coronavirus. So for the time being, even vaccinated people will need to wear masks, avoid indoor crowds, and so on. Once enough people get vaccinated, it will become very difficult for the coronavirus to find vulnerable people to infect. Depending on how quickly we as a society achieve that goal, life might start approaching something like normal by the fall 2021.
If I’ve been vaccinated, do I still need to wear a mask?
Yes, but not forever. The two vaccines that will potentially get authorized this month clearly protect people from getting sick with Covid-19. But the clinical trials that delivered these results were not designed to determine whether vaccinated people could still spread the coronavirus without developing symptoms. That remains a possibility. We know that people who are naturally infected by the coronavirus can spread it while they’re not experiencing any cough or other symptoms. Researchers will be intensely studying this question as the vaccines roll out. In the meantime, even vaccinated people will need to think of themselves as possible spreaders.
Will it hurt? What are the side effects?
The Pfizer and BioNTech vaccine is delivered as a shot in the arm, like other typical vaccines. The injection won’t be any different from ones you’ve gotten before. Tens of thousands of people have already received the vaccines, and none of them have reported any serious health problems. But some of them have felt short-lived discomfort, including aches and flu-like symptoms that typically last a day. It’s possible that people may need to plan to take a day off work or school after the second shot. While these experiences aren’t pleasant, they are a good sign: they are the result of your own immune system encountering the vaccine and mounting a potent response that will provide long-lasting immunity.
Will mRNA vaccines change my genes?
No. The vaccines from Moderna and Pfizer use a genetic molecule to prime the immune system. That molecule, known as mRNA, is eventually destroyed by the body. The mRNA is packaged in an oily bubble that can fuse to a cell, allowing the molecule to slip in. The cell uses the mRNA to make proteins from the coronavirus, which can stimulate the immune system. At any moment, each of our cells may contain hundreds of thousands of mRNA molecules, which they produce in order to make proteins of their own. Once those proteins are made, our cells then shred the mRNA with special enzymes. The mRNA molecules our cells make can only survive a matter of minutes. The mRNA in vaccines is engineered to withstand the cell’s enzymes a bit longer, so that the cells can make extra virus proteins and prompt a stronger immune response. But the mRNA can only last for a few days at most before they are destroyed.
Gov. Larry Hogan of Maryland, a Republican, announced Tuesday that he would immediately switch to what he called the “Southwest Airlines model” for vaccine allocation, referring to the airline’s open seating policy. “We’re no longer going to be waiting for all the members of a particular priority group to be completed,” he said, “before we move on to begin the next group in line.”
Gov. Mike DeWine of Ohio, a Republican, urged patience in a news briefing Tuesday as he declined to estimate when the state would start vaccinating people beyond the first priority group, known as “1a.”
“We’re asking every health department, ‘Don’t go outside 1a, stay within your lane,’” he said, adding about the vaccines, “This is a scarce commodity.”
By Thursday Mr. DeWine had set a date for people 80 and older to start getting the vaccine — Jan. 19 — and said he would phase in everyone 65 and older, as well as teachers, by Feb. 8.
The reasons so many doses received by states have not yet been administered to the first priority group are manifold. The fact that vaccination began around Christmas, when many hospital employees were taking vacation, slowed things. More health care workers are refusing to get the vaccine than many of their employers expected, and some hospitals and clinics received more doses than they needed but felt constrained by state rules from giving them to people outside the first priority groups. Some initially worried they could not even offer leftover doses in open vials to people in lower priority groups and let them go to waste.
And federal funding for vaccination efforts has been slow to reach states and localities: They got only $350 million through the end of last year, a little more than $1 per resident of the country. The economic rescue package that Congress passed in December included $8 billion for vaccine distribution that state health officials had long sought, but the first tranche of it, about $3 billion, is only now starting to be sent out.
“There was great funding in the development of these products, great funding in the infrastructure to ship them and get them out,” said Dr. Steven Stack, commissioner of the Kentucky Department for Public Health. “But then there was no funding provided of meaning for administering the vaccine, which is the last mile of this journey.”
The C.D.C. has recommended that a “1b” group consisting of people 75 and older and certain essential workers, including teachers, corrections officers and grocery store employees, be vaccinated next. The second group is much larger, about 50 million people. And the third recommended priority group — people 65 to 74, anyone 16 and older with high-risk medical conditions, and essential workers not already reached — numbers almost 130 million.
Pfizer and Moderna have pledged to deliver enough vaccine doses for 100 million people to each get the two necessary shots by the end of March, and many more in the second quarter. Several other vaccine candidates are far along in the pipeline, and if approved for emergency use here could help ramp up distribution more quickly.
The C.D.C. committee initially considered recommending that a wide range of essential workers get vaccinated before older Americans. Its rationale was that many essential workers are low-wage people of color, who have been hit disproportionately hard by the virus and had limited access to good health care. That sparked a backlash, and several governors, including Mr. DeSantis, quickly made clear they would cater to older people first.
Dr. Mark McClellan, who formerly headed the F.D.A. and now runs Duke University’s health policy center, said that while pushing ahead to vaccinate older people and other particularly vulnerable groups would accelerate the overall effort, “we’re going to be missing a lot of higher-risk individuals along the way.”
“I do worry about that becoming uneven in terms of access,” he said during a press briefing, “with lower-income groups, minority groups maybe in a tougher position if we don’t make it very easy for people in these high-risk groups to get vaccinated.”
Dr. Marcus Plescia, the chief medical officer for the Association of State and Territorial Health Officials, said he was surprised to hear federal officials like Mr. Azar and Dr. Jerome Adams, the surgeon general, advocate expanding vaccine access so broadly so soon.
“We didn’t come up with priority populations to slow things down, but because we knew there would be limited numbers of doses,” Dr. Plescia said. “If we try to do this in an equitable, fair way, it’s not going to be as fast as if our only goal is to get vaccine into as many arms as possible.”
Whether or not they are widening access now, governors are ramping up pressure on hospitals to use their allocated doses more quickly. Mr. Cuomo threatened to fine those that did not use their initial allocations by the end of this past week and not send them any more.
Mr. Hogan warned hospitals this past week, “Either use the doses that have been allocated to you or they will be directed to another facility or provider.”