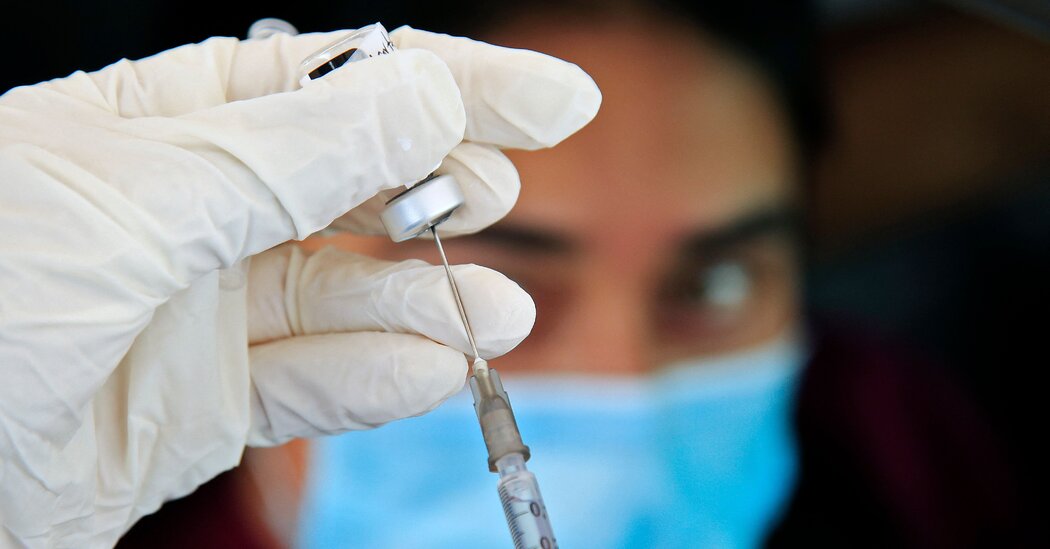
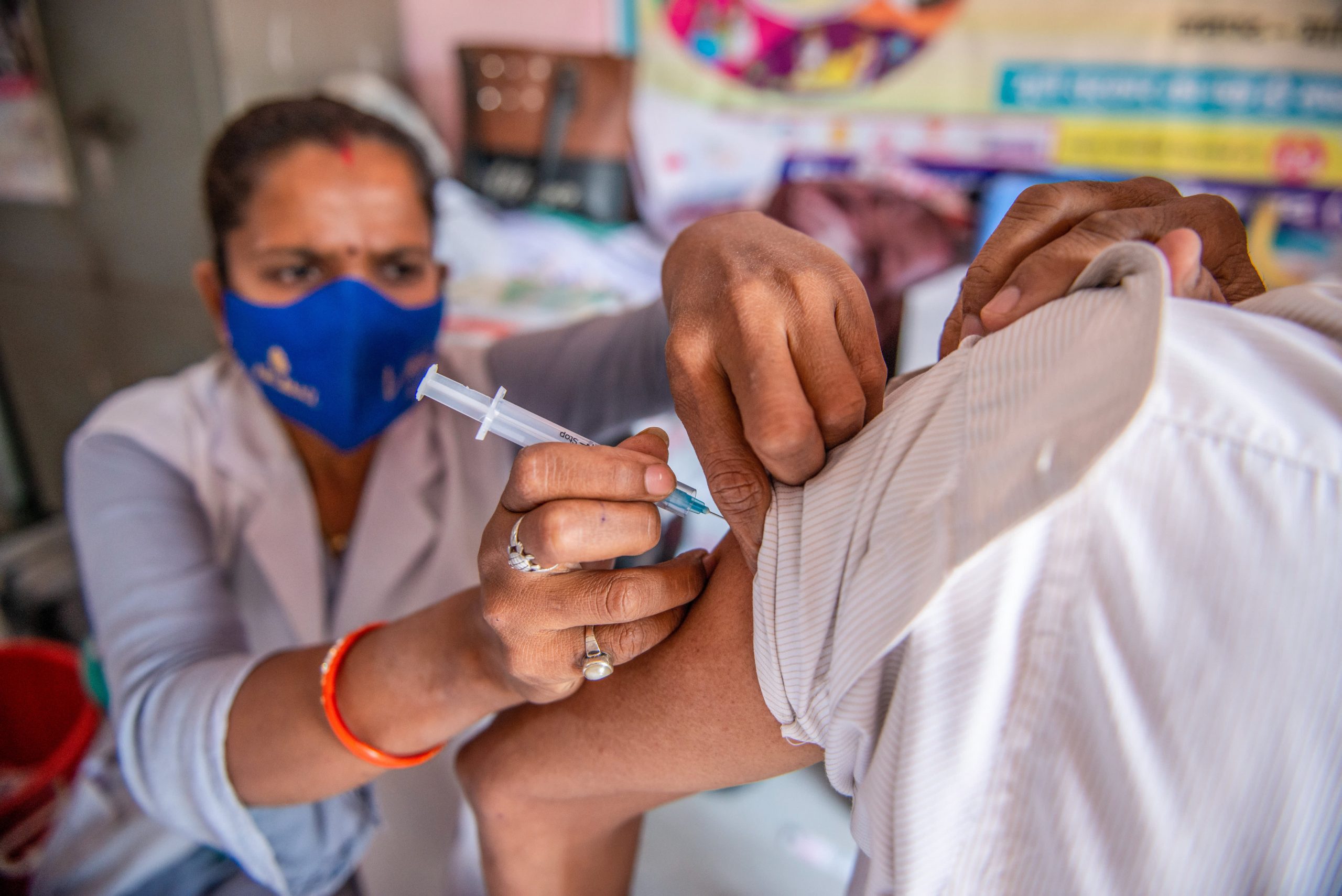
Dr. Anthony S. Fauci sagte am Donnerstag, er hoffe, dass die Nation bald wieder in der Lage sein werde, den Johnson & Johnson-Impfstoff zu verwenden, als eine „Pause“, die nun auf unbestimmte Zeit droht, die Impfbemühungen in Übersee und in einigen der am stärksten ausgegrenzten Länder anzukurbeln Gemeinden in den Vereinigten Staaten.
Dr. Fauci, Präsident Bidens oberster medizinischer Berater für die Pandemie, äußerte sich während einer Anhörung des House Select-Unterausschusses zur Coronavirus-Krise, in der er und andere hochrangige Gesundheitsbehörden des Bundes die Amerikaner anflehten, sich weiterhin impfen zu lassen, und versuchten, die Nation zu beruhigen dass alle drei staatlich zugelassenen Impfstoffe sicher sind.
“Hoffentlich werden wir bald eine Entscheidung treffen, ob wir mit diesem sehr wirksamen Impfstoff wieder auf Kurs kommen können oder nicht”, sagte Dr. Fauci dem Gremium. Angesichts der zunehmenden Fälle im Mittleren Westen, fügte er hinzu, befindet sich die Nation in einer „prekären Situation“, und es ist unbedingt erforderlich, „so viele Menschen so schnell und so schnell wie möglich zu impfen“.
Es wurde jedoch zunehmend klarer, dass eine Suspendierung, die ursprünglich zwei bis drei Tage dauern sollte, erheblich länger dauern würde, da die Beamten mit Berichten über mindestens sechs seltene Fälle von Blutgerinnung bei Frauen rangen, die mit dem Schuss von Johnson & Johnson immunisiert worden waren. Die Gesundheitsbehörden des Bundes versuchen zu entscheiden, ob sie den Ärzten empfehlen sollen, den Impfstoff wieder aufzunehmen, möglicherweise mit neuen Einschränkungen.
Der Impfstoff war kein wesentlicher Bestandteil der Impfkampagne der Biden-Regierung. Ungefähr 7,7 Millionen Amerikaner haben den Schuss von Johnson & Johnson erhalten, was weniger als 4 Prozent der mehr als 198 Millionen Dosen entspricht, die im ganzen Land verabreicht werden.
Obwohl diese Zahlen gering sind, sind viele der Menschen, gegen die der Impfstoff gerichtet ist, gefährdet: Obdachlose in Baltimore, Bewohner des District of Columbia, Arme und Nichtversicherte in Massachusetts, Landbewohner in einer Reihe von Bundesstaaten. Alle Populationen sind mit einer Einzeldosis leichter zu erreichen als das Zwei-Dosis-Regime der Impfstoffe Pfizer und Moderna.
Etwa 10 Millionen Dosen, die in die Staaten verschifft werden, stehen jetzt in den Regalen und warten auf eine Entscheidung. Und viele Menschen, die möglicherweise keinen Schuss suchen, aber mit mobilen Kliniken und einer konzertierten Kontaktaufnahme hätten erreicht werden können, könnten zumindest vorerst zurückgelassen werden.
„Alle unsere Impfstoffe, Anbieter im ganzen Bundesstaat und unser Team im Gesundheitsministerium von Minnesota arbeiten intensiv daran, die Dinge zu planen und zu verschieben. Es handelt sich offensichtlich um eine Reihe von Dominosteinen “, sagte Jan Malcolm, Minnesotas Gesundheitskommissar. “Wir bedauern sehr die Kliniken, die wegen der Pause bei J & J kurzfristig abgesagt werden mussten, und das wird auch in den kommenden Wochen ein Problem sein.”
Der Pressesprecher des Weißen Hauses, Jen Psaki, kalibrierte erneut das Versprechen von Präsident Biden, bis Ende Mai genügend Impfstoffe für alle amerikanischen Erwachsenen zu beschaffen. Jetzt betont das Weiße Haus, dass alle Erwachsenen, die einen Impfstoff wollen, einen bekommen werden.
“Das bedeutet, dass bis Ende Mai für etwa 80 Prozent der Bevölkerung, bis Ende Juli etwa 90 Prozent der Bevölkerung”, sagte Frau Psaki gegenüber Reportern.
In Lexington, Kentucky, wurde eine Johnson & Johnson-Klinik für Freitag abgesagt, sodass rund 400 Personen ohne Termin waren. Allen wurde eine Last-Minute-Option angeboten, um einen Moderna-Impfstoff zu erhalten, aber nur etwa 65 nahmen das Angebot an, sagte Kevin Hall, ein Sprecher des Gesundheitsministeriums von Lexington-Fayette County.
“Dies war ein großer Erfolg für unsere Planung”, sagte Hall, dessen Agentur den Johnson & Johnson-Impfstoff bereits für Insassen und Obdachlose verwendet hatte und geplant hatte, in den kommenden Wochen Nachbarschaftskliniken anzubieten. “Die Logistik für den Abzug einer Klinik für die erste und zweite Dosis wird sehr viel schwieriger.”
Dr. Letitia Dzirasa, die Gesundheitskommissarin in Baltimore, sagte, die Stadt habe bisher nur etwa 1.400 Dosen des Johnson & Johnson-Impfstoffs erhalten, aber viele seien auf obdachlose Bewohner ausgerichtet. Die Stadt muss möglicherweise ihre Pläne für Pop-up-Kliniken im Freien überdenken und sich bemühen, die Bewohner des Heimatlandes diesen Sommer mit dem Impfstoff mit einer Dosis zu erreichen, sagte sie.
“Wir dachten, J & J wäre der ideale Kandidat, um diese Arbeit zu unterstützen”, sagte sie.
In Washington, DC, verzögern Beamte ein Programm, um mit Johnson & Johnson-Schüssen heimatgebundene Bewohner zu erreichen. Die Stadt hat diese Woche Termine für etwa 1.200 Personen abgesagt, aber inzwischen sollten alle eine Einladung zu einem neuen Termin für einen der beiden anderen von der Bundesregierung zugelassenen Impfstoffe erhalten haben, die von Pfizer-BioNTech und Moderna entwickelt wurden.
Andere staatliche und lokale Gesundheitsbehörden sagten, sie würden mit diesen beiden Impfstoffen auskommen. In der Region Flint, Michigan, die einige der höchsten Fallraten des Landes in jüngster Zeit aufweist, gaben Beamte an, dass sie alle geplanten Kliniken auch ohne den Impfstoff von Johnson & Johnson abdecken konnten.
“Bisher war es reibungslos”, sagte Dr. Pamela Hackert, die medizinische Gesundheitsbeauftragte des Gesundheitsministeriums von Genesee County, in einer E-Mail.
Aktualisiert
15. April 2021, 16:49 Uhr ET
Am Des Moines Area Community College in Iowa konnten Administratoren diesen Monat drei Kliniken auf dem Campus einrichten, in denen die Studenten einen Impfstoff mit zwei Dosen erhalten können. Rob Denson, der College-Präsident, sagte, er sei erfreut und überrascht über seine Fähigkeit, diese zukünftigen Kliniken so schnell zu organisieren.
“Ich denke, wir werden in relativ kurzer Zeit mit Impfstoffen überflutet sein”, sagte er.
Eine längere Unterbrechung der Verfügbarkeit von Johnson & Johnson wird sich jedoch allmählich verschlechtern, insbesondere in ärmeren Staaten mit schwer erreichbaren Bevölkerungsgruppen. Eine Sprecherin von Dr. José Romero, dem Gesundheitsminister in Arkansas, sagte: „Die Pause sollte ausreichend lang sein, um Sicherheitsfragen zu beantworten, aber nicht länger als nötig verlängert werden.
“Seine Sorge ist, dass eine überlange Pause das Zögern erhöht und das Vertrauen verringert”, sagte die Sprecherin Danyelle McNeill. Dr. Romero leitet das Beratungsgremium zu den Zentren für die Kontrolle und Prävention von Krankheiten, die letztendlich empfehlen werden, wie mit dem Johnson & Johnson-Impfstoff verfahren werden soll.
Die Suspendierung in den Vereinigten Staaten kann tiefgreifendere Konsequenzen in Übersee haben, wo bisher nur ein Bruchteil der übrigen Welt geimpft wurde. Dr. Luciana Borio, eine ehemalige amtierende Chefwissenschaftlerin der Food and Drug Administration, die auch im Nationalen Sicherheitsrat des Weißen Hauses von Trump tätig war, sagte, der Impfstoff von Johnson & Johnson sei ein entscheidendes Instrument, um die Ausbreitung des Virus auf der ganzen Welt zu stoppen .
“Es ist ein Impfstoff, der schnell in sehr großem Maßstab hergestellt werden kann und viel einfachere Verteilungsverfahren hat”, sagte sie. “Die Welt braucht mehr Unternehmen wie J & J, die ihren Impfstoff liefern.”
Die Beamten zählten sowohl auf Johnson & Johnson als auch auf einen anderen leicht zu verteilenden Impfstoff von AstraZeneca, um Impfungen in schwer zugängliche Teile der Welt zu bringen. Jüngste Berichte über seltene Blutgerinnsel bei Empfängern des AstraZeneca-Impfstoffs haben jedoch eine Reihe von Nationen dazu veranlasst, seine Verwendung zu überdenken.
Einige Regionen beschlossen, zu Johnson & Johnson zu wechseln. Vor zwei Wochen hat die Afrikanische Union 400 Millionen Dosen erhalten, obwohl sich wohlhabendere Nationen gescheut haben. Die Europäische Union sagte, sie werde nicht mehr von Johnson & Johnson kaufen, und Australien kündigte an, keine Dosen zu kaufen.
In den Vereinigten Staaten schlugen Mitglieder des CDC-Beratungsgremiums am Mittwoch vor, dass es eine Woche bis 10 Tage dauern würde, bis sie über genügend Informationen verfügen, um die Risiken des Impfstoffs zu bewerten und eine Entscheidung über seine Zukunft in den Vereinigten Staaten zu treffen. Dr. Fauci und zwei weitere Beamte – Dr. Rochelle Walensky, der CDC-Direktor, und Dr. David Kessler, der die Impfbemühungen der Biden-Regierung leitet – forderten die Amerikaner auf, sich weiterhin impfen zu lassen.
“Ich hoffe, wir können alle zusammenkommen und diese Botschaft senden”, sagte Dr. Kessler, insbesondere angesichts der Verbreitung besorgniserregender Varianten, und fügte hinzu, dass die drei vom Bund zugelassenen Impfstoffe “ein ausgezeichnetes Sicherheitsprofil” haben.
Was Sie über die Johnson & Johnson Vaccine Pause in den USA wissen müssen
-
- Am 13. April 2021 forderten die US-Gesundheitsbehörden eine sofortige Unterbrechung der Verwendung des Einzeldosis-Impfstoffs Covid-19 von Johnson & Johnson, nachdem sechs Empfänger in den USA innerhalb von ein bis drei Wochen nach der Impfung eine seltene Erkrankung mit Blutgerinnseln entwickelt hatten.
- Alle 50 Bundesstaaten, Washington, DC und Puerto Rico, haben die Verwendung des Impfstoffs vorübergehend eingestellt oder von empfohlenen Anbietern unterbrochen. Das US-Militär, staatlich geführte Impfstellen und eine Vielzahl privater Unternehmen, darunter CVS, Walgreens, Rite Aid, Walmart und Publix, pausierten die Injektionen ebenfalls.
- Derzeit werden weniger als eine von einer Million Johnson & Johnson-Impfungen untersucht. Wenn tatsächlich ein Risiko für Blutgerinnsel durch den Impfstoff besteht – das noch ermittelt werden muss -, ist dieses Risiko äußerst gering. Das Risiko, in den USA an Covid-19 zu erkranken, ist weitaus höher.
- Die Pause könnte die Impfbemühungen des Landes in einer Zeit erschweren, in der viele Staaten in neuen Fällen mit einem Anstieg konfrontiert sind und versuchen, das Zögern des Impfstoffs anzugehen.
- Johnson & Johnson hat auch beschlossen, die Einführung seines Impfstoffs in Europa zu verzögern, da Bedenken hinsichtlich seltener Blutgerinnsel bestehen, was dem Impfschub in Europa einen weiteren Schlag versetzt. Südafrika, das von einer dort auftretenden ansteckenden Virusvariante am Boden zerstört wurde, stellte die Verwendung des Impfstoffs ebenfalls ein. Australien kündigte an, keine Dosen zu kaufen.
Die Berichte über Blutgerinnsel waren der zweite Schlag gegen den Johnson & Johnson-Impfstoff. Anfang dieses Monats hat eine Verwechslung von Inhaltsstoffen in einer Produktionsstätte in Baltimore, die Emergent BioSolutions gehört, bis zu 15 Millionen Dosen des Impfstoffs ruiniert. Die FDA inspiziert nun die Anlage, um festzustellen, ob dort hergestellte Dosen der Öffentlichkeit zugänglich gemacht werden können.
Während einer mehr als zweistündigen Anhörung fragte jedoch nur ein Gesetzgeber – der Vertreter Mark E. Green, Republikaner von Tennessee, der Arzt ist – nach dem Impfstoff von Johnson & Johnson. Er forderte die Ärzte auf, vorsichtig zu sein, wenn sie über die Ermittlungen sprachen, und sagte, er befürchte, dass sie Ängste schüren würden, die die Menschen davon abhalten würden, sich impfen zu lassen.
Und es gibt frühe Beweise dafür, dass die Besorgnis gut aufgenommen wird. Eine am Donnerstag vom Boston Children’s Hospital veröffentlichte Umfrage unter Survey Monkey ergab, dass die Bereitschaft, den Schuss von Johnson & Johnson zu erhalten, bei Amerikanern, die sich impfen lassen wollten, innerhalb von zwei Tagen um 26 Prozentpunkte zurückging. Laut der Umfrage, einem Projekt der Outbreaks Near Me-Initiative des Krankenhauses, einem Crowdsourcing-System zur Überwachung von Infektionskrankheiten, betrug der Rückgang bei Frauen, die sich impfen lassen wollten, 31 Prozentpunkte.
“Jedes Mal, wenn auf Bundesebene Bedenken oder rote Fahnen gehisst werden, wird dies die breite Öffentlichkeit beunruhigen”, sagte Dr. Dzirasa.
Die Sitzung am Donnerstag hatte den Untertitel „Ein wissenschaftlich fundierter Ansatz zur schnellen und sicheren Beendigung der Pandemie“. Aber was auch immer über Wissenschaft diskutiert wurde, wurde von parteipolitischer Haltung und Streit überschattet.
Demokraten machten sich Sorgen um den Fox News-Moderator Tucker Carlson, der seine Show genutzt hat, um fälschlicherweise zu behaupten, dass die Impfstoffe nicht funktionieren.
Die Republikaner, die gerade erst an der Südgrenze des Landes waren, nutzten die Sitzung, um den Umgang der Biden-Regierung mit der Einwanderungskrise anzugreifen. Sie winkten mit Fotos von Migranten, die unter beengten Verhältnissen lebten, und beschwerten sich über Testregeln für diejenigen, die in das Land einreisen.
Der Vertreter Jim Jordan, Republikaner von Ohio, und Dr. Fauci wiederholten ihren hitzigen Zusammenstoß, als Dr. Fauci das letzte Mal vor dem Panel im Juli aussagte.
“Sie schimpfen wieder”, sagte Dr. Fauci an einer Stelle.
“Ich schimpfe nicht”, antwortete Herr Jordan.
“Ja, das sind Sie”, beharrte Dr. Fauci.
Die Repräsentantin Maxine Waters, Demokratin von Kalifornien, deren Schwester an Covid-19 gestorben ist, sagte zu Dr. Fauci: „Ich liebe dich“ und sagte zu Herrn Jordan: „Halt den Mund.“
Noah Weiland, Rebecca Robbins und Sharon LaFraniere trugen zur Berichterstattung bei.