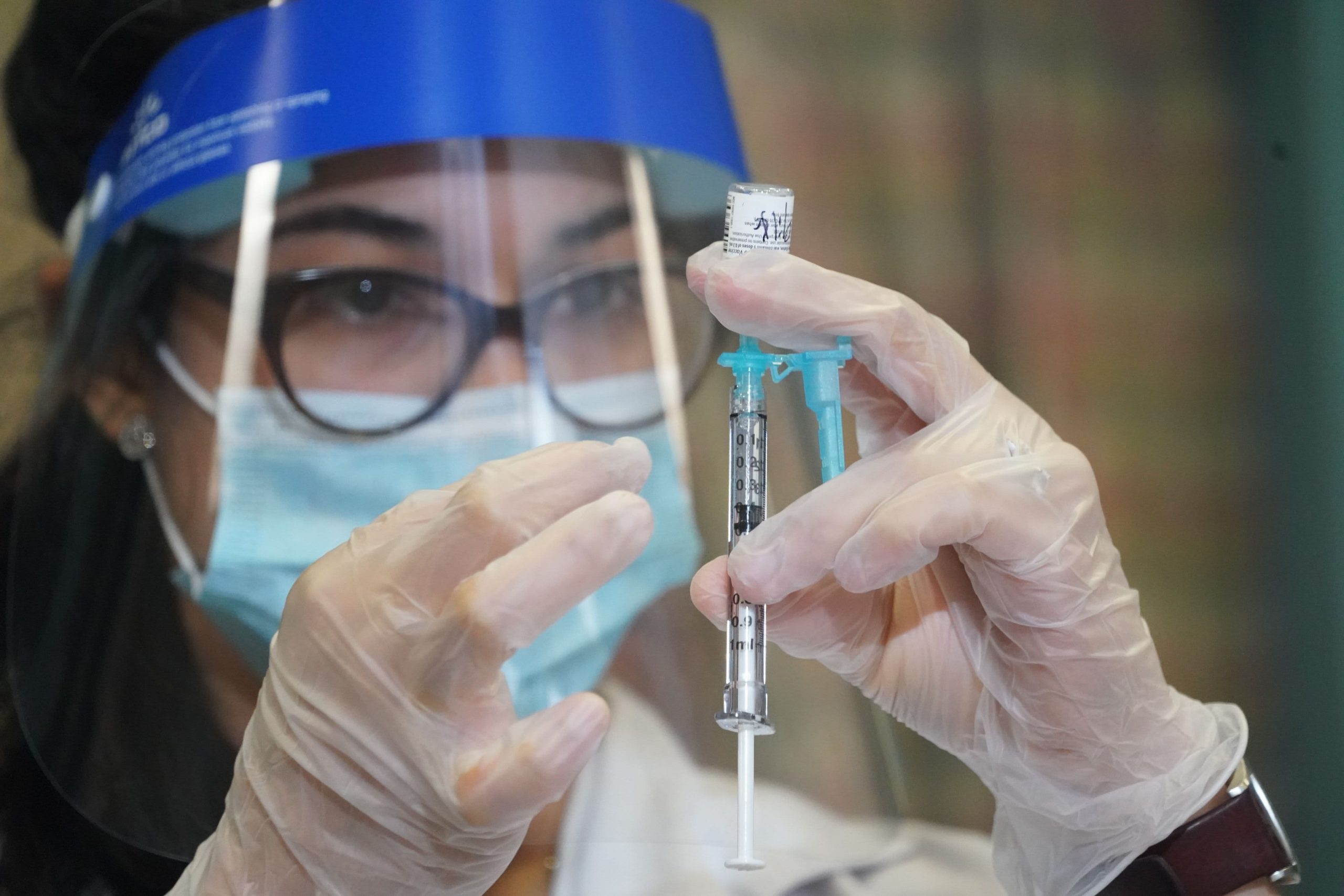
The invention of the Covid-19 vaccine will be remembered as a milestone in the history of medicine, creating in a few months what had previously taken up to a decade. Dr. However, Kayvon Modjarrad, director of the Emerging Infectious Disease Division at the Walter Reed Army Institute of Research in Silver Springs, Md., Is not satisfied.
“It’s not fast enough,” he said. More than 2.3 million people around the world have died, and many countries won’t have full access to the vaccines for a year or two: “Fast – really fast – got it on the first day there.”
There will be more coronavirus outbreaks in the future. Bats and other mammals abound in strains and species of this abundance Family of viruses. Some of these pathogens will inevitably cross the species barrier and cause new pandemics. It’s only a matter of time.
Dr. Modjarrad is one of many scientists who has been calling for a different type of vaccine for years: one that can work against all coronaviruses. These calls were largely ignored until Covid-19 showed how catastrophic coronaviruses can be.
Now researchers are starting to develop prototypes of what is known as a pancoronavirus vaccine, some of which show promise, albeit early. Results of animal experiments. Dr. Eric Topol, professor of molecular medicine at the Scripps Research Institute in San Diego, believes scientists should team up immediately on another major vaccine-making project.
“We have to find real workers to accelerate this so we can have it this year,” he said. Dr. Topol and Dennis Burton, a Scripps immunologist, called for this project on comprehensive coronavirus vaccines in Nature magazine Monday.
After coronaviruses were first identified in the 1960s, they weren’t a high priority for vaccine manufacturers. For decades, it seemed like they caused only mild colds. However, in 2002, a new coronavirus called SARS-CoV emerged, causing fatal pneumonia called SARS (Severe Acute Respiratory Syndrome). Scientists have been trying to make a vaccine for it.
Since no one had made a coronavirus vaccine for humans before, there was a lot to learn about its biology. Ultimately, the researchers chose a target for immunity: a protein on the surface of the virus called a spike. Antibodies sticking to the tip can prevent the coronavirus from entering cells and stop infection.
However, public health officials in Asia and elsewhere did not wait for the invention of a SARS vaccine to come to work. Their quarantines and other efforts have proven remarkably effective. Within a few months, they wiped out SARS-CoV with only 774 deaths.
The threat from coronavirus became even more apparent in 2012 when a second type of bat overflowed and caused another deadly respiratory disease called MERS. The researchers started working on MERS vaccines. However, some researchers wondered whether making a new vaccine for each new coronavirus – which Dr. Modjarrad called “One Bug, One Drug Approach” – the smartest strategy was. Wouldn’t it be better, they thought, if a single vaccine could work against SARS, MERS, and any other coronavirus?
That idea went nowhere for years. MERS and SARS caused relatively few deaths and were soon dwarfed by outbreaks of other viruses such as Ebola and Zika.
In 2016, Maria Elena Bottazzi, a virologist at Baylor College of Medicine, and her colleagues applied for assistance from the American government to develop a pancoronavirus vaccine, but were not given it. “They said there was no interest in pancorona,” recalled Dr. Bottazzi.
Their team even lost funding to develop a SARS vaccine after showing that it works in mice, is non-toxic to human cells, and can be manufactured on a large scale. A coronavirus that had disappeared from view just wasn’t a top priority.
Without enough money to start clinical trials, the scientists stored their SARS vaccine in a freezer and moved on to other research. “It was a fight,” said Dr. Bottazzi.
Dr. Matthew Memoli, a virologist at the National Institute for Allergies and Infectious Diseases, views these decisions as a huge mistake. “It’s a failure of our science system,” he said. “Funders tend to chase after shiny objects.”
Three years later, a third dangerous coronavirus emerged: the SARS-CoV-2 strain that causes Covid-19. Although this virus has a much lower death rate than its cousins that cause SARS and MERS, it spreads far better from person to person, resulting in and still increasing in more than 106 million documented cases around the world.
Updated
Apr. 9, 2021, 4:25 p.m. ET
All of the lessons researchers learned about coronaviruses helped them quickly manufacture new vaccines for SARS-CoV-2. Dr. Bottazzi and her colleagues used the technology they developed to make SARS vaccines to make one for Covid-19, which is currently in early clinical trials.
Other researchers used even newer methods to move faster. The German company BioNTech has developed a genetic molecule called messenger RNA that codes for the spike protein. Working with Pfizer, the companies received US government approval for their vaccine in just 11 months. The previous record for a vaccine against chickenpox was four years.
Although the Covid-19 pandemic is far from over, a number of researchers are calling for preparations for the next deadly coronavirus.
“It’s happened three times,” said Daniel Hoft, a virologist at Saint Louis University. “It will most likely happen again.”
Researchers at VBI Vaccines, a Cambridge-based company, took a small step towards a pancoronavirus vaccine last summer. They created virus-like shells that were studded with spike proteins from the three coronaviruses that caused SARS, MERS and Covid-19.
When the researchers injected this three-spike vaccine into mice, the animals made antibodies that were effective against all three coronaviruses. Interestingly, some of these antibodies could also bind to a fourth human coronavirus that causes seasonal colds – although the spike proteins from this virus were not in the vaccine. The scientists have published this data, but have not yet published it in a scientific journal.
David Anderson, chief scientist for the VBI, said it was not clear why the vaccine worked this way. One possibility is that an immune cell that is presented with multiple versions of a protein at the same time will not make antibodies against just one. Instead, a compromise antibody is made that works against all.
“You train it,” said Dr. Anderson, although he warned that this was speculation for now.
Last month, Pamela Bjorkman, a structural biologist at Caltech, and her colleagues published a more in-depth experiment with a universal coronavirus vaccine in Science magazine. The researchers only attached the tips of spike proteins from eight different coronaviruses to a protein core known as nanoparticles. After injecting these nanoparticles into mice, the animals produced antibodies that could attach to all eight coronaviruses – and to four other coronaviruses that the scientists hadn’t used in the vaccine.
Dr. Modjarrad leads a team at Walter Reed that is developing another vaccine based on a nanoparticle filled with protein fragments. They expect to begin clinical trials on volunteers next month. Although the vaccine currently only uses protein fragments from SARS-CoV-2 spikes, Dr. Modjarrad and his colleagues are preparing to convert it as a pancoronavirus vaccine.
Dr. Hoft at Saint Louis University is working on a universal vaccine that does not rely on antibodies to the spike protein. Working with Gritstone Oncology, a California-based biotech company, he developed a vaccine that prompts cells to make surface proteins that could alert the immune system as if a coronavirus – any coronavirus – was present. They are currently preparing a clinical trial to determine if it will be effective against SARS-CoV-2.
“We are interested in developing a third generation vaccine that is on the shelf and ready for the future outbreak,” said Dr. Court.
Dr. Topol believes that scientists should investigate another strategy as well: looking for the pancoronavirus antibodies that our own bodies make during infections.
Researchers studying HIV and other viruses have discovered rare types that act against a variety of related strains amid the billions of antibodies produced during infection. It might be possible to develop vaccines that will induce the body to make plenty of these largely neutralizing antibodies.
Coronaviruses are similar enough to each other, said Dr. Topol that it may not be that difficult to develop vaccines that make largely neutralizing antibodies. “This is an easy-to-remove family of viruses,” he said.
Finding a pancoronavirus vaccine may take longer than Dr. Topol’s sunny expectations. But even if it took a few years, it could help prepare the world for the next coronavirus to cross species boundary.
“I think we can have vaccines to prevent such pandemics,” said Dr. Memoli. “None of us want to go through that again. And we don’t want our children to go through this again, or our grandchildren or our descendants in 100 years. “