Fear isn’t the only factor that determines whether viewers act in moments like this. Bibb Latané, a social psychologist who pioneered viewer intervention in the years following the murder of Kitty Genovese, described another dynamic: the sharing of responsibility that can lead to inaction among strangers who witness a crime .
An increase in anti-Asian attacks
-
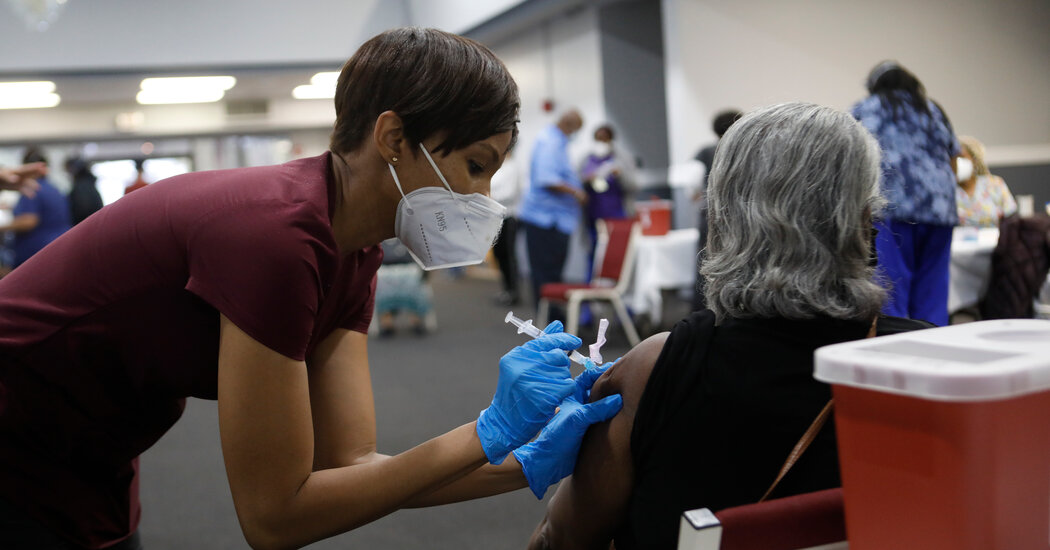
- In the early days of the coronavirus pandemic, a torrent of hatred and violence against people of Asian descent began in the United States last spring. Community leaders say the bigotry was fueled by the rhetoric of former President Trump, who called the coronavirus the “China virus”.
- A wave of xenophobia and violence in New York has been compounded by the economic fallout from the pandemic that dealt a severe blow to the Asian-American communities in New York. Many community leaders say racist abuse is overlooked by the authorities.
- In January, an 84-year-old man from Thailand was violently beaten to the ground in San Francisco, leading to his death in a hospital two days later. The videotaped attack has turned into a rally.
- Eight people, including six women of Asian descent, were killed in the shootings at the Atlanta massage parlor on March 16. The suspect’s motives are being investigated, but Asian communities in the United States are on high alert because attacks against Asian Americans have increased over the past year.
- A man was arrested and charged with hate crimes related to a violent attack on a Filipino woman near Times Square on March 30th. The attack sparked further outrage after security footage revealed that bystanders did not come to the woman’s immediate assistance.
Professor Latané, along with social psychologist John M. Darley, tried to replicate real emergencies through a series of laboratory experiments with people who did not know each other. The more viewers they found, the less likely it was that people would intervene. They also found that strangers unconsciously orientated themselves towards their fellow human beings, a concept known as social influence, and were less likely to intervene when others were similarly passive.
In an interview, Professor Latané said that the theories he and Mr Darley developed nearly five decades ago have often been overlooked by those who cling to popular notions of the emotionally distant viewer. He said these sentiments were often fueled by the news media, which tends to post incidents where witnesses failed to act while ignoring cases where viewers intervened. “It’s the unusual event that makes it current,” he said. “It was never about apathy, it was about social inhibition, and I’ve always thought it was unfair that New York should be judged for what happened to Genovese.”
Recent research examining real world interactions has challenged some of their earlier findings. For one, Professor Philpot’s 2019 study found that larger numbers of viewers increased the chances of intervention. When reviewing the surveillance footage, the researchers found that an average of at least three people had chosen an act, and they found that the presence of each additional bystander resulted in a 10 percent increase in the likelihood that a victim would receive help.
Although Professor Philpot said his research is not aimed at testing the theory of the side effect, the results suggest that there is safety in numbers. “While the presence of more bystanders can reduce the likelihood of each one of them intervening, it also provides a larger pool of potential helpers, increasing the overall likelihood that at least someone will help the victim,” he said.
Alan Berkowitz, an expert on the side effect and author of “Responsiveness: A Complete Guide to Viewer Intervention,” said other factors, including the race of the perpetrator or victim, could play an unconscious role in whether people help a stranger in need. “Research has found that viewers who are white, for example, may not feel like it is worth engaging in an incident with two people of color, but they may be more comfortable engaging in a fight between two whites male executives intervene, “said Dr. Berkowitz, a psychologist who runs workshops for students, community groups, and the military to find out how to intervene effectively to prevent acts of violence and sexual assault. “Once you are trained to become aware of these things and you are trained to conduct safe and effective interventions, you will feel more comfortable responding to your request for help.”
These tactics include distracting the perpetrator to call for help or find a way to get other bystanders to intervene more collaboratively. “It is very important to talk to other viewers as we often do not know that others are also affected,” he said.