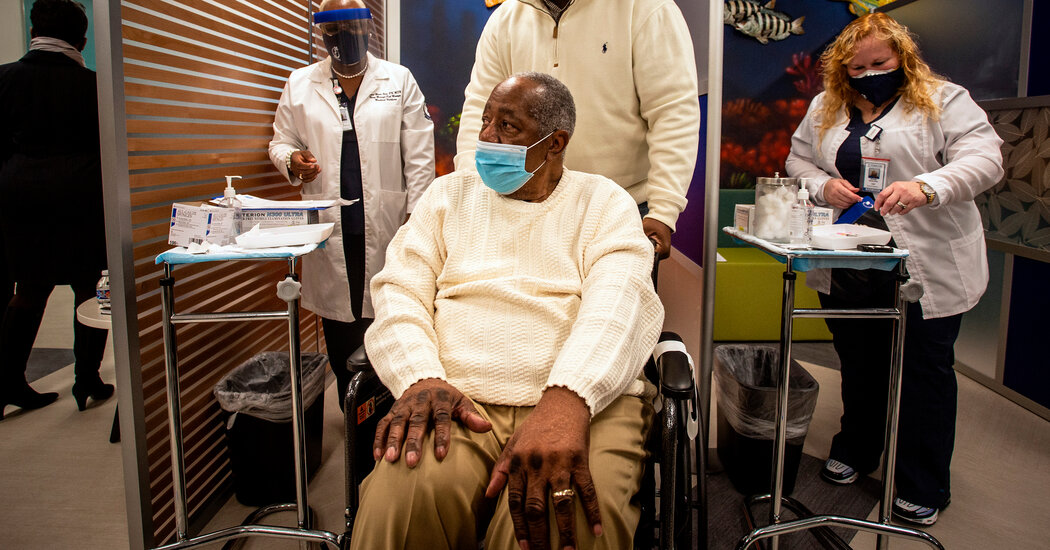At first glance, after a long wait for Johnson & Johnson’s coronavirus vaccine test, the results reported on Friday, January 29th, may have been disappointing. Its effectiveness – the ability to prevent moderate and severe illness – was 72 percent in the US, 66 percent in Latin American countries, and 57 percent in South Africa.
These numbers are well below those of Pfizer-BioNTech and Moderna, the first two emergency vaccines approved in the United States that were 94 to 95 percent effective.
Anthony Fauci, the nation’s leading infectious disease expert and now President Joe Biden’s chief medical officer on coronavirus pandemic-related issues, acknowledged the remarkable difference at a news conference on Friday, January 29.
“If you woke up and said, ‘Well, if I go to the left door I get 94 or 95 percent, if I go to the right door I get 72 percent.’ Which door would you choose? ”He asked.
However, Fauci assured that the most important indicator is the ability to prevent serious illness, which means people will not be hospitalized and deaths will be avoided. In that regard, Johnson & Johnson’s vaccine reported 85 percent in all countries it was tested in, including South Africa, where a rapidly spreading variant of the virus has shown some ability to escape vaccines.
More important than preventing “some aches and pains,” Fauci explained, is defending against serious illness, especially among people with underlying illnesses and older adults who are more likely to become seriously ill and die of COVID-19.
“If you can prevent serious illness in a high percentage of people, it will greatly alleviate the stress of human suffering and death from this pandemic that we are witnessing right now,” Fauci added. “As we all know, our healthcare system has been impacted by the number of people hospitalized and critical care over the past few weeks.”
Francis Collins, director of the National Institutes of Health, compared the ability to prevent serious illness to the effects of flu vaccines, which do not always prevent influenza completely but make it less severe.
“The same thing seems to be happening here, in a situation where this variant of the virus is clearly making it a little harder to get the strongest response you want,” Collins said. “But still he looks great with a serious illness.”
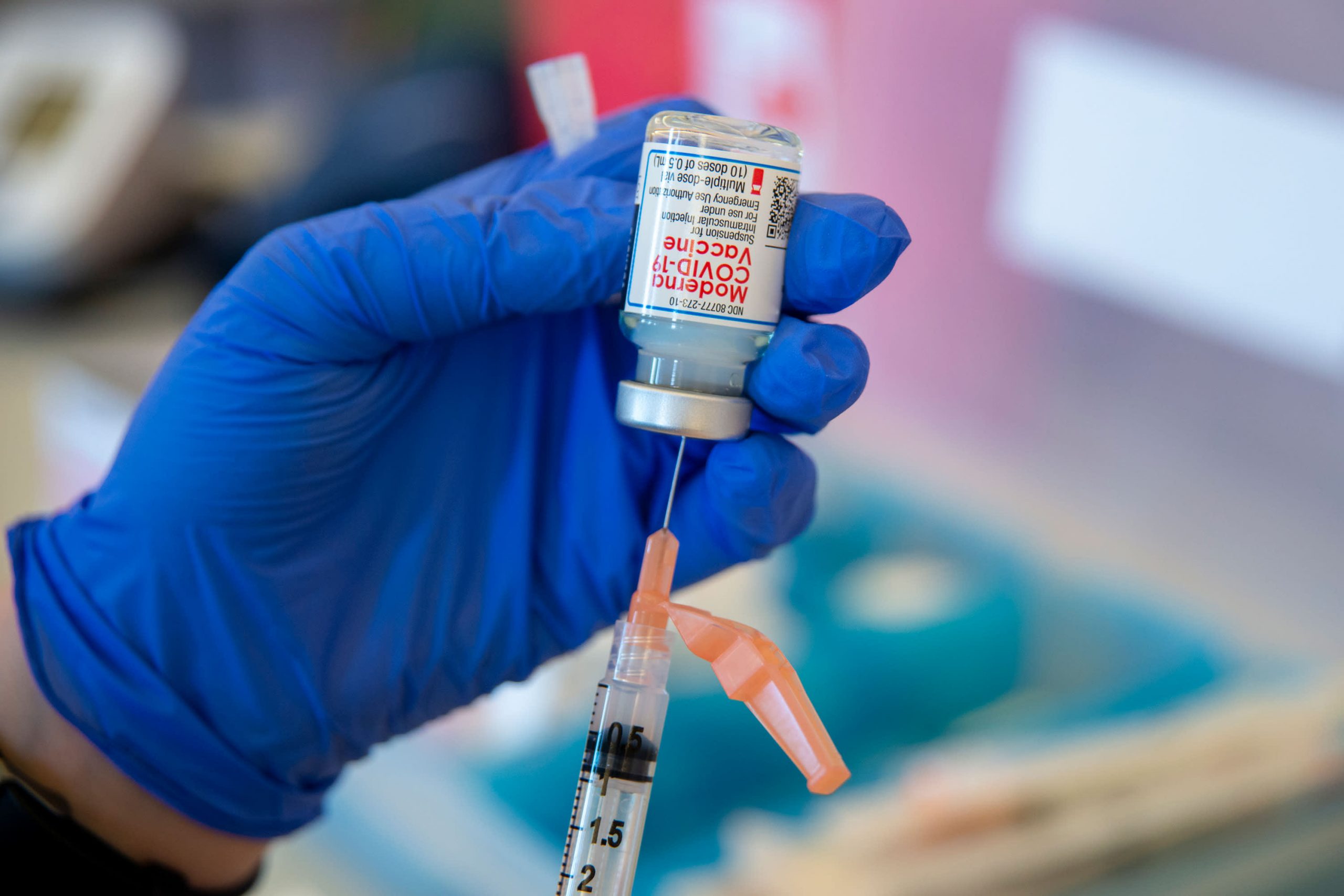
Moderna’s vaccine was also shown to be 100 percent effective against severe cases of the disease. Pfizer-BioNTech also reported similar numbers, but the total number of serious cases in the study was too few to be conclusive.
However, the researchers caution that trying to compare effectiveness between new and previous studies can be misleading because the virus is evolving quickly and tests have looked to some extent on different pathogens.
“You have to recognize that Pfizer and Moderna have an advantage,” said William Schaffner, an infectious disease expert at Vanderbilt University, in an interview. “They did their clinical studies before the strain variants became very obvious. Johnson & Johnson not only tested their vaccine against the standard strain, but they also had the variants. “
The best way to stop mutations from spreading and prevent new ones from emerging is to vaccinate as many people as possible as soon as possible, explain Fauci and other researchers. Viruses cannot mutate if they do not replicate, and they cannot replicate if they cannot enter cells. Keeping them in check with immunization can stop the process.
In addition to the Pfizer BioNTech and Moderna vaccines already used in the US, three more will be available shortly: those manufactured by Novavax, Johnson & Johnson and AstraZeneca. The use of the AstraZeneca vaccine has already been approved in the UK and other countries.
The Johnson & Johnson vaccine is expected to play an important role worldwide, but especially in low and middle income countries, as it works in one dose, is more or less cheap, and is easier to store and distribute than that Pfizer-BioNTech and Moderna vaccines because they don’t share their strict freezing and refrigeration requirements.
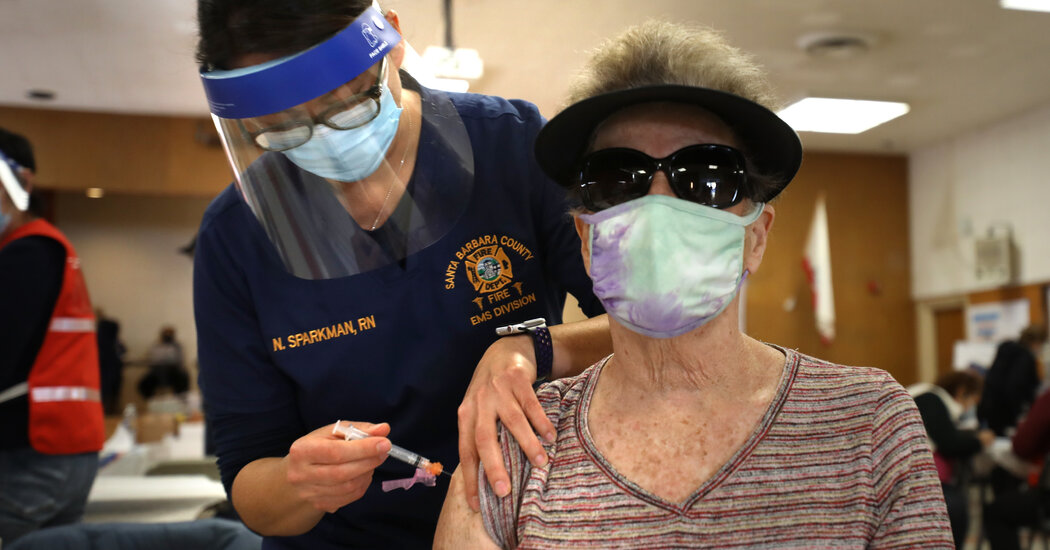
People waiting to be vaccinated may wonder if there is a choice between vaccines and if they should hold out and wait until the one that best suits them becomes available.
Paul Offit, a vaccines expert at Philadelphia Children’s Hospital, told CNN that if Pfizer BioNtech and Moderna vaccines were adequately supplied, they would be his first choice because of their overall greater effectiveness.
But right now there aren’t enough of these vaccines.
If you can’t get the Pfizer BioNTech or Moderna vaccine, you would choose the Johnson & Johnson injection, Offit said, as long as the data the company presents to the Food and Drug Administration is as good as Friday’s .
Offit said Johnson & Johnson’s report on reducing major illnesses was a huge benefit.
“This is what you are looking for,” added Offit. “You want to be away from the hospital, away from the morgue.”
The doctor noted that the company was also investigating a two-shot regimen that could make the vaccine more effective.
People who choose the Johnson & Johnson vaccine should be able to safely get a Pfizer BioNTech or Moderna vaccine later if a booster shot is needed, he added.
However, Schaffner warned that there is no data on the effects of receiving different types of vaccines. “We didn’t study that,” he said.
Schaffner said he had just attended a meeting with other public health experts and they had asked each other what they would say to their spouses or partners if they could get the Johnson & Johnson vaccine tomorrow or had to wait three weeks for Pfizer -BioNTech or Moderna.
“We all said, ‘Get it tomorrow,'” said Schaffner. “The virus is bad. You risk another three weeks of exposure instead of receiving protection tomorrow. “
He said Johnson & Johnson’s 85 percent effectiveness against the severe version of the disease was slightly less than that reported by Moderna and Pfizer-BioNTech, “but still quite high”.
Denise Grady has been a science reporter for The Times since 1998. She wrote Deadly Invaders, a book about emerging viruses. @nytDeniseGrady