MIAMI — Linda Kleindienst Bruns registered for a coronavirus vaccine in late December, on the first day the health department in Tallahassee, Fla., opened for applications for people her age. Despite being 72, with her immune system suppressed by medication that keeps her breast cancer in remission, she spent days waiting to hear back about an appointment.
“It’s so disorganized,” she said. “I was hoping the system would be set up so there would be some sort of logic to it.”
Phyllis Humphreys, 76, waited with her husband last week in a line of cars in Clermont, west of Orlando, that spilled onto Highway 27. They had scrambled into their car and driven 22 miles after receiving an automated text message saying vaccine doses were available. But by 9:43 a.m., the site had reached capacity and the Humphreys went home with no shots.
“We’re talking about vaccinations,” said Ms. Humphreys, a retired critical care nurse. “We are not talking about putting people in Desert Storm.”
Florida is in an alarming new upward spiral, with nearly 20,000 cases of the virus reported on Friday and more than 15,000 on Saturday. But the state’s well-intended effort to throw open the doors of the vaccine program to everyone 65 and older has led to long lines, confusion and disappointment.
States across the country, even as they race to finish vaccinating health care employees, nursing home residents and emergency workers, are under pressure from residents to reach a broader section of the public. Florida, which has already prioritized a large swath of its population to receive the vaccine, illustrates the challenges of expanding a vaccination program being developed at record speed and with limited federal assistance.
“How do you do something this huge and roll it out?” said Dr. Leslie M. Beitsch, the chairman of the behavioral sciences and social medicine department at Florida State University. “It’s not in any way surprising — to anyone who followed it closely, for sure — that there would be halting kind of progress and missteps getting something of this magnitude underway initially, whether we’re talking about Florida or the entire country.”
Guidelines from the Centers for Disease Control and Prevention recommend giving the next priority after the earliest groups to essential workers and people 75 and older. Some states, including Florida, Texas, Oklahoma and Hawaii, decided to vaccinate people 65 and older, even before essential workers, and other states are following suit.
But with states and counties left to largely sort out logistics by themselves, the rollout has gone anything but smoothly.
People camped out overnight in the Florida winter chill in Fort Myers and Daytona Beach for vaccines administered on a first-come-first-served basis, a spectacle that made national headlines. Health department offices in Sarasota and several other counties, unequipped to schedule vaccine appointments on their own websites, resorted to using Eventbrite, a service usually associated with invitations to dinner parties and art exhibitions.
Palm Beach County was accepting vaccine requests only by email, said the county’s health administrator, Dr. Alina Alonso, after the county’s phone system “absolutely died.” People in the queue were warned that they might have to wait months for an appointment. In the meantime, some wealthy people with connections to health care facilities have been able to get the vaccine more easily.
Adding to the complications, the Florida Division of Emergency Management announced on Sunday that its coronavirus testing and vaccination site at Hard Rock Stadium in Miami Gardens — the recent scene of long lines of people awaiting vaccination — would be shut down for much of Monday to make way for the College Football Playoff national championship game.
Experts say Florida is an example of what happens when officials attempt to distribute a vaccine that is still in very limited supply to a broad spectrum of the population. In a state with about 4.4 million people 65 and older, more than 402,000 doses had been administered as of Friday, according to federal data, the fourth-highest total in the nation. But Florida has used only about 30 percent of the vaccine doses it has received, behind 29 other states.
Some people have been successful, including Janice and Walter Greer, who were in the same line as the Humphreys in Clermont on Wednesday. Ms. Greer had called Lake County repeatedly, hoping to get information about vaccine availability.
Mr. Greer has a brother in Ohio with Covid-19. “I couldn’t go and see him,” he said softly, welling up with tears. “He has pneumonia.”
But while the Greers got in line early enough to receive shots, many more people left without one and were quite upset.
“My heart is beating 100 miles a minute,” said Shirley LaBoy, 65, of Polk County, who got to the recreation center only to see a line of cars and a digital road sign saying “NO VACCINES TODAY.”
Covid-19 Vaccines ›
Answers to Your Vaccine Questions
If I live in the U.S., when can I get the vaccine?
While the exact order of vaccine recipients may vary by state, most will likely put medical workers and residents of long-term care facilities first. If you want to understand how this decision is getting made, this article will help.
When can I return to normal life after being vaccinated?
Life will return to normal only when society as a whole gains enough protection against the coronavirus. Once countries authorize a vaccine, they’ll only be able to vaccinate a few percent of their citizens at most in the first couple months. The unvaccinated majority will still remain vulnerable to getting infected. A growing number of coronavirus vaccines are showing robust protection against becoming sick. But it’s also possible for people to spread the virus without even knowing they’re infected because they experience only mild symptoms or none at all. Scientists don’t yet know if the vaccines also block the transmission of the coronavirus. So for the time being, even vaccinated people will need to wear masks, avoid indoor crowds, and so on. Once enough people get vaccinated, it will become very difficult for the coronavirus to find vulnerable people to infect. Depending on how quickly we as a society achieve that goal, life might start approaching something like normal by the fall 2021.
If I’ve been vaccinated, do I still need to wear a mask?
Yes, but not forever. The two vaccines that will potentially get authorized this month clearly protect people from getting sick with Covid-19. But the clinical trials that delivered these results were not designed to determine whether vaccinated people could still spread the coronavirus without developing symptoms. That remains a possibility. We know that people who are naturally infected by the coronavirus can spread it while they’re not experiencing any cough or other symptoms. Researchers will be intensely studying this question as the vaccines roll out. In the meantime, even vaccinated people will need to think of themselves as possible spreaders.
Will it hurt? What are the side effects?
The Pfizer and BioNTech vaccine is delivered as a shot in the arm, like other typical vaccines. The injection won’t be any different from ones you’ve gotten before. Tens of thousands of people have already received the vaccines, and none of them have reported any serious health problems. But some of them have felt short-lived discomfort, including aches and flu-like symptoms that typically last a day. It’s possible that people may need to plan to take a day off work or school after the second shot. While these experiences aren’t pleasant, they are a good sign: they are the result of your own immune system encountering the vaccine and mounting a potent response that will provide long-lasting immunity.
Will mRNA vaccines change my genes?
No. The vaccines from Moderna and Pfizer use a genetic molecule to prime the immune system. That molecule, known as mRNA, is eventually destroyed by the body. The mRNA is packaged in an oily bubble that can fuse to a cell, allowing the molecule to slip in. The cell uses the mRNA to make proteins from the coronavirus, which can stimulate the immune system. At any moment, each of our cells may contain hundreds of thousands of mRNA molecules, which they produce in order to make proteins of their own. Once those proteins are made, our cells then shred the mRNA with special enzymes. The mRNA molecules our cells make can only survive a matter of minutes. The mRNA in vaccines is engineered to withstand the cell’s enzymes a bit longer, so that the cells can make extra virus proteins and prompt a stronger immune response. But the mRNA can only last for a few days at most before they are destroyed.
“I found myself on the computer all day. I feel, emotionally, all stressed out,” said Ms. LaBoy, who has been unable to see her children for fear of contracting the virus. “We are tired of being locked in. Then I get an opportunity to get the vaccine, and I can’t even get that.”
Aaron Kissler, the health administrator for Lake County, said officials wanted to get shots in arms quickly, even without a more organized appointment system available. “Right now, we just wanted to get out as much as possible,” he said.
In Texas, about 527,000 residents had received at least the first vaccine dose as of Friday, according to the Texas Department of State Health Services. About 107,000 of them were 65 or older, out of more than 3.7 million Texans eligible in that age range. But there have been problems similar to Florida’s.
Dr. Bob Kelly, a 77-year-old retired veterinarian in Austin, said he made 20 or more phone calls searching for a vaccine before he finally connected one night at 3 a.m. on a hospital internet link that offered an appointment for several days later.
He and his wife drove 25 miles to the appointment, only to be told that supplies were so limited that the vaccine would only be given to people with aggravating health conditions. So they are back to where they started, with their names on five waiting lists at pharmacies, chain hospitals and a doctor’s office.
“That’s what’s going on,” Dr. Kelly said. “The rollout is slow, the method of administration is not efficient and who gets it is kind of arbitrary.”
In Florida, Gov. Ron DeSantis, a Republican, has acknowledged that the initial rollout has been bumpy.
But he has steadfastly defended the state’s decision to open the door to all seniors, saying he could not in good conscience see a 20-something who bags groceries getting vaccinated before a grandparent, not in a state where of the more than 22,000 people killed by the coronavirus, 83 percent have been 65 or older.
The plurality of vaccine doses have gone so far to people between the ages of 65 and 74, not to people 75 and older who are the most vulnerable to the virus.
Some of the lag in numbers may be a result of older people who are being extra cautious about getting a new vaccine developed in record time. But older seniors may also be at a disadvantage because the process has often required a degree of computer proficiency and has generally not been clear or consistent, Dr. Beitsch said.
“Each of our 67 counties seems to be taking a slightly different pathway — and that’s remarkable, because we have a single department of health that is supposed to cover the entire state,” said Dr. Beitsch, whose 71-year-old tech-savvy brother got vaccinated in Orlando after filling out a request form that took him about 40 minutes.
The Florida Department of Health is working on an online appointment system for all counties, but it is not yet ready, though the DeSantis administration says it has been preparing for the vaccine rollout since July. It stockpiled millions of supplies and enrolled more than 270 providers to receive the shots once they became available.
Mr. DeSantis said his administration moved more aggressively than other states, getting teams of health workers and National Guard members to nursing homes the week before CVS and Walgreens pharmacies began vaccinating those residents. Florida is also distributing doses to Publix supermarkets and churches to increase community access.
“We’re going to be there for our parents,” he said in a news conference on Sunday. “We’re going to be there for our grandparents. And that will do more than anything else we can do to reduce mortality and change the scope of how this virus behaves in the state of Florida.”
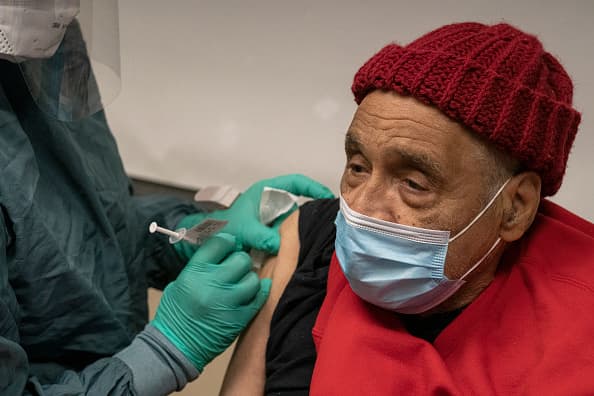
The lucky vaccine recipients have been thrilled.
“Everything was great,” Susan Hacker said after getting her shot on Thursday at the Century Village retirement community in Boca Raton.
The state has no residency requirement for people to get the vaccine in their home county — or to be Florida residents at all. News reports in Argentina have recounted how wealthy people vacationing in Miami managed to get vaccinations.
More worrying to officials have been private institutions distributing the vaccine to people who are not in any of the priority groups. MorseLife Health System, a nursing home and assisted living facility in West Palm Beach, is under investigation by the Florida inspector general and the health department after The New York Post and The Washington Post reported that it steered vaccines to rich donors.
In an interview on Tuesday, Hong Chae, the organization’s chief financial officer, said that a number of the nursing home’s board members and volunteers were offered the vaccine in case facility managers became incapacitated by the virus and board members needed “to come in and chip in,” he said.
Some hospitals in Miami have vaccinated board members as well, according to local doctors and patients.
One of them, Rosario Rico Toro, posted news of receiving the Pfizer vaccine to Facebook friends on Dec. 30. “Baptist vaccination day!!” she wrote alongside an image of her Covid-19 vaccination record.
In an interview, Ms. Rico Toro, a onetime Miss Bolivia who now does charitable work for hospitals, said she had received the vaccine as a result of her donations and volunteer work for Baptist Hospital in Miami. When one of the hospital’s doctors canceled an appointment to get the shot, the hospital offered her the spot.
“They called and said, ‘As a board member, would you like to get it?’” she recalled.
The hospital did not respond to requests for comment.
Ms. Rico Toro, who is 49 and in good health, said she initially hesitated. But the hospital gave her the impression that if she turned down the vaccine, it would be offered to another board member or possibly not even be used, so she took it. “My question is, why not?”
Dr. Perri Young, an internist in Miami, said that the distribution process has been shambolic and ineffective. Even as a doctor, she said, her access to information is minimal.
“It’s crazy here,” she said. “It became sort of lawless.”
By the end of week, Ms. Kleindienst Bruns in Tallahassee had gotten some good news: Her internist had received vaccine doses. Would she like one?
She got it on Saturday. “It was so easy,” she said.
Patricia Mazzei reported from Miami, Eric Adelson from Clermont, Fla., and Kate Kelly from New York. David Montgomery contributed reporting from Austin, Texas; Neil Reisner from Coconut Creek, Fla., and Boca Raton, Fla.; and Rachel Abrams from Los Angeles.